-
http://health.nytimes.com/health/guides/disease/cancer/overview.html?scp=1-spot&sq=cancer&st=cse
-
The Boston Globe, Op-Ed
SUSAN HOCKFIELD: "Gaining ground on cancer"
By Susan Hockfield, April 28, 2008
IN 1971, President Nixon launched the War on Cancer, with the optimistic goal of defeating the disease in eight years with $100 million. More than 35 years and $79 billion later, the war is far from won. While 2002 marked the first-ever yearly decline in US cancer deaths, more than 40 percent of Americans will still contract cancer in their lifetime. What's more, although effective therapies have emerged for some cancers, other types stubbornly resist therapy, and many patients find treatment itself debilitating.
Given the scale of the problem, advocates like Lance Armstrong call for increased federal funding for cancer research. But, if we have spent so much without defeating the disease, why should we think that further spending will finally conquer the 200 or more diseases we now know as cancer?
There are two reasons. First, fundamental research takes time, sometimes decades, and we are only now reaping some of the rewards of the fundamental work triggered by the War on Cancer. The drug Herceptin offers highly effective therapy for women with one type of breast cancer; its development depended on molecular discoveries made at MIT in 1979, amplified and extended by the work of researchers at many institutions since.
The second reason to be optimistic about progress on cancer is that recent innovations have dramatically accelerated cancer research.
In the early 1990s, when fundamental research in my own neurobiology lab opened a new approach to primary brain cancer, gains came slowly, one protein or one gene at a time, and depended on experimental systems that only partially mimicked human disease. Today, thanks to new technologies, researchers collect and analyze more data in a year than their mentors could in a whole career. Startling new tools from chemical, biological, and nano-scale engineering have dramatically shortened the road to new discoveries and new therapies - as we have seen already in revolutionary cardiac treatments like drug-eluting stents.
With these capabilities, we can finally tackle persistent problems in cancer treatment and detection: attacking the tumor specifically, rather than flooding the patient with drugs toxic to normal tissues as well as cancer; or detecting recurrence, not at scheduled check-up intervals, but when the tumor starts making new cells. At last, through the combined powers of biology and technology, we can start to talk seriously about doing for cancer what we have done for AIDS - transforming it from a terminal disease to a treatable chronic condition.
At MIT and elsewhere, for example, researchers are building a new class of anti-cancer "smart bombs," nanoscale particles filled with cancer-fighting drugs and covered with homing molecules that direct them exclusively to cancer cells. By leaving healthy cells untouched while delivering anti-cancer drugs directly to a tumor, these nanotherapies hold the promise of more effective treatments at much lower doses, with a dramatic drop in side effects like nausea, fatigue, and hair loss.
Other MIT research teams are developing minute sensors to lodge at the site of a tumor during surgery. If the cancer recurs, the sensor will detect it at the level of just a few cells, eliminating the agonizing uncertainty between doctor visits and allowing treatment to begin immediately.
New strategies like these are profoundly exciting, but further progress against cancer, at MIT and at leading hospitals and universities around the country, will depend on how much we are willing to pay for it. Federal and industry funding, along with farsighted private philanthropy, have fueled cancer research. Unfortunately, funding for the National Cancer Institute has been flat for the past four years. Further progress will require further investment.
In these increasingly difficult economic times, we rush to ask, "What would it cost?" A better question is "What would it return?" In 1980, HIV-AIDS did not even have a name; soon after, it was projected that AIDS patients would fill every bed in every hospital in America. NIH moved into action, investing $15 billion in research. That's a lot of money. But as Dr. Elias Zerhouni, director of the National Institutes of Health observes, that investment saved $1.4 trillion in hospital costs and has given AIDS patients the possibility of a normal life span.
In the same way, for cancer, in all its permutations, there will be only one cure: research.
-
Susan Hockfield, a guest columnist, is the president of the Massachusetts Institute of Technology.
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/04/28/gaining_ground_on_cancer/
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/04/28/gaining_ground_on_cancer?mode=PF
-
----------
"Kennedy has major cancer bill in Senate"
By Andrew Miga, Associated Press Writer, May 27, 2008
WASHINGTON --Sen. Edward Kennedy's battle with a malignant brain tumor is likely to put a dramatic personal stamp on a health care cause he first championed nearly 40 years ago: The nation's war on cancer.
Kennedy had already begun work on an overhaul of the 1971 National Cancer Act when his tumor was diagnosed, and advocates hope the fact that Kennedy has fallen victim to this disease will generate public support and lend new urgency to the need to update the bill.
"People think of Ted Kennedy as a fighter and as someone who has always been there for everyone," said Daniel E. Smith, president of the American Cancer Society Cancer Action Network, the American Cancer Society's advocacy arm. "The fact that he now is fighting this disease is a jolt. It's a wake-up call to everyone."
"With that diagnosis, the irony for us is Senator Kennedy has been one of our great champions," Smith said.
The 76-year-old Kennedy has been a prominent and passionate advocate of cancer research and other health care issues throughout his long tenure in the Senate.
His name has become virtually synonymous with the push for universal health care coverage. He was a leader in enacting several landmark bills, including the Americans with Disabilities Act of 1990, the State Children's Health Insurance Program and the Kennedy-Kassebaum bill protecting workers from losing health insurance when they switch jobs, or from being denied coverage due to pre-existing conditions.
He's been instrumental in promoting biomedical research, AIDS research and treatment, a national bone marrow donor registry and anti-tobacco bills.
"With his legacy in health care, this could be an incredible crowning achievement for him," said Hala Moddelmog, a breast cancer survivor and president and CEO of the cancer-fighting foundation Susan G. Komen for the Cure. "I really think people will rally behind it, I really do. I think they already were starting to -- and this will just bring it home to people."
Kennedy, who has been working closely with Republican Sen. Kay Bailey Hutchison of Texas, plans to file the legislation in the coming weeks, an aide said Friday. As one of the Senate's shrewdest legislators and dealmakers, Kennedy is known for joining forces with Republicans to win passage of major bills.
"His work is pretty much unparalleled in the area of cancer in many ways, and we're excited about the possibility of this bill moving forward because he wants to address cancer in a comprehensive way," Smith said.
The bill Kennedy plans to put forth seeks to improve the coordination of cancer research, prevention and treatment while giving more money to the National Cancer Institute and other public research agencies.
Congress is on a Memorial Day recess, and it is unclear when Kennedy, chairman of the Senate Health, Education, Labor and Pensions Committee, will be back on Capitol Hill. He returned to his family's Hyannis Port, Mass. compound last week after being released from Massachusetts General Hospital in Boston.
Kennedy emerged as a leader in winning passage of the National Cancer Act after he became chairman of the Senate's health subcommittee in 1971. At the time, there was wide concern about cancer as the nation's second leading cause of death.
His family has been touched by cancer over the years -- two of his children, Kara and Edward Kennedy Jr., are cancer survivors. Edward Kennedy Jr. lost a leg to bone cancer in 1973 at age 12, and Kara was diagnosed with lung cancer five years ago.
Both were given a 15 percent chance of survival, but are cancer-free now. The senator threw himself into their care, finding the best medical advice and treatment options for them.
A few weeks ago, Kennedy and Hutchison teamed up with seven-time Tour de France winner and cancer survivor Lance Armstrong at a Senate hearing and a news conference calling on Congress and the country to step up the fight against cancer. The events were aimed at building support for the bill. Kennedy mentioned how his children overcame the disease.
"This is personal for all of us," said Armstrong, who has worked closely with Kennedy on the bill.
When Kennedy's diagnosis was revealed, Armstrong said renewing the fight against cancer would be a good way to honor the senator.
"The timing of this news comes just as Senator Kennedy is leading the creation of bipartisan legislation to renew the fight against a killer that claims more than 560,000 American lives every year," Armstrong said in a written statement. "And in honor of Senator Kennedy, the time for a national call to action in the war against cancer is now."
--
On the Net:
On the Net: Kennedy: http://kennedy.senate.gov
Health, Education, Labor and Pensions Committee: http://help.senate.gov
----------
"Childhood cancer rates are highest in Northeast, study finds"
By Lindsey Tanner, Associated Press, June 2, 2008
CHICAGO - New research suggests that childhood cancer is most common in the Northeast, results that caught scientists off-guard.
The large government study is the first to find notable regional differences in pediatric cancer. Researchers say it also provides important information to bolster smaller studies, confirming that cancer is rare in children, but also more common in older children, especially among white boys.
The study from the Centers for Disease Control and Prevention is based on data representing 90 percent of the US population. It found that cancer affects about 166 out of every million children, a number that shows just how rare childhood cancers are.
The highest rate was in the Northeast with 179 cases per million children, while the lowest was among children in the South with 159 cases per million.
The rates for the Midwest and West were nearly identical, at 166 cases per million and 165 cases per million, respectively. The cancer incidence in boys was 174 cases per million, compared with 157 cases per million in girls. In white children, the rate was 173 per million, versus 164 per million in Hispanics and 118 per million in African-Americans. A total of 36,446 cases were identified in the study, which analyzed 2001-03 data from state and federal registries. The research appears in the June edition of Pediatrics, which was being released today.
"It's very powerful that this study includes so much of the US population so it gives us a good picture of where we are with the incidence of these childhood cancers," said Elizabeth Ward, the American Cancer Society's surveillance director.
Researchers said the regional differences, though small, are intriguing, but that reasons for them are uncertain.
Dr. Lindsay Frazier, a cancer specialist at Children's Hospital and the Dana-Farber Cancer Institute in Boston, said pollution and housing stock that's older than anywhere else in the nation might help explain the Northeast's higher rates.
----------
"Test can find tiny tumor level in blood: MGH method gives new treatment tool"
By Stephen Smith, (Boston) Globe Staff, July 3, 2008
Boston researchers have developed a test that can identify minute amounts of tumor cells floating in the blood of cancer patients, a discovery that could lead to better treatments with fewer side effects.
The technology, invented at Massachusetts General Hospital, uses a microchip scanner no bigger than a business card to analyze a patient's blood, hunting for stray cells shed by tumors. The device is so powerful that it can detect a single cancer cell among 1 billion healthy blood cells.
Once those cells are captured, their genetic fingerprints can help determine the most effective drug for a patient whose cancer has already begun spreading, and also show whether medication has lost its power. The technology is now being tried in patients whose cancer has already spread, but scientists hope in the fu ture the chip will be able to detect cancer's spread before secondary tumors have become established.
Although the device is not yet ready for widespread use, a report posted online yesterday by the New England Journal of Medicine showed that it successfully identified migrating cancer cells in lung cancer patients and spotted important genetic quirks in those cells.
Scientists not involved with the research said the innovation represents a significant improvement on existing cancer blood tests and predicted that it could revolutionize treatment, especially for lung cancer, which kills more Americans than any other cancer.
Mass. General's approach brings together two of the hottest fields in cancer research: the incredibly tiny devices of nanotechnology, and personalized medicine - tailoring treatments to individual patients.
"To me, as a scientist, this is huge," said Dr. Shakun Malik, director of the lung cancer program at Georgetown University's Lombardi Comprehensive Cancer Center in Washington, D.C. "To be able to just do a blood test, that opens a whole new, wide world."
For decades, physicians have relied on biopsies and medical snapshots such as CAT scans to track the progress of cancer, but both approaches carry significant limitations.
Doctors, for example, can conduct repeated biopsies, using a needle to extract chunks of a tumor. "But those biopsies are associated with significant risks, particularly if we're looking at a lung cancer buried deep in the lung," said Dr. Charles Rudin, a cancer specialist at Johns Hopkins University in Baltimore. "The risks can be bleeding, infection, collapse of the lung, shortness of breath."
And while high-tech scans can show whether a tumor is growing or shrinking, it can take a couple of months for that change to be evident on a scan. And an image cannot explain what is happening at a biological level, such as whether tumor cells are mutating. As a result, doctors try a hit-or-miss approach, leaving patients on treatments without always having a clear sense of how well those approaches will work.
"So we unfortunately have exposed those patients to drugs that have side effects, are costly, and have wasted the patient's time, and many of these patients don't have time," said Dr. Joan Schiller, deputy director of the cancer center at the University of Texas Southwestern Medical Center in Dallas. "They don't have time to try this, try that, try this, try that, hoping that you will eventually hit upon something."
The new research, underwritten by a $5 million federal grant and additional money from foundations, is an attempt to do for cancer what scientists had done for AIDS and other illnesses: develop an easy-to-use, highly sensitive treatment scorecard. If the number of cancer cells in the bloodstream falls, treatment is probably working. If they increase, it means the tumor is growing, and suggests the need for a new approach. The tiny device has 78,000 posts imbedded inside to trap cancer cells. Each of those posts is coated with a substance that acts like glue - glue designed to stick only to circulating tumor cells, known by the acronym CTC.
"It's like a pinball machine - the blood has to flow through all of these columns to get to the other side," said Dr. Daniel Haber, director of the Mass. General Hospital Cancer Center and senior author of the study. "All the normal blood cells flow right through, but the very, very rare cancer cells stick to the columns."
The technology, known as the CTC-chip, has been shown to accurately identify bloodstream cancer cells in patients with advanced cancer of the lung, prostate, pancreas, breast, or colon.
In the new study, researchers focused on non-small-cell lung cancer, the deadliest form of the disease. Overall, lung cancer kills more than 160,000 Americans annually, accounting for 29 percent of all cancer deaths.
The Mass. General team took blood from 27 lung cancer patients. In each, the chip technology accurately detected circulating tumor cells.
And then they looked for crucial genetic mutations that would suggest particular treatments. By confirming with biopsied tissue, the scientists found that their test detected all the important genetic features they had sought.
"Someday, we might pick our cancer drugs like we pick our antibiotics," said Dr. Roy Herbst, a lung cancer specialist at M.D. Anderson Cancer Center in Houston.
The Mass. General device can find more cancer cells than an existing technology and does so while the cells are alive, according to the Boston researchers and other scientists. By isolating living cells, doctors could ultimately grow copies for further testing.
Veridex LLC of New Jersey makes a cancer blood test used in patients with advanced breast, colon, or prostate cancer. A Veridex executive said while he was familiar with Mass. General's claims about the superiority of its test, he could not verify the assertion.
The Mass. General technology needs to be tested in larger groups of patients before it can be used routinely, and Haber said scientists need to speed up the device's ability to process samples - right now, it takes about eight hours to run a blood sample and analyze it.
-
Stephen Smith can be reached at stsmith@globe.com.
-
----------
"Cancer blogs become part of treatment: Patients can update loved ones, vent"
By Neil Munshi, (Boston) Globe Correspondent, August 20, 2008
Two months after learning she had breast cancer, Jennifer Boyd found herself sitting in the back room of a Newbury Street salon, picking out wigs to replace her thick, sandy-brown hair, stolen in bunches by chemotherapy.
She recounts the ordeal, for all the world to read, in a blog.
"When do I buzz it all off? The downside to all this hair is that there is so much more to fall out and get everywhere," she wrote on May 10, 2007. "The woman at the salon where I bought a wig last week said I would know the right time. And I'm still not ready yet."
Boyd is one of a growing number of cancer patients turning to the Internet to discuss their disease, keeping friends and family updated, and connecting with other patients, according to oncology social workers and psychologists. Personal blogs, listservs, and sites like CarePages, CaringBridge, and Breast Cancer Stories give patients an outlet to express the emotional turmoil associat ed with the disease, enabling a virtual catharsis for some.
That was the role blogging played for Robert and Donna Gregory, the Long Island couple who died when the plane ferrying them to Boston for medical treatment crashed last week. Donna Gregory chronicled how leukemia had affected her husband's health and the lives of herself and the couple's twins.
And Leroy Sievers, a former television newsman who died last week of colon cancer, gained an extensive following with a blog and commentaries presented by National Public Radio.
While there hasn't been much research done on the relatively recent phenomenon, patients attest to its many benefits. And two Ohio State University researchers, conducting one of the first studies on cancer patient blogs, said their preliminary findings suggest that online journals indeed help.
"It's definitely not hurting these folks . . . it's a good means to express yourself," said one of the researchers, Jennifer Moreland, who is earning a master's of health communication. "These folks will look back over the last few years and say: 'Look at what I've come through. Hopefully, someone else can read this and survive as well.' "
After analyzing 50 blogs, the researchers found that detailing the rigors of the illness online seemed to help patients cope.
While research on cancer patient blogging may be scant, studies on the healing effects of writing are abundant, said Harriet Berman, a clinical psychologist with the Wellness Community-Greater Boston, a nonprofit that provides support and counseling free to cancer patients and their families. "There's a very empowering process that goes on when cancer becomes something you can write about. It's not just this thing that's invaded you," she said.
But, Berman said, blogging does have its downside. "The danger to the individual, I suppose, is that some people could expose themselves more than they maybe want to," she said. "But I think the danger is more in the potential misinformation" to other patients, who might read the blog before they themselves reach such a point in the course of their illness.
Boyd's husband, Bryan Harter, urged his wife to start a CaringBridge page after hearing about the site at the Dana-Farber Cancer Institute, where he works as an oncology social worker. The sites, which can be password-protected, allow caregivers and patients to give frequent updates without fielding dozens of phone calls, he said, but they also provide the patient with an emotional outlet. "It really causes you, in the midst of having the rug pulled out from under you, to think about what you want to say and what you want people to hear," he said.
Boyd, 37, said she remembers writing and rewriting that wig post.
"The first version was probably my own cathartic dumping out of all my own feelings," said Boyd, of Jamaica Plain. "And I remember realizing . . . I could edit it a little bit and still get out some of those feelings without overwhelming people, but also letting people know it was really tough."
Boyd said she appreciated friends and family - including friends of friends and distant relatives - posting hundreds of notes of support. That's exactly what Christin Gachowski Martin, a Dana-Farber leukemia patient, uses her CaringBridge page for.
"It's been great for me, because when you're sick, it's tough to reach out to your friends individually," said Gachowski Martin, 48, of Clinton, N.Y., whose postings have logged 14,000 hits. "With this, you write one message and people respond with all these really beautiful things - it's really uplifting."
While that connection to loved ones is important, linking into a community of fellow bloggers in similar straits can also be critical, said Tim Cummings, a Wellness Community social worker. "When you get cancer, you've descended into a foreign country where you don't know the language and you don't know how to get around," he said. "And one of the ways you learn to do that is being able to talk to people who are members of this world."
David Hahn, 27, couldn't find those people when he was diagnosed with Hodgkin's lymphoma in July 2005. He Googled Hodgkin's and came upon scientific and medical information, but nothing detailing what he might eventually endure.
"After a while, you become more interested in the experience of the cancer than in the science of the cancer," said Hahn, a professional pianist. "You start to move past what the disease is, and you start to wonder what the disease will be like."
So he created "Chronicle of a Cancer Patient" and started writing, constantly, during his six months of chemotherapy and year of recovery. He did it to help himself, said Hahn, who lives in Norfolk, Va., and "in case there were others out there who wanted to know about the experience of cancer."
One of them turned out to be a childhood friend, Courtney Bugler, diagnosed with breast cancer just months after Hahn completed chemotherapy. He encouraged her to start her own blog, and the former "All My Children" script writer began "Biography of Breast Cancer." In it she leavened her cancer stories with humor, once comparing a nervous breakdown in the shower to "Tori Spelling in a Lifetime movie."
"I realized about four or five months into it that I had become part of this greater blogging community," said Bugler. She continues to be part of that community, not only in her day job with an advocacy group for young breast cancer patients, but in blog posts to new breast cancer patients.
"It's not that I'm stuck in the past and I'm not willing to move on," she said. "I've just come to accept that breast cancer in some way, shape, or form, will always be a part of my everyday life."
----------
"Breast Cancer Awareness Month - Healing through art: The Think Pink exhibit moves to the Colonial Theatre."
By Jessica Willis, Berkshire Eagle Staff
Wednesday, October 01, 2008
PITTSFIELD, Massachusetts
The message is about laughter and hope, and the outlook is rosy. Think Pink, the city's art show for breast cancer awareness, opens Friday at the Colonial Theatre.
The three-day exhibit, titled "Healing and Humor," features more than 50 pieces made by local artists and breast cancer survivors. The show, now in its fifth year, is a collaboration between the county's Breast Health Team, an affiliate of the American Cancer Society and the Storefront Artist Project.
This year marks the first time Think Pink has exhibited at the Colonial; for the past several years, the exhibit has packed them in at the much smaller Lichtenstein Center for the Arts on Renne Avenue.
"We just outgrew the space," said Linda M. Ruberto, Think Pink's co-chairwoman and a member of the Breast Health Team. "Every year, we have more and more art."
About 40,000 American women die from breast cancer each year, Ruberto said, adding that annual mammograms for women 40 and older, and early detection, are two of the best defenses against the disease.
Ruberto was diagnosed with Stage I breast cancer 10 years ago, at the age of 50. Since her surgery in 1998, she has been cancer-free.
"Thank goodness I didn't stop getting mammograms," she said. "They saved my life."
October is Breast Cancer Awareness Month.
Think Pink artwork includes whimsical photographs like Susan Geller's "Pretty in Pink," featuring a trio of girls wearing fuzzy hats of a certain hue, and Julie McCarthy's black and white portraits of cancer survivors laughing or lost in thought.
Julie Edmonds' oil on canvas, "Diane at the Co-Op," is a rendering of a Berkshire County everywoman: Lank gray hair, no-nonsense look on her face, sandals and long skirt.
"I saw (Diane) at the Co-Op Market in Great Barrington, looked at her in her pink tank top, and I knew I had to paint her for Think Pink," Edmonds said.
For Connie Caldes, Think Pink co-chairwoman and a six-year breast cancer survivor, lightheartedness is some of the best medicine.
"It's very difficult to recover from cancer without humor," Caldes said yesterday, watching Edmonds and Storefront Artist Project volunteers hang the work in the theater's lobby. "When someone is a new survivor, you can't expect to have humor, but eventually it comes back. When that happens, it shows you're healing."
-
To reach Jessica Willis: jwillis@berkshireeagle.com, (413) 528-3660.
-
----------
"Kennedy returns to Senate: Pushes healthcare amid personal battle"
By Susan Milligan, Boston Globe Staff, November 18, 2008
WASHINGTON - A beaming Senator Edward M. Kennedy returned to work in Washington yesterday, exactly six months after confronting a grave threat to his health, and declared himself ready to help lead an aggressive push for healthcare reform.
"I feel fine," the Massachusetts Democrat said, flanked by his wife, Vicki, and his two Portuguese water dogs, Splash and Sunny, as he entered a staff meeting to a roar of applause in the ornate Russell Caucus Room on Capitol Hill. "I'm looking forward to the session . . . I'm looking forward, particularly, to working with Barack Obama on healthcare," the 76-year-old veteran lawmaker told reporters.
Kennedy steadied his walk with his father's cane - the same cane the senator used after surviving a 1964 plane crash, and which he has lent to two of his colleagues, Senators Chris Dodd of Connecticut and John Warner of Virginia - and his voice trembled slightly when he spoke. But overall, Kennedy looked remarkably spry for a man battling a malignant glioma, a fast-growing brain tumor that was diagnosed after Kennedy had a seizure in May.
His color was strong, and he sported a full head of his characteristic white hair. He appeared to have lost a substantial amount of weight and displayed none of the puffiness he showed during his last ap pearance on Capitol Hill on July 9, when he made an emotion- laden visit to cast a critical vote on a Medicare funding bill.
While the senator is still receiving treatment, he didn't look tired as he prepared to get to work on issues facing the incoming Congress, with healthcare as his stated top priority.
"We're hopeful this will be a prime item on the agenda," Kennedy said. Asked whether he expected President-elect Obama to sign a healthcare bill early in his term, Kennedy responded, "Yes."
In the Russell Caucus Room Kennedy was greeted by a large banner that said "Welcome Back Senator!" and a round of applause heard well beyond the closed doors of the room. The 100 or so personal Senate office aides and committee staffers lunched on food from Legal Sea Foods - a favorite of the Massachusetts delegation - as they discussed the upcoming agenda.
Kennedy plans to work several hours a day from his Washington home and expects to be in the Senate this week for the special session, an aide said. Yesterday's appearance marked the first time that many people in the Capitol - including Kennedy's colleagues - had seen the Massachusetts lawmaker since his July vote to restore planned cuts in Medicare payments to doctors.
Kennedy also spoke at the Democratic National Convention in August, delivering a passionate endorsement of Obama and an appeal for healthcare reform and civil rights even as he fought back the pain from a kidney stone he had passed just hours before he spoke. Kennedy had been among the most influential Democratic elders to embrace Obama during his primary race showdown with Senator Hillary Clinton of New York.
Kennedy did not meet with his Senate colleagues yesterday, but was greeted by a delighted Boston-born Capitol police officer as he entered the building. He chatted briefly with Representative Jesse Jackson Jr., an Illinois Democrat interested in taking over Obama's Senate seat, when Jackson and Kennedy ran into each other in the hallway.
"He's pumped and ready," Senator John F. Kerry said of his Massachusetts colleague's return. "This is so super-exciting. I just feel emotional about it."
Kennedy has continued to conduct Senate work from his home in Hyannis Port, working with Health and Human Services Secretary Michael O. Leavitt to extend the federal rules allowing Massachusetts to continue its healthcare plan and crafting a major national service program with Kennedy's colleague and friend, Senator Orrin Hatch, a Utah Republican. Kennedy has also held video conferences with his staff and fellow members of the Senate Health, Education, Labor, and Pensions Committee, which Kennedy chairs, to discuss the panel's upcoming agenda.
Kennedy moved back to his Washington home from the Cape last month when the weather turned colder and his beloved sailing season ended.
While some of Kennedy's colleagues have worried he would not return to the Senate, Kennedy has been adamant about playing a role in moving quickly on the universal healthcare he has spent several decades trying to achieve. Not only is he aware of the potential limits of his own health, but he also wants to exploit the opportunities offered by Democratic control of the White House and Congress in January.
Senate aides said he declined a request by Clinton to create a subcommittee that would allow her to lead the effort, indicating that he felt well enough to spearhead the task. Since that request, Clinton has become a contender for secretary of state, which would take her out of the healthcare debate on Capitol Hill.
The Senate this week is expected to extend unemployment benefits to respond to the escalating jobless rate. Democratic lawmakers are hoping to reach agreement on some plan to help the embattled auto industry. A push for a broader stimulus plan appears nearly dead, since President Bush and GOP senators are opposed to it.
An automobile package is still possible, although lawmakers disagree on the details. Democrats want to take $25 billion from the $700 billion allocated for a financial services industry bailout, while leading Republicans want the money to come from an existing Energy Department program.
"We're going to be dealing with this later in the week," Senate minority leader Mitch McConnell, Republican of Kentucky, said yesterday, indicating that there was room for negotiation.
----------
"New Screening Could Lead to More Potent Cancer Drugs"
By NICHOLAS WADE, The New York Times, August 14, 2009
Researchers have discovered a way to identify drugs that can specifically attack and kill cancer stem cells, a finding that could lead to a new generation of anticancer drugs and a new strategy of treatment.
Many researchers believe that tumor growth is driven by cancerous stem cells that, for reasons not yet understood, are highly resistant to standard treatments. Chemotherapy agents may kill off 99 percent of the cells in a tumor, but the stem cells that remain can make the cancer recur, the theory holds. Stem cells, unlike mature cells, can constantly renew themselves.
A practical test of this theory has been difficult because cancer stem cells are hard to recognize and have so far proved elusive targets. But a team at the Broad Institute, a Harvard-M.I.T. collaborative for genomics research, has devised a way of screening for drugs that attack cancer stem cells but leave ordinary cells unharmed.
The Broad team, lead by Piyush B. Gupta, screened some 16,000 chemicals, including all known chemotherapeutic agents approved by the F.D.A. The team reports in Thursday’s issue of Cellthat 32 of the chemicals selectively targeted cancer stem cells. These particular chemicals may or may not make good drugs, but the screening system proves for the first time, the researchers say, that it is possible to target cancer stem cells with drugs that leave ordinary cells alone. Only one of the 32 chemicals is approved as a drug for cancer..
Another approach to targeting cancer stem cells, based on the use of antibodies, was reported this month by OncoMed Pharmaceuticals, a company founded by Michael F. Clarke, a Stanford researcher who in 2003 discovered cancer stem cells in breast tumors.
If effective drugs against cancer stem cells can be developed, one obvious strategy would be to use them in combination with standard chemotherapeutic agents, so that all types of cells in a tumor could be attacked. In that way, cancer would be attacked as AIDS now is, with a cocktail of chemicals that blocks all escape paths. Both the AIDS virus and cancer cells can change their DNA to dodge an effective drug, but are thought to perish if confronted with many drugs at the same time.
Standard chemotherapy is often effective because the chemicals are applied in such large doses that they kill all cells. But this scorched-earth policy is stressful for the patient.
“You could probably lower the doses considerably with a combination of drugs that attached specific types of cell,” Dr. Gupta said.
Eric S. Lander, director of the Broad Institute, said: “If we make a drug that kills 99.9 percent of the cells in a tumor but fails to kill the 0.1 percent, that is the real problem. It’s a pyrrhic victory.”
Mr. Lander said that, given the new drug screening system and the idea of using combinations of drugs against cancer, “there is a potential for a real renaissance in cancer therapeutics.”
“We have not been able to do that yet with cancer,” he said, “but, if we could, it’s a numbers game, and we win.”
The cancer stem cell theory has been thrust into the spotlight in the last five years with the discovery of stem cells in many different types of solid tumors, including those of the breast, brain, prostate, colon and pancreas. This month, a Stanford team led by Irving Weissman reported finding the stem cells of bladder cancer.
But the theory is not without critics.
“The cancer stem cell hypothesis has in the past year been challenged on many fronts,” said Bert Vogelstein, a leading cancer geneticist at Johns Hopkins University. “For example, a paper on melanomas last year showed that 100 percent of melanoma cancer cells were cancer stem cells.”
If many of a tumor’s cells are stem cells, then existing chemotherapy agents are clearly killing them, Dr. Vogelstein said, and the cancer stem cell theory is not an effective guide to finding new drugs.
The theory has also aroused opposition because, in its extreme version, it implies that standard chemotherapy goes after the wrong targets and is ineffective.
“It’s the most amazing polarity that I’ve seen,” Dr. Clarke said of the debate over stem cells among cancer researchers. “It’s like two religions fighting.”
Some advocates of the idea believe that to dissolve tumors, it would be necessary only to target cancer stem cells, if such drugs existed. But the Broad Institute team and others take the view that a combination of drugs attacking each of the different types of cells in a tumor would be the best strategy.
One reason for using a combination of drugs is the suspicion that mature cancer cells may be able to convert themselves back into stem cells, a route that is apparently prohibited to normal mature cells.
“The possibility is that the nonstem cells in a tumor may regenerate de novo new stem cells,” said Robert Weinberg, a leading cancer biologist at M.I.T. and, with Dr. Lander, a co-author of the Cell report. “If one had ways of treating both the stem cells and the nonstem cells, then the de novo generation of stem cells would be dealt with.”
The basic insight of the cancer stem cell theory is that there is a hierarchy of cells in a tumor, with the stem cells at the top generating the mature cells that are the majority. Most researchers accept that this is good description of leukemias because Gleevec, a highly effective drug for chronic myelogenous leukemia, does not kill the stem cells, and the leukemia returns if the treatment is stopped.
But with solid tumors, “the jury is out,” Dr. Vogelstein said. If stem cells are very common in solid tumors, not just a small resistant reservoir of cells, “then there’s no difference between the stem cells and the bulk cancer — so a screen for drugs to kill melanoma cells is by definition also going to kill the melanoma’s cancer stem cells.”
Still, in Dr. Vogelstein’s view, the Broad Institute’s new screening method is important whether or not the cancer stem cell theory is correct. “Because most of the compounds in use now clearly aren’t doing the job we’d all like,” he said, “then novel methods for screening could be extremely valuable.”
The Broad Institute researchers hope that pharmaceutical companies will use their screening method to begin the long road to develop drugs against cancer stem cells.
----------
"Double mastectomy doesn’t help most women, study shows"
By Lindsey Tanner | AP Medical Writer, September 02, 2014
CHICAGO — Removing both breasts to treat cancer affecting only one side doesn’t boost survival chances for most women, compared with surgery that removes just the tumor, a large study suggests. The results raise concerns about riskier, potentially unnecessary operations that increasing numbers of women are choosing.
The study involved nearly 200,000 California women treated for cancer in one breast and followed for several years afterward.
Ten-year survival rates were nearly identical — roughly 82 percent — for women who had lumpectomies to remove the tumor plus radiation, and for those who had double mastectomies. Women who had a single mastectomy, removal of just the cancerous breast, fared slightly worse.
The results confirm what many doctors have suspected, said Dr. Len Lichtenfeld, deputy chief medical officer of the American Cancer Society.
‘‘There’s no guarantee that by having the second breast removed that you will do better,’’ said Lichtenfeld, who had no role in the research.
In the study, just over half the women had lumpectomy treatment. But the number who had double mastectomies increased substantially to 12 percent between 1998 and 2011. The trend was most notable in women younger than 40, climbing from just 4 percent to 33 percent.
Other research suggests that removing both breasts to treat one-sided cancer may improve survival chances for the relatively small number of women who have genetic breast cancer or strong family histories of the disease, said study co-author Scarlett Gomez, a research scientist with the Cancer Prevention Institute of California. But most breast cancer patients have neither of those risks.
The medical community is paying increasing attention to over-treatment and excessive costs, and the study results raise questions about reasons for rising use of an expensive, potentially risky treatment ‘‘of dubious effectiveness,’’ the researchers said.
Patients’ preferences and fear that cancer will return play a role, but that fear ‘‘usually exceeds estimated risk,’’ the study said.
Reasons why survival was slightly worse for woman who had just one breast removed are uncertain, although this treatment is more common among Hispanic and black women and those with lower incomes and public insurance than among wealthy whites.
The study was published Tuesday in this week’s Journal of the American Medical Association. A journal editorial notes that the study echoes previous research and adds to a debate about the rising prevalence of double mastectomies.
The results may raise questions about whether surgeons, for financial reasons, are driving the trend, but that is unlikely, Dr. Lisa Newman, a surgery professor and director of the University of Michigan’s Breast Care Center said in the editorial.
‘‘A greater concern than financial incentives may be a surgeon’s preference based on his/her own experience, regardless of the data,’’ she wrote.
Patients should be given time to absorb a cancer diagnosis, and educated about treatment options, risks and benefits, before being pressed into decisions about irreversible surgery, Newman said.
Amy Curran Baker, an author from suburban New York City who chose a double mastectomy after her 2008 diagnosis, said her doctor presented her with options including lumpectomy. But he ultimately recommended the more invasive treatment because she had family members with breast cancer, and Baker said she doesn’t regret her choice.
‘‘I don’t think we can discount the importance of ‘peace of mind’ in a patient’s decision-making process,’’ said Baker, who wrote a book about mastectomy recovery. ‘‘We all work to heal ourselves psychologically in different ways and for some women this may be one of them.’’
Her cancer returned two years ago, in scar tissue from the operation on the breast where the disease first appeared, but Baker said she is doing well after chemotherapy and radiation.
The study authors examined data from the California Cancer Registry, part of a national cancer surveillance program. The data lacked information on how many women had genetic breast cancer or strong family histories of the disease.
__
Online:
JAMA: http://www.jama.com sboth
Breast cancer: http://tinyurl.com/28b6bs
___
AP Medical Writer Lindsey Tanner can be reached at http://www.twitter.com/LindseyTanner
----------
"Study shows yoga may reduce fatigue and inflammation for breast cancer patients"
By Deborah Kotz, Boston Globe Staff, January 31, 2014
At least one in three women diagnosed for breast cancer suffers from lingering fatigue months or even years after treatment ends, but practicing yoga significantly reduces this symptom and also helps lower levels of dangerous inflammation. That’s the finding of a new National Cancer Institute-funded clinical trial that randomly assigned 200 breast cancer survivors to take either a 90-minute hatha yoga class—a gentler form than the popular hot bikram yoga—twice a week for 12 weeks or to be in a control group that was waitlisted for the class.
At the end of the study published online Monday in the Journal of Clinical Oncology, those who practiced yoga reported about 50 percent less fatigue than those in the control group and had 20 percent lower levels of three proteins in the blood that are markers for inflammation. The proteins, generated by the immune system, are known to cause fatigue, headaches, and general malaise when we develop an infection—the body’s way of forcing us to get rest.
Excess inflammation has been linked to a higher risk of breast cancer recurrence and chronic diseases of aging such as diabetes, osteoporosis, and heart disease, according to study leader Janice Kiecolt-Glaser, a professor of psychiatry and psychology at The Ohio State University College of Medicine.
The more times women practiced yoga each week, the lower the levels of their tiredness and inflammation. What’s more, these benefits persisted three months after the study ended—presumably because many of the study participants were keeping up their yoga practice.
“Sleep was significantly improved in the women who did yoga, and that could be a major reason for the decline in their fatigue and inflammation,” said Kiecolt-Glaser. Many breast cancer survivors suffer from chronic insomnia, she added, often due to anxiety that persists after their diagnosis with a life-threatening disease.
“Studies show that some patients continue to have moderate-to-severe fatigue years after treatment,” states the National Cancer Institute website. Besides lack of sleep, anti-estrogen drugs like tamoxifen—given to many breast cancer patients for 5 to 10 years after their diagnosis to prevent a recurrence—can also contribute to fatigue, according to NCI.
Even in those without breast cancer, yoga has been shown to provide the same—or even bigger—mood-boosting effects than running and other forms of strenuous exercise. But newcomers to yoga also need to be careful not to overdo it since pushing too much, too fast, can raise the risk of injuries.
Breast cancer patients who are older or still recovering from surgery or chemotherapy could certainly benefit from the practice. Kiecolt-Glaser recommended starting with a hatha yoga class, a restorative form that focuses on gentle stretching and a period of resting meditation at the end.
----------
My other Blogs are: luciforo.blogspot.com & frankguinta.blogspot.com & aldermanpetersullivan.blogspot.com & I have also posted many comments on berkshireeagle.blogspot.com & I have also posted many comments on planetvalenti.com
Jonathan Melle

I turned 39 (2014)
Monday, April 28, 2008
Subscribe to:
Post Comments (Atom)
About Me

- Jonathan Melle
- Amherst, NH, United States
- I am a citizen defending the people against corrupt Pols who only serve their Corporate Elite masters, not the people! / My 2 political enemies are Andrea F. Nuciforo, Jr., nicknamed "Luciforo" and former Berkshire County Sheriff Carmen C. Massimiano, Jr. / I have also pasted many of my political essays on "The Berkshire Blog": berkshireeagle.blogspot.com / I AM THE ANTI-FRANK GUINTA! / Please contact me at jonathan_a_melle@yahoo.com
50th Anniversary - 2009

The Naismith Memorial Basketball Hall of Fame on Columbus Avenue in Springfield, Massachusetts.
Pittsfield Politics: Capitanio, Mazzeo agree on budget cuts, public safety

Paul Capitanio, left, speaks during Monday night's Ward 3 City Council debate with fellow candidate Melissa Mazzeo at Pittsfield Community Television's studio. The special election (3/31/2009) will be held a week from today (3/24/2009). The local issues ranged from economic development and cleaning up blighted areas in Ward 3 to public education and the continued remediation of PCB's.
Red Sox v Yankees

Go Red Sox!
Outrage swells in Congress!

Senate Banking Committee Chairman Sen. Christopher Dodd, D-Conn., left, and the committee's ranking Republican Sen. Richard Shelby, R-Ala., listen during a hearing on modernizing insurance regulations, Tuesday, March 17, 2009, on Capitol Hill in Washington. (AP Photo/Susan Walsh). - http://news.yahoo.com/s/politico/20090318/pl_politico/30833
Beacon Hill's $pecial Interest Tax Raisers & $PENDERS!

Photo Gallery: www.boston.com/news/local/massachusetts/articles/2009/03/15/St_Patricks_Day_Boston/
The path away from Wall Street ...

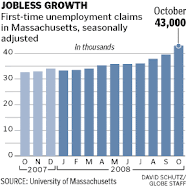
...Employers in the finance sector - traditionally a prime landing spot for college seniors, particularly in the Northeast - expect to have 71 percent fewer jobs to offer this year's (2009) graduates.
Economic collapse puts graduates on unforeseen paths: Enrollment in public service jobs rising...

www.boston.com/news/local/massachusetts/articles/2009/03/14/economic_collapse_puts_graduates_on_unforeseen_paths/
Bank of America CEO Ken Lewis

Should he be fired? As Bank of America's Stock Plummets, CEO Resists Some Calls That He Step Down.
Hookers for Jesus

Annie Lobert is the founder of "Hookers for Jesus" - www.hookersforjesus.net/home.cfm - Saving Sin City: Las Vegas, Nevada?
Forever personalized stamped envelope

The Forever stamp will continue to cover the price of a first-class letter. The USPS will also introduce Forever personalized, stamped envelopes. The envelopes will be preprinted with a Forever stamp, the sender's name and return address, and an optional personal message.
Purple Heart

First issued in 2003, the Purple heart stamp will continue to honor the men and women wounded while serving in the US military. The Purple Heart stamp covers the cost of 44 cents for first-class, one-ounce mail.
Dolphin

The bottlenose is just one of the new animals set to appear on the price-change stamps. It will serve as a 64-cent stamp for odd shaped envelopes.
2009 price-change stamps

www.boston.com/business/gallery/2009pircechangestamps/ -&- www.boston.com/news/nation/washington/articles/2009/02/27/new_stamps_set_for_rate_increase_in_may/
Red Sox v Yankees

Go Red Sox!
President Barack Obama

AP photo v Shepard Fairey
Rush Limbaugh lackeys

Posted by Dan Wasserman of the Boston Globe on March 3, 2009.
Honest Abe

A 2007 US Penny
Dog race

Sledding for dogs
The Capital of the Constitution State

Hartford, once the wealthiest city in the United States but now the poorest in Connecticut, is facing an uphill battle.
Brady, Bundchen married

Patriots quarterback Tom Brady and model Gisele Bundchen wed Feb. 26, 2009 in a Catholic ceremony in Los Angeles. www.boston.com/ae/celebrity/gallery/tom_gisele/
Mayor Jimmy Ruberto

Tanked Pittsfield's local economy while helping his fellow insider political hacks and business campaign contributors!
Journalist Andrew Manuse

www.manuse.com
New Hampshire Supreme Court Building

http://en.wikipedia.org/wiki/New_Hampshire_Supreme_Court
Economic State of the Union

A look at some of the economic conditions the Obama administration faces and what resources have already been pledged to help. 2/24/2009
President Barack Obama

The president addresses the nation's governors during a dinner in the State Dinning Room, Sunday, Feb. 22, 2009, at the White House in Washington. (AP Photo/Haraz N. Ghanbari).
The Oscars - 2/22/2009.

Hugh Jackman and Beyoncé Knowles teamed up for a musical medley during the show.
The 81st Academy Awards - Oscars - 2009

Hugh Jackman pulled actress Anne Hathaway on stage to accompany him during his opening musical number.
Rachel Maddow

A Progressive News Commentator
$500,000 per year

That is chump change for the corporate elite!
THE CORPORATE ELITE...

Jeffrey R. Immelt, chairman and chief executive of General Electric
The Presidents' Club

Bush, Obama, Bush Jr, Clinton & Carter.
5 Presidents: Bush, Obama, Bush Jr, Clinton, & Carter!

White House Event: January 7, 2009.
Bank Bailout!

v taxpayer
Actress Elizabeth Banks

She will present an award to her hometown (Pittsfield) at the Massachusetts State House next month (1/2009). She recently starred in "W" and "Zack and Miri Make a Porno," and just signed a $1 million annual contract to be a spokesmodel for
Joanna Lipper

Her award-winning 1999 documentary, "Growing Up Fast," about teenaged mothers in Pittsfield, Massachusetts.
Happy Holidays...

...from "Star Wars"
Massachusetts "poor" economy
Massachusetts is one of the wealthiest states, but it is also very inequitable. For example, it boasts the nation's most lucrative lottery, which is just a system of regressive taxation so that the corporate elite get to pay less in taxes!
Reese Witherspoon

Hollywood Actress
Peter G. Arlos.

Arlos is shown in his Pittsfield office in early 2000.
Turnpike OK's hefty toll hikes

Big Dig - East-west commuters take hit; Fees at tunnels would double. 11/15/2008.
The Pink Panther 2

Starring Steve Martin
Police ABUSE

I was a victim of Manchester Police Officer John Cunningham's ILLEGAL USES of FORCE! John Cunningham was reprimanded by the Chief of Police for disrespecting me. John Cunningham yelled at a witness: "I don't care if he (Jonathan Melle) is disabled!"
Barack Obama

The 44th US President!
Vote

Elections
The Bailout & the economic stimulus check

A political cartoon by Dan Wasserman
A rainbow over Boston

"Rainbows galore" 10/2/2008
Our nation's leaders!

President Bush with both John McCain & Barack Obama - 9/25/2008.
Massachusetts & Big Dig: Big hike in tolls for Pike looming (9/26/2008).

$5 rise at tunnels is one possibility $1 jump posed for elsewhere.
Mary E Carey

My FAVORITE Journalist EVER!
9/11/2008 - A Show of Unity!

John McCain and Barack Obama appeared together at ground zero in New York City - September 11, 2008.
John McCain...

...has all but abandoned the positions on taxes, torture and immigration. (A cartoon by Dan Wasserman. September 2008).
Dan Wasserman

The deregulated chickens come home to roost... in all our pocketbooks. September 2008.
Sarah Palin's phobia

A scripted candidate! (A cartoon by Dan Wasserman).
Dan Wasserman

Family FInances - September, 2008.
Mark E. Roy

Ward 1 Alderman for Manchester, NH (2008).
Theodore “Ted” L. Gatsas

Ward 2 Alderman (& NH State Senator) for Manchester, NH (2008).
Peter M. Sullivan

Ward 3 (downtown) Alderman for Manchester, NH (2008).
Jim Roy

Ward 4 Alderman for Manchester, NH (2008).
Ed Osborne

Ward 5 Alderman for Manchester, NH (2008).
Real R. Pinard

Ward 6 Alderman for Manchester, NH (2008).
William P. Shea

Ward 7 Alderman for Manchester, NH (2008).
Betsi DeVries

Ward 8 Alder-woman (& NH State Senator) for Manchester, NH (2008).
Michael Garrity

Ward 9 Alderman for Manchester, NH (2008).
George Smith

Ward 10 Alderman for Manchester, NH (2008).
Russ Ouellette

Ward 11 Alderman for Manchester, NH (2008).
Kelleigh (Domaingue) Murphy

Ward 12 Alder-woman for Manchester, NH (2008).
“Mike” Lopez

At-Large Alderman for Manchester, NH. (2008).
Daniel P. O’Neil

At-Large Alderman for Manchester, NH (2008).
Sarah Palin for Vice President.

Republican John McCain made the surprise pick of Alaska's governor Sarah Palin as his running mate today, August 29, 2008.
U.S. Representative John Olver, D-Amherst, Massachusetts.

Congressman Olver said the country has spent well over a half-trillion dollars on the war in Iraq while the situation in Afghanistan continues to deteriorate. 8/25/08.
Ed O'Reilly for US Senate in Massachusetts!

John Kerry's 9/2008 challenger in the Democratic Primary.
Shays' Rebellion

In a tax revolt, Massachusetts farmers fought back during Shays' Rebellion in the mid-1780s after The American Revolutionary War.
Julianne Moore

Actress. "The Big Lebowski" is one of my favorite movies. I also like "The Fugitive", too.
Rinaldo Del Gallo III & "Superman"

Go to: http://www.berkshirefatherhood.com/index.php?mact=News,cntnt01,detail,0&cntnt01articleid=699&cntnt01returnid=69
"Income chasm widening in the Commonwealth of Massachusetts"

The gap between rich and poor has widened substantially in Massachusetts over the past two decades. (8/15/2008).
Dan "Bureaucrat" Bosley

"The Bosley Amendment": To create tax loopholes for the wealthiest corporate interests in Massachusetts!
John Edwards and...

...Rielle Hunter. WHO CARES?!
Rep. Edward J. Markey

He wants online-privacy legislation. Some Web Firms Say They Track Behavior Without Explicit Consent.
Cindy Sheehan

She gained fame with her antiwar vigil outside the Bush ranch.
Olympics kick off in Beijing

Go USA!
Exxon Mobil 2Q profit sets US record, shares fall

In this May 1, 2008, file photo, a customer pumps gas at an Exxon station in Middleton, Mass. Exxon Mobil Corp. reported second-quarter earnings of $11.68 billion Thursday, July 31, the biggest quarterly profit ever by any U.S. corporation, but the results were well short of Wall Street expectations and its shares fell as markets opened. (AP Photo/Lisa Poole, File) 7/31/2008.
Onota Lake 'Sea Serpent'

Some kind of monster on Onota Lake. Five-year-old Tyler Smith rides a 'sea serpent' on Onota Lake in Pittsfield, Mass. The 'monster,' fashioned by Smith's grandfather, first appeared over July 4 weekend. (Photo courtesy of Ron Smith). 7/30/2008.
Al Gore, Jr.

Al Gore issues challenge on energy
The Norman Rockwell Museum

Stockbridge, Massachusetts
"Big Dig"

Boston's financially wasteful pork barrel project!
"Big Dig"

Boston's pork barrel public works project cost 50 times more than the original price!
Mary E Carey

My favorite journalist EVER!
U.S. Rep. John Olver, state Sen. Stan Rosenberg and Selectwomen Stephanie O'Keeffe and Alisa Brewer

Note: Photo from Mary E Carey's Blog.
Tanglewood

Boston Symphony Orchestra music director James Levine.

Chagall
Jimmy Ruberto

Faces multiple persecutions under the Massachusetts "Ethics" conflict of interest laws.
Barack Obama

Obama vows $500m in faith-based aid.
John McCain

He is with his wife, Cindy, who were both met by Colombian President Alvaro Uribe (right) upon arriving in Cartagena.
Daniel Duquette

Sold Mayor James M. Ruberto of Pittsfield two tickets to the 2004 World Series at face value.
Hillary & Barack in Unity, NH - 6/27/2008

Clinton tells Obama, crowd in Unity, N.H.: 'We are one party'
John Forbes Kerry

Wanna-be Prez?
WALL-E

"out of this World"
Crisis in the Congo - Ben Affleck

http://abcnews.go.com/Nightline/popup?id=5057139&contentIndex=1&page=1&start=false - http://abcnews.go.com/Nightline/story?id=5234555&page=1
Jeanne Shaheen

NH's Democratic returning candidate for U.S. Senate
"Wall-E"

a cool robot
Ed O'Reilly

www.edoreilly.com
Go Celtics!

World Champions - 2008
Go Red Sox!

J.D. Drew gets the same welcome whenever he visits the City of Brotherly Love: "Booooooo!"; Drew has been vilified in Philadelphia since refusing to sign with the Phillies after they drafted him in 1997...
Joe Kelly Levasseur & Joe Briggs

www.2joes.org
NH Union Leader

Editorial Cartoon
Celtics - World Champions!

www.boston.com/sports/basketball/celtics/gallery/06_18_08_front_pages/ - www.boston.com/sports/basketball/celtics/gallery/06_17_08_finals_game_6/ - www.boston.com/sports/basketball/celtics/gallery/06_17_08_celebration/ - www.boston.com/sports/basketball/celtics/gallery/06_15_08_celtics_championships/
"The Nation"
A "Liberal" weekly political news magazine. Katrina vanden Heuvel.
TV - PBS: NOW
http://www.pbs.org/now
The Twilight Zone

List of Twilight Zone episodes - http://en.wikipedia.org/wiki/List_of_Twilight_Zone_episodes
Equality for ALL Marriages

I, Jonathan Melle, am a supporter of same sex marriages.
Kobe Bryant leads his time to a Game 5 victory.

L.A. Lakers holds on for the win to force Game 6 at Boston
Mohawk Trail

The 'Hail to the Sunrise' statue in Charlemont is a well-known and easily recognized landmark on the Mohawk Trail. The trail once boasted several souvenir shops, some with motels and restaurants. Now only four remain. (Caroline Bonnivier / Berkshire Eagle Staff).
NASA - June 14, 2008

Space Shuttle Discovery returns to Earth.
Go Celtics! Game # 4 of the 2008 NBA Finals.

Boston took a 20-second timeout, and the Celtics ran off four more points (including this incredible Erving-esque layup from Ray Allen) to build the lead to five points with just 2:10 remaining. Reeling, the Lakers took a full timeout to try to regain their momentum.
Sal DiMasi

Speaker of the Massachusetts State House of Representatives
Kelly Ayotte - Attorney General of New Hampshire

http://doj.nh.gov/
John Kerry

He does not like grassroots democracy & being challenged in the 2008 Massachusetts Democratic Party Primary for re-election.
Tim Murray

Corrupt Lt. Gov. of Massachusetts, 2007 - 2013.
North Adams, Massachusetts

downtown
Howie Carr

Political Satirist on Massachusetts Corruption/Politics
Polar Bear

Global Warming
Elizabeth Warren - Web-Site Links

http://en.wikipedia.org/wiki/Elizabeth_Warren & http://www.creditslips.org/creditslips/WarrenAuthor.html
Elizabeth Warren

Consumer Crusader
Leon Powe

Celtics forward Leon Powe finished a fast break with a dunk.
Kevin Garnett

Kevin Garnett reacted during the game.
Rajon Rondo

Rajon Rondo finished a first half fast break with a dunk.
Teamwork

Los Angeles Lakers teammates help Pau Gasol (16) from the floor in the second quarter.
Kobe Bryant

Kobe Bryant took a shot in the first half of Game 2.
Kendrick Perkins

Kendrick Perkins (right) backed down Lamar Odom (left) during first half action.
Go Celtics!

The Boston Symphony Orchestra performed the national anthem prior to Game 2.
K.G.!

Garnett reacted to a hard dunk in the first quarter.
Paul Pierce

Paul Pierce reacted after hitting a three upon his return to the game since leaving with an injury.
Go Celtics!

Kobe Bryant (left) and Paul Pierce (right) squared off in the second half of the game.
James Taylor

Sings National Anthem at Celtics Game.
John Forbes Kerry & Deval Patrick

Attended Celtics Game.
Greats of the NBA: Dr. J, Bill Russell, & Kareem!

Attend Game 1 of the 2008 NBA Finals.
Bruce Willis

The actor (left) and his date were in the crowd before the Celtics game.
John Kerry

Golddigger attends Celtics game
Hillary Clinton

Ends her 2008 bid for Democratic Party nomination
Nonnie Burnes

Massachusetts Insurance Commish & former Judge
Jones Library

Amherst, Massachusetts
Barack Obama & Hillary Clinton

2008 Democratic Primary
"US vs Exxon and Halliburton"
.png)
U.S. Senator John Sununu took more than $220,000 from big oil.
Jeanne Shaheen
4- U.S. Senate - 2008
William Pignatelli

Hack Rep. "Smitty" with Lynne Blake
Ben Bernanke

Federal Reserve Chairman
Gazettenet.com
www.gazettenet.com/beta/
Boys' & Girls' Club

Melville Street, Pittsfield, Massachusetts
Denis Guyer
Dalton State Representative
The Berkshire Eagle
Pittsfield, Massachusetts
Carmen Massimiano

Williams College - May 2008
Larry Bird & Magic Johnson

www.boston.com/lifestyle/gallery/when_the_celtics_were_cool/
Regressive Taxation! via State Lotteries

New Massachusetts state lottery game hits $600 million in sales!
Andrea Nuciforo

"Luciforo"
John Barrett III

Long-time Mayor of North Adams Massachusetts
Shine On

Elmo

cool!
Paul Pierce

Paul Pierce kissed the Eastern Conference trophy. 5/30/2008. AP Photo.
Kevin Garnett & Richard Hamilton

Kevin Garnett (left) talked to Pistons guard Richard Hamilton (right) after the Celtics' victory in Game 6. 5/30/2008. Reuters Photo.
Paul Pierce

Paul Pierce showed his team colors as the Celtics closed out the Pistons in Game 6 of the Eastern Conference finals. 5/30/2008. Globe Staff Photo / Jim Davis.
Joseph Kelly Levasseur

One of my favorite politicians!
Mary E Carey

In the Big Apple: NYC! She is the coolest!
Guyer & Kerry

My 2nd least favorite picture EVER!
Mary Carey

My favorite journalist EVER!
Nuciforo & Ruberto

My least favorite picture EVER!
Jeanne Shaheen

U.S. Senate - 2008
NH Fisher Cats

AA Baseball - Toronto Blue Jays affiliate
Manchester, NH

Police Patch
Michael Briggs

#83 - We will never forget
Michael "Stix" Addison

http://unionleader.com/channel.aspx/News?channel=2af17ff4-f73b-4c44-9f51-092e828e1131
Charlie Gibson

ABC News anchor
Scott McClellan

http://topics.nytimes.com/top/reference/timestopics/people/m/scott_mcclellan/index.html?inline=nyt-per
Boise, Idaho

Downtown Boise Idaho
John Forbes Kerry

Legislative Hearing in Pittsfield, Massachusetts, BCC, on Wednesday, May 28, 2008
Thomas Jefferson

My favorite classical U.S. President!
NH Governor John Lynch

Higher Taxes, Higher Tolls
Paul Hodes

My favorite Congressman!
Portland Sea Dogs

AA Red Sox
New York

Magnet
Massachusetts

Magnet
New Hampshire

Magnet
New Hampshire

Button
Carmen Massimiano

"Luciforo" tried to send me to Carmen's Jail during the Spring & Summer of 1998.
Kay Khan - Massachusetts State Representative

www.openmass.org/members/show/174
Luciforo

Andrea F Nuciforo II
B-Eagle
Pittsfield's monopoly/only daily newspaper
Jon Lester - Go Red Sox!

A Red Sox No Hitter on 5/19/2008!
Go Red Sox!

Dustin Pedroia & Manny Ramirez
U.S. Flag

God Bless America!
Jonathan Melle's Blog

Hello, Everyone!
Molly Bish

We will never forget!
Go Celtics!

Celtics guard Rajon Rondo listens to some advice from Celtics head coach Doc Rivers in the first half.
Go Celtics!

Celtics forward Kevin Garnett and Pistons forward Rasheed Wallace embrace at the end of the game.
Go Red Sox!

Red Sox closer Jonathan Papelbon calls for the ball as he charges toward first base. Papelbon made the out en route to picking up his 14th save of the season.
Go Red Sox!

Red Sox starting pitcher Daisuke Matsuzaka throws to Royals David DeJesus during the first inning.
Go Red Sox!

Red Sox pitcher Daisuke Matsuzaka delivers a pitch to Royals second baseman Mark Grudzielanek during the second inning.
Go Red Sox!

Red Sox right fielder J.D. Drew is welcomed to home plate by teammates Mike Lowell (left), Kevin Youkilis (2nd left) and Manny Ramirez after he hit a grand slam in the second inning.
Go Red Sox!

Red Sox third baseman Mike Lowell crosses the plate after hitting a grand slam during the sixth inning. Teammates Manny Ramirez and Jacoby Ellsbury scored on the play. The Red Sox went on to win 11-8 to complete a four-game sweep and perfect homestand.
JD Drew - Go Red Sox

www.boston.com/sports/baseball/redsox/gallery/05_22_08_sox_royals/
Thank you for serving; God Bless America!
Master Sgt. Kara B. Stackpole, of Westfield, holds her daughter, Samantha, upon her return today to Westover Air Reserve Base in Chicopee. She is one of the 38 members of the 439th Aeromedical Staging Squadron who returned after a 4-month deployment in Iraq. Photo by Dave Roback / The Republican.
Kathi-Anne Reinstein

www.openmass.org/members/show/175
Ted Kennedy

Tragic diagnosis: Get well Senator!
Google doodle - Jonathan Melle Internet search

http://blogsearch.google.com/blogsearch?hl=en&q=jonathan+melle+blogurl:http://jonathanmelleonpolitics.blogspot.com/&ie=UTF-8
John Forbes Kerry

Billionaire U.S. Senator gives address to MCLA graduates in North Adams, Massachusetts in mid-May 2008
Andrea Nuciforo

"Luciforo"
A Red Sox Fan in Paris, France

Go Red Sox!
Rinaldo Del Gallo III

Interviewed on local TV
Andrea Nuciforo

Luciforo!
John Adams

#2 U.S. President
Jonathan Melle

I stood under a tree on the afternoon of May 9, 2008, on the foregrounds of the NH State House - www.websitetoolbox.com/tool/post/nhinsider/vpost?id=2967773
Jonathan Melle

Inside the front lobby of the NH State House
Jonathan Melle

Bill Clinton campaign memorabilia
Jonathan Melle

Liberty Bell & NH State House
Jon Keller

Boston based political analyst
Jon Keller

Boston based political analyst
Jonathan Melle

Franklin Pierce Statue #14 U.S. President
Jonathan Melle

NH State House
Jonathan Melle

Stop the War NOW!
Jonathan Melle

"Mr. Melle, tear down this Blog!"
Jonathan Melle

I stood next to a JFK photo
Jonathan Levine, Publisher
The Pittsfield Gazette Online
Jonathan Melle

I made rabbit ears with John & George
Jonathan Melle

I made antenna ears with John & George
Jonathan Melle

I impersonated Howard Dean
Jonathan Melle

mock-voting
Jonathan Melle

pretty ladies -/- Go to: http://www.wgir.com/cc-common/cc_photopop20.html?eventID=28541&pagecontent=&pagenum=4 - Go to: http://current.com/items/88807921_veterans_should_come_first_not_last# - http://www.mcam23.com/cgi-bin/cutter.cgi?c_function=STREAM?c_feature=EDIT?dir_catagory=10MorningRadio?dir_folder=2JoesClips?dir_file=JonathanMelle-090308? -
Jonathan Melle

Go Red Sox! Me at Fenway Park
Mary E. Carey

My favorite journalist! Her voice sings for the Voiceless. -/- Go to: http://aboutamherst.blogspot.com/search?q=melle -/- Go to: http://ongeicocaveman.blogspot.com/search?q=melle
Velvet Jesus

Mary Carey blogs about my political writings. This is a picture of Jesus from her childhood home in Pittsfield, Massachusetts. -//- "How Can I Keep From Singing" : My life goes on in endless song / Above Earth's lamentations, / I hear the real, though far-off hymn / That hails a new creation. / / Through all the tumult and the strife / I hear its music ringing, / It sounds an echo in my soul. / How can I keep from singing? / / Whey tyrants tremble in their fear / And hear their death knell ringing, / When friends rejoice both far and near / How can I keep from singing? / / In prison cell and dungeon vile / Our thoughts to them are winging / When friends by shame are undefiled / How can I keep from singing?
www.truthdig.com

www.truthdig.com
Jonathan Melle

Concord NH
The Huffington Post

http://fundrace.huffingtonpost.com/neighbors.php?type=loc&newest=1&addr=&zip=01201&search=Search
Barack Obama

smiles & beer
Jonathan Lothrop

A Pittsfield City Councilor
Michael L. Ward

A Pittsfield City Councilor
Peter Marchetti - Pittsfield's City Councilor at Large

Pete always sides with the wealthy's political interests.
Gerald Lee - Pittsfield's City Council Prez

Gerald Lee told me that I am a Social Problem; Lee executes a top-down system of governance. R.I.P. Gerry Lee.
Matt Kerwood - Pittsfield's Councilor at Large

Kerwood poured coffee drinks for Jane Swift
Louis Costi

Pittsfield City Councilor
Lewis Markham

Pittsfield City Councilor
Kevin Sherman - Pittsfield City Councilor

Sherman ran for Southern Berkshire State Rep against Smitty Pignatelli; Sherman is a good guy.
Anthony Maffuccio

Pittsfield City Councilor
Linda Tyer

Pittsfield City Councilor
Daniel Bianchi

A Pittsfield City Councilor
The Democratic Donkey

Democratic Party Symbol
Paramount

What is Paramount to you?
NH's Congresswoman
Carol Shea-Porter, Democrat
Sam Adams Beer

Boston Lager
Ratatouille

Disney Animation
Ruberto Details Plans for Success - January 07, 2008

"Luciforo" swears in Mayor Ruberto. Pittsfield Politics at its very worst: 2 INSIDER POWERBROKERS! Where is Carmen Massimiano? He must be off to the side.
Abe

Lincoln
Optimus Prime

Leader of the Autobots
Optimus Prime

1984 Autobot Transformer Leader
Cleanup Agreements - GE & Pittsfield's PCBs toxic waste sites

www.epa.gov/region1/ge/cleanupagreement.html
GE/Housatonic River Site: Introduction

www.epa.gov/region1/ge/
GE/Housatonic River Site - Reports

www.epa.gov/region1/ge/thesite/opca-reports.html
US EPA - Contact - Pittsfield's PCBs toxic waste sites

www.epa.gov/region1/ge/contactinfo.html
GE Corporate Logo - Pittsfield's PCBs toxic waste sites

www.epa.gov/region1/ge/index.html
Commonwealth Connector

Commonwealth Care
Blue Cross Blue Shield of Massachusetts

Healthcare Reform
Blue Cross Blue Shield of Massachusetts

Healthcare Reform
Network Health Forward - A Commonwealth Care Plan

Massachusetts Health Reform
Network Health Together: A MassHealth Plan - Commonwealth Care

Massachusetts Health Reform
www.network-health.org

Massachusetts Health Reform
Neighborhood Health Plan - Commonwealth Care

Massachusetts Health Reform
Fallon Community Health Plan - Commonwealth Care

Massachusetts Health Reform
BMC HealthNet Plan

Massachusetts Health Reform
Massachusetts Health Reform

Eligibility Chart: 2007
Harvard Pilgrim Healthcare
Massachusetts Health Reform
Business Peaks

Voodoo Economics
Laffer Curve - Corporate Elite

Reagonomics: Supply Side
Corporate Elite Propaganda

Mock Liberal Democratic Socialism Thinking
Real Estate Blues

www.boston.com/bostonglobe/magazine/2008/0316/
PEACE

End ALL Wars!
Freedom of Speech

Norman Rockwell's World War II artwork depicting America's values
Abraham Lincoln

A young Abe Lincoln
RACHEL KAPRIELIAN

www.openmass.org/members/show/218 - www.rachelkaprielian.com
Jennifer M. Callahan - Massachusetts State Representative

www.openmass.org/members/show/164 - www.boston.com/news/local/articles/2008/05/04/legislator_describes_threat_as_unnerving/
Human Rights for ALL Peoples!

My #1 Political Belief!
Anne Frank

Amsterdam, Netherlands, Europe
A young woman Hillary supporter

This excellent picture captures a youth's excitement
Hillary Clinton with Natalie Portman

My favorite Actress!
Alan Chartock

WAMC public radio in Albany, NY; Political columnist who writes about Berkshire County area politics; Strong supporter for Human Rights for ALL Peoples
OpenCongress.Org

This web-site uses some of my Blog postings
OpenMass.org
This web-site uses some of my blog postings!
Shannon O'Brien

One of my favorite politicians! She stands for the People first!
The Massachusetts State House

"The Almighty Golden Dome" - www.masslegislature.tv -
Sara Hathaway

Former Mayor of Pittsfield, Massachusetts
Andrea F. Nuciforo, Jr.

A corrupt Pol who tried to put me in Jail
Andrea F. Nuciforo, Jr.

Another view of Pittsfield's inbred, multigenerational political prince. Luciforo!
Luciforo

Nuciforo's nickname
"Andy" Nuciforo

Luciforo!
Carmen C. Massimiano, Jr., Berkshire County Sheriff (Jailer)

Nuciforo's henchman! Nuciforo tried to send me to Carmen's Jail
Andrea Nuciforo Jr

Shhh! Luciforo's other job is working as a private attorney defending wealthy Boston-area corporate insurance companies
Berkshire County Sheriff (Jailer) Carmen C. Massimiano, Jr.

Nuciforo tried to send me to Carmen's Jail! Carmen sits with the Congressman, John Olver
Congressman John Olver

Nuciforo's envy
The Dome of the U.S. Capitol

Our Beacon of American Democracy
Nuciforo's architect

Mary O'Brien in red with scarf
Sara Hathaway (www.brynmawr.edu)

Former-Mayor of Pittsfield, Massachusetts; Nuciforo intimidated her, along with another woman, from running in a democratic state election in the Spring of 2006!
Andrea F. Nuciforo II

Pittsfield Politics Pot $
Berkshire County Republican Association

Go to: www.fcgop.blogspot.com
Denis Guyer

Dalton State Representative
John Forbes Kerry & Denis Guyer

U.S. Senator & State Representative
John Kerry

Endorses Barack Obama for Prez then visits Berkshire County
Dan Bosley

A Bureaucrat impostoring as a Legislator!
Ben Downing

Berkshire State Senator
Christopher N Speranzo

Pittsfield's ANOINTED State Representative
Peter J. Larkin

Corrupt Lobbyist
GE - Peter Larkin's best friend!

GE's FRAUDULENT Consent Decree with Pittsfield, Massachusetts, will end up KILLING many innocent school children & other local residents!
GE's CEO Jack Welch

The Corporate System's Corporate Elite's King
Economics: Where Supply meets Demand

Equilibrium
GE & Pittsfield, Massachusetts

In 2007, GE sold its Plastics Division to a Saudi company. Now all that is left over by GE are its toxic PCB pollutants that cause cancer in many Pittsfield residents.
Mayor James M Ruberto

A small-time pol chooses to serve the corporate elite & other elites over the people.
Governor Deval Patrick

Deval shakes hands with Mayors in Berkshire County
Deval Patrick

Governor of Massachusetts
Pittsfield High School

Pittsfield, Massachusetts
Sara Hathaway

Pittsfield's former Mayor
Rinaldo Del Gallo III

Pittsfield Attorney focusing on Father's Rights Probate Court Legal Issues, & Local Politician and Political Observer
Rinaldo Del Gallo III

Very Intelligent Political Activists in Pittsfield, Massachusetts. Rinaldo Del Gallo, III, Esq. is the spokesperson of the Berkshire Fatherhood Coalition. He has been practicing family law and has been a member of the Massachusetts bar since 1996.
Mayor Ed Reilly

He supports Mayor Ruberto & works as a municipal Attorney. As Mayor, he backed Bill Weld for Governor in 1994, despite being a Democrat. He was joined by Carmen Massimiano & John Barrett III, the long-standing Mayor of North Adams.
Manchester, NH Mayor Frank Guinta

Cuts Dental Care for Public School Children-in-Need
Manchester, NH City Hall

My new hometown - view from Hanover St. intersection with Elm St.
Manchester NH City Democrats

Go Dems!
2008 Democratic Candidates for U.S. Prez

Barack Obama, Hillary Clinton, Mike Gravel, Dennis Kucinich, John Edwards
NH State House Dome

Concord, NH
Donna Walto

Pittsfield Politician -- She strongly opposes Mayor Jim Ruberto's elitist tenure.
Elmo

Who doesn't LOVE Elmo?
Hillary Clinton for U.S. President!

Hillary is for Children. She is my choice in 2008.
The White House in 1800

Home of our Presidents of the United States
John Adams

2nd President of the USA
Hillary Clinton stands with John Edwards and Joe Biden

Hillary is my choice for U.S. President!
Bill Clinton

Former President Bill Clinton speaks at the Radisson in Manchester NH 11/16/2007
Barack Obama

U.S. Senator & Candidate for President
Pittsfield's 3 Women City Councillors - 2004

Linda Tyer, Pam Malumphy, Tricia Farley-Bouvier
Wahconah Park in Pittsfield, Massachusetts

My friend Brian Merzbach reviews baseball parks around the nation.
The Corporate Elite: Rational Incentives for only the wealthy
The Elites double their $ every 6 to 8 years, while the "have-nots" double their $ every generation (or 24 years). Good bye Middle Class!
George Will

The human satellite voice for the Corporate Elite
Elizabeth Warren

The Anti-George Will; Harvard Law School Professor; The Corporate Elite's Worst Nightmare
The Flag of The Commonwealth of Massachusetts

I was born and raised in Pittsfield, Massachusetts
State Senator Stan Rosenberg

Democratic State Senator from Amherst, Massachusetts -/- Anti-Stan Rosenberg Blog: rosenbergwatch.blogspot.com
Ellen Story

Amherst Massachusetts' State Representative
Teen Pregnancy in Pittsfield, Mass.

Books are being written on Pittsfield's high teen pregancy rates! What some intellectuals do NOT understand about the issue is that TEEN PREGNANCIES in Pittsfield double the statewide average by design - Perverse Incentives!
NH Governor John Lynch

Supports $30 Scratch Tickets and other forms of regressive taxation. Another Pol that only serves his Corporate Elite Masters instead of the People!
U.S. Congresswoman Carol Shea Porter

The first woman whom the People of New Hampshire have voted in to serve in U.S. Congress
U.S. Congressman Paul Hodes

A good man who wants to bring progressive changes to Capitol Hill!
Paul Hodes for U.S. Congress

New Hampshire's finest!
Darth Vader

Star Wars
Dick Cheney & George W. Bush

The Gruesome Two-some! Stop the Neo-Cons' fascism! End the Iraq War NOW!
WAROPOLY

The Inequity of Globalism
Bushopoly!

The Corporate Elite have redesigned "The System" to enrich themselves at the expense of the people, masses, have-nots, poor & middle-class families
George W. Bush with Karl Rove

Rove was a political strategist with extraordinary influence within the Bush II White House
2008's Republican Prez-field

John McCain, Alan Keyes, Rudy Guiliani, Duncan Hunter, Mike Huckabee, WILLARD Mitt Romney, Fred Thompson, Ron Paul
Fall in New England

Autumn is my favorite season
Picturing America

picturingamerica.neh.gov
Winter Weather Map

3:45PM EST 3-Dec-07
Norman Rockwell Painting

Thanksgiving
Norman Rockwell Painting

Depiction of American Values in mid-20th Century America
Larry Bird #33

My favorite basketball player of my childhood
Boston Celtics Basketball - 2007-2008

Kevin Garnett hugs James Posey
Paul Pierce

All heart! Awesome basketball star for The Boston Celtics.
Tom Brady

Go Patriots!
Rupert Murdoch

Owner of Fox News - CORPORATE ELITE!
George Stephanopolous

A Corporate Elite Political News Analyst
Robert Redford

Starred in the movie "Lions for Lambs"
Meryl Streep

Plays a jaded journalist with integrity in the movie "Lions for Lambs"
Tom Cruise

Tom Cruise plays the Neo-Con D.C. Pol purely indoctrinated by the Corporate Elite's political agenda in the Middle East
CHARLIZE THERON

"I want to say I've never been surrounded by so many fake breasts, but I went to the Academy Awards."
Amherst Town Library

Amherst, NH - www.amherstlibrary.org
Manchester NH Library

I use the library's automated timed 1-hour-per-day Internet computers to post on my Blog - www.manchester.lib.nh.us
Manchester NH's Palace Theater

Manchester NH decided to restore its Palace Theater
Pittsfield's Palace Theater

Pittsfield tore down this landmark on North Street in favor of a parking lot
Pleasant Street Theater

Amherst, Massachusetts
William "Shitty" Pignatelli

A top down & banal State House Pol from Lenox Massachusetts -- A GOOD MAN!
The CIA & Mind Control

Did the CIA murder people by proxy assassins?
Skull & Bones

Yale's Elite
ImpeachBush.org

I believe President Bush should be IMPEACHED because he is waging an illegal and immoral war against Iraq!
Bob Feuer drumming for U.S. Congress v John Olver in 2008

www.blog.bobfeuer.us
Abe Lincoln

The 16th President of the USA
Power

Peace
Global Warming Mock Giant Thermometer

A member of Green Peace activist sets up a giant thermometer as a symbol of global warming during their campaign in Nusa Dua, Bali, Indonesia, Sunday, Dec. 2, 2007. World leaders launch marathon negotiations Monday on how to fight global warming, which left unchecked could cause devastating sea level rises, send millions further into poverty and lead to the mass extinction of plants and animals.
combat global warming...

...or risk economic and environmental disaster caused by rising temperatures
www.climatecrisiscoalition.org
P.O. Box 125, South Lee, MA 01260, (413) 243-5665, tstokes@kyotoandbeyond.org, www.kyotoandbeyond.org
3 Democratic presidentional candidates

Democratic presidential candidates former senator John Edwards (from right) and Senators Joe Biden and Chris Dodd before the National Public Radio debate yesterday (12/4/2007).
The UN Seal

An archaic & bureaucratic post WW2 top-down, non-democratic institution that also stands for some good governance values
Superman

One of my favorite childhood heroes and movies
Web-Site on toxic toys
www.healthytoys.org
Batman

One of my favorite super-heroes
Deval Patrick & Denis Guyer

Massachusetts' Governor stands with Dalton's State Rep. Denis E. Guyer.
Bill Cosby & Denis Guyer

TV Star Bill Cosby stands with Denis E. Guyer
Denis Guyer with his supporters

Dalton State Representative
Denis Guyer goes to college

Dalton State Representative
Peter Marchetti

He is my second cousin. Pete Marchetti favors MONEY, not fairness!
Matt Barron & Denis Guyer with couple

Matt Barron plays DIRTY politics against his opponents!
Nat Karns

Top-Down Executive Director of the ELITIST Berkshire Regional Planning Commission
Human Rights for All Peoples & people
Stop Anti-Semitism
Massachusetts State Treasurer Tim Cahill

State House, Room 227, Boston, MA 02133, 617-367-6900, www.mass.gov/treasury/
Massachusetts State Attorney General Martha Coakley

1350 Main Street, Springfield, MA 01103, 413-784-1240 / McCormick Building, One Asburton Place, Boston, MA 02108, 617-727-4765 / marthacoakley.com / www.ago.state.ma.us
Bush v. Gore: December 12, 2007, was the seventh anniversary, the 5-4 Supreme Court decision...

www.takebackthecourt.org - A political billboard near my downtown apartment in Manchester, NH
Marc Murgo

An old friend of mine from Pittsfield
Downtown Manchester, NH

www.newhampshire.com/nh-towns/manchester.aspx
Marisa Tomei

Movie Actress
Massachusetts Coalition for Healthy Communities (MCHC)
www.masschc.org/issue.php
Mike Firestone & Anna Weisfeiler

Mike Firestone works in Manchester NH for Hillary Clinton's presidential campaign
James Pindell
Covers NH Primary Politcs for The Boston Globe
U.S. History - Declaration

A 19th century engraving shows Benjamin Franklin, left, Thomas Jefferson, John Adams, Philip Livingston and Roger Sherman at work on the Declaration of Independence.
Boston Globe Photos of the Week - www.boston.com/bostonglobe/gallery/

Sybregje Palenstijn (left), who plays Sarah Godbertson at Plimouth Plantation, taught visitors how to roast a turkey on a spit. The plantation often sees a large influx of visitors during the holiday season.
Chris Hodgkins

Another special interest Berkshire Pol who could not hold his "WATER" on Beacon Hill's State House!
The Big Dig - 15 tons of concrete fell from a tunnel ceiling onto Milena Del Valle's car.

Most of Boston's Big Dig highway remains closed, after a woman was crushed when 15 tons of concrete fell from a tunnel ceiling onto her car. (ABC News)
Jane Swift

Former Acting Governor of Massachusetts & Berkshire State Senator
Paul Cellucci

Former Massachusetts Governor
William Floyd Weld

$80 Million Trust Fund Former Governor of Massachusetts
Mike Dukakis

Former Governor of Massachusetts
Mary E. Carey

Amherst, Massachusetts, Journalist and Blogger
Caveman

www.ongeicocaveman.blogspot.com
Peter G. Arlos

"The biggest challenge Pittsfield faces is putting its fiscal house in order. The problem is that doing so requires structural changes in local government, many of which I have advocated for years, but which officials do not have the will to implement. Fiscal responsibility requires more than shifting funds from one department to another. Raising taxes and fees and cutting services are not the answer. Structural changes in the way services are delivered and greater productivity are the answer, and without these changes the city's fiscal crisis will not be solved."
James M. Ruberto

"Pittsfield's biggest challenge is to find common ground for a better future. The city is at a crossroads. On one hand, our quality of life is challenged. On the other hand, some important building blocks are in place that could be a strong foundation for our community. Pittsfield needs to unite for the good of its future. The city needs an experienced businessman and a consensus builder who will invite the people to hold him accountable."
Matt Kerwood

Pittsfield's Councilor-At-Large. Go to: extras.berkshireeagle.com/NeBe/profiles/12.htm
Gerald M. Lee

Pittsfield's City Council Prez. Top-down governance of the first order!
Mary Carey

Mary with student
Boston Red Sox

Jonathan Papelbon celebrates with Jason Varitek
Free Bernard Baran!

www.freebaran.org
Political Intelligence
Capitol Hill
Sherwood Guernsey II

Wealthy Williamstown Political Activist & Pittsfield Attorney
Mary Carey 2

California Pol & porn star
Pittsfield's Good Old Boy Network - Political Machine!

Andy "Luciforo" swears in Jimmy Ruberto for the returning Mayor's 3rd term
Berkshire Grown

www.berkshiregrown.org
Rambo

The Mount was built in 1902 & was home to Edith Wharton (1862-1937) from 1903 to 1908.

The Mount, the historic home in Lenox of famed American novelist Edith Wharton, is facing foreclosure.
Blog Archive
-
▼
2008
(122)
-
▼
April
(9)
- Gaining ground on cancer
- Pittsfield's high teen pregnancy rate is by design...
- Berkshire County's Healthcare Inequalities. Also ...
- Suzanne Bump. Susan Windham-Bannister. Massachus...
- Jeanne Shaheen U.S. Senate - 2008 - NH
- Rachel Kaprielian - Massachusetts State Representa...
- Fourteen top executives at nonprofit Bay State hos...
- Veterans Affairs employees charged $2.6 billion to...
- UMass-Lowell Prez Martin T. Meehan raised more tha...
-
▼
April
(9)
No comments:
Post a Comment