"Rural quagmire: Health equality sought in area"
By Jack Dew, Berkshire Eagle Staff
Sunday, April 13, 2008
Trying to address health disparities in the Berkshires, the state's public health commissioner will return to the area next week to discuss progress toward a healthier county.
John Auerbach, commissioner of the Department of Public Health, visited the Berkshires last spring and delivered a range of statistics showing the county trailing the rest of the state in several critical areas, including prenatal care, teen pregnancy, tobacco use and diabetes.
Over the past year, Auerbach's DPH has been working with county health officials to identify the shortcomings and to seek ways to address them. He will deliver an update during a panel discussion on Wednesday at 1 p.m. at the Lenox Town Hall auditorium.
Auerbach said he wants "to ensure that the Department of Public Health is paying attention to the issues that are affecting the residents of the Berkshires." Through "regular and good dialogue" with health care providers and residents, he said he hopes his agency will improve care and the overall health of the community.
The challenges are clear. Last year's report found that only 72.5 percent of expectant Berkshire mothers receive adequate prenatal care, compared with 84 percent statewide. In Pittsfield, this disparity was even more pronounced, with only 61 percent making sufficient doctor visits during their pregnancy.
Auerbach said the DPH has identified a critical shortage of obstetrician-gynecologists in the Berkshires, along with a lack of primary care providers. Although he did not present specific numbers yesterday, he said the agency is working on several programs to try to boost those numbers.
"This is one of the issues the DPH needs to take very seriously," he said.
As a partial response to the provider shortage, Senate President Therese Murray has proposed legislation that would create a primary care recruitment center to attract doctors to rural areas such as the Berkshires. It also would authorize the University of Massachusetts Medical School to increase its class size and expand its primary care programs.
Auerbach said officials also are considering increasing the numbers of visas available to foreign doctors willing to work in the Berkshires as well as financial incentives for physicians moving to Western Massachusetts.
Health professionals have told the DPH that the county's rural geography makes the public health mission more difficult here. It is harder to deliver a public health message and for patients to reach their caregivers. When it comes to vulnerable populations without ready access to a car — such as teenage mothers — those problems are magnified.
Peter Kolodziej, director of the Tri-Town Health Department that serves Lee, Lenox and Stockbridge in South County, has been championing a regional approach to public health in the Berkshires that would share the resources of the individual health departments and, he hopes, create a broader and more comprehensive reach.
Kolodziej said a number of models could work. There is the Tri-Town model, in which three towns pool resources to create a single agency that does everything from routine health inspections to anti-tobacco initiatives. Tri-Town has expanded its services, helping communities such as Pittsfield and Lanesborough conduct wellness programs. A less comprehensive, "cafeteria" model would allow communities to contract with a larger board of health for specific services.
There also is a need to replenish the ranks of public health workers with younger employees, Kolodziej said. The work force is aging and, without an infusion of applicants, some jobs will soon go begging.
He said he hopes the combination of a regional approach and the collaboration with the DPH will result in some quantifiable improvements to the health of the county.
"If we work together, we can address the issues in Berkshire County," he said. "But it will take a number of years before we can really make a difference."
-
To reach Jack Dew: jdew@berkshireeagle.com (413) 496-6241
-
----------
"State aims to close health gap"
By Jack Dew, Berkshire Eagle Staff
Thursday, April 17, 2008
LENOX — A year after the state Department of Public Health identified several worrisome trends among the population of Berkshire County, the commissioner returned with a message of cooperation to tackle health disparities.
John Auerbach, commissioner of the Department of Public Health, convened a meeting that he billed as a "regional health dialogue" yesterday at the Town Hall. Speaking to an audience of health administrators, doctors, nurses and caregivers, he said his agency is trying to work with local institutions to respond to the needs.
Foremost among the Berkshire concerns is a shortage of primary care providers and obstetrician/gynecologists, or OB/GYNs. Coupled with the state's health care reform that expanded access to affordable insurance and brought coverage to an estimated 15,000 people in the Berkshires, the shortage means that more people are having a harder time finding care and longer waits to get it.
"If you can't find a primary care doctor or you are pregnant and can't find an OB/GYN, you don't have access to care" despite your insurance card, Auerbach said. "We are trying to eliminate that problem."
The shortage is a statewide and national problem that is resistant to treatment. Primary care doctors are being driven from the field by shrinking reimbursement rates and growing caseloads. OB/GYNs have similar problems while facing large malpractice insurance payments.
The trend is hitting Western Massachusetts harder than the rest of the state. A survey found that the number of OB/GYNs declined 8 percent statewide from 2002 to 2004. In that same period, the four counties that compose Western Massachusetts lost 16 percent.
The Department of Public Health is expected to issue a full report on the shortage to the Legislature later this spring. The agency has already collaborated with the state Senate on legislation that would increase financial incentives for doctors willing to work in rural areas such as the Berkshires and encourage the University of Massachusetts to train more primary caregivers.
Officials also are considering increasing the number of visas available to foreign doctors coming to the Berkshires.
The need for care is clear: Western Massachusetts has the highest percentage of overweight and obese adults in the state, with nearly 61 percent considered overweight, and it has one of the highest rates of diabetes.
Vicki White, practice manager of Community Health Programs Health Center in Great Barrington, said her agency has seen a bottleneck of patients trying to get care as the insurance rolls increased.
Before health reform, she said, patients waited two or three weeks for a doctor's appointment. Now, they are waiting eight to nine weeks.
"It has been a real challenge for us to get our patients in to see someone," White said.
Edward Perlak, vice president of Berkshire Medical Center's Hillcrest Campus, said Berkshire County is suffering from disparities that are rooted in its geography and demographics. With 15 percent of the state's land but only 2 percent of its population, it has a difficult time reaching centralized care.
As the population is declining, it also is getting older, Perlak said: 18 percent of Berkshire residents are 65 or older, compared with the state average of 13 percent.
Although there are fewer babies being born here, 50.5 percent are born to mothers receiving some form of public assistance, versus 34 percent statewide.
"We have a spread-out, small population that is aging and generally less affluent than the state as a whole," Perlak said.
Auerbach said the Department of Public Health has heard the message of rural disparity and has examined ways to ease the problem. It has increased grant funding to Western Massachusetts as a whole and to the Berkshires in particular and is adding a regional director who will be responsible for the state's western district. The department also is considering adding a satellite office in Berkshire County.
"Some of the things that we will do are very concrete. Some of the things are rethinking how we do things," Auerbach said following the meeting. "What we will try very hard to do is take (these problems) seriously, think through what is the right action step in response to what somebody is raising and make a commitment to come back and say, 'Did we hear you right, and are the action steps taken addressing the issues you wanted us to pay attention to?' "
--------------------
"Primary care dilemma"
The Berkshire Eagle - Editorial
Friday, April 18, 2008
Compared to the rest of the state, Berkshire County's population is older, poorer and more rural. This puts it at a disadvantage in a variety of areas, among them health care, and the statewide shortage of primary care physicians is magnified here. It is a problem that defies easy solution, but it is one that state officials are aware of and are seeking ways to address.
John Auerbach, the commissioner of the state's Department of Public Health, and Dr. JudyAnn Bigby, the secretary of the Massachusetts Office of Executive Health and Human Services, each visited the Berkshires last week and thoughtfully addressed the shortage of primary care physicians. The combination of lower reimbursements and higher case loads is driving primary care doctors out of the profession and discouraging young physicians from entering the field, a problem that is magnified in the rural Berkshires. The county's state-leading percentage of obesity and high rate of diabetes can be attributed at least in part to this shortage as it is the primary care physicians who assess a patient's overall health and advocate preventive measures.
Mr. Auerbach's DPH is working with the state Senate on legislation to offer financial incentives for doctors willing to work in rural areas and is encouraging UMass to develop a program to train more primary care doctors. Dr. Bigby, whose office advocates a program that will provide educational loans to doctors agreeing to join the primary care field in the state, declared in an editorial board meeting at The Eagle that primary care doctors should be better paid, even if that means specialists must make less money given the limited pool of funds available. A former primary care physician herself, the doctor argues convincingly that "bread and butter" medicine has been devalued in favor of the technology that, while valuable, encourages the costly tests fueling a rise in health care costs.
The Berkshires also face a shortage of obstetrician/gynecologists for the reasons noted above, along with punishing malpractice insurance costs. It is encouraging, however, that there are efforts afoot by state health leaders to assist the Berkshires in easing, if not solving, these dilemmas.
--------------------
"'Missionaries' reach out in county"
By Jack Dew, Berkshire Eagle Staff
Sunday, April 27, 2008
Missionaries from the Tri-Town Health Department are being dispatched to five Berkshire communities, spreading the gospel of good health to municipal employees.
Armed with an $85,000 grant, Tri-Town is sending health outreach workers to Lee, Lenox, Stockbridge, Pittsfield and Lanesborough, where they will conduct screenings, offer wellness programs and assess the workplace environment.
The state Department of Public Health — which is encouraging communities to work together to combat health problems — issued the grant. Tri-Town has used the funds to contract with Berkshire Health Systems, from which Roberta Orsi and Jenna Grelle-Laramee will lead the initiative.
Assessing employees and families
Working with a steering committee that includes a representative from the five communities, Grelle-Laramee and Orsi will develop ways to assess and improve the health of roughly 2,800 employees and their families.
They hope to conduct health assessments with interested employees and to use health claims data to identify problems. From there, they will design initiatives, perhaps offering weight-loss programs, stress-reduction workshops or smoking-cessation classes. They also can provide counseling, advising employees of their risk factors and connecting them to the proper health professionals.
Peter Kolodziej, Tri-Town's director, said the five communities are eager participants in the program and hope to improve the health of their work force while trimming spending because of lost hours and medical treatment.
"Administrators and managers know the importance of having a healthy work force for productivity, absenteeism and reducing health care costs," Kolodziej said.
Tab has doubled
Lenox Town Manager Gregory Federspiel said that all towns want employees to be as healthy as possible for their own sake, but that the town also has a real financial interest — Lenox's health insurance tab has doubled over the past six or seven years, he said, and is now close to $2 million.
"When you look at the drivers of our health costs, almost three-quarters of it is related to unhealthy lifestyles. It is preventable — that is the bottom line," Federspiel said. "We all complain about skyrocketing health costs, but we are the problem, at least in part."
Orsi and Grelle-Laramee hope that the outreach will produce a change in culture. As employees begin participating in smoking-cessation and weight-loss efforts, perhaps others will follow suit, replacing the smoke break with a brisk walk and the doughnut platter with a fruit bowl.
"These communities that have signed on are really taking a leadership role," Kolodziej said. "Once you get the culture changing and the employees see the benefit, it will be word of mouth. They might talk to a friend or relative out of town and, hopefully, if we get some good outcomes in these towns, other towns will think about it."
--------------------
"A smoking gun"
The North Adams Transcript Online - TheTranscript.com - Editorial
Monday, June 9, 2008
Statistics released by state health officials Friday about the smoking rates in Pittsfield and North Adams were alarming to say the least and bear repeating here:
In Pittsfield, 26 percent of the population smokes cigarettes, and in North Adams, more than 30 percent smokes, compared to a statewide average of 18 percent. More shockingly, among pregnant women, 26 percent in Pittsfield smoke and a whopping 33 percent in North Adams, compared to a statewide average of 7 percent.
In this day and age, when the dangers of smoking have been clearly documented -- particularly the dangers for unborn children -- something clearly needs to be done.
Kudos to the state for launching a program in which free nicotine patches will be given away to those who are at least willing to try to quit. Beyond that, the schools and local health departments should get involved. Somehow the word doesn't appear to be reaching our young people that smoking not only is bad for your health but also is potentially deadly. Furthermore, at well over $5 pack, the habit has become even more expensive than filling your gas tank.
Smokers can help with this situation, even if they don't care to quit or even to try. If you have children in the house, smoke outdoors or designate one room with good ventilation where your youngsters won't see you (or smell the aftereffects of your disgusting habit).
And please, can you try for a change to dispose of your cigarette butts properly? The landscape everywhere is littered with them, and all too many smokers still seem to think nothing of tossing butts out the car window or flipping them nonchalantly onto our streets and sidewalks.
Consider this from CigaretteLitter.Org: "It is estimated that several trillion cigarette butts are littered worldwide every year. That's billions of cigarettes flicked, one at a time, on our sidewalks, beaches, nature trails, gardens and other public places every single day. In fact, cigarettes are the most littered item in America and the world.
"Cigarette filters are made of cellulose acetate, NOT COTTON, and they can take decades to degrade. Not only does cigarette litter ruin even the most picturesque setting, but the toxic residue in cigarette filters is damaging to the environment, and littered butts cause numerous fires every year, some of them fatal."
Smokers, please try this: Carry a small bag or empty cigarette pack with you, field strip your cigarettes and temporarily dispose of the butts in the bag or pack until you can get to a waste receptacle. In the car, use a partially full water bottle (cap it after dousing butts to avoid the unpleasant smell).
Better yet, as the state Department of Health and numerous public officials have urged, just quit! There is no better time than right now, and your children and grandchildren (if you live to see them) will thank you for it.
--------------------
-

-
Stacy Michaud, a registered nurse, monitors the medication for Sandy Redman at North Adams Regional Hospital, where the performance in most key categories is in line with state and national statistics. (Photos by Ben Garver / Berkshire Eagle Staff)
-
"Health Care in the Berkshires: Where are we?"
By Jack Dew, Berkshire Eagle Staff
Sunday, June 22, 2008
Is Berkshire County a good place to get sick? For Steve Green, 64, it was. An administrator at the Massachusetts College of Liberal Arts, he felt chest pains while working at his dining room table one night five years ago. He rushed to North Adams Regional Hospital, where he was given clot-busting drugs, quickly reopening a clogged artery.
Two months later, Green went to Baystate Medical Center in Springfield, where cardiologists inserted a stent — a small metal tube — into the problem artery to hold it open.
"Since then, my checkups have been fine," Green said.
Throughout his experience — from the onset of symptoms to his final visit with a cardiologist in North Adams — Green said he had confidence in the treatment he received, despite the county's challenges of delivering health care in a relatively isolated setting to a relatively small population.
"I am well aware that the local hospital doesn't do it all, and people go to Albany or Baystate or Boston for procedures and second opinions," he said. "That's fine ... but I have just always had a really good feeling about our health care in the Berkshires."
Despite Green's optimism, the state of medicine in Berkshire County remains a mix of positives and negatives as the health-care system struggles to cope with a changing medical landscape.
Deaths from major cardiovascular disease declined 30.6 percent from 1995 to 2005. Berkshire Medical Center is the first hospital in the country to have earned a gold award from the American Heart Association for seven consecutive years for its basic care of patients with coronary artery disease. And state numbers show that BMC and NARH deliver the recommended care to heart attack patients 99 percent of the time while keeping costs under control.
Meanwhile, the Berkshires and Western Massachusetts have lower cancer rates than the rest of the state in most categories, particularly prostate and lung cancers, and an Eagle review of malpractice suits decided against Berkshire doctors showed no substantial deviation from the state norm.
But minuses exist in the region medically.
Just as the nation is experiencing a shortage of primary care doctors, so is Berkshire County. Just as Americans are suffering more of the conditions that produce a risk of heart disease, the Berkshires are unable to offer the best procedure for many heart attack patients.
"The biggest negative (about health care in Berkshire County) is accessibility," said John Rogers, vice president and general counsel for Berkshire Health Systems, the parent company of Berkshire Medical Center in Pittsfield and Fairview Hospital in Great Barrington. "We have ... high-quality physicians and people in Berkshire County — patients should have no concern about that — but the bigger issue is getting in to see someone."
There are roughly 1,333 adults for every primary care provider in the county. In calls to 20 randomly selected doctors this month, 12 were no longer accepting new patients. Calls to 15 doctors who still had open practices found an average wait time of nearly 11 weeks for an annual checkup.
Charles Joffe-Halpern, executive director of Ecu-Health Care in North Adams and president of the board of directors of Health Care for All, a statewide advocacy group, said the Berkshires face the challenges that come with the reorganization of medical care, including the rise of health maintenance organizations and the birth of state health reform.
"Doctors tend to concentrate in more densely populated areas, so it is a challenge to recruit physicians here," Joffe-Halpern said. "In areas like Great Barrington, Pittsfield and North Adams (the sites of the county's three hospitals), if one or two doctors leave, they will feel that more than in densely populated areas, where there are more doctors to begin with."
But like Green, Joffe-Halpern said he has always felt well-cared-for in the Berkshires, including five years ago, when he called his doctor with a complaint of frequent headaches. He had an MRI and was referred to Massachusetts General Hospital in Boston, where he was diagnosed with a benign brain tumor. His treatment — both in the Berkshires and Boston — was successful.
"I got excellent care. I was able to see my physician quickly, received the right tests and an appropriate referral," Joffe-Halpern said. "I see that all the time. There is a lot more that can be done at community hospitals now than could be done 10 years ago, but when certain specialties are needed, I have seen our patients get quick treatment at bigger hospitals."
By some measures, the Berkshires — particularly North Adams — appear to suffer from a lack of specialists. The Dartmouth Atlas of Health Care, which analyzes medical data for thousands of Medicare patients, found that patients in North Adams visited a specialist about half as often as the state average during the final two years of life.
For patients who need specialized care or whose hospital stay takes a turn for the worse, getting the right treatment may mean leaving the region.
There also are signs that a dearth of primary care providers could be contributing to the county's health problems. The number of pregnant women receiving adequate prenatal care is lower than the Massachusetts average, and the Berkshires have more diabetes sufferers, more smokers and more obese adults than the state average.
In the area served by North Adams Regional Hospital — including North Adams, Adams and Williamstown — statistics gathered by the Dartmouth Atlas of Health Care show that people are hospitalized for heart attacks at a rate that is 60 percent higher than the national average, and the rate for certain kinds of strokes is 40 percent higher, suggesting that higher rates of tobacco use, obesity and diabetes are taking a toll.
North Adams Regional has tried to tackle these problems with outreach and prevention. It runs nutrition and fitness classes for families at the public library, has started community gardens to help connect people with local, fresh produce, and it does dozens of cholesterol and blood pressure screenings a year.
"These are things that, statistically, we know are attacking the right problems," NARH spokesman Paul Hopkins said. "But we probably won't see the results for a generation."
When it comes to picking a doctor or hospital, patients have few places to turn for easy-to-understand, reliable information.
Health officials advise patients to do their homework using the few resources available: Find out which hospitals and doctors perform a procedure the most; talk with friends and family about preferred doctors; and turn to statistics such as those gathered by the U.S. Department of Health and Human Services at www.hospitalcompare.hhs.gov.
While the federal and state governments have been making more information on health outcomes available, officials acknowledge the system remains less than perfect.
"We are in the infancy of consumer information on health care," said Dr. Marylou Buyse, president of the Massachusetts Association of Health Plans. "We have much more information on toasters and cars than we do on our health care system. That needs to change."
The federal government has only recently started gathering patient opinion on hospitals; patients in the Berkshires report that they like their hospitals slightly less than patients do nationally.
In a federal survey conducted from October 2006 through June 2007, 53 percent of respondents gave Berkshire Medical Center a "high" mark of nine or 10 for an overall rating; for North Adams Regional Hospital, the number was 60 percent. In the state and nation, 63 percent of people rated their hospital a nine or 10.
Still, the Berkshires have outpaced the state in the reduction of deaths due to cardiovascular disease, coronary heart disease, heart attack and heart failure.
Gray Ellrodt, medical director at Berkshire Medical Center, said the hospitals have tried to live within their medical means, making the care they deliver the best it can be.
And all three hospitals have been honored by the American Heart Association for their performance in "Get with the Guidelines." The program rates how often hospitals conform to the basic — but often overlooked — standards of care for patients with coronary artery disease, stroke and heart failure, giving patients aspirin and other medications, and advising smokers to quit, among a variety of measures.
Health care providers throughout the Berkshires — from doctors' offices to hospitals — say they recognize there is room for improvement and are striving to do better. They are recruiting primary care doctors aggressively, working to improve the daily treatment they give patients, and trying to expand their services.
"We need to be better on the front end of health and wellness," Ellrodt said. "That is the challenge in this community."
-
To reach Jack Dew: jdew@berkshireeagle.com; (413) 496-6241.
-
--------------------
-

-
Dr. Mark Pettus withdrew from practicing mainstream medicine when his health started to decline. Pettus, the former chief of nephrology at Berkshire Medical Center, now practices at the Kripalu Center for Yoga and Health in Lenox. (Ben Garver / Berkshire Eagle Staff)
-
"Health care in the Berkshires: Where are we?"
"Diagnosis: a problem"
"Western Massachusetts has the biggest shortage of primary care doctors in the state, and the situation is only expected to worsen."
By Jack Dew, Berkshire Eagle Staff
Monday, June 23, 2008
For Dr. Mark Pettus, the epiphany came while he was sitting on an exam table in the office of his primary care doctor seven years ago.
An internist and chief of nephrology at Berkshire Medical Center in Pittsfield, Pettus was having his annual checkup. Like many of us, he had been skipping this yearly ritual — too busy, too stressed, too short of time to see his doctor.
"I was actually walking the walk for once," Pettus said. "I'm 51, and while I've never confronted serious health problems, my family history is horrible. Both my parents died young, had heart disease, were diabetics. They just had everything the average American either has or is at risk of getting."
Within a year, Pettus decided that the medicine he had been practicing for 20 years wouldn't cure his high blood pressure and high cholesterol. He opted to cut ties with mainstream medicine, giving up his practice.
As America is living longer, gaining weight and confronting more complicated health problems like diabetes, primary care doctors are fleeing the field. Practicing doctors are retiring younger, studies show, and medical students are choosing better-paying specialties.
Western Massachusetts and the Berkshires are no different, and in fact are in "crisis mode," suffering the worst primary care shortage in the state, according to Dr. Bruce S. Auerbach, head of the Massachusetts Medical Society.
In 2007, a group of primary care doctors, with the support of the Massachusetts chapter of the American College of Physicians, surveyed all 79 practicing internists and family practitioners in the county and found that 46 percent had reduced their clinical hours or were planning to leave the field in the near future. Ninety-one percent said they would have reservations or recommend against others going into primary care.
There are no hard rules for how many primary care doctors a region should have, or for the ideal ratio of patient to doctor. But health leaders say the Berkshires clearly are short of the necessary complement, and they are desperately trying to recruit new doctors from a dwindling supply.
Lisa Trumble, director of faculty services at Berkshire Medical Center, estimated that the county needs about 10 additional primary care doctors. With a drove of retirements expected in the next few years, she said the situation will only worsen.
"If you look at the supply of physicians going into primary care versus those coming out, it continues to decline," Trumble said. "There is never enough for the demographic demands."
There are roughly 1,333 adults for every primary care provider in Berkshire County. In calls to 20 randomly selected doctors this month, 12 were no longer accepting new patients.
Meanwhile, calls to the remaining eight doctors on that list, along with seven additional doctors still accepting patients, found an average wait time of nearly 11 weeks for an annual checkup.
Setting the tone
When the system is at its best, the primary care doctor is the quarterback of a patient's care, directing specialists, coordinating tests and bringing all the players together.
Pettus had been practicing medicine in Berkshire County for more than 20 years as he sat on his doctor's exam table. As a nephrologist, he consulted with people who needed dialysis, often in the advanced stages of liver or kidney disease. As an internist, he saw patients at BMC's walk-in clinic, treating those in need of care but who lacked insurance or a steady relationship with a primary care provider.
As his physician went through the routine exam, the numbers weren't good. Pettus' blood pressure, cholesterol and weight were up, the consequence of long, stress-filled hours in the office and too many hand-held meals washed down with soda. As he sat in the exam room, Pettus said he saw himself living out the genetic legacy of his parents.
"I thought, 'Thank goodness this is happening at a time when there is Lipitor (a cholesterol-lowering drug).' I began to think about all the treatments that I knew existed now that didn't exist for my parents that I could use to alter this natural history."
But Pettus then realized he'd gained 15 pounds over the past four or five years, and the extra weight might be to blame for a share of his bad numbers. Then there was his stressful job, his diet and the state of medicine in general, in which preventive care has taken a back seat to reactive care, treating conditions only after they surface.
"Soon after that, I wrote a letter to my partners saying I am going to resign from the practice. It shocked my wife. After 20 years, she never thought she would see the day."
Pettus unplugged from mainstream medicine. He started educating himself in nutrition — not just the saturated fat and high-fiber school, but the more esoteric framework of antioxidants, Omega-3 fatty acids and glycemic indexes. He said he has been able to control his blood pressure and cholesterol without medication.
Soon, he said, nutrition became like a second language, one he thought could help his patients if he had time to counsel them. And he knew he would never be given the time in today's medical marketplace, in which insurers put a premium on procedures while discounting the kind of consultation that primary care doctors practice.
So Pettus, like an increasing number of primary care doctors, left his field.
He now practices at the Kripalu Center for Yoga and Health in Lenox, an alternative health mecca that draws clients from around the country and the world.
While eating macrobiotic dishes in the dining hall and meditating on a hill overlooking the Stockbridge Bowl, patients can consult with Pettus, spending an hour discussing their health condition, how they could change their diet, whether they need so many medications, and what they can do to incorporate the lessons of Kripalu — yoga, meditation and diet — into their daily lives.
"It is continuous education that I value so much, and I'm able to bring it into a model of care and support that allows the time to share it more effectively," Pettus said.
But he also is one fewer doctor available at the medical walk-in, one fewer primary caregiver to meet a growing demand. Pettus has become part of a shortage that is occurring just as Massachusetts has massively expanded the number of insured, adding 300,000 people in less than two years to the insurance rolls with its health-care reform laws.
"The crisis already exists," said Auerbach, the president of the Massachusetts Medical Society and the chief of emergency and ambulatory services at Sturdy Memorial Hospital in Attleboro.
"If we don't address these primary care issues, I think it is going to be increasingly difficult to contain health-care costs, (and) there is a great likelihood that the health care of our population might decline overall as prevention becomes a smaller focus."
Auerbach said Western Massachusetts and the Berkshires have "the dubious honor of ranking number one among the areas where there is a crisis."
Doctors, patients, insurance
In interviews, doctors practicing throughout the county bemoan what they see as increasing interference in their relationship with patients. Every regulation, every new insurance guideline, is intruding further into the examination room, a space once considered sacred. That trend is accompanied by shrunken reimbursements from a medical system that places a higher value on specialists.
"It is the art of taking a (medical) history," said Dr. Robert Jandl, of Williamstown Medical Associates. "What you want in primary care is to take people who have the capacity to ask the right question, get responses and come up with an assessment."
A patient having chest pains can't just be referred to a cardiologist for tests, Jandl said. The pain could be angina or muscular, or the patient already could be treating high blood pressure and cholesterol problems but perhaps could stand to lose weight or exercise more often. Maybe the pain comes and goes, or responds to a home treatment such as a hot-water bottle.
It is a conversation between doctor and patient that might be repeated dozens of times a day in exam rooms throughout the Berkshires, but physicians say it is increasingly competing with the minutiae of regulatory compliance.
To prescribe diapers for an adult patient suffering from cerebral palsy, for instance, Jandl said he needs three forms of documentation: a written prescription, a letter to the insurer, and a photocopy of the point in his examination notes where he concluded the patient needed diapers. With the prescription, the patient's insurer will pick up most or all of the tab; without it, the patient will have to bear the cost. Over the course of a year, that bill could total more than $2,000.
"There is this whole micromanagement, trying to control what you do, as if you are an extension of an insurance company," Jandl said.
'A very complex issue'
Insurance companies say they aren't interfering in the relationship between doctors and patients but are trying to control the rapid rise of premiums. Dr. Marylou Buyse, president and CEO of the Massachusetts Association of Health Plans, said the insurance companies' concern is that patients get the proper treatment at the proper price.
Doctors are upset but reluctant to change, Buyse said. They are clinging to the Medicare model, which pays a pre-determined amount for each service, and they give little consideration to new approaches, such as paying doctors a salary based on the number of patients they treat, or on performance and the ability to control costs.
"This is a very complex issue and not an easy one to solve," Buyse said. "I think the doctors, rather than blaming the insurers, should look to Medicare (to place blame), because Medicare has been the leader in payment policy."
Faced with declining numbers of primary care physicians, hospitals have been forced to help solve the problem. Where doctors once ran practices as independent small businesses that recruited new physicians to replace older members, doctors now have neither the finances nor the reach to recruit, according to John Rogers, vice president and general counsel for Berkshire Health Systems, the parent company of Berkshire Medical Center.
For the past five years, BMC has partnered with independent practices, helping them underwrite new hires in return for a commitment to keep those doctors in the community for a certain number of years. The lure is quality of life in the Berkshires and fewer hospitals that doctors have to see patients in.
"It is critical for hospitals to maintain outside practices," Rogers said. "The portrait of the medical community in Berkshire County in 2008 would be entirely different if we weren't in partnership with those practices to help them."
To satisfy demand, the medical system needs to increase supply. But studies show that fewer medical students are interested in primary care.
Auerbach, of the Massachusetts Medical Society, said that decision is largely financial: A med-school student often graduates as much as $200,000 in debt, and primary care likely pays between $125,000 and $150,000 in the first year, while a specialist in dermatology, cardiology or radiology can earn a salary in the range of $300,000 to $400,000 in the first year.
The pay disparity is rooted in our reimbursement system, health officials agree. Procedures — a colonoscopy, an MRI, or a stress test — earn higher payments than a consultation. Primary care doctors likely will get paid for the 15 minutes they spend examining a patient but will earn little for the next 15 minutes spent talking to the patient about his or her concerns.
The doctors say the process puts a strain on their practices. Saddled with overhead expenses for support staff, malpractice insurance and the routine costs that come with running an office, they must generate enough income to keep the business running. That means seeing more patients, which means shorter patient visits.
"Primary care doctors are always feeling rushed. They are always feeling like they can't spend the time with the patient that they want," Auerbach said.
Meanwhile, insurance companies are pursuing new reimbursement systems, with the current trend toward "tiering," in which the insurer calculates the quality of a doctor's care and the doctor's ability to control costs. The two are combined to rate that physician, and the insurer will use lower co-pays to steer patients toward doctors with the best rating.
Tiering has been met with opposition from doctors and hospitals and, earlier this month, the Massachusetts Medical Society filed a lawsuit challenging it. The group questions how any formula could gauge the quality of a doctor's care and measure it against cost, and they ask who they'll be compared to — doctors across the street, across the county, or across the state or nation.
Calling all doctors
Berkshire health providers are seeking short-term solutions to the primary care shortage. Berkshire Health Systems has helped some of its foreign residents get visas, allowing them to stay in the area and treat patients.
And in its recruiting efforts, BHS pitches the Berkshires as an antidote to what ails primary care — a place where doctors can find a mix of quality of life and professional opportunity, where they only have to worry about covering patients at three hospitals instead of a dozen.
"We are finding that Berkshire County is an easier sell than we thought," said Arthur Milano, Berkshire Health's vice president of human resources. "We have something unique here, and we have capitalized on it."
The primary care shortage won't be fixed until the reimbursement system changes and doctors are paid more for the care they give, most health professionals agree. But that fix may be years in the making or may never arrive.
The alternative is that more physicians will choose a path similar to Pettus'. He traded a higher salary and busier lifestyle for a slower pace that allows him to practice what he considers to be the best care. By healing himself, he said, he is now better able to heal others.
"When you experience something in such a profound way, it influences the way you try to serve others," Pettus said. "It is easier for me now to talk about the power of food, the power of movement.
"I feel like the story I created for myself is one that will allow me to more effectively connect with others."
-
To reach Jack Dew: jdew@berkshireeagle.com, (413) 496-6241.
-
--------------------
-

-
Adams Police Chief Donald Poirot was a health and fitness devotee when he suffered a heart attack at age 47 last July. Poirot is fine now, but his heart stopped on the day he suffered the attack. (Ben Garver / Berkshire Eagle Staff)
-
"Health care in the Berkshires: Where are we?: Heart of the matter"
By Jack Dew, Berkshire Eagle Staff
Tuesday, June 24, 2008
Donald Poirot was devoted to fitness. The chief of police in Adams, he spent hours working out in the department's gym and on warm summer days would bike "the loop" — a 40-mile trek that took him around Mount Greylock. He had never been diagnosed with high blood pressure or high cholesterol.
Other than a stressful job, Poirot lacked the warning signs for a heart attack.
Late one afternoon last July, Poirot, 47, was coasting down his street, cooling off after a blazing loop, scanning his bike's computer to check his average speed.
"I started to get a pain in my back, kind of dead center," Poirot said. "It was like a hot poker. It hurt, it was intense, but it wasn't putting me to the ground."
Poirot hung up his bike in the garage and sat, as he usually did, to drink water and cool down, putting himself back together after a grueling workout. When he went inside, his wife joked about how long he'd been gone.
"I said, 'Leave me alone, I'm not feeling right.' I tried drinking water, taking in fluids, and took a shower. The pain wouldn't go away. I'm 47 years old, I work out every day, I watch what I eat. There is nothing wrong with me," said Poirot, who was 19 years shy of the average age for a male heart attack victim.
"I was in complete denial."
But his wife wasn't. She told Poirot she was taking him to the emergency room. Less than an hour after the onset of symptoms, the two climbed into their truck and headed to North Adams Regional Hospital.
A question of numbers
Like roughly 154 patients in Berkshire County each year, Poirot was having a heart attack, or acute myocardial infarction. One of the arteries feeding his heart was clogged, and his heart was failing as it tried to keep functioning.
The gold standard for care in a patient such as Poirot is cardiac catheterization and stenting. In catheterization, a doctor uses a tiny camera attached to a long wire to navigate from a blood vessel in the patient's groin up to the heart. Once the clot is found, the doctor can open a balloon at the end of the tube and break the clog apart. Then a stent — a tiny mesh tube made of metal — is inserted, holding the artery open.
While Berkshire Medical Center runs a small catheterization lab in Pittsfield, state law doesn't allow hospitals to perform stent procedures unless they also perform open-heart surgery, a complicated operation reserved for the largest, best-equipped hospitals.
BMC would also have to do at least 200 diagnostic catheterizations and 35 procedures on acute heart attack patients each year. Berkshire County, with its population of only 131,000 people, will never generate enough cases to meet those standards.
Thus, the chances of surviving a heart attack and making a full recovery in the Berkshires are slightly but measurably lower than if a patient received treatment at a facility that offered stenting.
"People in this county are at a distinct disadvantage when they have an acute heart attack in the sense that we can't deliver the one intervention that has the best short- and long-term outcome," said Dr. Jeffrey Leppo, division chief of cardiology at Berkshire Medical Center in Pittsfield. His group of 11 cardiologists now serves BMC, North Adams Regional and Fairview Hospital in Great Barrington.
A review of 23 trials published in the medical journal The Lancet in 2003 concluded that catheterization — both with and without a stent — resulted in a small but measurable difference in outcome.
Patients who underwent catheterization instead of treatment with clot-busting drugs — available in the Berkshires — that reopen clogged arteries had a reduced chance of short-term death (7 percent vs. 9 percent) and stroke (1 percent vs. 2 percent).
Leppo, Berkshire Medical Center and the 10 additional cardiologists in his division have been trying to devise a way to bring stenting to the Berkshires. By partnering with Baystate Medical Center in Springfield — the closest in-state hospital that performs the procedure — they hope to forge an arrangement that will allow doctors to split time between the two hospitals, solving the volume problem.
A matter of time
Studies show that the quicker a stent is inserted after the onset of a heart attack, the better. That action saves the most muscle and creates the best chance for recovery.
Ideally, qualified patients will be in a catheterization lab within 90 minutes of arriving at the hospital. But on a good day, it takes patients from North Adams Regional Hospital an hour and a half to reach Baystate by ambulance, and it takes about an hour from BMC and Fairview.
Patients from NARH may have a quicker trip to Albany Medical Center in New York, where stenting also is available, but the trip is about the same from Fairview and BMC.
In most cases, meeting the 90-minute deadline is nearly impossible. Patients often wait after the onset of symptoms before they call 911 or seek treatment. Once at the hospital, an evaluation takes time, followed by at least a 60-minute ride to Baystate.
"The adage in the trade is that time is muscle," said Dr. George W. Dec Jr., chief of cardiology at Massachusetts General Hospital in Boston. "The sooner you can establish blood flow, the better off you will be. In a perfect world, every hospital would have a (cardiac catheterization) lab and a team of cardiologists and nurses who could do the procedure and staff it 24/7. Clearly, that is not practical."
Leppo, the BMC cardiologist, said he hopes to get a waiver from the open-heart rule and overcome the logistical obstacles to offering stents within the next 18 to 20 months.
"Baystate is the only hospital in Western Massachusetts that does this, yet we are easily an hour away if nothing goes wrong," Leppo said. "And we can't just pick people up off the street when they say they have chest pain and take them to Baystate. They need to be evaluated."
Dr. JudyAnn Bigby, the secretary of Health and Human Services in Massachusetts, said she doesn't think there is data to support expanding this procedure to regions such as the Berkshires.
"This has to do with patient safety if (hospitals) don't do a certain number of this highly specialized procedure," Bigby said. "But there are things that can be done in community hospitals, and should be done" to improve patient outcomes.
Clot-busting drugs, called thrombolytics, are considered the next-best treatment. Given intravenously, they can dissolve a dangerous clot and restore blood flow. Time is still urgent, and hospitals aim to administer the drugs within 30 minutes of a patient coming through the emergency room doors.
In the Berkshires, two out of the six patients brought into North Adams Regional Hospital with symptoms of a heart attack were moved from door-to-drug in less than 30 minutes from October 2006 through June 2007, according to federal data.
At Berkshire Medical Center in Pittsfield, nine of its 10 patients were. And at Fairview Hospital in Great Barrington, only one patient met the criteria and was not given the drug in under 30 minutes.
If the drug fails, however, the patient must be transferred quickly to a cardiac catheterization lab, where the stenting procedure would be complicated by the presence of a powerful anti-clotting drug, making any kind of surgery more dangerous.
Dr. Gray Ellrodt, medical director at Berkshire Medical Center, said the health system recognizes its limitations. To compensate, it has tried to become better at every other level of cardiac care.
The system has focused on doing the basic "blocking and tackling," Ellrodt said, making sure patients are given the proper evaluation when they arrive at the hospital and the proper drugs for that diagnosis. Simple steps — putting patients on aspirin, counseling smokers to quit — help reduce the rate of recurrence.
The efforts appear to be getting results. Deaths from major cardiovascular disease — which includes heart attack, heart failure and stroke — were down 30.6 percent in Berkshire County from 1995 to 2005.
"I think we do the basics here as well or better than any hospital in the country," Ellrodt said. "The challenge becomes not to lose sight of that and continue to do (the basics) year in and year out. We don't want to be good one day and bad on the next."
Calling 911
Poirot and his wife had made their biggest — and probably only — mistake of the day when they didn't call 911 for an ambulance, opting to drive to the emergency room themselves.
This is a common error among heart attack sufferers. Doctors say patients often are in denial, unable to believe they could be suffering a heart attack.
But an ambulance is a far more efficient way to travel to the hospital. Not only can it run red lights and speed through traffic, many are now equipped with electrocardiogram machines that can detect a heart attack. The results can be radioed ahead to the hospital, which can have a crew standing by with the proper drugs ready to go, greatly reducing the delay from door to treatment.
Based upon the type of their heart attacks, about 30 percent of patients are eligible for catheterization, Ellrodt said. And between 40 and 50 percent of those patients walk into an emergency room on their own.
"They are not activating the 911 system," Ellrodt said, "and the reality is that your outcome from a heart attack is not related so much to the time from the (hospital) door to treatment, it is the time from onset."
At County Ambulance in Pittsfield, the Berkshires' largest ambulance company, president Brian Andrews said education efforts to increase calls to 911 have had some effect, but too many people still ignore the signs or fail to call for help.
"We know that the data shows that, if they have 911 intervention, their chances are going to be much better for a good outcome because we can get things rolling on their care much quicker," Andrews said.
But Poirot was fortunate. As he walked into North Adams Regional Hospital, he was greeted by an orderly he knew.
"He asked me if I was OK. I said I didn't think so, and he said, 'You look terrible.' He put me in a wheelchair and wheeled me in" past the waiting patients who typically fill any ER's waiting room, Poirot said.
'My heart stopped'
As doctors and nurses tended to Poirot, members of his family started showing up. He chatted with them and said he was going to be fine.
"I didn't know at this point that I was having a heart attack. I was thinking it was an OK thing," he said.
But then, suddenly, it wasn't.
Poirot's heart stopped. A clogged artery had been denying blood to his heart.
"Everything went out. The lights went out. My heart stopped," Poirot said.
Essentially, he was dead.
The medical team used a defibrillator to shock Poirot's heart, hoping to restore its rhythm. The first attempt failed. On the second, Poirot's heart started beating again, and he returned to life.
Doctors then administered the clot-busting drugs, which succeeded in reopening the artery. Poirot was taken to the intensive care unit to spend the night under close monitoring.
Within two hours of his symptoms setting in, Poirot had been given clot-busting drugs, a best-case scenario that too often isn't the case, doctors say.
Many patients wait too long to go to the hospital. Perhaps they awoke in the middle of the night and mistook chest pains for a case of indigestion, or they thought an overzealous session at the gym had left them sore between their shoulder blades.
With patients sometimes arriving at the hospital two hours or more after a heart attack has begun, there is even more pressure on the emergency room to diagnose quickly and begin treatment.
The emergency rooms of all three hospitals in the county now follow the same streamlined protocol that guides them from the moment the patient arrives. Emergency room doctors can diagnose a heart attack without calling a cardiologist, saving precious minutes.
"Once you make the ER doc have to call someone to find out what is going on, you waste incredible amounts of time," said J. Mark Peterman, an interventional cardiologist at Baystate who also practices at BMC. "In reality, the ER docs have been empowered and trained to have the responsibility to make the diagnosis and commit to treatment."
The "crucial piece," Leppo said, is deciding whether to start treatment at a Berkshire hospital or ship the patient immediately to Baystate. In the most dire of cases, the hospital might do both at once, starting the drug treatment in the ambulance as it heads to Springfield, a practice known as "drip and ship."
Once a clot is broken apart, the Berkshire hospitals have done all they can do, and most patients will eventually need to visit a cardiac catheterization lab — either immediately, the next day, or within the next few weeks.
'Enjoy life'
At first, Poirot said, doctors contemplated flying him to Baystate via LifeFlight helicopter. But as is often the case in the hills and valleys of North Adams, the wind was too strong for the helicopter to land.
The next morning, Poirot was put into an ambulance with a nurse and an IV drip and taken to Springfield. There, doctors already had his file on their computers, thanks to a tight communication link with the Berkshire hospitals.
Poirot was awake throughout the procedure. Afterward, doctors replayed what they had seen on a flat-screen monitor.
"There was this big screen and pictures of my heart, and they told me what went wrong. They showed me right where the artery was pinched together," Poirot said. "They said my arteries were huge and clean, except for that one little part, but we fixed it, so go and enjoy life."
Poirot was shortly back at work, resuming a full schedule.
"For a while, I had a really different perspective on life, and I don't want to lose that," he said. "Sometimes life sucks you back in, the hecticness of the job and what not, and that can get to you. When things aren't going right, I have learned to sit back and review and, on occasion, walk away, because it is just not worth it."
He also is back in training. Two weeks ago, as summer weather smothered the Berkshires and temperatures climbed into the 90s, Poirot climbed back onto his bike and rode the 40-mile loop.
-
To reach Jack Dew: dew@berkshireeagle.com, (413) 496-6241.
-
Lowering the risk of heart attack
Maintain a healthy weight, with a Body Mass Index of 18.5 to 24.9. To calculate your BMI, divide your weight in pounds by your height in inches squared. Then multiply that by a conversion factor of 703. Example: Weight = 150 pounds, Height = 5'5" (65 inches). Calculation: (150 / (65 x 65)) x 703 = 24.96, a weight at the top end of the "normal" scale.
Choose good nutrition, using a diet rich in vegetables, fruits, whole-grain and high-fiber foods, fish, lean protein and fat-free or low-fat dairy products.
Know your blood pressure and treat high blood pressure. For healthy adults, the target blood pressure is 120/80.
Know your cholesterol and treat high cholesterol. Total cholesterol should be less than 200 mg/dL. HDL — or "good" cholesterol — should be 40 mg/dL or higher for men and 50 mg/dL or higher for women. LDL — or "bad" cholesterol — should be less than 160 mg/dL for those at low risk for heart disease, less than 130 mg/dL for those at intermediate risk, and less than 100 mg/dL for those at high risk or who have diabetes.
Do aerobic exercise (walking, running, biking, swimming, etc.) at least 30 minutes a day on most or all days.
Control your blood sugar. A fasting glucose level should be under 100 mg/dL
Reduce stress.
Limit alcohol. Drinking too much can raise blood pressure and lead to heart failure or stroke. Women who have one drink a day and men who have two drinks a day, however, have a lower risk of heart disease, though non-drinkers aren't encouraged to start drinking.
Source: American Heart Association. To take a test that will analyze your risk of a heart attack and offer ways to control your risk factors, visit www.americanheart.org.
Signs of a heart attack
The American Heart Association says that some heart attacks are sudden, intense and obvious, but most start slowly with mild pain or discomfort. Patients often aren't sure what's wrong and wait too long before seeking help. Here are signs that can mean a heart attack is occurring:
Chest discomfort. Most heart attacks involve discomfort in the center of the chest. The feeling lasts more than a few minutes or goes away and comes back. It can feel like uncomfortable pressure, squeezing, fullness (the sensation of having eaten too much; might be felt in the stomach, chest or both), or pain.
Discomfort in other areas of the upper body. Symptoms can include pain or discomfort in one or both arms, the back, neck, jaw or stomach.
Shortness of breath with or without chest discomfort.
Breaking out in a cold sweat, nausea and/or lightheadedness.
For men and women, the most common heart attack symptom is chest pain or discomfort. Women, however, are somewhat more likely to experience other common symptoms, particularly shortness of breath, nausea/vomiting, and back or jaw pain.
Note: Even if you're sure you aren't having a heart attack, tell a doctor about your symptoms.
Seeking help
Don't wait more than five minutes to call 911, which is almost always the fastest way to get life-saving treatment. Emergency medical services (EMS) personnel can begin treatment when they arrive — up to an hour sooner than if someone gets to the hospital by car. EMS staff members are trained to revive someone whose heart has stopped. Patients with chest pain who arrive by ambulance usually receive faster treatment at the hospital, too. It is best to call 911 for rapid transport to the emergency room.
If you can't access the emergency medical services (EMS), have someone drive you to the hospital immediately. If you're the one having symptoms of a heart attack, don't drive yourself unless there is no other option.
Source: American Heart Association
--------------------
"Primary care survey"
Community: (Berkshire County, Massachusetts)
The Berkshire Eagle Online, Monday, June 23, 2008
A group of primary care providers, with support from the Massachusetts chapter of the American College of Physicians, conducted a survey last summer of all active primary care doctors in the county. Some of their findings:
Number of primary care doctors: 79
Average age: 51
Percent who expect to retire in 5 years or less: 18.5
Percent currently taking new patients: 65.2
Percent "very satisfied" with practice: 13.2
somewhat satisfied: 39.7
somewhat dissatisfied: 32.4
very dissatisfied: 14.7
Percent who would "definitely" choose primary care again: 10.3
probably yes: 26.5
probably no: 42.7
definitely not: 20.6
Percent who said it is "somewhat difficult" to recruit new doctors: 26.1
very difficult: 60.9
not applicable: 13
--------------------
"First issue is primary care"
The Berkshire Eagle - Editorial
Wednesday, June 25, 2008
The three-part Eagle series "Health care in the Berkshires" by Jack Dew painted a picture of a fine health network that, largely because of its rural location, is being hit hard by the problems that affect patients, doctors, nurses and administrators around the country to varying degrees. These problems are national in scope, leaving Berkshire residents to find ways, like a patient following a health trauma, of living with them while waiting for a cure.
The seven gold awards won by Berkshire Medical Center from the American Heart Association, the first hospital in the nation to win them consecutively, shows what our health care community is capable of doing. The awards recognized BMC's care of patients with coronary heart disease, and indeed, county deaths from cardiovascular disease declined by 30.6 percent between 1995 and 2005. Cancer rates are lower than the rest of the state, which speaks well of the preventive care offered.
There are challenges facing the Berkshire health care community, however, and the growing shortage of primary care physicians may be the most worrisome. There are too few now, and with coming retirements, many will not accept new patients, while current patients will face longer waits for appointments. Primary care providers are on the front lines of health care, and their scarcity may be a major reason why the county has disproportionate problems with diabetes, obesity and smoking.
Unfortunately, this Berkshire problem requires a national solution to a worrisome degree. It would help if the insurance companies would stop burying primary care doctors in the paperwork that takes time away from patients. Controlling costs is not the job of a physician, and the bureaucrats should not judge them on it. Primary care physicians are underpaid compared to specialists, and given that the pool of money is finite, it is no disrespect to specialists to argue that they should be paid less so primary care doctors can be paid more.
Berkshire County has good hospitals and a good quality of living to offer primary care physicians, as well as specialists. If the problems endemic to the health care industry were resolved, the shortage of primary care doctors would be resolved as well.
--------------------
"Strengths of community hospitals"
The Berkshire Eagle - Letters
Thursday, June 26, 2008
The June 22 article in the Berkshire Eagle regarding the state of health care in Berkshire County highlighted the scope of local hospital services, as well as quality data measurements and their favorable comparison to state benchmarks. The article was both enlightening and revealing, and the hospital systems, their employees and their respective medical staffs should be commended for achieving above-average results in the majority of quality indicators.
Hospitals are now required to report quality indicators by numerous state (Department of Public Health), federal (Centers of Medicare and Medicaid Services) and national agencies (The Joint Commission), to name only a few. The article supports this author's opinion that the majority of medical services can be and are provided by our local community hospitals. Transfer to a tertiary care center (such as Baystate or Albany Medical Center) occur in only a small number of cases.
Despite the majority of quality indicators with above-average scores when compared to the overall state benchmarks, the response by patients on the likelihood of recommending their hospitals was less than I would have expected. The data does not appear to reflect the patients' total hospital experience. I have always said that the caring aspect of medicine is an integral part of a patient's health care experience. It is a critical aspect of the overall care provided by our community hospital.
This is difficult to measure but to me is what distinguishes community medicine and the community hospital experience from the sometimes necessary tertiary care experience.
The quality of health care and overall ease of access of patients to the health care system is often one of the important aspects by which society and any geographic area is measured. This article supports the notion that Berkshire County has high quality health care. Our goals should be to continue to improve the overall patient experience.
I commend the Eagle for its timely and insightful journalism.
PAUL DONOVAN, M.D.
North Adams, Massachusetts
-
The writer is president of the medical staff, director of emergency services at North Adams Regional Hospital.
-
-----
"Primary flaw in health care system"
The Berkshire Eagle - Letters
Thursday, June 26, 2008
I commend the Eagle for its three-part series on heath care in the Berkshires. The article on the depressing troubles in primary care one day followed by the thrilling account of a patient who had a cardiac catheterization the next illustrates a deep and enormous flaw in our health care system.
According to the article, the advantage of having your heart attack at an institution such as Baystate Medical Center, where stenting and cardiac bypass surgery can be done at a moment's notice, is a mortality rate of 7 percent. This compares to a mortality rate of 9 percent if you have your heart attack in local hospitals that are not equipped for these procedures. The article went on to quote Dr. George W. Dec, Jr., chief of cardiology at Massachusetts General Hospital, as saying that "In a perfect world every hospital would have a (cardiac catheterization) lab and a team of cardiologist and nurses who could do the procedure and staff it 24/7."
So, on any given day, any one of us will have a 2 percent better chance of surviving a heart attack if we have access to this technology. Two per cent. Now consider the enormous cost of fully staffing and operating a cardiac catheterization lab 24 hours a day in order to reap that 2 percent reward.
Meanwhile, primary care is on life support with the brightest and best fleeing the field, 47 million of our citizens are completely uninsured with many millions more under-insured, and we rank near the bottom in international measures of quality of care among all developed countries. There are reams of data spanning the last 30 years, applicable to all areas of the country and across all demographic groups and across all developed countries of the world to indicate that communities with robust primary care have better health outcomes (than those dominated by specialists), at lower cost, and with greater equity for its citizens.
While high tech interventions make for compelling stories there is a massive lost opportunity in this systemic under-investment in primary care that makes a 2 percent mortality benefit pale in comparison.
ROBERT JANDL, M.D.
Williamstown, Massachusetts
-
The writer is president, Williamstown Medical Associates.
-
-----
"Appointment wait reveals problem"
The Berkshire Eagle - Letters
Thursday, June 26, 2008
I was interested in your series about health care in the Berkshires. I've certainly heard my fair share of horror stories from others, but thus far my experience had been OK.
Sure, it can be tricky, being fairly new to the area, to find a general practitioner. Yes, I had to wait seven months to get in with a dermatologist. But today I got the kicker.
I used to get my mammograms at Berkshire Radiological on North Street. I was so disappointed that they were squeezed closed. I was assured when that happened that BMC/BHS would continue to support their patients. Well, I had to call my doctor to find out when this year's mammogram was due because I never got notice it was due. Turns out, I should've had it done in February. As a woman who has a strong family history of breast cancer, this is very important.
After getting caught in voice mail hell twice, I finally found someone who told me the first chance I would have to get this year's mammogram was September! Ah, the joy of having a virtual monopoly in the county. They were so worried about someone else getting a piece of the pie, but they can't support the whole pie themselves!
DEB HASTINGS
Pittsfield, Massachusetts
-
Editor's note: The writer reports that after sending the letter she was able to get a mammogram appointment for this Friday at North Adams Regional Hospital.
-
--------------------
"Primary flaw in health care system"
The Berkshire Eagle - Letters
Friday, June 27, 2008
I commend The Eagle for its three-part series on heath care in the Berkshires. The article on the depressing troubles in primary care one day followed by the thrilling account of a patient who had a cardiac catheterization the next illustrates a deep and enormous flaw in our health care system.
According to the article, the advantage of having your heart attack at an institution such as Baystate Medical Center, where stenting and cardiac bypass surgery can be done at a moment's notice, is a mortality rate of 7 percent. This compares to a mortality rate of 9 percent if you have your heart attack in local hospitals that are not equipped for these procedures. The article went on to quote Dr. George W. Dec, Jr., chief of cardiology at Massachusetts General Hospital, as saying that "In a perfect world every hospital would have a (cardiac catheterization) lab and a team of cardiologist and nurses who could do the procedure and staff it 24/7." Consider the enormous cost of fully staffing and operating a cardiac catheterization lab 24 hours a day in order to reap that small reward.
Meanwhile, primary care is on life support with the brightest and best fleeing the field, 47 million of our citizens are completely uninsured with many millions more under-insured, and we rank near the bottom in international measures of quality of care among all developed countries. There are reams of data spanning the last 30 years, applicable to all areas of the country and across all demographic groups and across all developed countries of the world to indicate that communities with robust primary care have better health outcomes (than those dominated by specialists), at lower cost, and with greater equity for its citizens.
While high tech interventions make for compelling stories, there is a massive lost opportunity in this systemic under-investment in primary care that makes a modest mortality benefit pale in comparison.
ROBERT JANDL, M.D.
Williamstown, Massachusetts
The writer is president, Williamstown Medical Associates.
--------------------
-

-
Dental hygienist Kristabel Vargas performs a routine screening demonstration at the CHP clinic in Great Barrington.
-
"Filling a need: 'Access barriers' are the first to crumble"
By Jessica Willis, Berkshire Eagle Staff
Tuesday, July 01, 2008
GREAT BARRINGTON — The reclining chairs in the examining rooms were empty, and the tools were neatly arranged on metal trays, waiting to be used. In less than an hour, Community Health Programs Dental Center would be open for its first day of business.
Before the first patients arrived at 11 a.m., the Dental Center staff was joined by legislators, project fundraising heads, and Community Health Programs administrators, who toured the facility and expressed their relief that a dental clinic had finally opened in South Berkshire. It's a region where 80 percent of adults and children treated by CHP's health center face all kinds of "access barriers" to oral health care, according to studies.
Many problems
The barriers in the county are caused, at least in part, by its geographic remoteness, the financial problems that come from losing a day's wages to a dentist appointment, and insufficient insurance, said Judy Eddy, CHP's development director.
In the past, most South County patients were referred to Berkshire Medical Center's Dental Clinic in Pittsfield, which takes the MassHealth insurance plan, but the BMC clinic is so backlogged, it cannot accept new patients until further notice.
The new clinic, which has a waiting list of more than 1,700 patients, will provide free care or reduced rates based on a sliding scale formula, and accepts MassHealth insurance. It's the only dental care facility in South County to do so.
U.S. Rep. John W. Olver, D-Amherst, surveyed the clinic's five examining rooms, each with its own flat-screen computer monitor and state-of-the-art oral cancer screening equipment.
Suggestion from Olver
Olver suggested that many communities focus on building medical clinics, while dental health needs go unnoticed and untreated.
And then "we realize the dental needs (in a community) are far greater," Olver said.
State Rep. William "Smitty" Pignatelli, D-Lenox, cited the shortage of dentists in the state, and added that fewer still will "tackle" MassHealth.
Pignatelli also expressed his frustration with the idea that MassHealth "will pay to extract a rotten tooth but won't pay to prevent (the decay)."
Tooth decay that has gone beyond the preventive stage is wrecking more than just a lot of bright smiles in the county, said Luci Z. Leonard, an outreach nurse for CHP.
Leonard said she believed cardiovascular disease and diabetes had links to poor oral health, and she wondered if the "active disease process" could have been stopped if the patient had access to dental care years ago.
The 1,700 patients on the waiting list were found though CHP outreach programs — at schools, homes, churches, senior centers, and the like. Outreach was also responsible for the recruitment of the Dental Center's director, Dr. Monica Torrenegra, who completed her medical residency at Yale University and hails from Colombia.
"And that's not Columbia County (N.Y.)," quipped Marcia Savage, CHP's executive director, in her address at the opening ceremony. "That's pretty good outreach."
Torrenegra, who currently lives in Waterbury, Conn., and plans on moving to Great Barrington, told the group that she learned about the job at the clinic when she was on her way to her father's funeral.
"I had been thinking at the time, should I go back to Colombia?" Torrenegra recalled, her voice trembling with emotion. "But I realized my future was here."
The Dental Center, which is located at 343 Main St., is funded by a $1 million grant from the Oral Health Foundation, a $90,000 grant from the University of Massachusetts Medical School's Office of Community Programs, and a $25,000 grant from the state's Health and Educational Facilities Authority, which funded the clinic's information technology infrastructure. For more information, call (413) 528-5565.
-
To reach Jessica Willis: jwillis@berkshireeagle.com, (413) 528-3660.
-
--------------------
"Shortage hurts Commonwealth Care"
The Berkshire Eagle - Letters
Thursday, July 03, 2008
In his fine series of articles on health care in Berkshire County and western Massachusetts Jack Dew highlights the shortage of primary care physicians. The remediation of this problem is a long-term issue involving appropriate governmental funding, incentives to providers, increased sophistication in recruitment techniques and retention and encouragement of currently practicing physicians to remain in practice by changing the work environment. But this can only occur in the longer run and there is a need to consider transition problems.
One issue resulting from the lack of physician availability is the effect on quickly implementing Commonwealth Care, which was designed to provide those unable to afford health insurance but with income above the federal poverty guideline an opportunity to obtain care. Because of the shortage of primary care physicians in this region, individuals and families approved by Commonwealth Care are unable to find providers and are seeking alternative means of obtaining medical services.
This trend is apparent to those of us who work at the Volunteers in Medicine Berkshires (VIM) free health care clinic in Great Barrington. In the past several months, we have seen an increase in patients utilizing our facilities while waiting for the opportunity to become connected with a primary care physician. The clinic was founded to deal with the uninsured patient population but until there is more accessibility of primary care physicians, we are providing a transition link for many of the newly insured.
Berkshire County's situation raises an issue that needs to be accounted for as broader coverage is made available by state or federal governments: sufficient thought must be given to transition alternatives as individuals move from uninsured status to covered status. As our nation moves forward trying to make health care affordable and accessible for the 53 million of us who are presently uninsured, there must be a careful review of physician availability by region as well as a structure established to provide transition care to the newly insured unable to connect to a specific provider.
In VIM's case there is no cost to taxpayers for us to provide transition health care services as we are entirely supported privately though the generosity of individuals, businesses and foundations and our services are provided largely through volunteer health care and lay professionals. We exist because of the inadequacies of the present system. The designers of any future national or state health care systems must provide for what VIM is currently doing.
LEONARD S. SIMON
Monterey, Massachusetts
The writer is treasurer, Volunteers in Medicine Berkshires.
--------------------
"Berkshire County doctors get mixed review"
By Jack Dew, Berkshire Eagle Staff
Thursday, July 10, 2008
When it comes to communicating with patients, Berkshire County primary care providers and pediatricians are among the best in the state, according to a new survey that will be released today, but they aren't as good when it comes to administering preventive care and advice.
The study was conducted by the Massachusetts Health Quality Partners, a group that combines insurance companies, the Massachusetts Hospital Association, the Massachusetts Medical Society and state health officials. It surveyed patients about their experiences with primary care providers and their offices. The results will be available today on the group's Web site, mhqp.org.
On the whole, patients of the county's nine largest doctors groups said they feel their doctor communicates well with them: Five of the groups received four out of four stars, meaning they scored better than 85 percent of offices. No Berkshire office received fewer than three stars in that category.
But when patients were asked how well doctors administer preventive care and advice, the results weren't as strong. Five offices received two stars — meaning they scored poorer than 50 percent of hospitals but better than the bottom 15 percent. One office scored in the bottom 15 percent; two received four stars and one three stars.
'Action-oriented questions'
Barbara Rabson, executive director of the Massachusetts Health Quality Partners, said the results of the survey will likely be used more by doctors than patients, showing physicians where they can improve or confirming a job well done.
"If you tell (doctors) how they can improve, they will work on improving," Rabson said. "These are very action-oriented questions. If a physician looks at the survey and finds out that 30 percent of their patients feel they aren't being communicated with about test results, that is a pretty specific thing to work on."
For patients, the usefulness of the information is less certain. With the state suffering a shortage of primary care doctors, most have few options when seeking a doctor. That shortage is being felt even more acutely in the Berkshires and Western Massachusetts, health officials agree, and many doctors are no longer accepting new patients.
"For consumers, it is a little trickier," Rabson said. "If you have trouble with your existing physician and are closed out of others, that is unfortunate, and this (survey) is not going to help you."
Dr. Mark Snowise of Suburban Internal Medicine in Lee said it is "always helpful to get feedback," and he and his colleagues will look at the results. But the information also belongs to a universe of other data and must be considered in context, he said. His office scored low for how well doctors give preventive care and advice, yet it always scores highly on its Blue Cross Blue Shield evaluation of that same category
Skewed perceptions
"There is definitely a perception of what patients think they are getting and what they are actually getting," Snowise said. "If you ask the majority of Medicare patients if Medicare covers a physical, they say yes. In fact, it doesn't after the first six months."
Likewise, what might constitute prevention to a doctor — talking to patients about diet, exercise, smoking and other lifestyle choices — may not feel like prevention to the patient.
Dr. Andrew Potler of East Mountain Medical in Great Barrington said he and his partners will likely review the survey and discuss it at their usual weekly meeting.
"We may say that .. it doesn't seem true to the way we perceive things, or, if our patients' perceptions are clearly bent in one direction, we may say we need to re-look at it," Potler said. "Doctors have concerns about people looking in at us, but in the sense of taking a poll of our patients, I think that can be helpful."
Family practice rates high
The survey also sought to gauge patients' opinion of the overall office — getting timely appointments and their experience with other doctors, nurses and staff. Northern Berkshire Family Practice scored particularly high, with four stars in all three office categories.
Statewide, 51,000 adult patients and 20,000 parents of pediatric patients responded to the survey, which was mailed directly to patients on their insurance provider's letterhead in September and October. In all, 42 percent of people asked to participate either returned a survey by mail or filled one out online.
Four out of five patients in Massachusetts said their primary care provider always provided clear explanations, listened carefully and offered clear instructions.
But when patients were asked to assess other medical providers in the same office — be it another doctor, a nurse practitioner, or physician assistant — the responses were less positive. Only slightly more than half said the other provider always explained things clearly and spent enough time with them.
-
To reach Jack Dew: jdew@berkshireeagle.com (413) 496-6241
-
--------------------
Pittsfield, Massachusetts
"Health center expands services"
By Trevor Jones, Berkshire Eagle Staff
Tuesday, August 05, 2008
PITTSFIELD — As health care costs continue to rise, two local organizations have come together to provide expanded access, especially for the under- and uninsured.
The Neighborhood Health Center, located at 510 North St., officially became a Federally-Qualified Health Center yesterday, with expanded facilities and a broader range of services and care for patients.
The center will now be known as the CHP Neighborhood Health Center and is a collaboration between Berkshire Health Systems and Community Health Programs. They will provide treatment to anyone who comes through their doors, no matter what their economic or health care status is.
They will also provide information on how to obtain health insurance for any patients who are interested.
The major goal of the center's improvements was to "try to meet the needs of the most needy and to make it as easy as possible," said Marcia Savage, executive director of Community Health Programs.
In addition to several facility upgrades, to be a federally qualified health center the facility must offer care to patients of all ages. That meant the addition of several new kinds of care, including pediatrics and obstetrics, as well as future programs like gynecology, dental and nutrition.
"We had a good facility. Now, I think we have a terrific facility," said Ruth Blodgett, senior vice president of planning and development for Berkshire Health Systems.
The added services will allow the center to care for patients they were previously unable to, like pregnant women and children. Executives for the center believe the facility's improvements will make it a central location for families to meet as many of their medical needs as possible.
"This will only enhance what our staff and physicians can do for the community," added Savage.
--------------------
"A primary problem"
The Berkshire Eagle - Editorial
Friday, September 12, 2008
Only two percent of graduating medical students plan to work in primary care fields according to a study released this week. Welcome, America, to a serious problem Berkshire County is already well aware of.
It's not surprising that young doctors are gravitating to where the money is, and primary care physicians make far less on average than do specialists. As the backbone of the medical system, primary care doctors nip medical problems in the bud and encourage the preventive care that stops many costly medical problems from arising. These pay scale disparities must be rectified.
A more complex problem, however, was highlighted by radiology resident Dr. Jason Shipman of Vanderbilt University Medical Center, who told The Associated Press that primary care didn't appeal to him because he "didn't want to fight the insurance companies." Insurance company bureaucrats burden all doctors with needless paperwork, but the primary care doctors bear the brunt of it, along with all of the other red tape that binds our medical care system in ways that doctors in nations with government-provided universal health care never experience.
Massachusetts' innovative health care reform effort has helped many state residents, especially its poorest, get health care, but it is running into cost problems that will threaten its expansion. Helping generate those costs are the insurance companies, with their bloated overhead and highly paid executives, and any reform that doesn't address this mammoth problem is not truly extensive reform.
Governor Patrick and the Legislature are certainly aware of the primary care doctor shortage in the state. They have been pursuing financial incentives to persuade doctors to work in rural areas and educational loans to doctors who agree to join the primary care field in the state. UMass. is being encouraged by the Patrick administration to develop a program to train more primary care doctors. These are worthy initiatives that will help ease the shortage of primary care doctors, but as long as the health insurance bureaucracy is in place, this and many other problems in the health field will go unresolved.
--------------------
"The malpractice mess"
The Berkshire Eagle - Editorial, Wednesday, November 19, 2008
A Massachusetts Medical Society report released Monday asserting that defensive medicine on the part of physicians fearing lawsuits is adding a shocking $1.4 billion to annual health care costs in the state is the latest argument for malpractice reform. It is needed on a national basis, but there are ways that Massachusetts can address this problem on its own.
According to the MMS, 83 percent of physicians surveyed said they practiced defensive medicine, resulting in an average of 18 percent of tests (such as CT scans and MRI studies), procedures, referrals and consultations, and 13 percent of hospitalizations, which were ordered to avoid potential lawsuits. Given the advanced technology available, patients will demand tests that doctors believe are unnecessary but will agree to because of the fear of lawsuits.
The high cost of malpractice insurance is helping drive the shortage of primary care physicians and obstetrician-gynecologists plaguing the Berkshires. Forty percent of malpractice lawsuits are groundless, according to a Harvard School of Public Health study, and these high insurance rates can at least be partially addressed by placing a cap on damages and retooling a scale for fees so lawyers won't be walking away with millions of dollars when verdicts come down. Malpractice suits could drop in number if doctors and hospitals are encouraged to acknowledge errors and engage in compensation offers.
This would have benefits for patients and families, who would gain closure and avoid high legal costs, and legislation will be introduced on Beacon Hill next year to offer grants to hospitals that institute a pilot program applying this approach.
The malpractice system adversely affects doctors, patients, hospitals and the state as a whole. All parties have an interest in fixing it.
--------------------
North Adams, Massachusetts
"Tapestry Health closes 2 offices"
By Jennifer Huberdeau, New England Newspapers: The North Adams Transcript & The Berkshire Eagle, Friday, April 3, 2009
NORTH ADAMS — The state-funded family planning agency, Tapestry Health Systems, has closed its North Adams and Great Barrington offices and is directing clients to its Pittsfield location.
A clinic in Athol closed, too — the result of mid-year cuts made by Gov. Deval Patrick in October.
"We chose to close the clinics in North Adams, Athol and Great Barrington because those are our smaller sites," Suzanne Smith, Tapestry's director of health services, said Thursday. "Our Great Barrington and North Adams offices had already been scaled back to one day a week."
Smith said the agency weighed the cost of keeping the offices open versus keeping its services and larger clinics intact.
The Pittsfield office, which is open five days a week, handled 2,200 office visits last year — about 1,000 individuals. The North Adams office had about 220 clients, and the Great Barrington office had about 100 clients.
The closures did not result in any staffing cuts, since the sites already shared the Pittsfield office's staff, which includes a nurse practitioner, a health services manager, two family planning counselors and an office manager.
"We've sent out postcards to people about having to move our staffing hours to the Pittsfield office," Smith said. "The postcards also provided our clients with information about who they should contact in the Legislature to ask to restore our funding.
"We hope in the future, if funding is restored, to return our office to North Adams."
Beginning July 1, the governor has recommended cutting state support for Tapestry Health Systems, which serves all of Western Massachusetts, by about $599,610. The state money supports low-cost or free sexually transmitted infection testing, breast and cervical cancer annual testing, HIV testing and counseling, pregnancy testing, access to emergency contraception and access to birth control.
"We've been underfunded for quite some time," Smith said. "Our state subsidized services, funded by the Department of Public Health, will most likely run out by the end of this month."
While the agency is often perceived as serving only teenagers and college students, she said a vast majority of clients are under insured or uninsured men and women seeking exams and counseling. She said the agency does not perform abortions, but offers "options counseling" that makes prenatal care provider referrals, abortion referrals and offers adoption agency contact information.
In addition to closing the three offices, the agency has also relocated its administrative offices to a "less expensive" location, curtailed travel and has not filled vacancies, she said. The agency also has increased its private fundraising efforts.
"We're doing everything we can," Smith said.
-
www.topix.net/forum/source/berkshire-eagle/TC8HG0MF0HIU8454J
-
--------------------
"Varying reviews for primary care in county"
By Jack Dew, Berkshire Eagle Staff, Sunday, April 5, 2009
A new report on the quality of primary care in Massachusetts paints an uneven picture of Berkshire County medical groups, showing them among the very best in the country in some areas and, in others, lagging their peers in the state and the nation.
The Massachusetts Health Quality Partners gathered information from insurers about primary-care medical groups and then crunched the numbers to determine whether patients are given the health screens they need for such diseases as colon and breast cancer, or the best treatment for chronic conditions like asthma and diabetes. The full results are available at mhqp.org.
The Health Quality Partners — which includes insurance companies, the Massachusetts Hospital Association, the Massachusetts Medical Society and state health agencies — compared the medical groups' numbers to the national average, the state average, and the top 10 percent of medical groups nationwide. For some measurements, they also created their own benchmark: how the top 25 percent of medical groups in the state performed the prior year.
The medical groups were then given up to five stars for exceeding all the benchmarks or as few as one star for exceeding none.
The 10 medical groups in Berkshire County that were covered by the report received four or five stars 41 percent of the time, meaning they exceeded three or four benchmarks, putting them among the best in the state and the nation.
But 48 percent of the time, the groups received one or two stars, having failed to meet any benchmarks or only one.
Statewide, Massachusetts physicians performed better than the national average on 28 of 30 quality-of-care measurements and were in the top 10 percent on 14 of 30 measures.
The group has been compiling its report for five years, part of an increasing effort in the state to shed light on health care quality. It is both an attempt to help patients make informed choices about where they seek care and to encourage doctors to improve their performance.
"When patients make decisions, they are using a range of information, including referrals from friends and family," said Barbara Lambiaso, spokeswoman for the partners. "This is just another piece of information that can help."
Dr. Gray Ellrodt, medical director at Berkshire Medical Center, said the goal for the hospital and the three medical groups under the umbrella of BMC's corporate parent is to "be at the top of the very high bar" that is set by Massachusetts doctors. He said they will look to the report for areas where they can improve.
But it is less clear how patients will use the information. While the star ratings create the appearance of simplicity, what they actually mean is not always easy to divine. That comprehension gap is typical of efforts to assess health care quality, where nuanced medical decisions are rated with blunt tools like star rankings.
"There is a huge challenge on the part of all organizations to make these reports as understandable and accessible as possible," said Deb Wachenheim, health quality manager for Health Care for All, a statewide advocacy group. "If you get too much into the nitty-gritty, it can be too hard to explain what it means in a broader sense. The key is trying to hit that balance."
-
To reach Jack Dew: jdew@berkshireeagle.com (413) 496-6241
-
www.topix.net/forum/source/berkshire-eagle/TC6QFM9TTNFHP5GNL
-
--------------------
"'Correct' test is unfair to doctors"
The Berkshire Eagle, Letters, Tuesday, April 7, 2009
Jack Dew's April 5 article on Berkshire County doctors identified some apparent wide fluctuations in quality of performance. As a member of Berkshire Medical Group, I am very proud that my group received the highest possible ranking on colon cancer screening.
It is therefore all the more disturbing to see that we received a poor ranking in "Performing the Correct Imaging Test" for back pain. According to the criteria used by the Massachusetts Health Quality Partners, the only "Correct Imaging Test" for back pain is no test in the first 28 days after seeing the doctor. As a result, a physician will receive a bad score on this measure if he sees and evaluates his patients with back pain and does any X-ray or other imaging study.
The title "Performing the Correct Imaging Test" is misleading and is a misrepresentation of quality and skill. This measure should either be abandoned or should be renamed to avoid the implication that good doctors are choosing an incorrect test.
HARRY HARTFORD, M.D.
Richmond, Massachusetts
-
www.topix.net/forum/source/berkshire-eagle/T96MKNL24HQALJOKO
-
READER's link to story:
www.bloomberg.com/apps/news?pid=20670001&refer=columnist_mccaughey&sid=aLzfDxfbwhzs
-
--------------------
-

-
Alejandro Perez, above and below, takes an eye exam at Volunteers in Medicine in Great Barrington. The test is being administered by Janina Sulca, who serves as an interpreter at the clinic. (Photos by Ben Garver / Berkshire Eagle Staff)
-
"Health care on the fringe: Panel tackles solutions for immigrants"
By Jack Dew, Berkshire Eagle Staff, Thursday, May 14, 2009
Despite a health care reform effort that has given Massachusetts the highest rate of insured adults in the country, a population of immigrants remains on the edges, getting neither the care nor the coverage they need.
Estimates peg the Berkshire County immigrant population at roughly 12,000 people. That group comprises all manner of legal status — undocumented aliens, people with green cards, those with work or tourist visas. The health insurance system treats each group differently, and the regulations can be a dizzying mix of state and federal rules.
No one knows precisely how many immigrants in the Berkshires lack insurance coverage and how many fail to get basic medical care, but experts agree that the numbers are large and growing, even as the percentage of uninsured adults overall is shrinking.
Some agencies and social service organizations have stepped in to deliver care and try to pair immigrants with coverage. A handful of these groups will discuss the problems and some solutions next Thursday in a panel discussion sponsored by the Cross Cultural Action Network.
"It is a growing issue in the Berkshires," said Claudine Chavanne, a community planner for the Adult Learning Center who helped organize the discussion. "We've had such a surge in the last couple of years of immigrants in Berkshire County, and many are in the labor force. But the lack of immigration reform and the recession have put exceptional pressure on immigrants and all minority groups, so access to health care has become an increasing challenge."
Groups like Advocacy for Access — with offices at Berkshire Medical Center in Pittsfield and Fairview Hospital in Great Barrington, and Ecu-Health Care at North Adams Regional Hospital have tried to help anyone who qualifies for health insurance get enrolled.
Others, like Volunteers in Medicine in Great Barrington and Community Health Programs in Great Barrington and Pittsfield are delivering care at no or reduced cost. Often the missions overlap — those who seek cheap care get help enrolling in health plans.
"A lot of the immigrant population is not familiar with the process of accessing health care in this area," said Arthur Peisner, of Volunteers in Medicine, which offers free care from volunteer doctors, dentists and mental health providers. "Often, their only approach is to go to the emergency room. They don't, as a general rule, have a primary care physician, and certainly a large percentage is uninsured."
While some immigrants qualify for subsidized insurance through programs like Medicaid and the state's Commonwealth Care plans, undocumented immigrants usually do not.
They must rely on a patchwork of programs like Volunteers in Medicine that provide care to the needy, regardless of immigration status. Many, however, never seek care at all, waiting for a catastrophe that takes them to the emergency room where they are covered by the Health Safety Net, a pool of cash that is filled by the state, hospitals and insurance companies.
One of the goals of health care reform was to reduce demand on that fund by helping more people get insurance. Peisner said he hopes that formula will someday include immigrants, closing a large gap in the new system.
Politically, however, there is little momentum behind expanding health care to cover non-citizens, particularly those in the country illegally. Those who work in the field say there is very little state or federal money to help this group.
At the Berkshire Immigrant Center, co-director Brooke Mead said the Berkshires have "done an outstanding job of trying to provide some options for (immigrants without health coverage) because we place a lot of value on our community members and being strong, healthy and welcoming communities."
Mead said she hopes the upcoming panel discussion will strengthen those efforts, letting the agencies talk to the public and among themselves.
-
To reach Jack Dew: jdew@berkshireeagle.com; (413) 496-6241.
-
www.topix.net/forum/source/berkshire-eagle/T5EBH8CTTR8762V2U
-
--------------------
"Reps seek change in payment system"
By Trevor Jones, Berkshire Eagle Staff, Sunday, December 13, 2009
PITTSFIELD -- In order to sustain health insurance reforms that have opened access to nearly 98 percent of the state's residents, "seismic" changes to the health payment system have to begin within the next year, according to one state representative.
"It's not a five-year process," said State Rep. Harriett L. Stanley, D-Essex. "It's probably going to take 20 years to turn it around, but if we don't get started and we don't get started soon we can't sustain what we did in 2006."
Those comments were made during a meeting with The Eagle editorial board on Friday, as Stanley, State Rep. William "Smitty" Pignatelli, D-Lenox, and Eugene Dellea, president of Fairview Hospital in Great Barrington, made their case for payment reform.
Nearly 98 percent of all residents in the commonwealth have health insurance thanks to state reforms enacted in 2006, but those reforms have done little to curb costs, as the per capita costs of insurance for residents is projected to grow faster than the nation average in the coming years.
Stanley served on the state's Special Commission on the Health Care Payment System and said changes need to be made in all facets of the health care system, including patient accountability, government regulation and equity in payment models.
"Everybody is going to have to change a little bit and it's going to take a while, but if we don't get started in 12 months, I don't know that we can catch up," said Stanley.
Dellea said the problem for Critical Access Hospitals like Fairview is the disproportionate payment system for services.
"What these major medical centers do, is they do all the soft stuff where they make some extra money and they get paid a lot more," said Dellea. "We can set an ankle as good as anybody else. We're measured at the same quality level but were paid differently."
Stanley said it's irrational that simple procedures like setting an ankle cost five times more in other parts of the state, and that difference will eventually be detrimental to existing rural hospitals.
"If we keep allowing the imbalance of the system, you're going to basically let community hospitals die on the vine and everything is going to be Boston or a branch of a Boston hospital," said Stanley.
Another major recommendation of the commission centered on a transition from a fee-for-service system to a global payment system, in which efficiency and quality is incentivized.
Part of that payment restructuring, the trio said, will include a need to incentivize primary care positions, and decreasing dependence on trips to the emergency room.
Pignatelli said there is currently a shortage of 60 primary care doctors in Berkshire County, a dearth of which gets in the way of preventative measures and leads to greater problems down the road.
-
To reach Trevor Jones: (413) 528-3660 or tjones@berkshireagle.com.
-
www.topix.net/forum/source/berkshire-eagle/T99E814TBTMO38RV3
-
--------------------
"State Health Care Reform: Huge pay variations found
By Trevor Jones, Berkshire Eagle Staff, January 30, 2010
The amount of money Massachusetts health insurers pay to hospitals and doctors is not directly correlated to the quality of care patients receive, and some hospitals and doctors are paid 200 times more than other providers in the state for the same kinds of services, according to a preliminary report released by the Attorney General's Office on Friday.
The report -- titled the "Investigation of Health Care Costs, Trends and Cost Drivers" -- found that current contracting practices with the state's health insurance companies have resulted in significant differences in compensation rates among hospitals and physicians. Larger or more geographically isolated hospitals have the leverage to negotiate to receive higher reimbursements than others. In addition, the higher payments are evidently not connected to the quality of care or the amount of treatment provided.
"This is the step that we needed to take to move forward with health care reform and cost containment," said state Attorney General Martha Coakley in a phone interview with the Eagle.
Coakley cited the need for greater equity for providers in areas outside of greater Boston, including Berkshire County.
The analysis focused on contracting practices and contract prices -- negotiated prices between providers and insurers for physicians for inpatient and outpatient care, and professional services -- for commercial health insurance between 2004 and 2008.
Coakley called the report a "baseline" regarding the "dysfunctions" in the current system, and that "all of the work that needs to happen now has to be based on this data."
Larger hospitals have more leverage in reimbursements negotiations, the report says, because insurers need to maintain large and stable networks. Other leveraging factors include niche providers, brand-name recognition and geographic location: some hospitals garner better deals because insurers need to maintain a presence in an isolated region with little health care competition.
David Morales, commissioner of the state Division of Health Care Finance and Policy, said the report provides data that needs to be examined further to see which providers are taking certain advantage of things like a lack of regional competition. Morales did not specifically mention any local hospitals but added that in Berkshire County, "If you had more competition, [prices] would be much lower."
It is unclear where Berkshire County's three hospitals fall in the cost spectrum, as no hospitals or physician groups were named in the report. Organizations' names were not released, Coakley said, due to the preliminary nature of the report, and because it was not intended to be an indictment of any particular provider.
Further details on specific institutions are expected to be released when a final analysis is presented as part of a state hearing on health care costs scheduled to begin on March 16 (2010).
Representatives for Northern Berkshire Health Systems, which operates North Adams Regional Hospital, and Berkshire Health Systems, the parent company for Berkshire Medical Center in Pittsfield and Fairview Hospital in Great Barrington, were not immediately available for comment on this story.
The report, which came about from a legislative mandate for Coakley to investigate health care cost trends and cost drivers and has taken nearly a year to produce, is the result of dozens of interviews, and review of thousands of contract documents, and detailed cost and quality data over the past year.
Among hospitals and doctors providing similar services, the price has no correlation to quality of care, sickness or complexity of care of those patients served, the extent to which a provider is responsible for patients on government-subsidized insurance, or whether a provider is a teaching or community hospital.
Also, the state's disproportionate share hospitals, those with 63 percent or more of their patients' charges attributed to government-subsidized insurance, receive on average payments that are 10 to 25 percent lower than those at non-DSH medical centers.
Berkshire Medical Center is among the state's disproportionate share hospitals.
And as health care costs continue to rise in the state at a rate higher than the national average, roughly 75 percent of the increases between 2006 and 2009 can be attributed to price increases, not use.
Meanwhile, one of the proposals to stem the rising costs -- a proposal by a state-appointed committee which calls for a shift from a fee-for-service system to a global payment system -- could also come under fire from information provided in the analysis.
Global payment systems may provide better integration of care, the report finds. As of now, the analysis does not show that a global payment system would definitely reduce costs more than a fee-for-service system.
Coakley and Morales said they both support the shift toward global payment systems. Coakley said it needs to be part of a series of changes that have to take place, and Morales said the framework for the incentives of a global system still does not exist.
-
To reach Trevor Jones: tjones@berkshireeagle.com, or (413) 528-3660.
-
www.topix.net/forum/source/berkshire-eagle/TD5LFFH9HL8BG3HCL
-
--------------------
"One in four Berkshire moms not getting prenatal care"
By Anthony Fyden, iBerkshires.com - February, 23 2006
In stark contrast to other Massachusetts communities, fewer than 75 percent of Berkshire mothers received adequate prenatal care in 2004, according to a new statewide report. That means that at least one in every four pregnant women failed to get the care needed to safely deliver healthy babies.
From a statewide perspective, the Massachusetts Births 2004 report, released on Wednesday, held some good news, including that the state's teen birth rate reached an all-time low. In fact, the teen birth rate of 22.2 births per 1,000 women ages 15-19 was 46 percent lower than the national rate. (The teen birth rate for Berkshire County was 25.8 percent).
Also, smoking rates during pregnancy reached an all time low statewide, 7.4 percent, 28 percent below the national rate. And in 2004, Massachusetts had the second lowest Infant Mortality Rate in its history: 4.7 infant deaths per 1,000 live births.
But the report raised some startling red flags for Berkshire County, particularly in the area of prenatal care. The report noted "less than 75 percent of mothers received adequate prenatal care in the Community Health Network of Berkshire County.”
In contrast, over 90 percent of mothers living within the Beverly/Gloucester health network received adequate prenatal care.
In Pittsfield, only 69.4 percent of mothers received adequate prenatal care, compared to over 90 percent of mothers living in Brookline and Arlington.
Pittsfield's Berkshire Medical Center (64.6 percent) was among facilities with the lowest reported rate of adequacy of prenatal care among mothers delivering in 2004. Other hospitals in this category were Boston Medical Center (53.9 percent), Tobey Hospital (62.8 percent), Lowell General Hospital (64.5 percent).
The hospitals with the highest rates of prenatal care included Beverly Hospital (93.3 percent), Saint Vincent Hospital (94.8 percent), Beth Israel Deaconess Medical Center (95.1 percent), and Brigham and Women's Hospital (98.1 percent).
According to a summary issued to the press, other key findings of the report include:
"In 2004, there was a 2 percent decrease in the number of births statewide. The number of births has decreased by 15 percent from 92,461 births in 1990 to 78,460 in 2004.
"The percentage of low birth weight infants (LBW) (less than 2,500 grams or 5.5 pounds) was 7.8 percent, the highest rate ever, although it is 4 percent below the national rate. Two important factors that account for this increase are the ages of mothers giving birth and the increase in multiple births.
"Older women are more likely to deliver LBW infants. The average age of a woman giving birth in Massachusetts is increasing. In 1980, about 1 in 4 births was to a woman aged 30 or older. In 2004, 56 percent of women giving birth were 30 years or older.
"Multiple births accounted for more than one half of the increase of low birth weight since 1990. The percentage of multiple births remained high in 2004. In 2004, 1 out of 21 births was a multiple birth. In 1990 1 out of 38 births was a multiple birth.
"Teen birth rates were highest in Lawrence (79.4 per 1,000 women ages 15- 19), Holyoke (76.0) and Springfield (70.9).
"Disparities in birth outcomes continue. The Black non-Hispanic IMR is 3 times that of white non-Hispanics (11.4 verses 3.8).
"The report in its entirety is available at www.mass.gov/dph/pubstats.htm . The data is also available through MassCHIP at www.masschip.state.ma.us."
--------------------
"Study: Berkshire low on Massachusetts healthy counties list"
Associated Press, Feb. 18, 2010
BOSTON (AP) -- A new study finds the healthiest counties in Massachusetts are clustered in the eastern part of the state.
The report found that Nantucket, Dukes, Middlesex and Norfolk are among the healthiest, while Berkshire and Hampden are among the least healthy. Berkshire County is ranked 11 out of 14.
Suffolk County, which includes Boston, came in second to last.
The study by the University of Wisconsin Population Health Institute and the Robert Wood Johnson Foundation looked at every county in the country and ranked them in order of health based on a series of factors.
Those factors include the rate of people dying before age 75, the rate of low-birthweight infants, adult smoking rates, teenage pregnancy and obesity, and the number of uninsured adults.
------
On the Net:
County Health Rankings: www.countyhealthrankings.org
------
"Berkshire County not so healthy"
By Dick Lindsay, New England Newspapers: The Berkshire Eagle & The North Adams Transcript, 2/19/2010
While Berkshire County is tops in providing health care in Massachusetts, it ranks toward the bottom in residents staying healthy, according to a private, national study.
The County Health Rankings report released this week compared all 14 counties and found the Berkshires was first in clinical care but ranked 11th both in socio-economic factors and health behaviors -- such as smoking, drinking and eating -- and 12th in environmental factors. Overall, the county ranked 8th when the four categories are combined under the heading of health factors.
Furthermore, the county ranked 11th in health outcomes, which include premature death and the general mental and physical well-being of residents.
The first-of-its-kind study, co-authored by the University of Wisconsin and the New Jersey-based Robert Wood Johnson Foundation, also compared counties within each of the other 49 states. The Massachusetts portion has received mixed reviews from local public health officials.
"I'm not surprised by the study," said Sandra Martin, senior emergency planner for the Berkshire County Boards of Health Association. "We have more teens smoking and getting pregnant, per capita, than the rest of the state."
Martin noted rural areas usually score lower than urban areas on such surveys because most rural communities have small boards of health with no professional staff trained to promote wellness.
A countywide agency -- possibly her organization -- is needed to coordinate existing efforts to improve residents' health, she said.
"It's a huge gap and we're trying to fill that," Martin said.
North Adams Regional Hospital officials also found the study seems to reflect the Berkshires' current health status. Spokesman Paul Hopkins said all three area hospitals -- the other two being Berkshire Medical Center and Fairview Hospital -- spend plenty of time improving the quality of care. However, he noted Northern Berkshire has among the highest smoking rates in the state.
"We can provide the best health care possible," Hopkins said, "but it does no good if certain lifestyles point people in another direction."
Pittsfield Health Department Director James J. Wilusz said he "didn't realize Berkshire County ranked so low." He cited how the county's three hospitals provide wellness programs designed to help people stop smoking, eat better and exercise.
Since the study relied on data as far back as 2005, Wilusz said, "You have to be careful how you [interpret] these numbers."
Nevertheless, Wilusz agreed with Martin that public health officials must be more proactive in promoting a healthy lifestyle.
"As we progress, hopefully we'll improve our ranking," he said.
-
www.topix.net/forum/source/north-adams-transcript/T72E0QTV1I0T2LU3U
-
--------------------
"Running out of doctors"
The Berkshire Eagle, Editorial, October 21, 2010
The physician shortage in Massachusetts and Berkshire County revealed by the Massachusetts Medical Society's latest study isn't new but the extent of that shortage is increasingly alarming. The scarcity of physicians, in particular primary care physicians, in the Berkshires is equivalent to a skin lesion that has gone unaddressed until it has metastasized into cancer. The longer this problem festers, the more difficult it will be to resolve.
The findings of the 2010 Physician Workforce Study are essentially the same as in past years but the problems keep increasing in magnitude. Not only do there continue to be inadequate numbers of primary care physicians, this situation has expanded into specialty fields like dermatology and urology. If Berkshire residents have to travel elsewhere for medical help they will have to pay more out of pocket for going outside their "network," which in turn contributes to increasing medical costs everywhere. This poses a particularly severe strain upon Berkshire County's largely rural, elderly population.
The Berkshires' small, spread-out population may make it difficult to attract doctors, but that is only one component of a more complex problem. In the case of primary care physicians, they are undervalued and disproportionately underpaid, which encourages medical students to go into specialties, further fueling the shortage. Primary care doctors, who make up the front line of defense against disease, are needed to address issues like obesity, high blood pressure and diabetes before they evolve into serious problems that are more costly to treat.
Primary care physicians and their colleagues in the specialties share the frustration of being overburdened with paperwork from the health insurance companies that defy and undermine all efforts at reform. They are also swamped by the high cost of malpractice insurance, a product of our overly litigious society.
When half of the primary care physicians surveyed, many nearing retirement age, are not accepting new patients, the system is in critical condition. That Lee Family Practice has been unable to recruit a new physician since 1999, largely because it cannot offer a high enough salary, is nightmarish. State government can help to a degree by offering incentives to doctors to work in rural areas and to go into the primary care field, reducing the disparity in pay. But the headaches generated for doctors by the health care bureaucracy is a national issue, and as we have learned over the past two years, health care issues are apparently intractable at the federal level, where partisan politics makes real reform impossible.
-
http://disqus.com/forums/theberkshireeagle/running_out_of_doctors_berkshire_eagle_online/trackback/
-
---------------
"Doctor shortage 'critical' in Berkshire County"
By Amanda Korman, New England Newspapers: The Berkshire Eagle & The North Adams Transcript, 10/20/2010
PITTSFIELD - Physician shortages across the state continue, which means medical practices face a tough recruitment environment and patients encounter more barriers to seeing a doctor, a new study says. The shortages are among the state's most severe in Berkshire County, where the lack of physicians was deemed "critical" by the report's authors.
One of the central findings of the 2010 Physician Workforce Study, completed annually since 2002 by the Massachusetts Medical Society, is that the primary care fields of family medicine and internal medicine are in their fifth consecutive year of paucity across the state. Additionally, every region except for Boston is operating with physician shortages, and Berkshire and Worcester counties are facing "extraordinarily stressed conditions."
"The findings from this latest analysis clearly show how fragile access to care for patients is across the entire commonwealth," said Dr. Alice Coombs, president of the Massachusetts Medical Society, in a news release.
The scarcity has expanded into new specialty fields: Ten of 18 specialties were found to have shortages, three more than last year.
One telling statistic regarding the terrain in Berkshire County is the amount of physicians who reported dealing with an inadequate pool of physicians in the six tightest specialties (dermatology, family practice, internal medicine, neurology, urology and vascular surgery): Ninety-four percent in Berkshire County said there was an inadequate pool, compared to a 77 percent average statewide.
New patients searching for a family or internal medicine practitioner are also continuing to come up against roadblocks: The study found that approximately half of primary care physicians are not accepting new patients.
Lisa Trumble, vice president for physician services for Berkshire Health Systems, has been in physician recruitment for a number of years and has seen the landscape become tougher.
"Over the last few years, physician recruitment has become more difficult and competitive," she said. "Part of what's presenting an issue is the trend of physicians going into more procedural specialties than cognitive specialties," such as primary care.
The problem is all too familiar to Dr. Michael Kaplan, a family medicine physician at Lee Family Practice. He said that he and his partner, Dr. Melanie Levitan, have not been able to successfully recruit a new physician since their practice was incorporated in 1999.
Kaplan said that the infrastructure for reimbursing doctors for primary care means his small practice has little chance of offering a competitive salary to a candidate for hire.
"It isn't all about money, but an awful lot of it is about reimbursement," he said. "At our current level of reimbursement, it's just about impossible to recruit new people."
Both Kaplan and Levitan are in the second half of their working careers, Kaplan said, and although it's not yet of pressing concern, he is well aware that if they can't eventually bring in any younger physicians, their practice will not survive.
By the numbers ...
A sampling of additional findings from the 2010 Massachusetts Medical Society Physicians Workforce study:
Fear of being sued: Forty-six percent of practicing physicians surveyed said their practice has been altered or limited because of the fear of being sued, the same percentage as last year.
Satisfaction: For the first time, a slightly higher percentage (43) of physicians reported satisfaction with the practice environment compared to those who were dissatisfied (41).
Wait times: For internal medicine, the average wait time increased to 53 days, the highest it has been in six years. For family medicine, the average wait time is 29 days, shorter than last year's figure of 44 days.
Administrative tasks: More than half of physicians (51 percent) expressed displeasure with the tradeoff between caring for patients and administrative tasks.
--------------------
"Tobacco prevention funds go up in smoke"
By Amanda Korman, Berkshire Eagle Staff, December 4, 2010
PITTSFIELD -- Massachusetts ranks 37th in the nation when it comes to funding anti-tobacco efforts, and tobacco control specialists in Berkshire County -- where the smoking rate is above the statewide average -- say the state's financial strain is impacting smoking cessation and prevention efforts.
"This is the life we live now," said Joan Rubel, project coordinator of the Northern Berkshire Tobacco-Free Community Partnership at Berkshire AHEC. "I think what's in place in the state is an infrastructure at a very low level of tobacco cessation and prevention work."
At North Adams Regional Hospital's REACH for Community Health tobacco treatment program, the last state grant expired in June. To stay afloat, the program is depending on one in-house grant that will not last through 2011, said Linda Thomas, REACH's tobacco treatment specialist. REACH is seeking other grants for future funding.
"This is the only treatment program in this area, so if it were cut, who's going to provide the service?" Thomas said.
Smoking rates in North Adams are among the highest in the state at 30 percent, according to 2008 figures from the state Department of Health. The statewide average is 15 percent according to 2010 national statistics.
The nationwide rankings of tobacco control funding among the 50 states were compiled by the Campaign for Tobacco-Free Kids, the American Cancer Society and other health care groups. The measures included programs that keep kids away from tobacco and help smokers quit. Released in November, the report points to the frustration among tobacco control advocates that so little money from the 1998 tobacco settlement and tobacco taxes goes toward prevention.
Massachusetts will receive $821 million through these tobacco-related funds this year, and spend only 0.5 percent of that -- $4.5 million -- on prevention and cessation.
"A large amount of money is coming into the state, but it's not going to fund tobacco prevention work," Rubel said.
Recent budget cuts have eliminated several state programs aimed at preventing youths from using tobacco, according to state Department of Public Health spokeswoman Julia Hurley.
State programs to help pregnant women quit smoking are gone, Hurley said, as is the state tobacco control program's advertising budget. The cuts also forced reductions in the Massachusetts Smokers' Helpline hours.
Tobacco companies have also developed new ways of selling tobacco: Thomas said smokeless tobacco has become more popular among teens, who manage to get unsuspecting parents to buy it for them because, based on its packaging, they believe it's gum.
Berkshire Medical Center's tobacco cessation program director Carol McMahon said that youth tobacco use has become a larger problem because anti-tobacco marketing funds have been slashed.
State funding for BMC's program fell through in 2001, McMahon said, and the hospital has since been supporting the program. This past year, a 32-hour position was cut.
"That only leaves one full-time equivalent and one 16-hour [position], which is nowhere near enough to address the tobacco problems in Central Berkshire," McMahon said.
Pittsfield's smoking rate is 26 percent, according to 2008 statistics from the DPH. McMahon said she sees an average of 800 people each year who are trying to quit.
-
http://disqus.com/forums/theberkshireeagle/thread_104/trackback/
-
--------------------

Dr. Andrew Schamess, a primary care physician in Lenox, called the report a 'wake-up call.' (Patrick Dodson / Berkshire Eagle Staff)
"Unhealthy report card"
By Clarence Fanto, Berkshire Eagle Staff, April 5, 2011
PITTSFIELD -- Despite a strong showing in health care quality and availability, Berkshire County is third from the bottom out of 14 statewide in a study comparing healthiest to least-healthy counties.
The 2011 County-by-County Health Rankings released by the University of Wisconsin's Population Health Institute is based on data compiled by the National Center for Health Statistics and the National Center for Vital Statistics.
According to Angela Russell, associate researcher at the university's institute, key factors in Berkshire County's low ranking include the percentage of people in poor or fair physical and/or mental health, the rate of people who die before reaching 75, teen pregnancy rates, low-weight newborns, single-parent homes, children in poverty, obesity, smoking and binge drinking.
"You're among the least healthy counties in Massachusetts, for sure," said Russell in a telephone interview from Madison, Wis.
She also listed limited access to affordable healthy food -- "much lower than the rest of the state and the nation" -- and lack of gyms and fitness clubs in parts of the county.
But there's an important silver lining.
"You're really doing well in clinical care -- No. 1 in the state -- with good access to primary care providers, a great percentage of diabetes and mammography screenings and a low number of uninsured people," said Russell.
Dr. Andrew Schamess, a primary care physician at his Lenox Internal Medicine practice, credited Berkshire Medical Center for "a superb job so we really do have good outcomes in hospital-based clinical care.
"For a small rural county, we attract good physicians, though there's still a shortage for primary care," he added.
But a lack of pedestrian walkways is a problem in some areas, as well as little time for healthy recreation by hard-working families, Schamess pointed out.
Schamess termed the report "a wake-up call."
"We have this image of the Berkshires as a healthy, outdoorsy place for robust New Englanders, but the study shows us the reality is somewhat different, so we can't sweep it under the rug. There are some social needs that deserve greater attention."
At Berkshire Health Systems, Roberta "Bobbie" Orsi, a registered nurse and the program director for Wellness at Work who also oversees community health outreach, asserted that "we beat our scores from last year and it shows a consistent effort to get people access to insurance and health care."
"Where you live and work really matters," Orsi said. "Outside the doctors' offices and hospital walls, you have to look at behaviors, the socio-economic world and the environment.
"We've worked hard to try to achieve a level of top-qualityhealth care providers since access to health insurance alone isn't enough. A strong physicians' network is needed."
Orsi listed outreach efforts by the Berkshire VNA and the WIC (Women, Infants and Children's) Program as crucial to improving access to health care.
"It's well-known that health-care outcomes track very closely to poverty levels and individual income," said Dr. Charles Wohl, site director for the CHP-Neighborhood Health Center at 510 North St. in Pittsfield. He pointed to the countywide network of Community Health Program facilities and 30 resident physicians at BMC as positives.
But Wohl cautioned that some patients can't afford prescribed medications or lack access to specialists. The county's Medical Home pilot program is a prime example of a comprehensive effort involving nurse-practitioners, dietitians and substance abuse counselors assisting patients, he said.
The report is available at www.countyhealthrankings.org/Massachusetts.
Health rankings
Massachusetts counties, rated from most to least healthy.
1. Nantucket
2. Dukes (Martha's Vineyard)
3. Middlesex
4. Norfolk
5. Hampshire (Northampton area)
6. Barnstable (Cape Cod)
7. Essex
8. Franklin
9. Worcester
10. Plymouth
11. Berkshire
12. Bristol
13. Suffolk (Boston)
14. Hampden (Springfield area)
Source: University of Wisconsin Population Health Institute County-by-County Rankings, 2011
In an earlier version of this story, there was a discrepancy in the county's rank. Berkshire County is fourth from the bottom, not third.
--------------------
"County health study urges collaboration"
By Amanda Korman, Berkshire Eagle Staff, August 14, 2011
PITTSFIELD -- Health care leaders serving the poor need to better collaborate and "defragment" the services they offer, an analysis of the county’s public health found.
The study was conducted by five graduate students this summer in cooperation with the Berkshire Area Health Education Center.
"I was struck most by the recurring concept of fragmentation," said Kate Kelly, who is training as a nurse practitioner at the Yale School of Nursing. "Efforts and funding could be partnered, if people only knew what others were doing."
Using data from the national County Health Rankings, a group of students of nurse practitioning and dentistry spent six weeks analyzing five of the health outcomes in which the Berkshires fared the worst compared to the state as a whole: Motor-vehicle crash deaths, poor physical health days, access to healthy foods, single-parent households and teen births.
The students integrated these data, which are compiled by the Robert Wood Johnson Foundation and the University of Wisconsin, with interviews with area health and public safety leaders, who expanded on other additional health concerns including mental health, domestic violence and substance abuse.
Presenting their findings at Berkshire AHEC in Pittsfield on Friday, the students underscored the fact that poor health outcomes were always linked to socioeconomic status -- that poverty in the Berkshires drives undesirable health rankings.
At the same time, the students said, there are clearly a significant number of organizations and leaders devoted to solving these problems in the county.
"There’s a lot of work going on here -- a lot of human capital and good will," said Toy Lim of the UMass Graduate School of Nursing.
Citing existing community partnerships -- like Fairview Hospital’s outreach work with nutrition programs -- the students suggested that many other organizations would do well to find creative ways to work together to tackle these broad social and health issues.
Tim Diehl, executive director of Berkshire AHEC, agreed that services were often splintered throughout the county.
"A lot of the fragmentation, regretfully, happens around North versus South counties, Pittsfield versus North Adams," Diehl said. "We tend in the Berkshires, because it’s a large county, to be more focused around an area of the county rather than the county as a whole, so we tend not to think about ourselves in broader collaborations."
Another impediment, he said, is the fact that the little funding organizations rely on is tied with so many stipulated activities that there simply isn’t time to also figure out ways to collaborate.
To reach Amanda Korman: akorman@berkshireeagle.com (413) 496-6243
--------------------
"Lack of doctors is still a concern"
By Amanda Korman, Berkshire Eagle Staff, October 3, 2011
PITTSFIELD -- A shortage of primary care and certain specialist doctors persists in Berkshire County, according to a new study, although local health officials say the situation is less grim than the study's rhetoric might suggest.
The Massachusetts Medical Society's 2011 Physician Workforce Study findings illustrate that the county's "critical shortages" of medical professionals is rooted in part in the difficulty of filling vacancies and retaining staff, according to the report.
The study showed that fewer than half of the internists and family medicine physicians in Massachusetts are accepting new patients, confirming the experience of local doctors whose practices are already stretched to their limit.
Dr. Anthony Smeglin, medical director of the Williamstown Medical Associates, said his practice receives requests "all the time" for new patients it doesn't have the staff to accommodate. The small team of doctors, nurse practitioners and physician assistants already manages about 12,500 patients.
"We have to say no," Smeglin said. "It's really across the whole area -- Southern Vermont, the Berkshires, the upstate eastern border area of New York -- it's a really bad shortage of primary care and other specialists."
Officials at Berkshire Health Systems, who said they have been aware of and working to address the physician shortage since 2003, noted that many of the issue's roots go deeper than just the Berkshires.
"The overall issue of supply of physicians in Massachusetts and the country is going to be a community need that everyone's going to have to pay attention to," said Ruth Blodgett, BHS senior vice president of planning and development.
In areas outside of Boston, the report cited "severe" shortages in family medicine, general surgery, neurosurgery, dermatology and orthopedics. Internal medicine, psychiatry and urology were deemed "critical" in the report.
BHS consolidated several urology practices in the county several years ago, and while officials said there is still a need to recruit more urologists, they don't view the situation in the Berkshires as dire.
In other specialist areas, local health officials cited the use of mid-level providers like physician assistants and nurse practitioners in easing the physician supply problem.
"In primary care, I think that we have some needs down here, [but] not in the category of ‘critical' or ‘severe,'" said Dr. Brian Burke, medical director of Fairview Hospital in Great Barrington.
Nonetheless, he said, primary care is changing, and the shortage could become severe without oversight.
"We need to keep an eye on that," he said.
According to the report, 73 percent of physicians in the Berkshires reported that there was an inadequate pool of physicians to recruit from, compared to a state average of 52 percent.
"There's a lot of challenges to recruitment," said Smeglin of Williamstown Medical Associates. "We offer a lovely place to live and lifestyle, but it's hard to get that message out to people who are looking for jobs; they're so used to being in major medical centers."
The report's findings also demonstrate the continuing difficulties as the state tries to reform its health care system. A significant portion of physicians were dubious about payment reform initiatives being discussed in the Legislature, and half of all specialists and primary care doctors said that fear of being sued has caused them to limit or alter their practice.
To reach Amanda Korman: akorman@berkshireeagle.com (413) 496-6243
--------------------
"Failed status quo on doctor shortage"
The Berkshire Eagle, Editorial, October 5, 2011
The conclusions of the Massachusetts Medical Society’s 2011 Physician Workforce Study are not appreciably different than those of the 2010 study, and the status quo is not acceptable. With doctors retiring and practices unable to accept new patients, the shortage of primary care physicians and some specialists in Berkshire County will become a more severe problem the longer it goes unaddressed.
Statistical and anecdotal evidence attests to what the study refers to as "critical shortages" in the Berkshires. Fewer than half of the county’s primary care doctors are accepting new patients because they are already overwhelmed, and nearly three-quarters of those physicians report that there is an inadequate pool of incoming physicians to enable them to expand their practice. This is not only bad for the health of residents it contributes to the skyrocketing cost of health care. Primary care doctors constitute the front line of defense, and patients whose ills are not treated quickly develop more complex problems that are costlier to resolve.
Primary care doctors are undervalued and underpaid in comparison to specialists, which discourages physicians from entering the profession. In an editorial board meeting with The Eagle last spring, state Health and Human Services Director JudyAnn Bigby asserted that Governor Patrick’s health care reform proposal, centered around the end of the fee for service model of health care, would enable doctors to reduce the number of short appointments required to appease insurance companies. Ending this financial pressure could encourage more physicians to enter the primary care field. Malpractice reform continues to be desperately needed so doctors burdened with expensive insurance premiums won’t limit their practices or abandon the profession entirely.
The introduction of physician assistants and nurse practitioners have helped ease the problem, but as capable as they are, this is still a Band-Aid. The physician shortage must be resolved, and this will require rarely seen will and cooperation at the state and federal levels.
--------------------
"Still hard to find a doctor in Berkshire County"
By Clarence Fanto, Berkshire Eagle Staff, August 9, 2012
Confirming what many area residents already know from personal experience, the Massachusetts Medical Society's study of patient access to medical care offers dramatic evidence of Berkshire County's severe shortage of primary caregivers.
The data, gathered this past February through April and released on Wednesday, does not reflect recent or pending departure or scale-downs of nearly a dozen practices from North Adams to Great Barrington.
But it shows that while it's relatively easy and quick to see a pediatrician or certain medical specialists in the Berkshires, internists and family-medicine doctors are overbooked. Many doctors are not accepting new patients and those who do often exclude seniors on Med icare or residents on Mass Health (Medicaid) or state-subsidized Common wealth Care.
For example, all of the county's pediatricians, orthopedic surgeons and gastroenterologists were accepting new patients at the time of the survey. Among obstretricians-gynecologists, 86 percent were.
But only 57 percent of internists could take on new patients; among family-medicine physicians, 43 percent had open practices. Cardiologists were the only specialists very difficult to see: just 25 percent would accept new patients.
By comparison, in early 2011, 71 percent of family practitioners were taking on new patients, along with 57 percent of internists, the same as in 2012. Orthopedic surgeons and pediatricians all had open practices last year; figures were lower in 2011 for other specialties.
Waiting times to see a doctor are another hurdle for Berkshire patients seeking general care. In this year's survey, it took three months to get an appointment with an internist, and nearly a month to see a family practitioner or an OB-GYN.
For pediatricians, the average wait time was two weeks. Gastroenterologists required a wait of a month and a half. But heart specialists could see patients within several days and an appointment with an orthopedic surgeon could be booked within two weeks.
Another challenge for low- to moderate-income Berkshire residents: Fewer than half of fam ily doctors would see Mass Health clients, and only three out of 10 internists would. Among pediatricians, a paltry 13 percent accepted Mass Health youngsters earlier this year.
Lower reimbursement rates for federal-state MassHealth (Medicaid) insurance have been cited by child-care physicians as reasons for their policy.
On the other hand, all the specialists for adults accepted the government-subsidized insurance.
For seniors, the picture was brighter. Nearly three out of four internists would see Medicare patients, and just over half of family-medicine practices were willing to do so. Again, among the specialists surveyed, all accepted Medi care insurance.
The Massachusetts Medical Society's annual study painted a brighter portrait statewide, although two counties, neighboring Franklin and Barnstable on Cape Cod, faced even tougher problems than Berk shire County.
"Our latest research shows an improving picture of access to and satisfaction with health care in the Commonwealth," stated the society's president, Dr. Richard Aghababian. "While we continue to have shortages of physicians and average wait times for new patients for primary care are still longer than we'd like them to be, we are seeing more people getting care. And that's positive."
Availability of primary care improved only slightly this year compared to 2011 across the state, with nearly half of the practices still closed to new patients. The access changed only marginally over the past three years, according to the medical society.
Delays in obtaining appointments averaged 45 days for family medicine and internal medicine throughout Massa chu setts, with some improvement for internists but a dramatic increase in wait times for family doctors.
Wait times to see specialists were either stable or shorter, according to the study.
-----
Medical care snapshot ...
The following data shows the percentage of open medical practices in Berkshire County:
In 2012:
Cardiology 25%
Family medicine 43%
Internal medicine 57%
OB-GYN 86%
Pediatrics 100%
Gastroenterology 100%
Orthopedic surgery 100%
In 2011:
Cardiology 20%
Internal medicine 57%
Family medicine 71%
Gastroenterology 80%
OB-GYN 86%
Orthopedic surgery 100%
Pediatrics 100%
The following chart lists waiting times earlier this year for practices and the percentage accepting Medicare or MassHealth (Medicaid):
Cardiology 2 days Medicare 100% MassHealth 100%
Orthopedic surgery 10 days Medicare & MassHealth 100%
Pediatrics 13 days MassHealth 13%
Family medicine 25 days Medicare 57% MassHealth 43%
OB-GYN 26 days Medicare & MassHealth 100%
Gastroenterology 46 days Medicare & MassHealth 100%
Internal medicine 90 days Medicare 71% MassHealth 29%
Source: Massachusetts Medical Society, founded in 1781, located in Waltham and representing about 24,000 physicians and students. The study was based on 830 telephone interviews with physicians' offices statewide between Feb. 28 and April 2 this year.
--------------------
Our Opinion: "Dental care must be established early"
The Berkshire Eagle, Editorial, 4/10/2016
Dental care goes beyond teeth — it is critical to overall health. The Berkshires and state must do better, beginning with children.
In an April 6 letter to the editor, Drs. Steven and Louis Yarmosky and Lauren Bullinger of Yarmosky Pediatric Dentistry of Pittsfield and Great Barrington made the case for parents establishing a dental home for their children at the age of one. Citing an April 2 Eagle article on a dental care seminar for southern Vermont pediatricians and primary care doctors, the writers observed that when a child's teeth hurt it affects eating, sleeping and ability to learn.
In an April 6 report on dental care, the Massachusetts Health Policy Commission drew attention to a related issue, the high rate of dental care provided by emergency rooms. The report indicates that this could be partially attributed to gaps in MassHealth coverage, resulting in only 35 percent of dentists in 2014 treating a MassHealth patient. Emergency department treatment of a dental problem is four to seven times more costly than a dental office visit nationally, according to the report, which found that the Berkshires had the second highest rate of emergency visits for preventable dental conditions of any region in the state.
Parents must work with a medical professional to establish dental care for their children. Overall, the state must make it easier to get dental care, sparing people misery and saving the state money.
--------------------
“Pignatelli has plan to increase dental care access by creating mid-tier provider”
By Scott Stafford, The Berkshire Eagle, 4/19/2016
PITTSFIELD - Berkshire County residents end up at the emergency room for preventable dental treatments at the second-highest rate in the state, according to a recent report by the Health Policy Commission.
And many of those treatments, which are far more expensive than a typical dental visit, end up being billed to the state because the patients can't afford the cost.
"We have a real dental access problem in the Berkshires," said state Rep. William "Smitty" Pignatelli, D-Lenox, who has introduced legislation designed to make dental care more accessible by bolstering the number of dental providers. "This is especially troubling because taxpayers end up on the hook covering the costs of emergency care when we could have prevented the issue at a routine checkup."
According to data reported by the commission, between eight and 10 people per 1,000 of population end up in the ER for dental emergencies. Most of them are lower income, and most of them were children.
A visit to an emergency room for dental treatment can range from $400 to $1,500 per visit, which is four to seven times more than a dental office visit, which averages between $90 and $200.
The bill (S.2076 or H.2076), introduced by Pignatelli and state Sen. Harriette Chandler, D-Worcester, aims to address the problem by introducing a new level of dental practitioner. The House version was favorably reported out of the Joint Committee on Public Health and is currently in the Joint Committee on Health Care Finance.
Modeled after a Minnesota program, the bill calls for the addition of dental hygiene practitioners, who would be authorized to perform some of the more routine dental procedures currently only handled by dentists.
In order to become a dental hygiene practitioner, a dental hygienist would be required to earn the certification with two years of college courses and training. This would be a mid-level practitioner with more training and certifications than a dental hygienist, and would work under the guidance of a dentist.
"We need dental hygiene practitioners so that dentists can expand their capacity and treat families before they end up in the emergency room," Pignatelli said.
But some dentists say the plan doesn't address the real problem: reimbursement under MassHealth.
The state health care insurance plan is only reimbursing dentists for only 40 to 50 percent of the cost of treatment. Some dentists won't even see MassHealth patients because of low reimbursement rate. Others limit the number of MassHealth patients they'll see to minimize the financial sacrifice.
As a result, some MassHealth patients either can't find a dentist to treat them, or don't even try until an acute condition forces them to visit the emergency room.
Many dentists don't accept MassHealth dental patients because of the low reimbursement rate. Others limit the number of MassHealth patients they see. In 2014, 35 percent of dentists treated MassHealth patients and only 26 percent billed at least $10,000 to the program.
Pignatelli said it's not the fault of the dentists: "It is very difficult for a dentist to book patients when they're getting a reimbursement of only 40 cents on the dollar. That's the struggle we're in."
And while the political climate makes it an uphill battle to increase the reimbursement rates, in the meantime, giving dentists a tool to increase their revenue and see more MassHealth patients could buy some more time, Pignatelli said.
"What we've got is a perfect storm of people not getting care," he said.
But Dr. Louis Yarmosky, co-owner of Yarmosky Pediatric Dentistry, said adding another level of practitioner wouldn't help at his practice, which has locations in Pittsfield and Great Barrington.
It's a matter of space, he said. Both offices already operate at capacity and couldn't see a higher volume of patients if they wanted to.
"It's not about having more people to provide care; it's about being able to afford to provide the care." he said. "And for the patients, for most of them they don't have access to care because they can't afford it. So adding another level of dental care provider is not necessarily going to help the problem."
Yarmosky agrees that lack of access to dental care is a serious problem in the Berkshires that needs to be addressed. But a simpler and faster way to do what this legislation tries to do would be to expand the duties of a dental assistant to include some of the other routine dental procedures currently limited to full dentists.
And that wouldn't take two years in college, saving time and money.
"We applaud Smitty's efforts, but you have to deal with the reimbursements," Yarmosky said. "All kids deserve dental care. But access is not good because somebody has to pay for it. You can't work for nothing. If we were seeing 100 percent MassHealth patients, we would have to close our doors."
According to Michael Supranowicz, director of business development at Hillcrest Educational Centers, the dental hygiene practitioner would not only free up time for the dentist, but it would allow some practices to bring dental services to retirement homes or schools, bringing to services to those who can't get to a dentist office.
At Hillcrest Dental, part of the Hillcrest umbrella of services, approximately 75 percent of its patients in Pittsfield and North Adams are covered through MassHealth.
"Here at Hillcrest, we serve a large number of MassHealth patients, but there's a limit to how many people we can see in a given day," Supranowicz said. "Reimbursement rates, combined with provider shortages, can lead to more people going to the emergency room for care. Allowing for dental hygiene practitioners, combined with an increased MassHealth reimbursement rate, could potentially allow more MassHealth patients in the Berkshires to access care."
sstafford@berkshireeagle.com @BE_SStafford on Twitter.
-----
Our Opinion: "Addressing region's major dental issues"
The Berkshire Eagle, Editorial, 4/20/2016
A bill increasing the number of dental care providers will help address a severe dental care problem in the Berkshires and state. Increasing MassHealth reimbursements, however, is crucial to a long-term solution.
State Representative "Smitty" Pignatelli, a Lenox Democrat, has introduced legislation creating a new level of dental practitioner between a dental hygienist and a dentist (Eagle, April 20). Modeled after a Minnesota program, the dental hygiene practitioner would perform routine dental procedures and ideally free dentists for more severe problems and to nip potential problems in the bud.
A recent Health Policy Commission report found that Berkshire County residents seek emergency room treatment for dental problems at the second highest rate of any geographic group in the state. This is four to seven times more costly than treatment in a dentist's office, and as many of those treated are low-income residents or children, these high costs often get passed on to the state, and its taxpayers.
The mid-level dental practitioner should lessen this reliance on emergency room treatment. But as Representative Pignatelli acknowledges, a state health care plan that reimburses dentists for only 40 to 50 cents on the dollar makes it difficult for dentists to treat those patients while remaining economically solvent. Again, residents on MassHealth are in large part low-income, and if they do not get regular dental care they end up being treated in costly emergency rooms.
The combination of a new mid-level dental practitioner and better MassHealth reimbursement could go a long way toward addressing a painful and expensive problem in the Berkshires. Residents can help by establishing a dental home for their children at the age of one and by insisting that their children regularly brush and floss and avoid sweets. Preventing problems is preferable to finding ways for government to address them after they have arisen.
-----
Letter: "Mid-level dental care practitioner is critical for Berkshires"
The Berkshire Eagle, 4/27/2016
To the editor:
I would like to thank and applaud state Rep. "Smitty" Pignatelli for his long-standing commitment to the expansion of quality oral health care across all of Massachusetts. As The Eagle wrote, he is the lead House sponsor of a bill that would markedly increase access by creating a mid-level provider, a dental hygiene practitioner (DHP), modeled after the nurse practitioner model of care.
The DHP would be a licensed dental hygienist who has completed educational requirements equivalent to other mid-level practitioners such as nurse practitioners and physician assistants. Like them, DHPs would expand access to underserved areas and low-income populations. This has already been demonstrated by mid-level dental practitioners in Minnesota, where 78 percent of patients seen by these practitioners are publicly insured.
To expand access, it is necessary to create a new highly trained and educated mid-level practitioner who would establish a collaborative agreement with a licensed dentist, as opposed to adding additional duties to lower-level practitioners. Expanding the responsibilities of existing practitioners, such as a dental assistant, is not the correct approach. As compared to the four-plus years of education that a DHP would be required to complete, a dental assistant may only need two years of formal education in the field, or perhaps even less.
The curriculum for DHPs builds on licensed dental hygienists' training and includes a more rigorous licensing exam. These additional requirements allow DHPs to have a larger scope of practice where the level of education and experience directly correlates to increased public safety and greater expertise.
I'd also like to clear up the misconception that public health dental hygienists (PHDHs), established by the omnibus oral health legislation of 2010, are not making a marked difference. Every day, many of the most vulnerable residents of the commonwealth, often children and elders, receive much-needed oral health care from PHDHs. The existence of PHDHs does not cost the state anything, and yet saves the state thousands of dollars in unnecessary expenditures on oral health care, including in emergency rooms.
Access to dental care is an especially salient issue in the Berkshires, which lacks care for low-income individuals with public insurance. Creating a mid-level dental practitioner will increase the number of highly skilled dental providers and will ensure greater access for publicly insured individuals.
Joanne Simpson, Lee
The writer is past president of the American Dental Hygienists' Association — Massachusetts, Berkshire.
-----
Letter: "Fluoridation part of dental access issue"
The Berkshire Eagle, 4/30/2016
To the editor:
Regarding The Eagle's recent story about the number of Berkshire County residents who end up in the emergency room for dental care, it would be interesting to know if the majority of those visits occurred during the day when dental facilities are open or at night when they're closed.
Furthermore, most of the cities and towns in Western Massachusetts that have community water supplies are still not fluoridated. Fluoride is an important component of any dental health program. It's the single most effective way to prevent cavities.
If the focus is more on prevention, then it would likely reduce the number of visits to emergency rooms by those needing treatment. Prevention of dental disease through community water fluoridation should be a part of every discussion regarding access to care.
John P. Fisher, DDS, Salem
The writer is a trustee, Massachusetts Dental Society, and past president, Massachusetts Dental Society.
--------------------
"Smitty" Pignatelli: "A way to assure dental care for all"
By "Smitty" Pignatelli, Op-Ed, The Berkshire Eagle, 5/20/2016
LENOX - Last year, 47 percent of children with MassHealth coverage — more than 300,000 kids — did not see a dentist. Additionally, 59 percent of seniors in long-term care facilities have untreated dental disease. That is simply unacceptable, and is why Sen. Harriette Chandler and I have filed and advocated on behalf of a state policy change which evidence has shown improves access to quality care for children, the elderly, and low-income people.
S2076, the bill that Sen. Chandler and I filed together, would authorize a new type of dental professional in the commonwealth: a Dental Hygiene Practitioner (DHP). These dental providers — similar to physician assistants — would work under the supervision of a dentist and perform routine, critically needed care such as filling cavities and pulling badly diseased teeth. Similar providers have been practicing successfully in Minnesota and Alaska for years, expanding care to people in rural communities, reducing wait times, and improving the ability of dentists to treat more low-income patients.
The Health Policy Commission recently released preliminary findings which found that people insured through MassHealth disproportionately go to the emergency department for preventable oral health conditions, and the Berkshires has the second-highest rate of hospital visits for dental conditions in the state. Put another way, people in the Berkshires and across Massachusetts aren't getting the dental care they need, and they end up in the emergency room because they are experiencing pain that could have been prevented if they had received regular dental care.
Dental access is a particular problem in the Berkshires in part because we are more geographically dispersed than other parts of the state and have little public transportation, so it is harder to get to the dental office. We also have an aging population of dentists with little help on the way.
Consider these facts: nearly half the dentists in the Berkshires are nearing retirement, our county only has two percent of all private dental practices in the state, and dental students are now facing hundreds of thousands of dollars in loan debt. That's a recipe for a severe dental provider shortage for our region.
Additionally, many dentists in the Berkshires and across the state (79 percent) are not active MassHealth Providers, meaning they either do not accept MassHealth patients or they have a few established MassHealth patients and are not accepting any more. In other words, if you have MassHealth in the Berkshires and you're trying to access dental care, you are likely to be turned away by roughly 4 out of the 5 dentist offices that you call.
SADDENED BY FOES
The bottom line is that we will have fewer dentists in the future, and the dentists we have now are often picking and choosing their clients. Therefore, it saddens me that the primary organized opposition to this bill has been from dentists. Many dentists are not serving people who are in need, but they don't want someone else — even a type of provider that a recent meta-analysis of studies around the world found do good, safe work — filling a simple cavity before it becomes an abscess and lands someone in the ER.
Several weeks ago, the Berkshire District Dental Society and the Massachusetts Dental Society took out a full page ad in the Sunday Berkshire Eagle. The ad commends me for bringing attention to oral health care, but says that I have it wrong: this legislation will not fix the problem by getting care to those who need it. However, of the 39 Berkshire County dentists who signed the ad, only 19 of those dentists are general dentists, and of those general dentists, only three are currently accepting new MassHealth patients.
In fairness to dentists, the reason so many of them will turn you away is that MassHealth pays significantly less money for the same services than private insurers, so it is very difficult for a dentist to make a living providing care to only MassHealth patients. However, public reimbursement rates will never catch up with private rates, and Massachusetts already has one of the highest Medicaid reimbursement rates for dental care in the country.
That is why we need a creative, evidence-based solution to this problem, and creating a mid-level provider has been shown to increase access to care, especially for the neediest populations. That is why Maine and Vermont recently passed bills to create a similar mid-level dental provider.
Sen. Chandler and I invited the Massachusetts Dental Society to sit down and talk to us about how we can make this legislation stronger, because we value their expertise. However, after a lengthy negotiation session, which, at the time, both sides agreed had been productive, the Dental Society said it no longer wished to talk with us.
I was saddened by that development, but there is always resistance to change in how medical care is delivered. Just as doctors resisted the creation of physician assistants and nurse practitioners, dentists are now fighting the creation of a mid-level dental provider. But if we are going to provide quality care to everyone who needs it, we need innovative solutions, and evidence from other states and around the world shows that this approach works.
There is no silver bullet that will magically get care to everyone in need, but this is a piece of the puzzle, and I will continue to fight for this strategy as a piece of the larger fight for dental care for all.
"Smitty" Pignatelli is state representative, 4th Berkshire District.
--------------------
Letter: "Dental hygiene practitioner is not a solution"
The Berkshire Eagle, 5/31/2016
To the editor:
As one of the 19 dentists Rep. "Smitty" Pignatelli referred to in his May 22 op-ed column, "A way to assure dental care for all," I feel it is important to respond and explain my position. [The column referenced the 19 Berkshire general dentists among the dentists who signed an Eagle ad sponsored by the Berkshire district and Massachusetts dental societies.)
The honorable Mr. Pignatelli and the Berkshire District Dental Society agree upon the need for better dental health care for Berkshire residents. At present, health care and in particular dental health care provided by the Berkshire Medical Center emergency room is expensive and inefficient. The Berkshire Medical Center dental clinic located at 510 North St. has a walk-in clinic for dental emergencies Monday through Friday from 9 a.m. to 5 p.m. The emergency room is only used after hours and on weekends.
The problem is that patients do not come during regular clinic hours to seek dental care but like to get dental care at their convenience on nights and weekends. Mr. Pignatelli's response is with a dental hygiene practitioner, but that does not answer this problem. It would be better taken care of through the actions of social services, for instance with free tax stipends issued to individuals who have MassHealth to get to a MassHealth provider or the BMC dental clinic.
The Massachusetts Dental Society has recommended the hiring of at least eight community dental health workers to connect patients with appropriate care. We also proposed preventative measures (required dental exams for children entering school and community water fluoridation) to help reduce the need for dental treatment.
The number of providers in dentistry in the Berkshires is not growing because it is difficult to attract individuals to a community where economic development is stagnant or diminishing, as is occurring in the Berkshires. The new providers, as proposed by Mr. Pignatelli, have in Minnesota and Alaska ended up working in large cities similar to Boston, Worcester or Springfield. MassHealth lists two open providers within a 5-mile radius of every MassHealth patient in Berkshire County. Public health resources should be addressing issues such as education to seek dental treatment prior to occurrence of pain and for municipal fluoridation of water systems.
Many of my colleagues and I find it more feasible to volunteer our time, as I do as an attending dentist and teacher at the Berkshire Medical Center dental clinic, and/or as Volunteers in Medicine in Great Barrington, than to take MassHealth in our office, which carries high overhead.
Edwin J. Helitzer, D.M.D. Pittsfield
The writer is Berkshire dental representative to the Mass. Council on Dental Care and Benefits Programs, and chairman of the Massachusetts Dental Society Peer Review Council.
--------------------
"Lack of nearby medical marijuana dispensaries a hardship for Berkshire patients"
By Derek Gentile, The Berkshire Eagle, 10/23/2016
PITTSFIELD — When a marijuana dispensary was proposed in Adams last summer, it raised the hopes of "Callie," a North County resident who uses medical marijuana to alleviate crippling pain in her joints associated with multiple sclerosis.
A dispensary in Adams would eliminate the need to make the 40-mile drive to Northampton to fill her prescription.
"My mobility issues, and the fantastic amount of pain that comes with being in the car for any measurable amount of time, make it exhausting to get down to Northampton to get cannabis," said Callie, who asked that her real name be withheld.
But the Select Board shot down the plan amid concerns by some Select Board members, and even the police chief, who called it a "bad idea."
"I was devastated," she said.
Nearly three years since Massachusetts voters approved a referendum approving the use of medical marijuana in the state, Berkshire is among four counties — as well as Hampshire, Dukes and Nantucket — that have no dispensary. That despite language in the referendum that stipulated that by 2015, each county in Massachusetts should have at least one dispensary.
Two companies, Heka Health and Khem Organics, have received special permits to open dispensaries in Pittsfield. And provisional approval also has been granted to companies that want to operate in Lee and Great Barrington. But none of those businesses have received the required license from state Department of Public Health.
"We can't speculate on when new Registered Marijuana Dispensaries (RMDs) will be open," according to a spokesman for the state Department of Public Health, who requested anonymity because he was not authorized to speak officially on the matter. "There are a number of variables beyond the DPH application process to consider."
Since the first dispensary opened in Massachusetts in 2014, the use of medical marijuana has grown steadily over the past 30 months. From an initial core group of 64 patients, the state Department of Public Health now reports there were 29,999 patients statewide, as of Aug. 31.
Estimates of how many medical marijuana users live in the Berkshires varies from 200 to 500, but absent information from DPH, the number is difficult to pin down.
"The department does not currently provide county breakdowns," the spokesman said. "However, after some enhancements to our reporting system, we anticipate being able to provide county breakdowns by January 2017."
State Rep. William "Smitty" Pignatelli, D-Lenox, said he was confident that medical marijuana will be available in the Berkshires.
"It's coming," he said. "It's going to happen. But I don't know if it will be six months, or a year or more."
Pignatelli said that part of the issue is that approval of the ballot question sparked a premature creation of dispensaries.
"We made policy before we figured out how to implement it," he said. "That has slowed the process down considerably, as we try to figure out how to regulate it.
"Then, you bring in a new administration in 2015 [when Gov. Charlie Baker took office], and that slows it down further," he said.
Another part of the issue, many believe, is the stigma associated with marijuana use.
"It's pretty ironic," said "Rick," a city resident who uses medical marijuana to help treat his cancer. He also did not want his real name to be published. "Doctors dispense opioids like candy, and you have people addicted to pain pills.
"The stigma of 'Pot is bad' is embedded into our brains," he said. "It's hard to overcome."
The trip to Northampton also is difficult for "Donald," a 70-something South County resident who uses marijuana to alleviate his glaucoma symptoms.
"It's a project for me," he said. "I can't drive for extended periods."
He said he has to co-opt his daughter, who lives in Northern Connecticut, to take him to the Northampton dispensary.
Donald doesn't like to talk about his treatment — many members of his extended family don't know he uses marijuana — because he believes many in his generation would be judgmental.
"The ignorance is pretty breathtaking," he said. "And I included myself in that number for quite a while.
"I was a frat boy in college. I never smoked 'reefer,' " he said, making quotation marks with his fingers.
When his physician suggested cannabis to help treat his symptoms, "I was very nervous," he said with a laugh. "I watched all those "Reefer Madness" movies in high school in the 1950s."
"Reefer Madness," a movie released in 1936, was part of an anti-marijuana propaganda movement during that era.
For Donald said, the drug, which he takes as a pill, has been effective.
He said hopes a medical marijuana facility will open closer to his home, possibly on a county bus route.
"I'd like to see that," he said, "and so would my daughter."
Contact Derek Gentile at 413-496-6251. dgentile@berkshireeagle.com @DerekGentile on Twitter.
--------------------
"Berkshires Drop A Spot In County Health Rankings"
By Andy McKeever, iBerkshires Staff, March 31, 2019
PITTSFIELD, Mass. — Berkshire County has dropped a spot in the county health rankings.
The annual rankings measure in two categories — health outcomes and health factors. The county ranks 13 out of 14 counties in Massachusetts in the former and 11 out of 14 for the latter.
Neighboring Hampden County was dead last in both categories.
The report was released by local health officials on Monday and will serve as the basis for efforts to improve the well-being of residents throughout the county. The data used was garnered largely between 2015 and 2017.
"Our overall rank is not where we'd like it to be. Berkshire County currently ranks 13th out of the 14 counties in Massachusetts. We were hovering around 11th for a number of years, fell to 12th last year, and this year fell to 13th," Public Health Program Manager for Berkshire Regional Planning Commission Laura Kittross said.
However, Kittross was quick to point out that while the county may be low in the state's rankings, Massachusetts as a state is toward the top nationally.
"Ranking near the bottom in Massachusetts still means we are ranking very well compared to a lot of the United States," she said.
Health outcomes are a particular issue with Berkshire County. It is partly measured by years of potential life lost before the age of 75, for which the county is last in the state. Kittross noticed a big difference between race and ethnicities when digging into the data.
"The lowest life expectancy in Berkshire County is the Morningside neighborhood here in Pittsfield at 71 years. The highest is in New Marlborough at 87.5 years. But even just a couple miles away from Morningside is Lanesborough, we see a life expectancy of 86.6 years," Kitross said. The national average is 79.1 years.
She said even in Pittsfield there is a 12.5-year difference in life span between those who live in Morningside and those residing in the southeast neighborhoods. Kittross called on health officials to look even closer at the data to determine issues in those neighborhoods to help "level the playing field."
The other factor in outcomes is the quality of life. The county is slightly better there while being ranked at 11. Kittross pointed out a measure of those reporting themselves to be in poor or fair health is on par with the rest of the state but the number of days people have self-reported as being poor physical or mental health days are above average. She said those measurements are good indicators of health.
In the second broad category, health factors, the Berkshires are 11th. This category measures health behaviors and that, Kittross said, is what local officials can specifically address to help change outcomes.
"We are trending in the right direction on smoking. We are still in the lower half as far as the state goes but we have been steadily moving up [in the ranking]," she said. About 15 percent of Berkshire adults smoke compared to 14 percent statewide; the percentage was 19 in the 2012 health rankings for the Berkshires.
Kittross credits the decrease in smoking to efforts such as municipalities banning smoking from parks and the raising of the smoking age to 21.
The county is "doing great" when it comes to alcohol usage. The Berkshires ranks at the top of the list for the lowest percentage of people who reported binge drinking in the last 30 days. Overall, though, about a fifth of Massachusetts residents reported binge drinking.
However, Kittross said it is a mixed bag. While the binge-drinking numbers are down, about a quarter of the motor vehicle deaths in the last five years were because of alcohol. That is twice the rate of the best performers in the United States.
"Our obesity rates have typically been below the U.S. as well as Massachusetts. We are trending up, however, which is the wrong direction. We are now just slightly above the Massachusetts average. That is an indication of limited access to healthy food," Kittross said.
The report also shows that the county lacks access to recreational facilities, even though the Berkshires is considered a prime natural recreational area.
"We're actually doing really well on sexually transmitted infections, we are third, which is good. We are doing less well on teen birth rate though this is another one where we see the trend upward, we are ranking better than where we ranked a couple of years ago," Kitross said.
The county isn't doing so well with motor vehicle crash deaths. Kittross said fatal accidents related to alcohol are in the "middle of the pack" but the overall fatal motor-vehicle crash rate is the worst in the state.
She said that is another area to focus on — is it the quality of the roads, the distance of travel, or what?
Access to care is another strength, which may be a surprise to many. The Berkshires are 5th in the state when it comes to access to primary care physicians, 6th for dentists, and 3rd for mental health.
"We rate extremely well in this measure but there is at least a perception that we don't have enough primary-care providers and dentists," Kitross said.
The quality of care also ranked high. Kittross said that measurement is the rate of hospital stays for things that could have been treated as outpatient care, which is another indicator that access to primary-care doctors is doing well.
However, "this is only based on Medicare data so only people 65 and older so we may be missing trends in younger people," she said.
In preventive care, Kittross said the data is somewhat deceptive as well because such things as vaccinations are taken into account through Medicare data but locally there are strong pushes to make sure younger generations are vaccinated.
Plus, "preventative care is an area Massachusetts does really well," she said.
The county ranks 11th in social and economic factors. That takes into account such things as unemployment, which has been linked to higher mortality rates, unhealthy behavior, and a lack of access to health care because of insurance coverage.
Kittress highlighted the number of children in poverty as another stark inequity.
"This is a place we see huge inequities. Only 11 percent of the white children in Berkshire County are living in poverty and 51 percent of black children and 36 percent of Hispanic children live in poverty in Berkshire County," Kitross said.
The county is also doing poorly in the rate of those who attend any type of postsecondary education. Kittross said those with more education tend not to smoke, are more likely to exercise, are more likely to earn more, and live a life with less stress. Only 64 percent of the county has some post-secondary education whereas the top performer, Norfolk, is at 82 percent.
"We're not doing too poorly on high school education. We are at the Massachusetts mean. But where we are not doing as well is with people without any postsecondary education," Kitross said.
Kittross added another area the county is doing well in is housing.
While the report seems bad for the county overall, there are some bright spots. And for the negative areas, county organizations are prepared to roll out a strategic plan for change.
"Our goal is to improve the health status of Berkshire County by fostering a healthy lifestyle environment and our vision, and this is a pretty amazing vision, is to become the healthiest county in Massachusetts and the nation. We have some ways to go in Massachusetts," said Kim Kelly, who is heading the Community Health Initiative.
The CHI, as it is called, has been in existence since 2015 and has been growing. The membership now includes the Northern Berkshire Community Coalition, the Pittsfield Health Department, South County Rural Health Network, Berkshire Opioid Abuse Prevention Collaborative, BRPC, Tri-town Health, Fairview Hospital, Berkshire Public Health Alliance, Berkshire County Boards of Health Association, Volunteers in Medicine, and Berkshire Health Systems.
Kelly, who is the director of community health and public health initiatives for Berkshire Health Systems, said the group plans to create and implement a county health improvement plan to address the target areas in which the county is performing poorly.
The process restarts now as the now larger group readdresses the priority areas identified in 2015. Then the group will identify best practices and support initiatives to drive those changes.
"We have many strengths in our community, many strengths that you folks work on, and we have some opportunities," Kelly told the audience at the Zion Lutheran Church on Monday when the health data was presented.
link: https://www.iberkshires.com/story/59581/Berkshires-Drop-A-Spot-In-County-Health-Rankings.html
report link: http://www.countyhealthrankings.org/app/massachusetts/2019/rankings/berkshire/county/outcomes/overall/snapshot
--------------------
Opioid epidemic takes toll in county
In 2010, Berkshire County registered four deaths as the result of opioid-related overdose.
Those numbers have exploded, with a total of 218 deaths over the past 10 years. The annual count would increase tenfold by 2018, according to the Department of Public Health, increasing steadily each year except 2017, during which there was a slight decline.
Officials have linked the increase to the rise of fentanyl, a synthetic opioid pain relief that is 50 to 100 times more potent than morphine.
While early 2019 data showed a decrease in opioid-related deaths in some pockets of Massachusetts, Berkshire first responders noted that they didn’t see a reduction in overdose calls.
Some attributed the decrease to the availability of the overdose-reversal medication naloxone.
source: HINDSIGHT 2020: BERKSHIRE COUNTY'S TOP STORIES, 2010-2019, The Decade in News: North Adams loses hospital, Berkshire Mall flatlines, millions spent in Berkshire arts — and more, The Berkshire Eagle recounts decade's biggest news stories, December 28, 2019
— Tom Tripicco
--------------------
“From home offices and cars, Berkshire lawmakers are in incessant battle to fight effects of crisis”
By Damian Burchardt, Boston University State House Program via The Berkshire Eagle, March 27, 2020
Boston — Berkshire lawmakers are working long hours every day in search of solutions to the coronavirus crisis, all while practicing social distancing — even though it does not always mean working from the solitude of their home offices.
For Rep. Paul Mark, D-Peru, it means spending an enormous amount of time in his car so he does not miss updates from fire chiefs or public health department officers as the legislators are making painstaking efforts to ensure hospitals have enough medical supplies and adequate staffing, small businesses will not be doomed due to the statewide shutdown, and local elections can take place in a safe environment.
Mark does not have access to high-speed broadband service, similarly to more than a dozen other towns in western Massachusetts. His satellite-based internet service, with a cap on the amount of data he can use every month, only allows him to exchange emails, check social media, read newspapers and send text messages —exclusively to those, however, who can receive them through the web.
But he can't watch videos or make normal phone calls, so to attend remote meetings he has to either sit in his car parked on the side of the road or take detours while driving around areas that are still in service.
"I've had to spend a lot of time going out and doing things in my car," Mark says from the comfort of his vehicle, two miles away from his house while Massachusetts was hit with an unexpected snowfall early in the week.
"I think as more people are looking to set up these conference videos and these conference calls, it's going to be [...] it's potentially difficult to keep up, so I'm going to have to find a way to work Zoom remotely in my car parked somewhere. There's going to have to be a way to do it."
Some Massachusetts lawmakers still do come to the Statehouse despite the building being closed to the public. The lower chamber holds informal sessions every 72 hours under the state Constitution, although the turnout is significantly lower than usual.
Rep. William "Smitty" Pignatelli, D-Lenox, said that for the legislators, working from Beacon Hill is an individual choice. Two cases of coronavirus have been confirmed among the Statehouse staff, one of them being Rep. Mike Day, D-Stoneham, who announced falling ill on Wednesday.
Pignatelli said he has completed his committee work and stays in touch remotely. But with confirmed cases now reported in the Statehouse, he acknowledged, "I have no interest to step foot in there."
In terms of office work, he said his staff has adapted to new circumstances well, despite challenges that the inability to see each other face-to-face has posed.
Food insecurity, landlord-tenant issues — both residential and commercial — and small business assistance are among the problems he has had to address. But the biggest of them all, Pignatelli said, is unemployment.
"This is a very fluid situation that's changing hour by hour. But giving people the opportunity to sign up for unemployment gives them some sense of security [and] is really paramount," he said. "We're just trying to provide people with some guidance and some calmness — that we just need to keep it in perspective. Let's be calm, let's be smart, and let's stay healthy."
Mark said, however, that the lawmakers who still go to Beacon Hill — for reasons such as attempts to push a bill forward — adhere to safety guidelines. They preserve the 6-foot rule, try to sit at safe distances to other members, and don't congregate on the floor. But suggestions on the solutions to the abundance of issues that have arisen since the beginning of the coronavirus outbreak are often delivered remotely, via email or phone.
"I now spend almost all of my time with a phone to my ear from first thing in the morning until after dinner," said Sen. Adam Hinds, D-Pittsfield. "I used to drive sometimes three hours a day, just for meetings within my district. And now, all of that travel time is taken up with additional phone calls and conference calls."
For the lawmakers, one priority is to ensure health care centers receive enough help as the number of coronavirus cases rises daily, topping 2,000 in Massachusetts and 82,000 in the U.S. Mark said he has been trying to convince colleges and technical schools to donate medical equipment to local hospitals, and reaching out to federal officials to help cities and towns gain access to supplies from the Strategic National Stockpile.
Another priority is to mitigate the implications of the state-of-emergency call and other orders that resulted in many local businesses shutting down for the foreseeable future. Hinds points out that understanding the ripple effects of every action the lawmakers are taking has been particularly challenging.
"There's some clarity around the necessary public health actions needed," he said. "But then we are finding as legislators, as constituents come to us, that it then has unintended consequences for other state regulations and functions."
Rep. John Barrett III, D-North Adams, aware of the number of difficult decisions that have to be made, said he is happy to spend more time in his district to address the concerns of his constituents and assure them they will get through the crisis together.
He reeled off a list of challenges he's had to face amid the pandemic, which includes ensuring the food pantry remains open, working with local command centers and hospitals, while also dealing with proposals coming out of Gov. Charlie Baker's office on Beacon Hill, where he sits on the panel of the House Ways and Means Committee.
But while Barrett acknowledged the committee will not be able to flesh out its budget proposal as it normally would by the end of April, he thinks more burning issues are awaiting in his district.
"I'm a strong believer that I want the public to know that I'm here to help them," he said. "It's good that I'm in the district at this time. I want to be helpful to them, be helpful to the local governments."
Barrett said he is particularly worried about the surging unemployment and local restaurants, whose operations have been limited to takeout and delivery services following Baker's safety orders.
"I'm worried that some of our small-business owners will not survive this pandemic because they've had to close their businesses down," he said.
Barrett, who served as the mayor of North Adams for 26 years before becoming a member of the city council and eventually being elected as a state representative in 2017, said he has never seen a crisis of this magnitude and characterized by a similar degree of uncertainty.
"I've been in this business for a long time. And I've never encountered anything quite like this," he said. "We don't know when it's gonna end. We don't know what the magnitude is. We've had a lot of problems getting assistance from the federal government."
But knowing that the worst might be yet to come, Barrett claims that his district is prepared to provide additional medical beds if necessary or deliver food to the most vulnerable. "Those are the things that the command centers are working on. We are preparing for the worst," he said.
Rep. Tricia Farley-Bouvier, D-Pittsfield, was unavailable for comment.
--------------------
Letter: “BMC policy is a sick joke”
The Berkshire Eagle, April 6, 2020
To the editor:
If the article in the April 3 Eagle regarding BMC nurses had appeared on April 1 I would have had a good chuckle. A great April Fools joke.
I can't imagine an organization that would require it's front line responders and support staff to use their sick time if they are quarantined or infected by the COVID-19 virus. The people who came up with this cost-cutting idea should come out of their safe areas and go down on the floor where the action is. You can bet there would be face masks and gowns instead of having to wear the same one over and over.
Requiring a nurse (or any support staff) to use their own sick and vacation time if infected would be comparable to requiring a soldier wounded in combat to use up his leave time while recovering.
These professionals are putting their lives on the line for our community. Let's treat them with the respect they deserve.
Dick Eastland, Hinsdale
--------------------
Letter: “BMC isn't backing up nurses who get sick”
The Berkshire Eagle, April 6, 2020
To the editor:
I've been an ICU nurse here in the Berkshires for almost 37 years. I love nursing. I love critical care.
From my heart, I want to thank so many - our coworkers from all departments who've sent food, who show up asking "how can I help?". All the support staff who make our work possible. To my friends across the country checking in, wanting to know I'm OK. And those in our community who have shown such love and respect during this crisis. Today, a woman had food delivered for every employee. Every one! You all have no idea how much it means.
We will continue to do the work we do because...well, that's what we do. But these are tough times. Extraordinary times.
On Tuesday, we were notified that if we are exposed at work, we are expected to monitor our temperature and come in.....OK. If we are sickened by this virus, it will be assumed we acquired it in the community and therefore workman's comp will not apply, we can use our sick time, which includes vacation time in our case. Not OK at all.
The CDC continues to downgrade standards of personal protection, not because they work, but due to low supplies. What used to be "unsafe" and you could be disciplined or fired for is now the standard. As I read the notification, I was wearing the same mask and face shield for nine days. They go in a paper bag, and I bring them out, put them in again and again. It's called contamination. Under these circumstances, presuming medical staff are surely being infected in the community is bizarre.
No one expects my hospital to have a magic wand when it comes to these precious supplies, which is why we reuse them, we have no choice. But I do expect my hospital to back us up if we get sick. The latest policy is not OK.
I can't explain what the world is like in my ICU now, it's beyond description. It's stressful, heartbreaking, scary.
We'll continue doing what we do. We need you to do what YOU can do...social distancing, staying home as much as possible, wash your hands. Love your friends and family by doing your part to protect them.
I work at a small hospital in the country. It's here. This is real.
Alexandra Huber, Lenox
--------------------
Letter: "Losing cardiac rehab program a big blow to BMC's service"
The Berkshire Eagle, September 9, 2020
To the editor:
As one of the original founders of the cardiac rehab program at Berkshire Medical Center, I was gravely disappointed to read about the decision to terminate operations.
When we began the program, cardiology had emerged from the "dark ages" of treating heart attacks with six weeks of bed rest and, if patients survived, a lifetime of restricted activity. We were so innovative that Benita Zahn and a crew from Channel 13 came to Pittsfield to film our operation and broadcast it because we were even ahead of Albany Medical Center in starting it.
Over the years, countless people recovering from heart attacks, heart surgery, heart failure and subsequently those with lung issues benefited from not only supervised exercise but also nutritional counseling, social services and smoking cessation, and achieved healthier lifestyles.
The dedicated staff became not only educators but friends to their patients and families.
I understand the impact of COVID-19, but as hospitals have reassured patients that they are back to full service, not finding a way to continue cardiac rehab while emphasizing and advocating better population health seems counter-intuitive.
Please rethink this decision.
Henry Tulgan, M.D., Pittsfield
The writer worked at Berkshire Medical Center until 2008, and was a founding medical director of the hospital's Cardiac and Pulmonary Rehabilitation Maintenance Exercise Program. He is currently the director of medical education at Baystate Wing Hospital in Palmer and professor of medicine at University of Massachusetts Medical School in Worcester.
--------------------
Letter: "We shouldn't neglect pediatric dentistry for families in need"
The Berkshire Eagle, May 18, 2021
To the editor:
It is disappointing to see no reaction to the lead article that appeared in The Eagle last week referring to the strains on delivery of pediatric dental care in Massachusetts. ("Amid pandemic stress and stagnating dental care reimbursements, Berkshire dentists pull out of MassHealth," Eagle, May 2.)
The issue was publicized by two pediatric dentists in Berkshire County being forced to make the decision to curtail their availability to treat the young segment of population with distressed health care means due to low or nonexistant Mass Health reimbursement levels. Most of these needed services for financially strained families are supported by meager, insufficient reimbursement to the dentist, who, along with the youngster, depends on Mass Health coverage for at least some basic level of care.
The bureaucratic wisdom falls on the premise that taxpayer support for the low-income families cannot solve many deeper needs and that some care is better than none. Additionally, many erroneously subscribe to the fact that so-called “baby” teeth fall out and therefore are expendable in the long run. “No permanent deficit,” alas, is not even close to being true.
Pediatric Dentistry is far from simply filling or extracting teeth. Obligation to recognize neonatal defects begin the continued concern to correct function, speech, nutritional and appearance disorders. Growth and development of the face and jaws should be guided by professional scrutiny. Often interrupted or deviated by airway stricture, breathing impediments, oral habits and sleep deficit, facial deformity may occur. Scrutiny for neoplastic growths and tumors is constant. Nutritional guidance is so important during these formative years for both caries control and metabolism for strong bone and teeth themselves.
Contrarily, the so-called expendable primary teeth serve a valuable roadmap for the growth and development of the jaws and face. Premature loss of these teeth, or their destruction by decay, causes jaw collapse, pain and eating disorders. Later, crowding and facial deformity ensue necessitating orthodontic intervention, sometimes including surgery.
The financial dissuading of regular developmental care pushes it harder to get regular dental visits for this vulnerable population. It only postpones the inevitable — more damage, more repair, more dysfunction, perhaps more discomfort and pain. But the bigger misfortune, other than the human factors, is that the intended savings to health agencies and their coffers for demurring on fair reimbursement for these basic preventive and protective service expenses will be dwarfed by the future costs that will be astronomically multiplied for what lies ahead.
Our young patients deserve much better.
Dr. Ronald I. Maitland, DMD, Lenox
The writer is a retired associate professor at New York University’s College of Dentistry and a visiting professor at the Tufts University School of Dental Medicine.
--------------------
Rep. Smitty Pignatelli: "It’s time to act on HOPE"
By Rep. Smitty Pignatelli, Op-Ed, The Berkshire Eagle, October 26, 2021
This week, I testified in support of H.2125 — An Act helping overdosing persons in emergencies, also known as the HOPE Act — which I filed with Sen. Joan B. Lovely, D-Second Essex, and it was well received by the Joint Committee on Mental Health, Substance Use and Recovery.
In 2020, overdose deaths from opioid use reached a record high of 93,331, according to the Centers for Disease Control and Prevention. While these estimates are not final, this is more than 20,000 deaths above the previous high in 2019 and the largest single-year percentage increase on record since 1999, directly highlighting the drastic toll that the COVID-19pandemic had on the raging opioid epidemic in our commonwealth and across our nation.
In 2017, an individual in my district died from an overdose in the presence of a first-responder while waiting for Narcan to arrive. Narcan (naloxone) is a life-saving opioid antagonist that saves thousands from opioid death each year, and is a critical resource that we need in order to combat the worsening opioid crisis. This is a particularly crucial resource in rural areas like the Berkshires, where we can’t be sure which first-responder will be the first to arrive. But in Berkshire County, nearly 60 percent of first responders do not carry an opioid antagonist. This is why I filed the HOPE Act, and this is why we need to act on it.
When first responders arrive on the scene, it should be a guarantee that they can administer life-saving treatments like Narcan without hesitation. This bill requires all first responders to carry an opioid antagonist on their person or in their vehicle while on duty, and reinforces the importance of training so that any person who enters an overdose situation is equipped, prepared and able to save a life. With numerous police and fire departments throughout Massachusetts already implementing these protocols and procedures, this bill seeks to codify the important steps that are already being taken across the state.
Not only is this legislation important for people at risk of overdosing, but it also protects first responders and families who may be exposed to lethal substances. In 2018, two Southwick police officers self-administered Narcan while responding to an overdose after exposure to what they believe was fentanyl. This is not an isolated case — there are countless other examples where opioid antagonists have not only saved a person at risk of overdose but have simultaneously ensured the health or safety of those around them.
The cost of implementing Narcan programs — which has been mitigated and simplified by the work of the Attorney General’s Office and the Baker administration’s recovery relief efforts — does not come close to equating the cost of losing a life that could have been saved with access to proper treatment. If we want any chance of tackling the opioid epidemic and if we want to see those struggling with substance use get to the stage of recovery, we need to take swift, bold and urgent action to implement comprehensive solutions. It’s time to give our communities and families an opportunity for a healthier tomorrow, and it’s time to act on HOPE.
--------------------
Letter: "An opportunity for significant change at BHS"
The Berkshire Eagle, December 18, 2021
To the editor: As Darlene Rodowicz takes over the leadership of Berkshire Health Systems, we hope that she will see the value of listening to and considering the advice of Berkshire Health Systems front-line health care staff — from housekeeping workers, dieticians and pharmacists to nurses and physicians.
In past years, our community has witnessed the departure from BHS of excellent physicians and nurses who were deeply committed to the health of our community but who lacked the support of the hospital leadership. In addition, significant suggestions by the nursing staff for improving working conditions and patient safety, particularly during the COVID-19 pandemic, have gone unheard. The apparent managerial philosophy of BHS may be consonant with what their business consultants advocate, but it defies the advice of most scholars of complex organizations. Rather than creating a "fearless organization," as advocated by Amy Edmondson, Professor of Harvard Business School, who has actively studied the management of hospital systems, they instead seem to have established a "fearful organization," with a noncollegial working environment for their staff.
It is disappointing to us that the descriptions of Mr. Phelps' and Ms. Rodowicz's leadership in recent Berkshire Eagle articles mentioned only their success in improving BHS' financial circumstances, but not their record on patient care outcomes or staff satisfaction. When leadership changes in any system, it provides a unique opportunity to make significant alterations in its culture, values and vision. We hope that Ms. Rodowicz will take advantage of her new role to make BHS a more positive workplace for all staff. Doing this will have a direct impact on the quality of care that we, residents and patients in Berkshire County, deserve.
Peter M. Lazes, West Stockbridge
Marie G. Rudden, West Stockbridge
Peter Lazes is the visiting professor and co-coordinator of the Healthcare Partnership Initiative at Penn State University's School of Labor and Employment Relations. Marie Rudden is an assistant clinical professor of psychiatry at the Weill Cornell School of Medicine. They are co-authors of "From the Ground Up: How Frontline Staff Can Save America's Healthcare."
--------------------
Letter: "Let's make health care affordable for all"
The Berkshire Eagle, December 24, 2021
To the editor: I am writing to voice my support for state Rep. Smitty Pignatelli’s position on affordable care outlined in The Berkshire Eagle on Dec. 7 [2021].
If Congress wants to ensure that Americans are well-equipped to recover from this pandemic, then access to affordable health care must be a priority in any spending bill. As Rep. Pignatelli explains, the crucial subsidies expanded under the American Rescue Plan Act are set to expire. That would mean millions of Americans who are enrolled in the federal and state marketplaces would face higher premiums and the risk of losing coverage altogether.
Expiration of this program would impact more than 12 million Americans. At a time when access to quality care has never been more important, we must take any and all steps to ensure our community members can get the best care they deserve. This is why I am urging U.S. Rep. Richard Neal to push for making these subsidies permanent as Congress debates health care spending in the new year.
If Congress can do this, 19,000 uninsured Bay Staters could have access to affordable care through marketplace tax credits next year. It is essential that Americans are more equipped to handle health challenges like a pandemic. Let’s get this done.
Michele E. Darroch, Pittsfield
The writer is the coordinator for the physical therapist assistant program at Berkshire Community College.
--------------------
"In Massachusetts, health and human services is run by one department; a job too big for one executive office, says John Barrett"
By Danny Jin, The Berkshire Eagle, December 24, 2021
NORTH ADAMS — State Rep. John Barrett III has proposed to split the largest agency in state government into two agencies, an effort that he hopes will advance in the new year.
“I’ve said from Day One that I think the Executive Office of Health and Human Services is much too large,” Barrett, D-North Adams, said in a Thursday phone interview when asked what steps the state can take to avoid COVID-19 spikes in nursing homes.
“I testified at a hearing, I thought there was some support from the committee, and time will tell if it moves forward,” he said.
EOHHS oversees 12 agencies, two soldiers’ homes and the MassHealth program. Its budget makes up around 56 percent of the state budget, and EOHHS has expanded rapidly since it was last reorganized in 2003, Barrett said at a September hearing before the Joint Committee on State Administration and Regulatory Oversight.
“All I know is I’ve had children die in my district because of neglect,” Barrett said. “I’ve had people die at veterans homes. I’ve seen problems with our health care.”
“But I’ve seen a secretary who’s worked very hard in doing what she’s doing,” he said, praising Secretary of Health and Human Services Marylou Sudders. “It’s just my conclusion [that] it’s too much for one person to be undertaking.”
EOHHS agencies include the Department of Public Health, Department of Children and Families, Executive Office of Elder Affairs, Department of Developmental Services, Department of Transitional Assistance Department of Mental Health, Department of Veterans' Services, Department of Youth Services, Massachusetts Commission for the Blind, Massachusetts Rehabilitation Commission, Massachusetts Commission for the Deaf and Hard of Hearing, and Office for Refugees and Immigrants.
Barrett’s bill would establish a nine-member commission to study the benefits of dividing EOHHS into an executive office for public health and oversight and an executive office for human services.
Nine lawmakers have signed on as co-sponsors for the bill, including state Reps. William “Smitty” Pignatelli, D-Lenox, and Paul Mark, D-Peru.
State Sen. Rebecca Rausch, D-Needham, said at the September hearing that her time as an attorney at EOHHS led her to support Barrett’s proposal.
“I, too, have for a long time looked at this from a structural perspective and said, ‘Wow, we really need to make some changes and make some improvements here,’ ” Rausch said.
The Joint Committee on State Administration and Regulatory Oversight can advance Barrett’s bill to the Ways and Means Committee with a favorable report.
“There’s a lot to talk about on this,” State Administration and Regulatory Oversight co-chairman Antonio Cabral, a Democratic state representative from New Bedford, said at the September hearing. “I have a lot of interest in this area as well.”
--------------------
Our Opinion: "Filling the worrisome holes in dental care access"
The Berkshire Eagle, Editorial, February 12, 2022
If we care about expanding health care access to all regardless of income, that must include dental care, too. Community Health Programs knows that, and thankfully the nonprofit is doing something about it for the worrying fraction of Berkshire Medicaid enrollees who don’t have a dentist. Deprivation of decent dental care, though, is a broader structural problem that shouldn’t and can’t fall to a single nonprofit to solve.
For thousands of patients enrolled in Medicaid, getting critical preventive care and other dental services is nearly impossible. Why? In no small part because there are not enough dentists willing to care for them, a gap that Community Health Programs wants to help close.
We are encouraged to hear CHP’s planned $6 million expansion will hopefully double its capacity to provide dental services to those with Medicaid. We also must underscore why this move is so imperative. In the Berkshires, about four in 10 enrollees in MassHealth — the state’s version of Medicaid, which assists limited-income people with health care costs — lack a dental provider. A big part of the reason why is an unfortunately familiar theme for low-income people seeking access to physical, mental and behavioral heath care: Like many rural, underserved regions across America, ours has a dearth of providers. Meanwhile, lackluster Medicaid reimbursements for dental care have led more and more private practitioners to stop serving Medicaid clients.
For many poor people, that squeeze means accessing basic dental care is essentially impossible. We can’t allow this to continue. That some of our neighbors suffer the pain and stress of dental issues simply because they’re low-income is morally unacceptable in the richest nation in history. Further, oral health is like all others in an important way: Prevention is far more cost-efficient than treatment. If low-income people can’t get dental check-ups, they’re far more likely to develop downstream problems that require expensive oral surgery or an emergency room visit, a heavier cost for them that also impacts their communities through more strain on the safety net, insurers and ERs.
Our community is lucky to have an organization that seeks to provide quality and compassionate care to all regardless of ability to pay. But as groups like CHP attempt to help vulnerable people trapped in care gaps, we as a society owe it to those groups and those people to address the gaps themselves. If Medicaid is meant to help limited-income folks access critical care like dental check-ups, why is the reimbursement rate such that it actually dissuades many providers from caring for them? That is a policy choice, and it’s one we can choose to make differently.
A bill currently on Beacon Hill (H.1250) would increase the dental enhancement fee that community health centers like CHP receive for their life-giving work. Another bill (H.1180), filed by state Rep. Smitty Pignatelli, D-Lenox, seeks to address the bottleneck of available providers by allowing dental hygienists and assistants to perform more basic services and thereby increase capacity. Both of these measures deserve the Legislature’s serious attention as ways to increase quality of life for vulnerable constituents in rural and less populous corners of the state. Meanwhile, Congress should move on the Medicaid Dental Benefit Act, which would increase the reimbursement rates for such services.
Beyond policy, this is an issue of priority. Yes, all of these proposals to make decent dental care more equitable cost money — whether it’s the $6 million CHP is putting up originating from grants and subsidies or the tax dollars that could provide more expansive funding in our public budgets at the state and federal level. If we say we care about health care access as a priority issue, that conversation requires some parity for the consideration of dental care, just as it does for mental and behavioral care.
Health care and dental care are often construed as different concepts. Tell that to the 28-year-old who came to CHP with teeth so deteriorated every single one required extraction. John Brazill, CHP’s director of dental programs, told The Eagle about seeing just such a patient recently. “It was shocking,” Brazill said. It should be shocking to all of us in a nation of plenty that we let such fates befall our neighbors because of economic barriers to care.
--------------------
February 12, 2022
The Dirty Bird had an editorial about how a lot of people on MassHealth (Medicaid is administered by the state government) are unable to receive dental care. While Trippy Country Buffet, Shitty Pigpen, Paul Marxism, the career Mayor, and Chrome Dome are voting for undocumented immigrants' interests, they are doing nothing about MassHealth's huge gap in dental coverage. The Dirty Bird said that Shitty Pigpen has a bill (H.1180) in Boston to allow dental hygienists and assistants to perform more basic dental services, but the fact is that Shitty Pigpen is doing nothing about MassHealth long history of underfunding dental payments to dental providers for patients on Medicaid, which is administered by the state government that Shitty Pigpen has been in since 2003, which is over 19 years and counting.
Smitty Pignatelli annoys me to no end because he writes the loftiest op-eds in Western Massachusetts newspapers about his would-be futile efforts in Boston, but his public record is nothing but lofty because he mostly votes in lockstep with the all-powerful Speaker of the State House of Representatives. Shitty Pigpen is a financially educated man who graduated from a business college who then worked at Lee Bank prior to serving on Beacon Hill. He knows damn well that his lofty words contradict Boston's long public record of systemically underfunding critical institutions and services throughout the Commonwealth of Massachusetts. In closing, he NEVER puts the state's money where his lofty words are!
Jonathan A. Melle
--------------------
"Massachusetts no longer will provide free COVID testing in the Berkshires. State lawmakers say there needs to be regional equity"
By Danny Jin, The Berkshire Eagle, March 7, 2022
Massachusetts no longer will cover free, asymptomatic COVID-19 testing at Berkshire Health Systems sites in Pittsfield, Great Barrington and North Adams, as the state downsizes its Stop the Spread program.
Berkshire Health Systems will continue to provide testing at those locations, hospital spokesperson Michael Leary said in a Monday email, as it has done throughout the coronavirus pandemic. Other testing providers also will continue to operate in the county.
But, the absence of Stop the Spread sites means that everyone going for a test will have to pay through insurance, as they do now, or out of pocket.
The state began opening Stop the Spread sites across the state in July 2020, providing free tests, regardless of insurance, in order to reduce virus spread. The three Berkshire County sites were added to the free testing program in December 2020.
Last week, the state announced that it would discontinue Stop the Spread testing at all but 11 high-volume sites as of April 1. The change comes as case and testing rates have declined dramatically since the omicron surge.
In an effort to ease the transition for communities with discontinued sites, it will provide at-home rapid tests to municipalities, including 1,260 tests for Pittsfield, and nearly 1,100 each for Great Barrington and North Adams.
Berkshire County lawmakers have asked the state to keep at least one Stop the Spread site open in the Berkshires. The county’s five state lawmakers sent a letter to Secretary of Health and Human Services Marylou Sudders on Friday.
“If closed, Berkshire County residents would be forced to travel to Springfield for free, non-symptomatic testing, which is a 60-90 minute drive depending on where one lives in the county,” lawmakers wrote in the letter.
The change largely will affect people without health insurance, who now will have to pay out of pocket for at-home or lab tests. It also could affect the region’s capacity for testing in the event of another surge.
Those with insurance will be able to test, as usual, at Berkshire Health Systems or retail pharmacies. Insurers now also are required to reimburse the costs of up to eight at-home, over-the-counter tests per month.
Getting those free at-home tests through insurance has become easier since the program kicked off, though the process still can be onerous at times. Many insurers, including MassHealth and Blue Cross Blue Shield, allow members to purchase tests at the pharmacy counter of certain retail pharmacies at no-upfront costs. Others, though, require the purchaser to front the cost and file for reimbursement.
Anyone, regardless of insurance, also can receive free at-home testing kits from the federal government through the U.S. Postal Service. A second round of ordering began in early March, which means that anyone can order four additional tests via special.usps.com/testkits.
The Executive Office of Health and Human Services did not immediately respond to an inquiry Monday about the Stop the Spread sites.
The state said last week that the remaining 11 sites, which include two in Springfield, accounted for nearly 72 percent of Stop the Spread testing from Jan. 20 to Feb. 16. In addition, cases are down 96 percent from the January peak, and Stop the Spread testing volume has decreased by 80 percent since the start of January, the Executive Office of Health and Human Services said.
State Rep. Tricia Farley-Bouvier, D-Pittsfield, said the delegation believes that “if the state feels there needs to be Stop the Spread sites anywhere in the state, we should make sure there’s one here.”
“It seems like what they did was, they went to the highest rates of tests without taking into account the other factors,” Farley-Bouvier said, noting that test positivity rates in Berkshire County typically have exceeded the state average.
From Feb. 13 through Feb. 26 [2022], the most recent two-week period of state data, test positivity rates in much of Western Massachusetts were well above the state average of 2.3 percent. Berkshire County recorded a 14-day test positivity rate of 3.7 percent, on par with Hampden County, according to state data. Only Barnstable County had a higher positivity rate, at 4.5 percent.
For people paying out of pocket, at-home testing is more accessible financially than lab-based tests. Over-the-counter tests, though less accurate than lab tests, typically cost $10 to $12 each. Also, the state has provided free kits for low-income residents at times.
Berkshire Health Systems would not say how much it charges insurers or individuals for testing. But, major hospitals across the U.S. have priced COVID-19 diagnostic tests at $148, on average, according to an April 2021 report by the Kaiser Family Foundation.
The analysis found that nearly half of all charges were $100 to $199, though prices could vary from $20 to more than $1,000, depending on the hospital and the lab used for testing.
--------------------
Letter: "We need a single-payer health care system now"
The Berkshire Eagle, February 18, 2023
To the editor: Your article on the possibility of a single-payer health system in Massachusetts makes clear that the current medical system is driven by the profit motive — and that the speaker of the House is intent on maintaining the status quo. ("Berkshire doctors, activists, confront lawmakers about prioritizing single-payer health care legislation," Eagle, Feb. 11.)
I thank Reps. Smitty Pignatelli and Tricia Farley-Bouvier for their ongoing support of a single-payer system. To Rep. Pignatelli’s concern about “quality health care and maintaining small hospitals in the Berkshires,” I would add that the current system continues to produce ongoing closures of rural hospitals and medical bankruptcies.
We need to put people’s welfare over profits when it comes to health care — and a single-payer system will make that happen.
Michele Marantz, Dalton
--------------------
"The proposal to reopen North Adams Regional Hospital has drawn pushback from a surprising source: long-term health care facilities in the area"
By Sten Spinella, The Berkshire Eagle, November 4, 2023
NORTH ADAMS — Reopening North Adams Regional Hospital would benefit the community in myriad ways, including bringing new jobs, a return of inpatient care and shorter ambulance response times.
But it also could have a negative impact on Northern Berkshire County’s long-term care facilities, according to representatives of the senior care industry.
During a Department of Public Health hearing last week, some of those representatives noted that the benefits of granting the facility critical access hospital designation — including greater reimbursements and flexibility in how it uses its inpatient beds — could put existing senior care facilities at a competitive disadvantage.
“The combination of this enhanced reimbursement coupled with the ability to swing beds to use as a nursing home presents a real threat to the viability of nursing homes in Northern Berkshire," said Integritus Healthcare President William Jones. Integritus owns several local nursing care facilities countywide, including Williamstown and North Adams Commons in North County.
Berkshire Health Systems announced in June that the hospital, which closed abruptly in 2014, could reopen with 25 inpatient beds on a medical-surgical floor this winter if it receives critical access hospital designation. Such a designation, which provides additional financial help for hospitals in remote or rural areas, would make providing hospital-level care financially viable.
During the public hearing, held as part of the DPH determination of need process, several state and community leaders lined up in a forceful show of support for the change, which was made possible due to a change in federal regulations.
Others, however, voiced concern that a resurrected NARH will take staff and business away from long-term care facilities. And allowing NARH to use all of its 18 acute care beds as “swing beds,” meaning they can also be used for rehabilitation, could put some of the county’s 13 nursing facilities out of business, according to Tara Gregorio, representing the Mass Senior Care Association.
The senior care advocates avoided saying they were opposed to the hospital outright, but implored the DPH to impose conditions on its determination, including barring Berkshire Health Systems from recruiting local long-term care staff for two years, and limiting swing beds.
"With that critical access designation, they can access swing beds. That essentially means they can use beds in different ways, either on the hospital side or for folks who would generally go to a nursing home," Integritus spokesperson Lisa Gaudet said Wednesday. "Instead of having 18 to 25 swing beds, a lower number would serve the community while also allowing North Adams Regional to do all the great things they're going to do."
State Rep. John Barrett III, D-North Adams, was taken aback by the testimony by Jones, the Integritus president.
“I cannot believe someone in his position would speak out against creating an area hospital that’s so important to the Northern Berkshire area,” Barrett said. “I can’t believe an agency of this type, in health care, would do this. We need that hospital.”
Barrett joined state Sen. Paul Mark, D-Becket, North Adams Mayor Jennifer Macksey, Massachusetts College of Liberal Arts President James Birge, BHS CEO Darlene Rodowicz, and many others, including Northern Berkshire natives, who threw their weight behind the effort to reopen NARH.
Rodowicz said the cost-based reimbursement that comes with a critical access hospital designation “is a lifeline for rural communities like ours.” She and others made the point that NARH will improve access to inpatient care for those stuck between the two nearest hospitals in Pittsfield and Bennington, and that it would improve social and economic opportunity.
Mark said NARH would offer new jobs as doctors, nurses, clinicians, support service professionals and technicians, “not to mention the multiplier effect that having a vibrant professional organization in the heart of North Adams will have on other businesses in the city and the surrounding region.”
“I’m also particularly grateful that Berkshire Health Systems has committed to upholding the union agreements for bargaining unit positions at the new North Adams Regional Hospital campus,” Mark added, “which is an important recognition of the rights of our dedicated health care workforce.”
Referencing MCLA’s new nursing program, Birge said NARH would pose “a promising avenue for future employment.”
“The presence of a top-tier hospital in our community is a significant draw for prospective college students” as it could lead to “employment right in their backyard,” Birge said.
Macksey and others pointed out the psychological effect of bringing the hospital back.
“Our hospital’s return represents more than a medical facility,” she said. “It symbolizes our collective commitment to healthy progress and community resilience.”
In reflecting on the devastating effect closing the hospital had on North Adams, Barrett recollected 1988.
“I was mayor when the administration of the former North Adams Regional Hospital decided not to move forward in seeking a permanent designation as a critical access hospital in 1988,” he said. “If they hadn’t made that terrible decision, how much different would the face of Northern Berkshire be today, especially in regard to our economy.”
U.S. Rep. Richard Neal, who has long lobbied for a regulatory change that would allow NARH to be designated a CAH, submitted written testimony in support.
Doctor Alec Belman, who works at Fairview Hospital in Great Barrington, which is a critical access hospital, spoke to the importance of swing beds at a new NARH.
“In my experience at Fairview, swing beds have been an invaluable resource for patients to have a convenient, transitional care option that is close to home,” he said.
John Meaney, general manager of Northern Berkshire EMS, said reopening NARH could mean a drastic reduction in transport times.
"Fewer hour-and-a-half to two-hour round trips to connect patients with in-person care at Berkshire Medical Center in Pittsfield will reduce wear and tear on our vehicles and equipment, keep staff and patients safer during poor winter weather conditions, and allow us at Northern Berkshire EMS to instead direct our resources to ongoing system improvements,” he said.
Michelle Byron, who was born and raised in Northern Berkshire County and is currently a resident of Adams, talked about her parents’ struggle with health care after NARH closed in 2014.
“My parents are now in a nursing home, but I am almost 72, and I would like to know that if I need hospital care, I could be taken care of in North Adams so that it would be easier on my family,” she said.
--------------------
Letter: "Follow the money behind testimony against NARH's reopening plan"
The Berkshire Eagle, November 8, 2023
To the editor: State Rep. John Barrett III, D-North Adams, cannot believe that the president of Integritus Healthcare would speak out against reopening a critical access hospital. ("The proposal to reopen North Adams Regional Hospital has drawn pushback from a surprising source: long-term health care facilities in the area," Eagle, Nov. 4.)
It's really very simple. Just follow the money. In 2021, Integritus' then-CEO David Phelps was paid $1,137,632 and Integritus' president William Jones Jr., who is now CEO, was paid $511,933, according to ProPublica's nonprofit explorer project.
I think that says it all.
Nancy Stuart, Lee
--------------------
Letter: "My reply to Rep. Barrett's remarks after NARH determination of need hearing"
The Berkshire Eagle, November 9, 2023
To the editor: Being a longtime admirer of state Rep. John Barrett III with his commitment to public service and his community, I must admit I was very disappointed by his criticism of Bill Jones, CEO of Integritus Healthcare, in a recent Berkshire Eagle article. ("The proposal to reopen North Adams Regional Hospital has drawn pushback from a surprising source: long-term health care facilities in the area," Eagle, Nov. 4.)
I guess you could say I was "irked."
If you listen closely to Bill Jones' public testimony during the public hearing, he was being supportive of the application, while advocating for his facilities, the residents, the employees, the community and doing what the Massachusetts Department of Public Health requested as part of the determination of need review. In other words, he was doing his job and doing it well.
The determination of need program as administered by each state is intended to ensure that there are adequate health care services available for its citizens while limiting duplication of services and ensuring that they're cost effective.
John was no longer mayor of North Adams at the time of North Adams Regional Hospital's closure, but he had a front-row seat to many of the events that led to the closure of North Adams Regional Hospital. The incredible lack of governance and oversight, combined with the absence of accountability from the regulators, resulted in a predictable outcome.
In fairness, the hospital closure plan was totally inadequate. NARH got a pass. The hospital acquired Sweetbrook nursing home and subsequently ran it into the ground. NARH got another pass. There are many outstanding financial issues with the adjacent retirement communities. Apparently, NARH got another pass. Is John suggesting that we rubber stamp this application and give out another pass?
I believe the appropriate expression at this time is "if we ignore history, we are condemned to repeat it."
It appears there is unanimous support for this application some with conditions.
Considering the justifiable concern about the existing labor market and the fragile nature of other health care providers, it would be a good time to listen rather than criticize someone for doing their job. And John, if you're interested in learning more about health care leadership, I'm sure Bill Jones could spare a few minutes of his time.
Richard J. Herrick, Lenox
--------------------
Letter: "A Prescription for Survival: Solving Western Mass Physician Crisis"
iBerkshires.com - Letter to the Editor - March 09, 2025
To the Editor:
In the shadow of the Berkshires' rolling hills, a quiet calamity unfolds. Rural western Massachusetts — Berkshire, Franklin, and parts of Hampden and Hampshire Counties — teeters on the edge of a health-care abyss. Primary care physicians (PCPs), the bedrock of community wellness, are vanishing. With wait times stretching six to 12 months and ratios dipping to 60-70 doctors per 100,000 residents — half the state's average — this is no mere inconvenience. It's a crisis of equity, economics, and survival, demanding bold, bipartisan action now.
The numbers are stark. Berkshire County, home to 125,000 souls, has lost a third of its PCPs since the 2014 closure of North Adams Regional Hospital. Half the remaining workforce is over 55, poised to retire as an aging population (20-30 percent over 65) battles chronic ills — heart disease, diabetes, depression — at rates outpacing urban Massachusetts. Nationally, rural areas claim just 10 percent of physicians despite housing 20 percent of Americans. Here, that disparity yawns wider, a chasm between Boston's medical bounty and our western neglect.
Why this erosion? The culprits are legion. Rural PCPs earn $220,000 annually — $60,000 less than Boston counterparts — while juggling heavier loads with scant specialist support. Medical students, saddled with $250,000 in debt, shun primary care for lucrative specialties; only 15 percent of residents stick with it five years out. Recruitment falters as young doctors spurn isolation and harsh winters for urban vibrancy. Burnout, seared into 60-75 percent of clinicians post-pandemic, accelerates exits. Add a broadband lag — 15-20 percent of Berkshire households lack reliable internet — and telemedicine, a touted fix, stumbles.
The fallout is visceral. In Pittsfield, a retiree skips blood pressure meds, his last visit a memory from July 2024. In Greenfield, Baystate Franklin's ER chokes on non-emergent cases — hypertension, anxiety — because PCPs are phantoms. Health outcomes sag: rural heart disease deaths soar 15 percent above state norms; suicide rates, untended by a skeletal mental health network (one psychiatrist per 10,000), climb 30 percent since 2010. Economically, small businesses bleed workers to untreated illness; property values stall as healthcare deserts repel newcomers.
Politically, this transcends partisanship, yet it's mired in it. Gov. Maura Healey's administration touts the Physician Pathway Act — signed January 2025 to fast-track international doctors into underserved areas — but rural rollout lags. Republicans decry urban-centric spending, pointing to $425 million diverted to migrant housing amid a $1 billion FY26 deficit. Both sides have merit: progressives prioritize equity, conservatives fiscal prudence. Neither has stanched the bleeding here.
Solutions demand innovation beyond stale debates. First, reimagine incentives. Massachusetts could pioneer a "Rural Residency Bonus" — $75,000 annually for PCPs committing five years west of Worcester—funded by taxing second-home buyers inflating Berkshire housing costs. Pair this with a "Telemedicine Equity Fund," redirecting a sliver of urban hospital profits to rural broadband, ensuring virtual care isn't a privilege of the connected.
Second, flip the training paradigm. UMass Chan Medical School's rural track trains 10-15 students yearly, but most drift eastward. Mandate half serve western counties post-residency, bolstered by a "Community Preceptor Network" where retiring PCPs mentor successors, preserving institutional knowledge. Federally, HRSA grants could triple rural residencies here if Healey lobbies Trump's incoming administration, leveraging his rural voter base.
Third, empower communities. Berkshire Health Systems, straining under a $10 million deficit, could seed "Healthcare Co-ops" — towns pooling resources for shared NPs and mobile clinics. Tax credits for local businesses sponsoring these units would spur investment, marrying economic vitality to health access.
Critics will cry cost. Yet inaction's price — lost lives, hollowed towns — dwarfs any budget line. The Physician Pathway Act promises 50-100 doctors by late 2025, but without rural focus, they'll cluster near Springfield. Spring's Lyme season and winter's COPD spikes loom; delay is death.
This isn't Boston's crisis to solve alone. It's ours — readers of iBerkshires.com, voters, neighbors. Demand Healey prioritize western equity, not just urban optics. Press lawmakers to fund rural lifelines, not merely point fingers. Our hills deserve more than nostalgia; they deserve a pulse. Let's prescribe survival — together.
Ronald Beaty
Barnstable, Mass.
--------------------
https://www.masslive.com/news/2025/09/why-your-local-pharmacy-might-be-the-next-to-disappear-as-massachusetts-has-lost-nearly-300-since-2010.html
--------------------
"Nonprofit Raising Awareness of Rare Cannibis-Related Condition"
By Breanna Steele, iBerkshires Staff, September 27, 2025
PITTSFIELD, Mass. — The Stephanie Rose CHS Foundation is raising awareness of a rarely known condition.
Cannabinoid hyperemesis syndrome is an often misdiagnosed condition in someone who may use cannabis consistently over a long period of time. According to the Cleveland Clinic, up to 33 percent of frequent cannabis users seeking emergency room care displayed its symptoms of nausea, intense abdominal pain and vomiting. This can cause dehydration, loss of appetite, electrolyte imbalance and kidney failure.
Cannabis is often used to reduce pain and nausea and promote the appetite, especially with those undergoing chemotherapy. CHS does the opposite.
The syndrome was first reported in 2004 but has more frequently been diagnosed with the legalization of marijuana. The first deaths from conditions related to CHS were reported in 2016.
The Stephanie Rose CHS Foundation was started in June in memory of Pittsfield native Stephanie Rose Whipple, who was diagnosed with CHS and passed away from cardiac arrythmia last year at age 28.
"Most people with this condition, they don't even realize that they have it. There's not a lot of information or an awareness. So our loved one, Stephanie, she suffered with this for years, and she was diagnosed once by a doctor," said the foundation's treasurer and Whipple's aunt, Brittany Garcia.
Garcia and Alyssa Farella, Whipple's older sister and foundation president, said the family had not known about the syndrome, explaining there's not a lot of information about CHS.
"I just want people to know the risk factors, and I want Stephanie's death to have meaning where she loved helping people," Farella said. "She worked with the elderly, she did activities in a nursing home with elderly, and everything, she was very dedicated to helping people. So I feel like this continues her legacy of doing that to help."
The two want it to be known that they are not telling people to stop using cannabis, which doctors say is the only option now, but to simply inform them of the risks and to be a support for those who may have been touched by the syndrome.
"We're not trying to knock it. We're just showing that someone that we cared about passed away very young because of this. And if we can help anyone else and be there to support ... that's our mission," Garcia said.
The nonprofit is raising funds to invest into CHS education and research and to, hopefully, find a cure.
"Our donations are going towards research. I've looked into the Mayo Clinic. They do a lot of test studies on people that are experiencing CHS, and they have age ranges from like 18 all the way to people in their 70s, elderly people dealing with the effects. So a portion of the donations are going to research to find out find a cure for this," Farella said.
The foundation is holding its first event on Oct. 19 at Greenridge Park in Dalton from 1 to 4 p.m. People will be able to carve pumpkins, enjoy raffles, and more to celebrate Whipple.
"October is a very special month. Stephanie would turn 30 on Oct. 1. She loved all fall things. So this is a good time of year to really honor her," Garcia said. "She loved pumpkins, she went pumpkin picking with us and our little ones and she just loved all fall things. So we really want to do something that represents her birthday."
The foundation hopes to share Whipple's story with the local community and around the world.
"I want to reach other people. I want people that live in another state, that have lost someone. I want them to see this article and to see this and go, 'Oh my gosh, like I know someone that struggles with that,' read Stephanie's story, be inspired and to pass it along to another grieving mother or sister or aunt. I want to reach out not just our small circle, but I want other people to see this and go, 'Oh my gosh, this is real,'" Garcia said.
The family also wants to make sure Whipple is never forgotten.
"We want to put our grieving into something good, something that'll keep her name alive, because that's something we've always worried about, too, is she'll be forgotten," Farella said. "This is a way that she won't be and it's a way that we can take her sickness that she had and help others do good out of it."
--------------------






































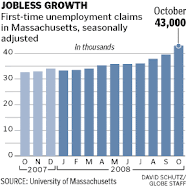







































































































.png)












































































































































































































































































No comments:
Post a Comment