www.boston.com/news/specials/healthcare_spotlight/
-

-

-
www.issuesource.org/issue.cfm?ID=130
-
www.boston.com/business/healthcare/
-
www.boston.com/news/health/blog/masshealthlaw/
-
www.wbur.org/weblogs/commonhealth/
-
Health care law benefits insurers
The Berkshire Eagle - Letters
Saturday, January 19, 2008
The Access Project, based in Boston, released the findings of its recent independent study of the health insurance industry in its publication, "The Illusion of Coverage." The report demonstrates the specific ways in which health insurance products deliberately fail to protect people financially and fail to guarantee their access to needed care. Our legislators would do well to read it.
The new health care law that mandates the purchase of these health care products from private for profit insurance companies is no solution. Those who can only afford the minimal plans will remain largely exposed. The premiums are still too high and can cause real economic hardship for those who do not qualify for subsidization. The program increased the number who qualify for subsidization but had no provision to fund them. The cost of that legislative blunder is already being passed on to those who can least afford it in the form of more penalties in 2008, a discriminatory and possibly illegal act that essentially raises the income tax rate for a targeted population.
The real winner here is not the health care consumer, but the unscrupulous insurance companies. I suggest that a major motive behind this legislation was to shift the cost of uncompensated care from the wealthy insurers, who largely fund the "free care pool," on to the unsuspecting public.
Instead of mandating the purchase of defective insurance products and stealing taxpayer income and deductions , our lawmakers should reform managed care and mandate insurance companies to further reduce premiums by substantially decreasing their large profits. There can be no real improvement in health care services or the cost of coverage until the greed of the insurance companies is contained.
It's time to hold insurance companies, and the legislators who empower them, accountable for their actions by demanding the repeal of this poorly and prematurely executed law.
LINDA GILARDI
Pittsfield, Massachusetts
----------
"Insurers at root of health care mess"
The Berkshire Eagle - Letters
Tuesday, March 11, 2008
Most of our health care woes can be traced back to the advent of the managed care system and the insurance companies who run it. This is well illustrated in Michael Moore's movie "Sicko" and the independent report, "The Illusion of Coverage," which can be read at www.accessproject.org
More than 250 Massachusetts physicians recently signed an open letter to the rest of the country warning of the failure of the Mass. model. They cited the million dollars a day surplus reaped by Blue Cross as well as the $16.4 million retirement bonus given, in addition to a $3 million salary, to its chairman, as just one example of insurance company greed and corruption.
The program is not affordable for the state or its citizens. Premiums have remained excessive and will continue to rise. The affordability guidelines are unrealistic and unfair. Each family has a unique financial situation. Affordability cannot be fairly determined unless they use the same debt to in income ratios that lending institutions use. Gaps in coverage still exist that can leave insured patients without care and financially exposed, and children were not even included in the mandate.
Linking penalties to income tax deductions, etc., is just a convoluted and discriminatory way of forcing a higher income tax rate on a selected population. The employer mandates and penalties likely violate ERISA, a federal law that prohibits states from forcing businesses to provide health insurance to employees.
Clearly, there can be no improvement in the delivery or cost of health care services until managed care is reformed and the obscene profits of the insurers are drastically reduced and capped. Since the insurance industry only cares about profits and our legislators only care about protecting the insurers, it is unlikely that will ever happen. The only viable solution is the single-payer, non-profit program largely supported by the medical community nationwide.
The defects in the current plan are too serious to ignore. Our legislators should remove the related mandates and penalties until the problems are resolved. Defenseless taxpayers should not be penalized for this huge legislative blunder.
LINDA GILARDI
Pittsfield, Massachusetts
----------
5 Massachusetts insurers control about 90 percent of the healthcare insurance market in the Commonwealth of Massachusetts:
#1 - Blue Cross Blue Shield
#2 - Harvard Pilgrim Health Care
#3 - Fallon Community Health Plan
#4 - Health New England
#5 - Tufts Health Plan
-
There are also national healthcare insurance companies such as United HealthCare Insurance Co., Aetna, and CIGNA.
Source: "200,000 may need to get more insurance: State healthcare law sets higher minimums" (By Alice Dembner, [The Boston]Globe Staff, January 30, 2007).
-----
Questions on Massachusetts healthcare insurance mandate program:
#1 - Will insurance be truly affordable?
#2 - Will individuals revolt when the state starts fining those without coverage next year?
#3 - Will employers maintain the insurance they now offer?
#4 - Will there be enough federal and state funding to cover rising costs?
-
The state's plan relies largely on two sources: federal funds that are committed only through June 30, 2008, and the state's free-care pool, now used to pay for charity care at hospitals and health centers.
-
Source: "MANDATORY HEALTH INSURANCE | THE FIRST YEAR: Progress and perils - Thousands more in state have coverage under ambitious program, but challenges lie ahead over funding and getting message out to all" (By Alice Dembner, (Boston) Globe Staff, April 22, 2007).
----------
"State punishes the uninsured"
The Berkshire Eagle - Letters
Tuesday, March 18, 2008
I am a Berkshire County resident, who is disgusted and angry with the mandated health insurance law.
The thought of forced health insurance is outrageous for Americans to swallow. However, considering the commonwealth of Massachusetts already misuses taxpayers' money by footing the bill for illegals' health care, it doesn't come as a total shock it also devised this "law" to rip off more residents out of their hard earned income.
Hence, under the guise of "universal health care," Massachusetts has become the first state to force health insurance down the throat of law-abiding citizens; and the first state to threaten its residents with severe penalties if they don't conform. There are no carrots in this plan, only sticks and evil schemes.
I thought the primary purpose of universal health care was to provide "affordable" health services for all residents, not punish the uninsured, twice. Initially, it requires a huge number of people that do not qualify for free or subsidized insurance to purchase it at exorbitant premiums. Subsequently, it imposes stiff fines, hiked at will, on those that reject this plan. To ensure no one escapes its grip, the state has tied health insurance to income tax returns!
As an uninsured, healthy individual, a taxpayer, I'd like to know what business has the state to strong-arm me or any other resident into buying insurance? Why after my taxes go to subsidize others' freebies, I am put in a position to have to choose whether to pay my mortgage or the health insurance premiums?
I did not ask the state to provide me with health insurance. What right does the state have to determine how much each individual or family is able to afford based primarily on age and revenue? No two families' needs and income are alike. Why does the state presume it is wiser in making choices than we are?
The list of grievances with this law is bigger and deeper than the affordability issue. Some examples: The "estate recovery program" that applies to people 55 and older who sign into the Commonwealth Care plan. These individuals are not told when signing on this plan, that they are also, giving their assets over to the state. Why?
The invasion of privacy that allows 20-plus agencies (including the D.O.R.) to share every resident's personal and medical info without any accountability. Don't they know it is in direct contrast with the federal HIPAA law created to protect our medical information?
The 4 to 5 percent kickback the connector authority receives for every policy sold. This newly created agency is comprised of 43 bureaucrats whose high salaries we are financing! The penalties for those who will not purchase the insurance are treated as a tax evasion! There are no "robust" or "generous" waivers as advertised by the Connector. People need to be destitute to receive a waiver.
Any change of income by residents has to be reported immediately to the Department of Revenue so your premiums can be "adjusted." Medical providers are required to report any services to the Connector, even if paid in cash!
This law was not conceived to benefit the residents of Massachusetts, but rather greedy politicians and bureaucrats who have forgotten they work for us, not the other way around.
ELISA POPLASKI
Pittsfield, Massachusetts
----------
"Care program doesn't take assets"
The Berkshire Eagle - Letters
Thursday, March 27, 2008
I am writing to correct misinformation in Elisa Poplaski's letter of March 18, "State punishes the uninsured," in regard to Massachusetts health reform. In her zeal to criticize health reform, she incorrectly states: "The estate recovery program that applies to people 55 and older who sign into the Commonwealth Care plan. These individuals are not told when signing on this plan, that they are also, giving their assets over to the state."
The state recovery program she is referring to does not apply to Commonwealth Care members, it applies to MassHealth members, and then only in very limited situations. Her confusion comes from the mutli-purpose state health care application which alludes to the state recovery program. But again, this does not apply to Commonwealth Care.
Commonwealth Care has enabled over 180,000 previously uninsured Massachusetts residents to obtain health insurance they would otherwise be unable to obtain. Uninsured individuals, especially those over age 55, should not be discouraged from applying for critically needed health coverage.
CHARLES JOFFE-HALPERN
North Adams, Massachusetts
The writer is executive director, Ecu-Health Care.
----------
"Revise clause on estate recovery"
The Berkshire Eagle - Letters
Wednesday, April 02, 2008
In response to Charles Joffe-Halpern's letter on March 26, "Care program doesn't take assets," in which he states, "The state recovery program she (Elisa Poplaski) is referring to does not apply to Commonwealth Care members . . .": The Connector has long been aware that the estate recovery clause on the application is a problem. It has revised the form twice but has yet to add language that specifically excludes Commonwealth Care applicants from estate recovery. Perhaps it needs to keep this option available so if it is decided that money is needed and the estates of Commonwealth Care members should be pursued, the application form as it is will allow it to do so.
Ms. Poplaski is not confused. She is a savvy consumer unwilling to sign her name to a form that does not have full disclosure.
Mr. Joffe-Halpern's statement is probably not legally binding nor are those made by the Connector or legislators who are giving constituents various explanations about this clause. What will probably be legally binding is the multi-purpose Commonwealth Care application that says the estate can be recovered. A good attorney would advise you never to sign any document that has things in it that the other party told you "not to worry about, it doesn't apply to you."
I recently read some information that was compiled for outreach workers who are unsure how to advise potential applicants concerned about estate recovery with regard to Commonwealth Care. At the top of the page is a disclaimer stating that this is not intended as legal advice; it is a summary of statements made by people knowledgeable about the topic. The content is based on a discussion with Jeff Luekens, an attorney with experience in public health insurance programs. It says that there are no current regulations that would authorize Commonwealth Care to seek and obtain estate recovery; that the Commonwealth could create one in the future, but this has not happened. It goes on to say that the clause specifically gives the right to MassHealth to pursue estate recovery and that in other parts of the form, rights are given specifically to named programs.
Mr. Leukins suggests that if Commonwealth Care is not specifically named for estate recovery, it does not have that right. Not to discredit Mr. Luekens, but this piece could have also stated that people are not legally protected from estate recovery if they sign this form as it is now; they will have no protection if the current regulations are changed.
Mr. Joffe-Halpern also claims that estate recovery applies to MassHealth members but only in limited situations. He has this backward. The conditions under which MassHealth will not pursue an estate are limited; the system is set up to go after estates and the probate courts inform MassHealth as part of their process.
If the state or the Connector have no intention of pursuing the estates of Commonwealth Care members now or in the future, the application should be revised. It's that simple. Actually, there will be some extra work and expense involved as they will have to legally notify those who have already enrolled, and there will be a few more caveats to deal with, but these can be taken care of as soon as the form has been revised.
To the cash-strapped Massachusetts health care reform, estate recovery looks like easy money, especially if a mortgage is nearly paid off which could very well be why the magic numbers start at age 55.
DIANNE BRIDGES
Lenox, Massachusetts
----------
"Cost of health initiative up $400m: Number expected to seek coverage exceeds earlier estimate"
By Alice Dembner, (Boston) Globe Staff, January 24, 2008
Spending on the state's landmark health insurance initiative would rise by more than $400 million next year, representing one of the largest increases in the $28.2 billion state budget the governor proposed yesterday.
The biggest driver of the cost increase is projected growth in the number of people signing up for state-subsidized insurance, which now far exceeds earlier estimates.
State and federal taxpayers are expected to bear nearly all of the additional cost.
Although the price tag for the initiative is ballooning, the governor yesterday reaffirmed the state's commitment to ensuring that nearly every resident is covered.
"We have fully-funded healthcare reform," Governor Deval Patrick said at a news conference. Patrick listed the initiative among several programs started by previous administrations that he supports.
But the long-term cost of the insurance initiative continues to concern pol icy makers and analysts, who are worried that it may become unaffordable.
"These increases are more than anticipated, so we absolutely have to find ways to hold down the rate of growth in future years," said Michael Widmer, president of the Massachusetts Taxpayers Foundation, a business-funded budget watchdog that has supported the initiative.
This year the state is expected to exceed the initial budget for the health insurance initiative by about $245 million, and next year's budget would boost spending by another $400 million.
The budget now goes to the Legislature, which last year accepted the governor's recommendations on funding the health insurance initiative. A final budget is expected to be approved by the end of June.
The state's top budget official, Leslie Kirwan, said yesterday that projecting costs for the health insurance initiative is difficult because the state is in "uncharted territory."
"We're ultimately working with a lot of uncertainty about the number of uninsured that remain out there in the population," said Kirwan, secretary of administration and finance and chairwoman of the state panel overseeing the health insurance initiative. "Every significant decision we've made in healthcare reform" that draws on enrollment projections is based on "our best educated guess."
The administration is currently working to develop a better way to count the uninsured.
When the law mandating that nearly all Massachusetts residents have health insurance was signed into law by then-governor Mitt Romney in April 2006, the state estimated that about 400,000 residents were uninsured.
Census estimates of the uninsured were far higher - about 650,000 - and many independent observers suggest that the truth lies somewhere in between.
Officials had projected that about 140,000 would enroll in the new state-financed insurance plan, called Commonwealth Care, which provides full or partial subsidies.
But by the end of last month, 169,000 people had signed up for Commonwealth Care, and the state is now estimating enrollment will reach 225,000 by June 2009, the close of the next fiscal year.
More than 70,000 have obtained Medicaid coverage since the law passed expanding eligibility, and the cost for covering those additional people, plus rate increases for hospitals, doctors, and others, is projected to grow significantly above this year's spending.
Those who don't qualify for subsidies or Medicaid are expected to buy private insurance or remain uninsured. Illegal immigrants are not subject to the insurance mandate or eligible for state insurance, but they can qualify for free care.
When the initiative was approved, the state expected that over time there would be a significant drop in spending on healthcare for the uninsured. The initial funding plan counted on shifting a significant portion of those "free-care" costs to pay for insurance subsidies.
But that shift is not going to happen to any large extent in 2009, according to the proposed budget.
To fund the overall increases, the state is counting on getting about half from the federal government. But officials have just begun negotiations on how much Massachusetts will actually receive.
Patrick said he is optimistic about federal support, but acknowledged that "nothing is certain."
Separately, the state is counting on $5 million in revenue from businesses that don't provide insurance for their employees, down from the $24 million included in this year's budget that has not materialized.
-
Alice Dembner can be reached at Dembner@globe.com.
----------
"Doctor shortage is major issue"
The Berkshire Eagle - Letters
Thursday, January 31, 2008
I read with gravest concern the articles about the looming shortage of primary care physicians. In the last five to six years, I have had three very good, very qualified primary care doctors, none of whom stayed more than a year or two before they were gone. I made the last one promise he was not going to leave, because I just established a relationship, and he said he was here to stay. In a year and a half, he was gone. Since that doctor has left, nobody has been hired to replace him, and I now see physicians' assistants.
It is a great thing for Massachusetts to be a leader in getting health insurance for everyone in the state, but we need to face the fact that health insurance without doctors is a moot point. One of the signs of a third world country is the lack of health care. I think we are sliding in that direction. Additionally, how can you build an area economically when people find out that primary doctors are impossible to get? Do you think they will want to come here?
We need to call upon Gov. Patrick, Reps. Guyer and Olver and Sens. Downing, Kerry and Kennedy to let them know that one of our greatest problems is out of hand and not being addressed. The doctors cannot solve this problem and the insurance companies will not solve the problem, and with the cost I pay for health care, I think it should be available. I know nowhere to turn for a solution, except to the legislators.
EUGENIE DANIELS
Williamstown, Massachusetts
----------
THE BOSTON GLOBE: Op-Ed: ALISON BASS
"An underinsured kick in the groin"
By Alison Bass, January 21, 2008
THE NEARLY 300,000 Massachusetts residents who signed up for health insurance under the state's new initiative are in for a rude awakening. They may now have some form of coverage, but many of them, even the very poor who used to get free care, are going to be socked with steep medical bills.
Welcome to the shadowy world of underinsurance, where high premiums, copays, deductibles, unexpected co-insurance charges, and skimpy coverage have put the lie to the dream of health coverage for millions of Americans. According to a 2005 Kaiser Foundation study, more than 58 million Americans already find themselves in this category: underinsured and at high risk of incurring punishing medical bills. My family is among them.
On Aug. 17, my 14-year-old son was kicked in the groin during a preseason soccer match. He could barely walk and was in considerable pain, his testicles having swollen beyond proportion. The urologist at our community hospital suggested an ultrasound to make sure there was no internal damage. Since it was late on a Friday afternoon, the doctor recommended that my son go to the hospital's emergency room for the scan. The results, fortunately, were benign and my son recovered quickly.
But a month later, the bills started flooding in: hundreds of dollars from the hospital ER, plus a few hundred more from several ER doctors and the urologist who treated my son. We also owed hundreds more for other medical services my family and I had used. On top of that, we still were obligated to pay hundreds to the orthodontist for my son's braces and several hundred dollars to podiatrists for services not covered by our plan.
By last fall, we owed nearly $3,000 in medical expenses. The bills had begun accumulating shortly after my husband, a social worker, switched jobs and we were forced to change health insurance from a local Blue Cross plan to a for-profit national plan. My husband was not offered a choice of health plans, and when we signed up it was not made clear that our deductible for the year would be $3,000 (for in-network expenses; $4,500 for out-of-network expenses).
Nor did we understand that once we met the deductible (i.e., spent $3,000 to $4,500 of our own money), we would then have to pay co-insurance: 15 percent of every in-network expense we incurred and 45 percent of any out-of-network expenses. Some Massachusetts residents who sign up for health insurance under the state's new plan will face even higher premiums and deductibles. Even some low-income residents who used to get free care will have to pay co-insurance charges that they may not be able to afford, according to Physicians for a National Health Program, which advocates for single-payer national health insurance.
It wasn't until my son's injury that we began to experience what it was like to be underinsured. As the bills piled up, I could only imagine how much worse it must be for the millions of those with less health coverage or none at all.
Fortunately, we found help. After a few calls, I was directed to the Access Project (www.accessproject.org), a Boston nonprofit that helps people throughout the country negotiate unaffordable medical bills. Andrew Cohen, Access Project's community research coordinator, gave me advice on how to appeal our medical bills, not only with our local hospital but with our health insurer as well.
With the latter, I argued that we had already satisfied our $3,000 family deductible for 2007, having spent more than that amount in medical expenses; thus we should have been covered for some of the expenses incurred from my son's ER visit as well as any subsequent medical services.
The local hospital forgave the balance of our debt to it, while the insurer repeatedly denied our appeals. In the process, I discovered that the company, which paid its CEO more than $17 million in salary, bonuses, and stock options over the last two years, was playing a shell game with us.
Instead of counting the full amount of our medical bills toward the deductible, the company only included a lower "discounted" amount and excluded the cost of our co-insurance charges. According to the Access Project, such tactics are not that unusual. But they often go unnoticed because of the sheer complexity of the system.
This experience has taught me that our system of private health insurance is badly broken and individual states cannot institute reform alone. We need universal healthcare on a federal level and more organizations like Access Project to tide us over until we get it.
-
Alison Bass is a former medical writer for The Boston Globe and author of the forthcoming book, "Side Effects: A Best-selling Drug on Trial."
----------
"Recognizing progress in Massachusetts health reform"
The Boston Globe, Letters, February 1, 2008
ROBERT KUTTNER'S Jan. 26 op-ed "A health law with holes" was misleading. As one of the designers of the Massachusetts law and a current member of the Commonwealth Connector board implementing the law, I would like to clarify the issue for your readers.
Kuttner criticizes the individual mandate without offering a concrete alternative. Without an individual mandate, universal health insurance coverage is impossible. In our nation today, more than one-third of the uninsured are already offered free or heavily subsidized insurance and choose not to take it. A plan such as Senator Barack Obama's is an excellent step forward, but would not provide universal health insurance coverage. By my estimates his plan would leave about 15 million Americans without health insurance.
The only way to get to universal coverage without an individual mandate is to move to a single payer system where every citizen is given free government-provided insurance without charge. Such a system would cost many multiples of the current Massachusetts reform effort. So it is misleading for Kuttner to criticize our current plan on its cost without highlighting that the alternative is either non-universal coverage or a plan that would make our current efforts look cheap by comparison.
JONATHAN GRUBER
Lexington, Massachusetts
The writer is a professor of economics at the Massachusetts Institute of Technology.
--
The Boston Globe, Op-Ed, ROBERT KUTTNER
"A health law with holes"
By Robert Kuttner, January 28, 2008
JON KINGSDALE is a good man playing a bad hand dealt him by the Massachusetts Legislature and the Bush administration.
Kingsdale heads the Commonwealth Connector, created in 2006 by then-Governor Mitt Romney and the Legislature, as part of an effort to cover most of the state's uninsured. Kingsdale takes justifiable pride in having brought health insurance to more than 300,000 Massachusetts residents.
However, as the Globe recently disclosed, the program's costs are outstripping its projections by $245 million this year, and $400 million next year. This is not Kingsdale's fault. The program's designers underestimated the uninsured by some 200,000 people (costs of service are also rising). By doing his job - reaching those without coverage - Kingsdale adds to the program's costs.
The Massachusetts program, by going beyond standard Medicaid (which is 50 percent federally funded), needed a waiver of federal rules. The waiver must be renegotiated this year. President Bush has mandated cuts in state aid - during an economic downturn no less - using a characteristically backdoor directive that limits states' ability to extend health coverage beyond the poor. Going forward, Massachusetts will bear more of the program's cost.
The deeper problem is the program's piecemeal design, and the Legislature's failure to levy more than a token annual tax of $295 per worker on businesses that take a free ride by failing to cover employees. If the law had charged delinquent employers the actual cost of decent insurance - more like $5,000 a year - the state would have adequate funds for the uninsured.
By addressing only the poor, near poor, and those without "access" to employer coverage, but not the whole system, the 2006 law produces perverse results.
For the poor, decent insurance is heavily subsidized under an expanded version of Medicaid. For lower-middle-class people without employer-provided insurance, the Connector has worked with private insurers to offer affordable plans partly subsidized by the state ("Commonwealth Care"). Most of this insurance, Kingsdale noted in an interview, is a lot better than what people had before.
Yet another layer of the cake, "Commonwealth Choice," offers unsubsidized plans for moderate income people without access to insurance. But approved plans with affordable premiums have high deductibles and copays - while plans with affordable out-of-pocket charges have high premiums. A family that can only afford lower-premium plans can incur as much as $10,000 in annual costs, plus premium costs, if a member becomes seriously ill.
But people whose employers offer insurance coverage (the vast majority) get scant benefit from the new law, and the program largely fails to address escalating deficiencies in employer-provided plans. Rather, the law legislated an "individual mandate" requiring everyone to get insured one way or another.
Bottom line: the reform helps a great many uninsured but compounds a crisis that Dr. Marcia Angell, former executive editor of the New England Journal of Medicine, calls "coverage without care." As employers and insurers contain their costs by shifting them to individuals, more people find that their insurance fails to pay many expenses when they are sick.
So as a middle-class Massachusetts resident not eligible for the 2006 program, here's what you get: If your employer offers lousy coverage, or sticks you with most of the premiums, you must still buy the plan, or some other plan, or the state penalizes you. The Connector's website helpfully trumpets in large type, "New Penalties for 2008."
This idea of an individual mandate absent comprehensive reform - how to say this politely? - is nuts. It makes a social failure the problem of the individual. As Angell points out, "It gives the idea of government-sponsored universal coverage a bad name."
When Lyndon Johnson devised Medicare in 1965, he didn't order senior citizens to go out and buy private insurance, adequate and affordable or not, or be fined. Medicare covered everyone, bypassing the notoriously inefficient private insurance industry.
Barack Obama has been criticized by some for not including an individual mandate in his health plan. But Obama is correct. The individual should not be punished for government's failure to do reform right. Universal social insurance signals government help. A mandate signals government coercion.
Kingsdale says he is betting that the holes in the current reform will logically lead to more fundamental reforms. I sure hope he's right. But I'm with Marcia Angell. The Legislature, by building half a bridge, has set up one more perceived government failure.
-
Robert Kuttner is co-editor of The American Prospect and a fellow at Demos, a New York-based think tank.
----------
"Subsidized care plan's cost to double: Enrollment is outstripping state's estimate"
By Alice Dembner, Boston Globe Staff, February 3, 2008
The subsidized insurance program at the heart of the state's healthcare initiative is expected to roughly double in size and expense over the next three years - an unexpected level of growth that could cost state taxpayers hundreds of millions of dollars or force the state to scale back its ambitions.
State projections obtained by the Globe show the program reaching 342,000 people and $1.35 billion in annual expenses by June 2011. Those figures would far outstrip the original plans for the Commonwealth Care program, largely because state officials underestimated the number of uninsured residents.
The state has asked the federal government to shoulder roughly half of the program's cost from 2009 through 2011, but there is no guarantee of that funding. Commonwealth Care provides free or subsidized insurance for low- and moderate-income residents.
"The state alone cannot support that kind of spending increase," said Michael Widmer, president of the Massachusetts Taxpayers Foundation, a business-funded budget watchdog group.
Even with federal backing, the state may not be able to afford the insurance initiative as designed, because the law did not make any attempt to trim wasteful health spending, said Alan Sager, a Boston University professor who specializes in healthcare costs.
Currently, 169,000 people have enrolled in the program, which is expected to cost $618 million in the fiscal year ending June 30. When it authorized the program in 2006, the Legislature estimated that about 215,000 people would eventually be enrolled at a cost of $725 million. State officials in late 2006 reduced that estimate to between 140,000 and 160,000 - a number that was surpassed last year.
"We're paying the price of our own success," said Widmer.
The administration of Governor Deval Patrick produced the new estimates to launch negotiations for federal funding, and has shared them with some state health leaders at closed-door meetings. Patrick is seeking about $1.5 billion over three years, half the cumulative cost for Commonwealth Care. The administration declined to discuss the numbers or the assumptions behind them, citing the ongoing negotiations.
In a statement, however, the governor's spokesman, Joseph Landolfi, said, "It is clear that paying for healthcare reform will pose a much greater fiscal challenge than was anticipated by the previous administration. We are committed to making health reform a success by aggressively pursuing cost savings and efficiencies in the healthcare system, as well as working with legislative leaders to review options for additional state revenues so that we can continue to afford this important initiative."
The expanding need for new state and federal money is in sharp contrast to the statements made by former governor Mitt Romney, when he proposed the initiative in 2004 and as he campaigns for president. He has repeatedly suggested that the state could insure low-income residents largely by reallocating money paid to hospitals and health centers that serve the uninsured.
"The bill that I submitted to the Legislature didn't cost $1 more than what we were already spending," he said Wednesday night during a GOP debate. "However, the Legislature and now the new Democratic governor have added some bells and whistles."
In fact, Romney signed the law in 2006 as modified by the Legislature, approving most of the changes, but vetoing a few provisions that were overridden. Lawmakers then estimated that the initiative would cost the state only a small amount of new money in the first few years. It is now apparent that both Romney and lawmakers underestimated the cost of insurance subsidies as well as other parts of the initiative, largely because they based their projections on low estimates of the number of uninsured and the rising price of insurance. When the law was passed, neither Romney nor the Legislature estimated the costs beyond next year because they believed the enrollment growth would be all but complete.
From the beginning, many health policy specialists said the initiative would cost the state more than expected. Now, some say, the benefits of reaching near-universal insurance coverage may counterbalance the financial pain.
"I wouldn't say there's an imminent danger that the whole thing is going to collapse," said Robert Seifert, senior associate at the Center for Health Law and Economics at the University of Massachusetts Medical School. "It's challenging, but if it's a priority for the administration, then I think it's doable. There are benefits that don't appear in the budget numbers," including healthier residents, who are less of a financial drain in the long run.
Government-funded costs of another part of the insurance initiative - expansion of the state's Medicaid program, called MassHealth - are also projected to grow significantly. The state is also seeking federal reimbursement for half of those expenses.
MassHealth covers the poor and disabled who have minimal financial assets. Commonwealth Care provides free or subsidized insurance to those who don't qualify for MassHealth but have low to moderate incomes and no access to insurance through work.
Overall, spending on the healthcare initiative will total about $1.95 billion this year. Slightly less than half of that will be funded by the federal government, with the rest coming from state taxpayers and other sources.
If the state doesn't get all of the federal funds it is seeking, policy makers could face difficult choices: spend more state money or cut back the two programs by reducing enrollment, cutting subsidies, or eliminating benefits.
"We need that [federal money] to be able to continue the effort to provide MassHealth and Commonwealth Care to everyone who is eligible," said Thomas Dehner, director of MassHealth.
Dennis Smith, the federal official who will negotiate the details of the federal contribution, declined to comment about the state's request for more money.
The federal government has supported that state's insurance experiment so far - contributing about $300 million for Commonwealth Care since it began in October 2006 and millions more for other parts of the initiative. But the Bush administration has also been trying to curb federal spending in the Medicaid program, which would be the source of the new money Massachusetts is requesting.
Negotiations on the state's latest funding request are expected to wrap up by July 1.
The financial pressures come as the state struggles to balance the budget for next year, and as the federal economy appears headed for a downturn. The budget proposed by Patrick on Jan. 23 included money for the first wave of the projected increase in Commonwealth Care - $869 million, a figure some observers suggest may itself be too low because of growing enrollment and healthcare costs. The budget counts on the federal government paying less than half of that total.
There has been no discussion of a tax increase to pay for the healthcare plan.
One architect of the initiative said the state should work to build public backing for the measure.
"I hope that the citizens of Massachusetts are willing to provide the support to maintain our status as the only place in the nation that offers universal coverage," said Jonathan Gruber, an MIT economist.
Two sources of money that were part of the original financing plan have fallen short, contributing to the budget crunch. As more uninsured residents were covered, the state had expected to shift hundreds of millions of dollars from free care to insurance subsidies, but the drop has been slower than predicted.
Lawmakers had also counted on collecting tens of millions of dollars from businesses that do not insure their workers. But the Romney administration reduced the number of businesses subject to penalties, and the state expects to collect only about $5 million from them this year.
Sager suggested that the state look to another source to make up the difference: multimillion-dollar payments to hospitals that were included in the law to win political support.
"It would be tragic to renege on the law's promises to cover all citizens of the Commonwealth, especially if those promises can be redeemed by . . . repealing the ill-targeted, unnecessary, and unaffordable Medicaid rate increases to hospitals that are already enormously profitable," Sager said.
-
Alice Dembner can be reached at dembner@globe.com.
-

-
----------
A Boston GLOBE EDITORIAL
"The health law is working"
February 10, 2008
DON'T BE fooled by the national press coverage suggesting the Massachusetts health plan is in trouble. The plan is suffering from a bit too much success, but the state has the resources to pay for it this year and next.
Enrollment in Commonwealth Care, the subsidized insurance offering, is higher than anticipated, but Governor Patrick and the Legislature are ready to pay the extra costs this year. In the fiscal year that begins this July, the governor has budgeted $869 million for Commonwealth Care, but over half that increase will be defrayed by the federal government. Rising costs are inevitable as the plan is rolled out.
Barring a financial collapse, the state will have the money to pay for the health initiative through fiscal 2009. In case more is needed, House Speaker Salvatore DiMasi and Senate President Therese Murray are talking about a cigarette tax increase. The Legislature will not let this initiative fail for want of money.
The state needs continued federal support for the plan. To seek this aid, it has to make three-year cost estimates. Much is uncertain about healthcare economics over the next few years, so it is wise not to panic about imprecise forecasts - in this case a $1.35 billion cost in 2011. Instead, providers, insurers, consumers, businesses, labor, and the government need to unite around a campaign to control costs.
Even though Massachusetts is a high-cost state, buffeted by competitors on all sides, and dependent on federal policies it cannot control, its elected representatives resolved to do what no state has ever attempted: require everyone (with hardship exemptions) to get health insurance and provide the means for most of them to afford it.
In a little less than two years, here's what Massachusetts has achieved:
Expanded Medicaid by 60,000 for the poor and near poor and children.
Established Commonwealth Care to provide insurance for adults living near poverty - more than 169,000 enrolled.
Created Commonwealth Choice policies for more affluent people - 16,000 enrolled.
Merged the individual and small-group markets so the self-employed can buy affordable insurance and encouraged businesses to set up programs so employees could get a tax savings on premiums - tens of thousands more enrolled in private insurance.
Structured an individual mandate so penalties only fall on those for whom affordable coverage is available.
Provided a national model to show how different interest groups can unite to support significant social progress.
Governor Arnold Schwarzenegger's plan to do something similar died in a California Senate committee recently. In Massachusetts, the coalition behind the health reform law is holding firm. The plan itself is creative and sound. Who dares call this a failure?
----------
www.boston.com/bostonglobe/editorial_opinion/letters/articles/2008/02/10/estimated_cost_of_states_health_plan_raises_alarm/
----------
The Boston Globe - Letters
"Estimated cost of state's health plan raises alarm"
February 10, 2008
THE COST of the new Massachusetts health plan was quite high to start. Now estimates have spiked just as it leaves the gate ("Subsidized care plan's cost to double," Page A1, Feb. 3). Among folks who run households, pay taxes, and struggle to get by, there's one pretty obvious thought: Pull the plug now.
Meanwhile, with no sense of irony, other folks decry inadequate public school funding, high local taxes, and the lack of sufficient state aid to municipalities. They talk about the long list of additional social services our governor ought to rush to provide.
It's fine to wish to expand idealistic social programs. But that doesn't mean you're free to ignore the math. Massachusetts just can't afford this healthcare program. If we pull the plug now, we can avoid the need to slash the state budget this summer and gut local aid. The only way this can happen is if our leaders have the courage to face the truth today. Otherwise, we can wait for the numbers to overwhelm us.
Healthcare costs are a huge national problem. Why are we so eager to be the guinea pigs to show the rest of the country what won't work?
BRIAN KEEGAN
Attleboro
-
IS THE choice between fighting cancer and financial ruin really a choice? That's the scenario too many Americans face without access to quality care. Last month the American Cancer Society released a report about the critical link between cancer outcomes and health insurance, a connection at the heart of the group's support for Massachusetts' healthcare reform law.
The real issue raised by Alice Dembner's front-page article is not unforeseen cost or revenue options, but rather how we respond to the latest test of our state's commitment to preserving quality care. There are long-term solutions to the revenue issue - a tobacco tax increase, for example - but sacrificing quality at the first sign of cost increases is the one thing Massachusetts cannot afford.
DONALD J. GUDAITIS
Framingham
The writer is chief executive of the New England division of the American Cancer Society.
-
JONATHAN GRUBER suggests that a single-payer system "would cost many multiples" of the current effort to expand health insurance coverage in Massachusetts through an individual mandate ("Recognizing progress in Massachusetts health reform," Letters, Feb. 1). Yet at least 18 studies conducted since 1991, including two that examined single-payer plans for Massachusetts in 1998, have found that a single-payer plan could provide comprehensive coverage for everyone while costing less than is now being spent. Savings in insurance overhead and hospital and physician office billing costs would more than offset the cost of providing access to care for those who now don't have it. Massachusetts should reconsider this cost-effective alternative to the increasingly costly approach now being attempted.
LEONARD RODBERG
New York
The writer is a research director with Physicians for a National Health Program.
------------
“Heath plan rates may rise 14%: State officials worry previously insured may enter program”, Also, “State weighs raising health plan rates 14%”, The Boston Globe: City & Region, Friday, February 15, 2008, By Alice Dembner, Boston Globe Staff Writer
To hold down state costs, officials are considering raising premiums as much as 14% and doubling some co-payments for the subsidized insurance program that is at the heart of healthcare reform.
State officials said they want to ensure that the program, called “Commonwealth Care”, does not collapse under the weight of soaring costs or under a potential influx of residents whose employers drop coverage because the program offers a better deal for their workers.
“If we are not only trying to insure the uninsured, but insure the previously insured, that is going to blow the doors off,” said Leslie Kirwan, the state’s top budget officer and chairwoman of the “Commonwealth Health Insurance Connector Authority” board that oversees “Commonwealth Care.”
But advocates and some members of the authority board that reviewed the proposed increases yesterday (2/14/2008) said the proposed hikes would price people out of the program. In addition, advocates called them unfair when compared with the 5% premium increase the state expects for unsubsidized insurance plans.
“We think it undermines the very principle on which the reform stands, to provide access to quality, affordable healthcare and to protect the poor and the most vulnerable,” said the Rev. Hurmon Hamilton, president of the Greater Boston Interfaith Organization, a group of congregations that advocates for healthcare access.
The proposed increases might be modified or avoided if insurers lower their prices for covering enrollees in the next fiscal year or if the state finds other sources of revenue. The state is currently negotiating with insurers who are seeking far more than the state wants to pay. Neither side would disclose the size of the gulf.
As proposed, the increases would affect about half of the 170,000 low-income people now enrolled in “Commonwealth Care”. The premium increases would apply to those whose income is above 150% of the federal poverty level. State residents are eligible for the program if their income is at or below 300 percent of the poverty level and they do not have access to work-based insurance.
Under the proposal, the lowest premium would rise from $35 to $40 a month, a 14% increase.
Jon Kingsdale, executive director of the connector, defended the proposed “Commonwealth Care” premium increases of $5, $10, or $15 a month as fair, adjusted for income, and far lower than most premium increases in private insurance. Kingsdale said that the subsidized program and the private insurance plans are completely different and that comparing the increases was like comparing apples to oranges.
Connector staff members, who proposed the increases, said they could help prevent the state plan from becoming so attractive that employers drop coverage for their workers and send them to “Commonwealth Care.” The state is already predicting that enrollment and costs for Commonwealth Care could double over the next three years.
“If we’re going to preserve political support and keep it economically viable, we’ve got to maintain some comparability between the benefits and contributions in “Commonwealth Care” and in the private market,” Kingsdale said.
Several connector board members opposed the increases, while others said they seemed reasonable and might be necessary to sustain the program. The board is expected to vote in 2 weeks on whether to impose any increases, after it reviews insurers’ bids. “It is too extreme,” said Celia Wcislo, a board member and assistant division director of Local 1199 of the SEIU. She said the state should look to insurers and hospitals instead to foot more of the cost.
In addition to the premium increases, copayments for office visits and prescription drugs could rise by $5 or $10, and some enrollees could see an increase in the total amount of out-of-pocket costs they must cover.
A Brockton mother of five children said those increases could make the plan unaffordable for her family. Mona Divers pays $37 a month in premiums for herself; the rest of her family has other insurance. With a heart condition, high blood pressure, high cholesterol, and a thyroid problem, she needs regular care and racks up copayments for office visits and prescriptions. Her husband's income of about $23,000 doesn't go very far, she said. The family is also paying off about $4,000 in medical bills run up before she enrolled in the state plan. "Back in September, when I signed up, I thought, 'Thank God I have Commonwealth Care to help me,' " she said. If the cost increases, she added, "I don't know if I'm going to be able to keep it up."
-
Alice Dembner can be reached at Dembner@globe.com.
-
www.boston.com/news/local/articles/2008/02/15/health_plan_rates_may_rise_by_14/
-
www.boston.com/news/local/articles/2008/02/15/health_plan_rates_may_rise_by_14?mode=PF
-----
Questions for Massachusetts on healthcare reform:
So “Commonwealth Care” should offer “worse” or "substandard" benefits than its respective competitors' non-subsidized or unsubsidized insurance plans?
So the low-income state residents receiving subsidized healthcare insurance (or "Commonwealth Care" are going to be asked to pay more money for a substandard product?
So the low-income state residents receiving this new subsidized healthcare insurance are going to be insured in name only with a substandard policy without really ever being able to afford the product and therefore will be unable to receive proper healthcare?
So these proposals to raise premiums and hike co-payments are really about the state’s revenue shortage in subsidizing insurance companies, compounded with the insurance companies demand for increased state subsidies?
How big is the financial gap between what the state is able and willing to pay the insurance companies and what the insurance companies’ subsidies costs the state, and how much additional public money is being requested by the insurance companies to the state for the next fiscal year for healthcare reform?
WHERE IS THE TRANSPARANCE IN STATE GOVERNMENT & ACCOUNTABILITY BY THE PARTICIPATING INSURANCE COMPANIES?
-----
Jonathan Melle's thoughts:
This is very BAD governance! The socioeconomic incentives are being DIMINISHED & substituted for private and bureaucratic special interests. The state is using PERVERSE INCENTIVES to induce the Federal Govenment to grant Massachusetts more federal dollars for "healthcare reform" so that Massachusetts will then give the lion's share of the cut to the participating insurance companies within its state borders and use the rest to cover their excessive operational costs for the next fiscal year.
In response to the first paragraph of the Boston Globe's 2/15/2008 news article: My thoughts are--That means subsidies to the participating insurance companies will increase, but costs will be inequitably born by low-income residents. That is robbing the common man to pay the corporate elite. That defeats the point in economically and financially subsidizing a "social" program.
Re the 2nd paragraph: My thoughts--That is NOT why employers would drop coverage. PLUS, the law mandates employers cover their full-time employees.
Re the 3rd paragraph: My thoughts--But then employers would be in violation of laws mandating healthcare coverage. The state is making a spurious argument.
Re the 4th paragraph: My thoughts--That means low-income residents will inequitably receive a 14% increase, while middle-income residents will receive a 5% increase in premiums.
Re the 5th paragraph: My thoughts--Proposed increases would make public subsidies to insurance companies even more meaningless than they are now! This is all so Massachusetts can shakedown the Federal Government for Federal Dollars and give it to their insurance companies in the false name of low to middle income residents who are uninsured. This is a SCAM!
Re the 6th paragraph: My thoughts--This really about the corporate interest of Massachusetts' insurance companies (financial institutions) + the bureaucratic interest of fiscal stability of the state government. Moreover, there is NO transparency and accountability on either the side of the corporations or the state government!
Re the 7th paragraph: My thoughts--That would be 85,000 low-income state residents, who most likely work multiple part-time jobs.
Re the 8th paragraph: My thoughts--This is a regressive revenue fee system! These low-income resident are paying the state $35/mo now, which is $420/yr, but the proposed next fiscal year, they may be paying the state $40/mo, which is $480 per year. That is a nearly 14.3% increase on the poor. When I do the math: $60*85,000=$5.1-Million more a year to the state from low-income working poor adults working multiple part-time jobs if the proposal is affirmed. If the proposal goes through as planned, Massachusetts Insurance Companies via the state will receive $40.8-Million next fiscal year from the poor. UNREAL!
Re the 9th paragraph: My thoughts--Jon Kingsdale is trying to debunk the inequity argument of +14% for poor v. 5% for middle-income residents. He is making a very BUREAUCRATIC argument!
Re the 10th paragraph: My thoughts--That is so the state can get more Federal Government dollars for "healthcare reform" to turn over to its insurance companies. Governance by SPECIAL INTERESTS in the false name of the People! The elites in Massachusetts are making a MOCKERY out of the common man.
Re the 11th paragraph: My thoughts--But poor people are getting a substandard product that is going to be more unaffordable if the proposal is affirmed in a fortnight.
Re the 12th paragraph: The vote will be at the end of February or the beginning of March, 2008. My thoughts--But hospitals are getting the SHAFT already! Public $'s for hospitals are going to the insurance companies under "healthcare reform".
Note: I have no written responses to the 13th & closing 14th paragraph.
My concluding thoughts:
If the state was truly rational -- "Economic Man" -- and truly wanted "healthcare reform" to produce SOCIAL BENEFITS for the COMMON GOOD, then Massachusetts would now be a SINGLE-PAYER healthcare system focused on the low-income residents. However, the state is NOT at all rational -- "Political Man" -- and Massachusetts' financial and economic interests lie with its corporate elite institutions or the private benefits for the corporate interest centering on their financial insurance companies owned by big banks and investment houses that sit within the state's borders in and around Boston, Massachusetts. "Healthcare Reform" in Massachusetts should be called "Public Subsidies for the private benefits of Massachusetts' Elites." This is similar in nature to the "Big Dig" and I deem it as government and corporate greed at its very worst!
------------
"Hit up relatively untapped source in health reform"
The Boston Globe, Letters, February 25, 2008
EGREGIOUS AND upside-down are how I describe the Commonwealth Care premium and benefit changes that have been proposed to the Commonwealth Health Insurance Connector Authority ("Health plan rates may rise by 14%," Page A1, Feb. 15). Officials justified the premium increase as an attempt to hold down costs in the face of a possible move by employers to drop their coverage because Commonwealth Care may offer their workers a better deal. However, the authority offered no evidence that any trend of this sort has developed since the healthcare reform law went into effect.
If the Connector Authority wants to discourage employers from dropping coverage, it has a much fairer means at its disposal than burdening those who are already struggling in a region with a high cost of living. It can raise the employer penalty for non-coverage from its present minimal $295 per employee per year to something that better reflects the cost of insurance. The authority might also strengthen enforcement of the employer fee, collections of which have fallen short of the anticipated totals.
I'm reminded of Willie Sutton, who, when asked why he persisted in robbing banks, answered: "Because that's where the money is." I urge the Connector Authority to go where the money is, not where it isn't.
DAVID SCHREIBER
Arlington, Massachusetts
------------
"Is health insurance affordable?"
The North Adams Transcript - Letters
Friday, February 22, 2008
To the Editor:
I was one of the uninsured. My family could not afford health insurance, even though it was offered by previous employers. I paid out of pocket for the care my children received from their pediatrician, who agreed to continue to care for them in spite of our lack of insurance. We have been lucky enough to not need much care.
Just before the law requiring medical insurance for Massachusetts residents became effective, my husband lost his job. The company that he had worked for 12 years was sold, and we chose not to relocate. He looked for work and for the first time ever, collected unemployment. We were provided with medical insurance through the unemployment insurance program. I chose a doctor and had a "full workup" done.
Not having seen a doctor since my children were born, I needed basic annual women's care as well as basic blood work (i.e. cholesterol screening) and urinalysis (i.e. protein checking for early diabetic screening). In addition, I needed a baseline mammogram. Needless to say, it was expensive. Of course, the insurance paid for it and my total out-of-pocket expense was $15.
Just as the law requiring medical insurance for Massachusetts residents became effective, our unemployment benefits ran out, and with it my insurance. Because we have very little cash flow, we qualified for MassHealth and were able to obtain it thanks to the help of EcuHealth. Since the doctor with which I had established a relationship is still in the process of being certified as a MassHealth provider, I need to choose a new provider who will want an initial visit with me and to see all of my test results.
There was no way to continue the benefits from the unemployment insurance medical insurance, even by paying a premium, or I would have to have been able to continue seeing my doctor. Now I am being urged to choose a new doctor and set up an initial appointment.
Still wondering why the cost of the new mandatory insurance is so high? As I see it, I can't be the only one who is experiencing this type of situation.
Jeanne Matthew
Adams, Massachusetts
Feb. 20, 2008
------------
"Physicians are still hard to come by"
By Jennifer Huberdeau, North Adams Transcript
Tuesday, February 26, 2008
NORTH ADAMS -- The Health Care Reform Act of 2006 has enabled Bay State residents to find affordable health insurance -- subsidized and unsubsidized -- but one thing the legislation isn't doing for patients is ensuring they will find a nearby primary care physician.
"It's been a challenge," Charles "Chip" Joffe-Halpern, executive director of ECU-Health Care, said Monday in regards to connecting patients with primary care physicians. "There are a few physicians that are accepting Commonwealth Care and have openings. It varies. We've had to refer a couple of clients to Pittsfield."
When the state Legislature signed the reform act into law, it also created Commonwealth Care, a subsidized health insurance where premiums are based on income guidelines, and Commonwealth Choice, an insurance program with multiple choices and premiums open to anyone without health insurance.
But unlike Commonwealth Cho-ice, where participants are covered by participating health insurance companies, Commonwealth Care clients are covered by program similar to the state-sponsored Mass-Health -- where physician's reimbursements are similar to that of Medicare and Medicaid.
Some physicians and physician groups, such as the Williamstown Medical Associates, the largest physicians group in North County with six primary care physicians and a number of physicians assistants and nurse practitioners, are not accepting patients with Commonwealth Care.
"We want very much to accept Commonwealth Care," Dr. Robert Jandl, president of Williamstown Medical Associates said Monday. "We're not able to accept it at this time, but hope to be able to in the future. It's a matter of working out a contract with the state, and we are in negotiations at this time."
He declined to comment on how many people had approached the doctors group about the need for a physician, saying that negotiations prevented further comment.
"There are very few places that are accepting it at this time," he said. "There are some genuine issues with the program -- that I can't get into -- but we are hoping to be able to accept it in the future."
However, Joffe-Halpern doesn't believe the problem lies with doctors not accepting the subsidized health insurance, but with a lack of primary care physicians.
"A lot of the doctors in the area who accept it already have full case loads," he said. "I think we're seeing a separate issue. Folks are accepting the coverage, but there's a bigger issue at work."
He said the state's health care mandate, which requires all state residents to carry insurance, created an even greater need for primary care doctors in the Bay State.
"It's highlighted the nationwide shortage, which is exacerbated in rural areas like ours," Joffe-Halpern said. "Some of our clients are being inconvenienced by having to go to Pittsfield for care, but hopefully that need will be ameliorated in the near future."
Commonwealth Care only provides coverage for adults who do not qualify for MassHealth, and fall below the income guidelines to qualify for the unsubsidized Common-wealth Choice. Children whose parents qualify for Commonwealth Care are covered by MassHealth.
------------
"Health reform costs rising: A vote tomorrow could boost the cost of subsidized insurance plans across the state"
By Jack Dew, Berkshire Eagle Staff
Wednesday, February 27, 2008
The cost of subsidized health insurance could be rising for thousands of Berkshire residents.
The board overseeing the state's health insurance reform is expected to vote tomorrow on a slate of increases to the subsidized Commonwealth Care health plans for people making up to 300 percent of the federal poverty level.
The proposal comes as the cost of Massachusetts' groundbreaking health reform has far exceeded expectations while adding roughly 300,000 people to the insurance rolls. The overrun this fiscal year has not been pinned down but is expected to be about $150 million, officials say. Gov. Deval L. Patrick's budget for the fiscal year that begins July 1 seeks $869 million to fund Commonwealth Care, an 84 percent increase.
Meanwhile, the governor has been lobbying federal officials to continue a waiver that allows Massachusetts to use federal money to help pay for Commonwealth Care.
The Commonwealth Health Insurance Connector board tomorrow will decide how much of the increased costs will be passed on to patients.
The premiums are set according to an individual's income. Someone making 150 percent of the federal poverty level, or $15,135 a year, would see his monthly premium rise from $35 to $40. A patient making 300 percent, or $30,630 a year, would pay $120 a month, up from $105.
A range of copays would likewise increase. A visit to a primary care doctor for lower cost plans would go from $5 to $10, while a trip to a specialist would go from $10 to $20, and the patient's share of prescriptions would also go up, doubling for most drugs.
Richard Powers, a spokesman for the Commonwealth Connector, said the numbers could still change before tomorrow's vote.
In addition to coping with increased costs, Powers said, the Connector wants to maintain parity between those on subsidized state plans and those who get insurance through an employer.
"It's a matter of fairness. It's not right that someone with private insurance should pay more in premiums and copays than his neighbor who makes the exact same amount of money but qualifies for Commonwealth Care," Powers said.
"Whether or not Commonwealth Care is even here in two or three years will depend on decisions like the one being made (tomorrow)," he said.
But health advocates say the increased premiums and copayments will put insurance and medical care out of reach for some residents.
Affordable Care Today, a coalition of more than 40 health organizations, sent a letter to the Connector board, urging it to vote against the increase and saying that higher copays — also known as "cost sharing" — will discourage low-income people from seeking treatment.
Brian Rosman, research director of Health Care for All, an advocacy group that champions expanded health coverage, said the proposal to increase copays in public insurance comes as many private plans are reducing them, particularly for chronic care.
"There is very good evidence that high copays discourage people from getting needed care, and we know that this leads only to higher costs in the long run, when small problems become big problems," he said.
In Pittsfield, Advocacy for Access has helped enroll hundreds of residents in Commonwealth Care. Its executive director, Pat Duma, said the impact of the proposed increases will depend on each individual.
"People ask us if these will be permanent rates, and we have always said that nothing is ever permanent, we are not even sure if (Commonwealth Care) is permanent, but this is how you can access health care today. And anybody who has had to get care or a prescription filled has said that this is a great program," Duma said.
Charles Joffe-Halpern, executive director of Ecu-Health Care in North Adams and a former member of the Connector's board, said the goal has always been to make Commonwealth Care as affordable as possible.
"That will always be balanced with the fiscal needs of the program," he said. "So we look forward to a good, open dialog about this."
------------
A Boston GLOBE EDITORIAL
"A fair share for healthcare"
February 27, 2008
THE AUTHORITY overseeing the state's new universal healthcare law is about to raise its rates on people who are living on limited incomes. This insurance is subsidized by the state, and the Commonwealth Health Insurance Connector Authority wants to make sure that co-pays and monthly premiums are high enough to discourage people from switching from private insurance. These costs should not be so high, however, that they are a burden for people with chronic conditions or discourage them from getting necessary care. When the connector board meets to set the rates tomorrow, actuarial prudence needs to be leavened by compassion.
Anyone in Commonwealth Care would face higher co-pays: $5 more for a prescription and $5 more for a visit to a primary care provider. That may not sound like much, but it adds up to a major burden for people with multiple ailments and several prescriptions, especially when it applies to those earning just above the federal poverty line - $10,400 a year for a single person.
And the monthly premium rates would go up for people from 150 percent to 300 percent of the poverty limit. Again, it might be just a few dollars a month, but when combined with increases in the cost of food and fuel, the total healthcare increase would strain the budgets of the very people that Commonwealth Care is designed to help.
Those premiums need to be high enough that people who can afford private insurance do not try to save money by flocking to the subsidized policies. Figures from the state Division of Health Care Finance and Policy show that the number of employers offering coverage was holding steady at a little more than 70 percent in 2007, the first full year of the Health Reform Law. No one knows what will happen this year, when uncertainty hangs over the economy, but there is as yet no compelling case for the connector to shift so much cost onto the insured.
The connector is still negotiating with the four providers of Commonwealth Care over the overall cost of the insurance. Rates will be going up, as they nearly always do. Yet one exception to this rule is the $295-per-worker penalty leveled on companies employing more than nine workers that do not offer insurance. The law mandates that the state reassess this figure every year to reflect the cost of living and usage of the free-care pool for the uninsured. Under the law, the penalty can go down, but it can never exceed $295.
The connector alone can't change that $295, but the Legislature ought to revisit the fee, at least to index it to the rate of healthcare inflation. The goal of the Health Reform Law - to cover nearly everyone in the state - is a shared responsibility that requires continual reassessment. If people on limited incomes must pay more, why not employers?
------------
The Boston Globe, Op-Ed, JOSEPH L. DORSEY AND DONALD M. BERWICK
"Dirty words in healthcare"
By Joseph L. Dorsey and Donald M. Berwick, February 27, 2008
THE CLOSEST you can come to heresy in today's healthcare policy debate is to suggest that managed care can help and that capitation is the best way to pay for it. No presidential candidate even whispers the terms. What a shame.
Massachusetts faces a $147-million shortfall this fiscal year in its subsidy for the universal insurance coverage that it courageously mandated two years ago. That raises a question: What system of payment will best support innovations that can make care less expensive and better at the same time? The easier solution - make care less expensive and worse at the same time - is neither necessary nor worthy of us.
The answer to the question is that healthcare should be managed in the same way, and for the same reasons, that school systems and air traffic are managed. Managed healthcare was a great idea when it first emerged, before the term got hijacked by insurance companies that claimed to manage care but in many cases only managed money.
We practiced medicine in one of the best managed-care systems in the nation: the former Harvard Community Health Plan. What made it great was the freedom of staff to think creatively about what patients really needed, and to reinvent care to meet those needs. Harvard Community Health Plan pioneered innovations that most US healthcare still pines for: electronic medical records, patient reminders, creative roles for advanced practice nurses and physician assistants, quality measurement, and more.
The financing system that allowed all that to happen is today as dirty a word as managed care, namely "capitation." That means bundled, prospective payment to an organization for the care of a defined population. In the case of HCHP, that population was our patients, enrolled through their employment-based health insurance, Medicare, or Medicaid. Our job was not to produce transactions. It was to take care of people, and that is what we did. Capitation gave us the flexibility to use our budget with creativity limited only by our imaginations and habits.
The innovations that managed care and capitation made possible were good for almost everyone. For example, with extended hours of service, off-hours telephonic access, and outreach, HCHP's population had a rate of emergency department visits less than half the statewide average. Thousands of people avoided needless hospital visits; they got more appropriate, less expensive, better coordinated care in office settings. Of course, our care systems were far from perfect, but our extensive investments in quality measurement enabled us to identify defects, and capitation gave us the resources to act swiftly and prudently to fix them.
Physicians worked on salary. We were supported to create proper clinical pathways for our patients. A strong professional ethic among our clinicians, reinforced by strong member presence on our board, and by extensive quality measurement, kept us from doing too little. "Managed care" did not mean "restricted care"; it meant "care that makes sense." We can recall a single instance of being told by management to withhold from a patient any care that we thought, based on evidence, could help.
When the term "managed care" got hijacked, the public rapidly lost faith. That is because the restrictive, often unspoken, principle of "manage the money, not the care" led to handcuffs on physicians' decisions, aggravating and annoying both patients and clinicians, and sometimes even causing harm. The backlash was violent, and it swept the good forms of managed care and capitation into disrepute.
Rage against managed care mounted as some CEOs reaped multimillion-dollar compensation from savings derived from limiting care. In the storm, successful models found too few champions.
So, America, we have a question. Would you like to think again about managed care and its financing mechanism, capitation? Details matter - a strong focus on patient satisfaction, compensation and incentives, sound leadership, transparent and sophisticated measurement and information - but done right, managed care works. We lived it. Maybe, properly defined and designed, these may not be dirty words after all.
-
Dr. Joseph L. Dorsey is former medical director at Harvard Pilgrim Health Care. Dr. Donald M. Berwick is president and CEO of the Institute for Healthcare Improvement.
-
------------
"Health care meeting canceled after insurance bids come in high"
The Associated Press (via Berkshire Eagle Online)
Thursday, February 28, 2008
BOSTON (AP) — New bids from four insurers who provide subsidized insurance under the state's universal health care law have come in far higher than expected.
Chairwoman Leslie Kirwan has canceled today's meeting of the Connector Board and instead is considering a public statement discussing the unanticipated cost growth and her hope the insurers can cut their proposed rate increases.
The insurers — Fallon Community Health Plan, BMC HealthNet Plan, Neighborhood Health Plan and Network Health — service the Commonwealth Care program. It provides subsidized health care to people earning up to three times the federal poverty level.
Last month, the board proposed raising co-payments on the 169,000 people covered by the program. The concern is the suggested rate increases won't be enough if coverage is more expensive than expected.
----------
"Patrick lukewarm on health mandate"
By Glen Johnson, Associated Press
Saturday, March 01, 2008
Barack Obama is no fan of the individual mandate that has been central to the successful launch of the Massachusetts universal health care law. He likes to cite its foibles as he criticizes his Democratic presidential rival, Sen. Hillary Rodham Clinton of New York, for including a similar mandate in her national health care plan.
Gov. Deval L. Patrick has been noticeably silent as Obama has leveled his criticisms, as he did during a nationally televised debate this past week. It turns out it is not just because he has endorsed his fellow Chicagoan for president.
It sounds as if Patrick has a lukewarm view of his current homestate's provision himself.
"It's a feature," was what the governor first mustered on Wednesday when asked about the mandate. It required everyone in Massachusetts to have some form of health insurance by Jan. 1.
Patrick went on to say, "I think it's a component; if it were freestanding, if it were all on its own, it wouldn't make any sense. Otherwise, you could cure homelessness by ordering everybody to buy a house."
The governor added that requiring people to get health insurance — which has proved fundamental in helping reduce the number of insured in the state by 300,000 since the law went into effect — will make no sense going forward if premium costs continue to rise.
Fresh proof of that challenge came Thursday, when state officials postponed a meeting where they were to consider rate increases for those buying subsidized policies. Bids from the four insurers who were to provide the coverage came in far over budget, so the officials were forced to consider alternatives.
"We have a whole lot more work to do to make the overall system costs affordable to people, and obviously, we want to make sure that we're not penalizing people for not buying something they can't afford," Patrick said.
Under the terms of the Massachusetts plan, the state government is providing free coverage to the most needy, offering subsidies for those struggling to pay the cost, and has helped create discounted policies for those left to pay for coverage on their own.
Those who have not signed up face a series of escalating fines unless they get a hardship exemption.
State officials have estimated that could be 60,000 people.
"I have no objection to Senator Clinton thinking that her approach is superior, but the fact of the matter is ... we still don't know how Senator Clinton intends to enforce a mandate, and if we don't know the level of subsidies that she's going to provide, then you can have a situation, which we are seeing right now in the state of Massachusetts, where people are being fined for not having purchased health care but choose to accept the fine because they still can't afford it, even with the subsidies," Obama said Wednesday night during a debate in Cleveland.
The senator added: "They are then worse off: They then have no health care and are paying a fine above and beyond that."
Patrick drew the line at that comment. He said he disagreed that anyone is worse off for the institution of the plan.
"No," the governor declared. "The system as a whole is about getting insurance to everybody, but just ordering people to have insurance, without the other components, is just not going to work."
He added: "A mandate with cost controls, and the other features of our system, including the subsidies where they apply, is part of what we have here and what we're trying to make work."
The bifurcated opinion illustrates two points.
First, the danger in endorsing someone for political office is that you can become liable for their negatives as much as you might become the beneficiary of their positives.
Second, Patrick's muted support for the mandate highlights his challenge as he implements a program signed into law by someone else.
That has left Patrick walking the fine line between a policy that appears to be working and an enactment tool for which he — and Obama — have little regard.
----------
"Blue Cross chief earned $3.6m in '07"
By Jeffrey Krasner, Boston Globe Staff, March 1, 2008
Cleve L. Killingsworth, the chief executive of Blue Cross and Blue Shield of Massachusetts, earned $3.6 million in 2007, an 18.6 percent increase over his compensation in 2006. Killingsworth's bonus accounted for most of the additional money. It grew to $1.87 million last year, up from $1.36 million in 2006.
William C. Van Faasen, chairman of Blue Cross-Blue Shield through the end of 2007, earned $1.73 million in 2007, including a bonus of $1.23 million.
The salary disclosures are contained in a supplemental filing all insurers are required to complete this year for the Division of Insurance, and in the healthcare firms' annual reports.
The high salaries at Blue Cross con tinued to generate criticism, because the firm is a public charity. Blue Cross-Blue Shield, the state's largest health insurer, came under fire in November when it was disclosed Van Faasen received a $16.4 million retirement payment in January 2006, when he stepped down as chief executive. He continued as chairman until the end of 2007.
The Globe reported in January that Attorney General Martha Coakley is investigating the $16.4 million payment to Van Faasen.
Chris Murphy, a Blue Cross-Blue Shield spokesman, said the generous bonuses are part of an incentive package in which the payment is based on the aggregate performance over three consecutive years. "We can't offer things like stock options, and we compete with large public companies to get the executive talent," Murphy said.
State Senator Mark Montigny, Democrat of New Bedford, said the pay seemed excessive. "At a time when healthcare cost increases are rampant, and no one can afford healthcare - not the employee, not the employer, not the uninsured - these so-called charities are a pretty comfortable place to land," he said.
Blue Cross-Blue Shield's directors are also paid, unlike those at most nonprofits, earning from $47,400 to $53,900 a year.
At Harvard Pilgrim Health Care, the state's second-largest health insurer, chief executive Charles D. Baker earned $1.38 million last year, compared to $1.57 million in 2006, a decrease of 12.5 percent. Directors earn from about $20,000 to $30,000 a year.
James Roosevelt Jr., chief executive of Tufts Health Plan, earned $1.19 million in 2007, including a bonus of $552,909. Directors earn between $11,500 and $29,000.
The insurers also reported financial results. Blue Cross-Blue Shield, with about 3 million members, said it earned $53.4 million in operating income and $156 million from investments in 2007. It had revenue, mostly premiums, of $6.7 billion. The average premium increase was 7.5 percent, it said.
Harvard Pilgrim said it earned net income of $45.6 million in 2007 on revenue of $2.5 billion. It was recently named the top commercial health plan in the United States for the third consecutive year according to the National Committee for Quality Assurance.
Tufts Health Plan reported net income of $110 million on revenue of $2.2 billion.
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
----------
"Senate president to unveil plan to control health care costs"
The Berkshire Eagle Online, Monday, March 03, 2008
WORCESTER, Mass. (AP) — Senate President Therese Murray is pushing a bill requiring the state to adopt electronic medical records and ban pharmaceutical marketing gifts.
The bill sets aside $25 million to help create the statewide system of electronic medical records by 2015. Doctors would have to show competency in the technology for medical board registration.
Under Murray's bill, Massachusetts would be the first state to ban pharmaceutical marketing gifts. It bars representatives of pharmaceutical companies from offering them and bans physicians from accepting gifts of any kind. The ban extends to physicians' staff and family members.
The legislation allows distribution of drug samples to doctors.
Murray unveiled the bill today at the University of Massachusetts Medical School in Worcester.
----------
"Murray reveals health care plan"
By Hillary Chabot, Berkshire Eagle Boston Bureau
Tuesday, March 04, 2008
BOSTON — Senate President Therese Murray unveiled health care reform meant to boost primary care doctors in the Bay State and to force health insurers to explain any large rate increases.
The bill, filed with the Senate yesterday, also would implement electronic medical records by 2015 in an effort to curb the skyrocketing health care costs sparked by the universal care law.
"These initiatives will modernize the health care system, reduce waste and inefficiencies, and improve health care quality for every citizen of the commonwealth," Murray said in a statement.
Health care costs have increased by 60 percent in the past six years, Murray said. The cost of implementing the landmark health care reform law has cost the state $150 million this year, as more than 300,000 people signed up for state-funded insurance, said Senate Ways and Means Committee Chairman Steven C. Panagiotakos, D-Lowell.
Sen. Benjamin B. Downing, D-Pittsfield, said the cost of health care is one of the most important issues facing the state. He applauded Murray's move to give nurse practitioners a stronger role as primary care providers.
"This is a simple no-cost step which would help alleviate some of the backlog. In the Berkshires, some people wait six to eight months to see a primary care doctor when a nurse practitioner could provide a similar level of care right away," Downing said.
Support for electronic records
State Rep. William "Smitty" Pignatelli, D-Lenox, supports moving to electronic records.
"It will help the environment, it will cut down on paperwork. But we have to make sure we continue with broadband expansion," Pignatelli said. "The cost of health care is something we still haven't gotten a handle on, but every small step will help."
Panagiotakos said the electronic records could save the state "tens of millions, if not hundreds of millions, of dollars." Senators who hope to pass the bill before July assigned a hearing on March 12. The bill would put $25 million a year toward creating an electronic medical records system, funding that would come from a $1-per-pack cigarette tax that hasn't been filed yet.
Curbing costs
Michael Widmer, executive director of the Massachusetts Taxpayers Foundation, said the bill takes important steps to curb health care costs, including making sure insurance companies explain any increase over 7 percent.
"I think the public hearings and the seven percent marker will put important constructive pressure on the system," Widmer said. "At the same time, there is no cure-all, and there is no simple way to hold down health care costs."
The Massachusetts Association of Health Plans, which represents 12 health plans providing care to 2.4 million residents, supported the legislation.
The plan also would create a primary care recruitment center and expand enrollment at UMass Medical School for primary care students.
----------
-

--
www.boston.com/news/local/articles/2008/03/03/decline_is_seen_in_use_of_free_care/
--
"Decline is seen in use of free care: State health law having an effect"
By Alice Dembner, Boston Globe Staff, Monday, March 3, 2008
In one sign that Massachusetts' healthcare initiative is succeeding, use of the "free care pool" dropped by about 16 percent in the program's first year, as the state insured 200,000 low-income residents, according to new state figures.
The decline in free care use is a crucial measure of the impact of insuring people, and is being watched by the federal government and others to gauge the progress toward universal health insurance.
"It's very important to the financing of reform and to the goal of getting people better primary and preventive care," said Nancy Turnbull, associate dean at the Harvard School of Public Health and a member of the board overseeing healthcare reform. Turnbull said a long-term goal is also to reduce costs by keeping people with conditions that can be treated in a doctor's office out of the hospital.
But the state, which is counting on using former free care funds to help pay for soaring insurance subsidies, did not save any money on the pool in the fiscal year that ended Sept. 30, 2007, because it based its payments on the previous year's expenditures.
"We're seeing things trending down, but the real impact of all these changes is yet to come," said Sarah Iselin, commissioner of the Division of Health Care Finance and Policy.
State officials project an even bigger free care decline this year, one they are banking will bring actual savings of about $240 million. That drop is expected to come not only from insuring more people, but also from changes in the way hospitals are paid and in who is eligible for free care. The savings are included in the state's 2008 budget figures.
The free care program pays for medically necessary services provided by hospitals and health centers to the uninsured or underinsured. In fiscal 2007, the program covered 16 percent fewer medical visits than the 1.9 million in 2006, Iselin said, as patients shifted from free care to Medicaid or the state's Commonwealth Care insurance program. Funding for free care comes from the state treasury as well as from a tax on hospitals and insurers.
The overall decline in free care spending projected through fiscal 2009 is about $140 million less than anticipated by the Legislature when it passed the healthcare reform law in April 2006.
The savings, while significant, will only go a small way toward paying for insurance subsidies. The state estimates that subsidies for Commonwealth Care will total $869 million in fiscal 2009 as enrollment continues to grow.
In fact, reductions in free care spending were never expected to cover the total cost of subsidies, because insurance costs substantially more than the episodic visits paid through the free care program. The insurance program also covers a broader range of care, including prescription drugs, specialists, and visits to private doctor's offices.
State officials also believe there will be a continuing need for the pool, which has been renamed the health safety net trust fund. The program serves undocumented immigrants, who are not eligible for other insurance programs. It also pays bills for seniors with basic Medicare coverage who cannot afford large hospital copayments, and helps others of modest income whose medical bills, despite insurance, present a serious financial hardship.
And it serves people like Henry Murphy, who suddenly find themselves without insurance because of a change in job status or income.
When Murphy's heart unexpectedly conked out in November 2006, doctors were able to revive him and insert a pacemaker and defibrillator. But the 62-year-old Chelsea resident could no longer work as a tractor-trailer driver, leaving him uninsured - and in serious need of regular medical care.
With help from staff at Cambridge Health Alliance, Murphy got on Medicaid. Then, his Social Security payments put him over Medicaid's income limit.
Free care provided a bridge for two months until he could complete the enrollment process for Commonwealth Care.
"The system is excellent for people who don't have much," said Murphy, during a visit last week to Revere Family Health Center.
While on free care, Murphy got needed heart medication and care for his diabetes that kept him out of the emergency room, according to his doctor, Somava Stout. After moving to Commonwealth Care, he had heart surgery to replace a valve last November and is feeling better, but is often winded. He now pays $108 per month for the state-subsidized insurance.
Cambridge Health Alliance, one of the state's three largest providers of free care, saw a 2 percent increase in free care use last year, running counter to the state trend, according to chief financial officer Gordon Boudrow Jr. According to the Massachusetts Hospital Association, it was one of 29 hospitals where free care visits increased. Boudrow wasn't sure of the reasons, but suggested that the hospital's reputation for helping "cultural and linguistic" minorities, including immigrants, might be a factor.
Boston Medical Center, the state's number one free-care provider, saw the largest reduction in usage - 35 percent fewer free-care patients in one three-month period, according to vice president Tom Traylor. BMC was one of 37 hospitals that saw decreases, according to the hospital association.
Most hospitals and health centers assigned staff to help eligible patients transfer from free care to insurance.
The institutions have an additional incentive this year, because the state will no longer reimburse them for free care provided to patients eligible but not enrolled in Medicaid or Commonwealth Care.
In a report released last month, the hospital association questioned whether free care costs would decline this fiscal year as much as the state predicts.
-
Alice Dembner can be reached at Dembner@globe.com.
-
----------
"Health care question can't go on ballot without legislative OK"
The Berkshire Eagle Online, The Associated Press
Monday, March 10, 2008
BOSTON (AP) — The state's highest court won't force the secretary of state to put a proposed health care question on the ballot despite the Legislature's failure to vote on the measure.
The proposed constitutional amendment would guarantee comprehensive and affordable health coverage for all residents.
Lawmakers overwhelmingly approved the measure on an initial vote in 2004, but let it die without taking a needed second vote.
Supporters asked the state Supreme Judicial Court to put the question on the ballot anyway.
The court said that while the constitution required the second vote, it has no way of forcing lawmakers to act.
----------
"Health leaders seek to change payment system: Urge state to look at link between hospitals, insurers"
By Alice Dembner, Boston Globe Staff, March 13, 2008
To control soaring healthcare costs in Massachusetts, the state needs to overhaul how doctors and hospitals are paid, several healthcare leaders said yesterday during legislative testimony.
Last week Senate President Therese Murray proposed dozens of ways to cut costs, including an end to payments for botched treatment and increasing payments for demonstrated improvements in care. But yesterday two former chairmen of the Legislature's healthcare committee said those changes don't go far enough.
"The big bogeyman . . . is payment system reform," said Senator Mark Montigny, a New Bedford Democrat, at a hearing on Murray's bill and another proposed by health insurers. The state needs to take on "the cozy relationship" between the state's largest hospital system, Partners HealthCare, and its largest insurer, Blue Cross-Blue Shield, Montigny said.
John McDonough, executive director of Health Care for All and a former House healthcare committee chairman, said large healthcare providers, particularly hospitals, have driven up the costs through secret negotiations with insurers. He proposed that the state seek federal approval to impose a system in which payments would be made based on the service provided and not on who was shelling out the money or how much clout the provider had.
Spending on healthcare in Massachusetts grew 33 percent between 2002 and 2006, to $62.1 billion, Murray said yesterday, urging the joint Committee on Health Care Financing to support her bill. "We cannot afford to stand by and let this continue."
Murray's bill also contains a ban on drug company gifts to doctors, a requirement that doctors and hospitals switch to computerized records by 2015, and public hearings on any insurance company proposal to raise rates for any group of people by more than 7 percent a year.
Dr. Lucian Leape, a Harvard specialist on medical safety, said a much larger infusion of money is needed for the switch to computerized records than the $25 million a year proposed by Murray. Cost estimates top $500 million, and the state should tax insurance companies to pay that upfront price because they will get most of the savings, he said.
Jon Kingsdale, executive director of the Commonwealth Health Insurance Connector, said the state should require all insurers to explain price increases, not just those more than 7 percent. The Massachusetts Association of Health Plans, which represents most of the state's insurers, agreed.
Lawmakers also heard opposition to some provisions of the bill. A trade group representing pharmaceutical companies said the proposed ban on gifts to doctors could hurt patients by eliminating some company-funded research grants to doctors for medical experiments. The Massachusetts Medical Society, which represents doctors, said the ban could also limit support for continuing medical education programs that help doctors keep up with new research and treatments.
----------
"Health provider predicts big loss: Hospital alliance cites impact of reform law; Could cut 300 jobs, suffer $25m shortfall"
By Jeffrey Krasner, Boston Globe Staff, March 17, 2008
Cambridge Health Alliance, a key part of the Boston area's healthcare network, is facing a potentially "catastrophic" loss this year and is looking to eliminate up to 300 jobs, or about 9 percent of its workforce, in an effort to stabilize finances.
The alliance, which includes Cambridge Hospital, Somerville Hospital, and Whidden Hospital in Everett, says it is being hit hard by the state's new healthcare reform law, which has left it responsible for providing free care for those without insurance while reducing the hospitals' compensation for such services.
"A significant downturn in our volume and the transition to the new free care pool reimbursement system created a perfect storm for us," said Dennis D. Keefe, chief executive of the alliance.
Before healthcare reform took effect last year, Keefe said, Cambridge Health Alliance was reimbursed by the state for the full cost of providing services to the uninsured. Under the new system, "we only get 60 to 70 percent," he said. The reduction is particularly significant for the alliance because its hospitals serve a high percentage of uninsured patients. Despite the state's efforts to enroll all low-income residents in free or subsidized insurance programs, many still do not have coverage.
Keefe said the hospital was especially bruised in its second fiscal quarter, which ended Dec. 31, when the new payment system for uninsured patients took effect. Government payments for free care to the uninsured fell by nearly $14 million compared with the previous quarter, he said.
At the same time, the number of patients admitted to the alliance's hospitals dropped by about 3 percent, while patients kept overnight for observation - a category for which insurance companies do not pay as well - grew by 48 percent. Additionally, the number of walk-in patients, which do not generate as much revenue as inpatients, also grew substantially in the six months that ended Dec. 31, Keefe said.
During a department meeting last month, the chief administrative officer of the health system's physicians' group predicted a potential loss of $25 million to $35 million for the year.
"This would be catastrophic," Dave Porell told members of the Department of Psychiatry, according to the approved minutes of the meeting, which were obtained by the Globe.
On Friday, Gordon H. Boudrow Jr., chief financial officer of the system, met with bargaining representatives for nurses at Cambridge Hospital, who have worked without a contract since last summer. He said the system lost $13.2 million in the first six months of the fiscal year, and is on track to lose about $26 million for the year.
Cambridge Health Alliance is the last publicly funded healthcare system in the state. In addition to the three hospitals, the system includes 20 community health centers. It is the largest provider of mental health and addiction treatment services in the state. Of 348 beds in use, 45 percent are devoted to mental health and addiction treatment, an unusually high proportion.
Keefe said he has met several times with Dr. JudyAnn Bigby, state secretary of health and human services, to discuss the alliance's finances. Bigby, in an interview, said Cambridge Health Alliance posted a surplus of $1.6 million in fiscal 2007 and is receiving "substantially" more public funding this year than last year.
She acknowledged that the healthcare system is burdened because mental health services don't pay as well as complex medical procedures like heart surgery and cancer treatment. But she also said the state had compensated the alliance for payments that were delayed by the federal government.
"The Commonwealth will continue to support Cambridge Health Alliance with public funding as much as we can," Bigby said.
Keefe said the alliance is indeed receiving more money from the government this year, but that it is because of increased reimbursement for treating low-income patients, not additional funds to help the system stay afloat.
"It's accurate for her to say that payments have gone up, but you have to deduct the expenses for providing medical services," he said.
To stem losses, the health system has put in place a hiring freeze and eliminated discretionary spending, such as for travel and conferences. It is seeking to eliminate the use of contract nurses and other outside care providers, which cost more than using staff.
The system is also trying to keep more patients under its care for longer periods. It wants doctors to limit referrals to specialists or other physicians outside the alliance - something hospitals refers to as "leakage."
"All staff needs to continue to focus on keeping patients within our system, as appropriate, and to continue to focus on improving our inpatient volume in particular by increasing admissions on each campus each day," Keefe wrote in a Jan. 16 memo to staff. "We must also refer our patients for necessary services within our ambulatory care system whenever possible."
Keefe said the hospital is also exploring ways to combine services among its three hospitals to minimize duplication. Cambridge Hospital and Somerville Hospital are ripe for consolidation of specific services, he said, because they are close to each other.
The Massachusetts Nurses Association, in an update to its 400 members at Cambridge Hospital, said the alliance's financial problems are the result of poor management.
"The introduction of the new health reform law was years in coming, and the changes in reimbursement rates and other factors have been well known and should have been anticipated," the union said in a newsletter. "Our management built a budget that anticipated unachievable growth and set up this hospital for the failed situation it now faces."
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
----------
Therese Murray and Richard Moore
"Health care reform II: Bending the cost curve"
BOSTON, Massachusetts
Berkshire Eagle, Op-Ed
Wednesday, March 12, 2008
The first phase of Massachusetts health care reform took advantage of some of Massachusetts' historic strengths, most notably the state's high percentage of employer-sponsored insurance and its nationally low percentage of uninsured. This is not to diminish the enormity of its planning and implementation, which continues to engage state policymakers.
Considering the challenges we are facing now, however, the second phase of health care reform could be billed as an all-or-nothing proposition. Some health care experts have suggested that we have become a victim of our own success. In some ways, this is true.
Since health care reform became law in April 2006, we have enrolled more than 300,000 newly insured individuals. By most accounts, we are halfway to our goal of insuring every person in the commonwealth.
This has exceeded our expectations and brought some anticipated challenges. We knew, for example, that as more people entered the system, access to quality health care would become a greater concern due to the pre-existing shortage of primary care providers. And we understood that enrolling more people would contribute to escalating costs.
The irony is that the first step in health care reform was necessary, and yet we cannot continue to increase coverage without bringing down costs and advancing primary care. Our health care system could collapse under the pressure of such an unbalanced formula.
We should also remember, however, that health care cost-drivers have been threatening our system long before health care reform became law almost two years ago.
Now is the time to address those issues in the all-important second phase of health care reform. Health care costs have become the number one issue facing our economy. Rising health care costs are squeezing our state finances and cutting into resources for other essential public services, including education, public safety and transportation. These costs also make it increasingly difficult for young people, families and businesses, large and small, to make ends meet.
The Senate legislation announced last week seeks to control the cost curve through a comprehensive approach to the health care system. The bill is designed for the future of the commonwealth — to make health care efficient, sustainable and affordable, while increasing access to primary care and setting new standards for providers, insurers and drug makers.
This legislation attacks some of the biggest and traditional costs to consumers. For example, in an effort to halt years of double-digit rate increases, the bill requires public review of any insurance company submitting premium increases above 7 percent. This initiative will help peel back the curtain on how insurance companies themselves contribute to rising health care costs.
The Senate bill also requires an annual public hearing with health care providers and insurance companies to investigate industry-wide cost-drivers, including expenses and surpluses. It also establishes an outright ban on pharmaceutical gifts to physicians.
Transparency in these matters is crucial to the integrity of our health care system. Everyone must be held accountable. The gift ban, for example, seeks to pull physicians away from the marketing influences of the drug companies and re-emphasize the value of academic physician education and knowledge, while re-aligning spending needs and expectations on prescription drugs.
Another major cost hindrance to our health care system is the failure to implement information technology systems. The Senate legislation requires statewide adoption of electronic health records by the year 2015, supported by $25 million a year from the proposed cigarette tax increase.
It will also set a deadline of 2012 for statewide adoption of computerized physician order entry systems (CPOE), and require physician competency in health information technology for board registration. Updating these systems could save us billions of dollars while also reducing the occurrence of medical errors.
The Massachusetts Technology Collaborative (MTC) and the New England Healthcare Institute (NEHI) tell us that statewide adoption of CPOE alone could save us $170 million a year and prevent 55,000 adverse drug events annually that result in patient injury or death.
Standardized billing and coding is another area where technology can save money. The current system for documenting services and processing claims is antiquated. Our proposed legislation sets a statewide standard for uniform billing and coding among health care providers and insurance companies to reduce administrative costs, saving hundreds-of-millions of dollars.
Finally, the proposed legislation seeks to bridge the primary care access gap through a variety of measures, including a statewide workforce recruitment campaign; increasing enrollment slots at the our state medical school for students committed to providing primary care in the Commonwealth; and expanding the role of nurse practitioners as primary care providers.
Participation and collaboration will be the keys to our success. The first phase of health care reform was possible thanks to the broad coalition of citizens, businesses, providers, insurers and state government committed to increasing access. This next phase — cost control — will require a new and even greater commitment. This legislation is the beginning of that effort. The time to act is now.
-
Therese Murray is president of the Massachusetts Senate and a Democrat from Plymouth. Richard Moore is Senate chairman of the Health Care Financing Committee and a Democrat from Uxbridge.
-
----------
-

-
Mass Health Law
"Health insurance costs rise again; those with subsidies to pay more"
Posted by Karen Weintraub March 20, 2008, 3:38 PM
-
By Alice Dembner, Globe Staff
The state's new subsidized health insurance program will cost "signficantly" more than the $869 million proposed in the governor's FY2009 budget just two months ago, the state's top financial official said today.
The budget gap looms despite steps taken today to hold down state costs -- approval of a tough contract with insurers, and increased premiums and copayments for about half of the 176,000 people enrolled.
"We have closed some of the fiscal gap here, but we have not closed most of it," said Leslie Kirwan, state secretary of administration and finance. She declined to quantify the gap in funding for the Commonwealth Care program, which is at the heart of the state's healthcare reform initiative.
Kirwan said the governor is asking all the powerful players that have supported healthcare reform to contribute to a solution. In the last two weeks, during closed-door meetings, several dozen proposals have been put forward, including raising assessments on insurers, hospitals and businesses.
Healthcare advocates had vehemently opposed the increased premiums and copayments for enrollees, arguing that the insurance would become unaffordable for many and that it was unfair to ask low-income people to contribute more without also asking more of businesses, hospitals and insurers.
The administration muted their criticisms by lowering the increases slightly and by agreeing to seek similar "sacrifices" from other parties.
The premiums will go up 10 percent on average. For example, people with incomes between $21,000 and $26,000 who are now paying $70 per month, will pay $77. Only those with incomes over about $15,000 pay any premiums.
Copayments will rise $5 for a primary-care doctor's visit and between $2.50 to $5 for generic drugs. For enrollees at the highest income levels covered in the program -- those making between $26,000 and $31,000 a year -- copayments for use of the emergency room and for outpatient surgery will also rise. For the first time, there will be caps on out-of-pocket expenses, adjusted by income level.
----------
March 20, 2008
The Massachusetts State Government is going to raise rates in order to cover its fiscal gap in subsidized mandatory healthcare insurance under “Health Reform”. This situation is similar to the U.S. Government’s projected future fiscal insolvencies with Social Security & Medicare. They are all taking the taxpayer’s money for these social programs and using the money for other purposes. Last Fiscal Year, the Massachusetts State Government transferred $300 million from the Health Care Security Trust to its General Fund to make up part of its budget deficit. Moreover, they made the fiscally irresponsible decision to not make any interest payments and a $100 million contribution to this fund, resulting in $500 million toward the budget. That was mostly federal dollars for “Healthcare Reform” that went to the state’s operations, not its poor and working class uninsured residence. If the state divided ½-Billion Dollars among its 176,000 Commonwealth Care recipients instead of given themselves (the state government) the money then they would have solved the poverty issue right then and there one year ago next month.
In Dissent,
Jonathan A. Melle
--
ANNOTATED CITATIONS FROM TWO RESPECTIVE NEWS ARTICLES:
The state's new subsidized health insurance program will cost "significantly" more than the $869 million proposed in the governor's FY2009 budget just two months ago, the state's top financial official said today.
"We have closed some of the fiscal gap here, but we have not closed most of it," said Leslie Kirwan, state secretary of administration and finance.
Kirwan said the governor is asking all the powerful players that have supported healthcare reform to contribute to a solution. In the last two weeks, during closed-door meetings, several dozen proposals have been put forward, including raising assessments on insurers, hospitals and businesses.
Last Fiscal Year (FY2008), the Massachusetts State Legislature and Governor transferred $300 million from the Health Care Security Trust to the State’s General Fund to make up the difference on the then-disputed figure for the FY2008 state government budget deficit. Moreover, they made the fiscally irresponsible decision to not make any interest payments and a $100 million contribution to this fund, resulting in $500 million toward the budget.
--
Source: (“House lawmakers toss Patrick's plans”, By Hillary Chabot, Transcript Statehouse Bureau, The North Adams Transcript, Thursday, April 12, 2007)
BOSTON — House lawmakers snubbed many of Gov. Deval Patrick's initiatives while focusing on money for municipalities and additional higher education funding in their $26.7 budget, released Wednesday.
House members tossed out Patrick's plan to add 250 police officers, introduce a $24.8 million immunization program, add $25 million in emergency funds and to close corporate tax loopholes to rake in an additional $295 million. They relied more heavily on one-time funding instead.
"This year was a particularly difficult budget because of the shortfall," said Rep. Robert DeLeo, D-Winthrop, House budget author. "But we did not include any tax increases. We feel it's important to give the economy time to grow before we talk about any increases in taxes."
The renovated budget was nothing personal against the new governor, it just highlights different priorities, said Rep. Christopher N. Speranzo, D-Pittsfield, a House Ways and Means committee member.
Patrick's budget was released two months ago, and the budget penned by the Senate is due next month. Lawmakers are expected to hammer out a final version by July 1.
Patrick's much referenced $1.2 billion deficit had come under fire. The House budget maintains the state is only $800 million in the hole, saying the difference was due to estimates in spending and revenues. House leaders used $300 million from the stabilization fund and the Health Care Security Trust to make up the deficit. They also delayed making interest payments and a $100 million mandatory contribution to the funds, resulting in $500 million toward the budget.
Administration and Finance Director Leslie Kirwan called the heavy use of one-time funds and the level-funded line item for community police a real concern.
Rep. Daniel E. Bosley, D-North Adams, said the 250 additional officers would likely be put in urban areas and therefore would hurt suburban areas. Patrick had drained funding from the community police officers' account to pay for the new officers' salaries.
"We shouldn't suffer because of what's happening in urban areas," Bosley said.
Michael Widmer, executive director of the Massachusetts Taxpayers Foundation, backed the decision by House leaders to use the one-time revenues instead of hiking corporate taxes, saying that increasing jobs is the only way to improve the economy.
The budget boosted higher education by $16.1 million over Patrick's budget. Massachusetts College of Liberal Arts received $13.93 million, while Berkshire Community College got $9.16 million. The budget also included funding for an office devoted to bring wireless and broadband to all communities and $10 million for the Cultural Facilities Fund.
Education funding will increase by 6.4 percent, which exceeds Patrick's estimate by $20 million. North Adams will receive $367,449 more in this budget, but Pittsfield will get $532,843 less than anticipated in the governor's budget.
"I think you can see it's a difficult revenue year," Speranzo said, maintaining that the Chapter 70 funding was distributed appropriately. "We're meeting our responsibilities to cities and towns. This was something we had set in last year's budget."
Rep. William "Smitty" Pignatelli, D-Lenox, and other lawmakers will work for the next two days to include earmarks for their districts. Pignatelli is working on appropriations for the Berkshire Youth Initiative. Bosley said he hopes to work on funding for tourism and regional transportation.
Patrick cut $86 million in earmarks in his budget. The House budget spends less than Patrick on Extended Learning Time grants, extended day kindergarten and low-income child care. Tourism was cut by $15 million, which is about $2 million less than Patrick's budget, and regional transportation was cut by $500,000.
--
Source: (Mass Health Law: "Health insurance costs rise again; those with subsidies to pay more", Posted by Karen Weintraub March 20, 2008, 3:38 PM, By Alice Dembner, Globe Staff)
The state's new subsidized health insurance program will cost "significantly" more than the $869 million proposed in the governor's FY2009 budget just two months ago, the state's top financial official said today.
The budget gap looms despite steps taken today to hold down state costs -- approval of a tough contract with insurers, and increased premiums and copayments for about half of the 176,000 people enrolled.
"We have closed some of the fiscal gap here, but we have not closed most of it," said Leslie Kirwan, state secretary of administration and finance. She declined to quantify the gap in funding for the Commonwealth Care program, which is at the heart of the state's healthcare reform initiative.
Kirwan said the governor is asking all the powerful players that have supported healthcare reform to contribute to a solution. In the last two weeks, during closed-door meetings, several dozen proposals have been put forward, including raising assessments on insurers, hospitals and businesses.
Healthcare advocates had vehemently opposed the increased premiums and copayments for enrollees, arguing that the insurance would become unaffordable for many and that it was unfair to ask low-income people to contribute more without also asking more of businesses, hospitals and insurers.
The administration muted their criticisms by lowering the increases slightly and by agreeing to seek similar "sacrifices" from other parties.
The premiums will go up 10 percent on average. For example, people with incomes between $21,000 and $26,000 who are now paying $70 per month, will pay $77. Only those with incomes over about $15,000 pay any premiums.
Copayments will rise $5 for a primary-care doctor's visit and between $2.50 to $5 for generic drugs. For enrollees at the highest income levels covered in the program -- those making between $26,000 and $31,000 a year -- copayments for use of the emergency room and for outpatient surgery will also rise. For the first time, there will be caps on out-of-pocket expenses, adjusted by income level.
----------
-

-
Healthcare advocates attended a meeting yesterday in Boston of the panel that oversees the subsidized health insurance program. The panel voted to raise premiums for some enrollees. (David L. Ryan/Globe Staff)
-
"State health plan underfunded: Finance secretary seeks proposals on closing gap"
By Alice Dembner, Boston Globe Staff, March 21, 2008
The state's new subsidized health insurance program will cost "significantly" more than the $869 million Governor Deval Patrick proposed in his 2009 budget just two months ago, the state's top financial official said yesterday, after insurers were granted an increase of about 10 percent.
To close the gap, the Patrick administration has asked insurers, hospitals, healthcare advocates, and business leaders to propose ways to cut costs and raise revenue. During two closed-door meetings in the last two weeks, several dozen proposals have been put forward, including raising assessments on insurers, hospitals, and businesses. The goals are to solve the short-term funding problem for next year and ensure the long-term survival of the state's near-universal health insurance initiative.
Leslie Kirwan, secretary of administration and finance, declined yesterday to discuss specifics of the proposals or the size of the budget gap, but said that without changes, the state doesn't expect "to be able to live within" the proposed budget.
A state panel yesterday approved a contract to pay insurers about 10 percent more for each person enrolled in the subsidized insurance program, starting July 1. The insurers had asked for about a 15 percent increase, but agreed to take less after weeks of negotiations. Still, the state's cost is higher than was included in the governor's budget. Under the contract, the state also would assume more of the financial risk if the enrollees were to use more medical care than expected.
To partly offset the increased costs, the panel yesterday also voted to raise premiums by 10 percent for some of the 176,000 people enrolled in Commonwealth Care, and to increase copayments for many more. Starting July 1, the lowest premiums will range from $39 to $116 per month.
"We have closed some of the fiscal gap here, but we have not closed most of it," Kirwan said during the meeting at which the Commonwealth Health Insurance Connector approved the contract and premium increases.
Kirwan said the gap also is because of increased enrollment, now expected to exceed projections for both the current fiscal year and the next, which will begin July 1. Paradoxically, enrollment dropped slightly last month, because the state has begun disqualifying people who became ineligible because of changes in income or access to other insurance. But that is expected to be a temporary downturn. The budget figure of $869 million already was significantly higher than projected by legislative architects of the plan because of the enrollment boom.
Healthcare advocates vehemently had opposed increased premiums and copayments for enrollees, which were first proposed in February. They argued that the insurance would become unaffordable for many of the low-income people it was designed to serve and that it was unfair to ask enrollees to pay more without also asking more of businesses, hospitals, and insurers.
The administration muted its criticism by negotiating slightly smaller premium and copay increases, and by agreeing to seek similar but unspecified "sacrifices" from other parties.
"We're still disappointed that, at this point, the only ones making the sacrifices are enrollees and taxpayers," said the Rev. Hurmon Hamilton, president of the Greater Boston Interfaith Organization, a group of congregations that advocates for healthcare access. "But the administration is very committed to seeing all the stakeholders do their share. That's where the fight goes now."
Hamilton and other advocates pointed to private health insurers and some hospitals that they said are benefiting greatly from healthcare reform through additional members and insured patients. Some suggested that both insurers and hospitals should contribute more than the $160 million each they now pay annually to the state's free-care pool, which pays for hospital care for the uninsured. Money is being shifted from the pool to help pay for subsidies.
Advocates also said the state needs to get more money from businesses that are not providing insurance for their employees. A penalty on those businesses - of up to $295 per uninsured employee per year - has raised only about $6 million this year, far less than originally expected.
"Healthcare reform is not sustainable financially and it's also not sustainable politically if the best we can do is more taxpayer money and shifting costs to consumers," said Nancy Turnbull, an associate dean at the Harvard School of Public Health and member of the connector board. "We have to find other ways [to raise money and control costs] and we have to find them very quickly."
Kirwan declined to say that the state was targeting any particular sector for help. Most of the groups that helped the state pass healthcare reform two years ago are participating in the administration-led discussions about addressing the cost of Commonwealth Care. Yet, convincing them to cough up more money will not be easy.
Organizations representing insurers, businesses, and hospitals said yesterday they were already doing a lot. "The employer community is picking up its fair share," said Richard Lord, president of Associated Industries of Massachusetts and a member of the connector board. More than 85,000 employees were newly insured by employers last year, according to data released yesterday by the Massachusetts Association of Health Plans.
"This is successful because everyone has done something," said Tim Gens, senior vice president for policy at the Massachusetts Hospital Association. "We're willing to consider doing more," if everyone else is.
For members of Commonwealth Care, the premiums will go up 10 percent on average. For example, people with incomes between $21,000 and $26,000 who are now paying $70 per month, will pay $77. Only those with incomes more than about $15,000 pay any premiums.
Copayments will rise $5 for a primary-care doctor's visit, to $10 for some patients and $15 for others. Copayments for drugs also will rise. For enrollees at the highest income levels covered in the program - individuals making between $26,000 and $31,000 a year - copayments for use of the emergency room and for outpatient surgery also will rise. For the first time, there will be caps on out-of-pocket expenses for all medical care, excluding medicines, of $750 or $1,500, depending on the individual's income. They placed a separate cap on medication expenses.
The copayments and premiums originally proposed would have raised about $30 million in revenue, according to Celia Wcislo, assistant division director of labor union 1199 SEIU and a member of the connector board. She said the revised schedule shaves off nearly $10 million, which she called a substantial concession to the concerns raised by advocates.
Underlying the discussions yesterday was the issue of rising healthcare costs statewide. State Medicaid director Thomas Dehner, also a connector board member, said the healthcare reform law had accelerated the increase by providing care for more people and increasing the rates the state pays hospitals and doctors.
Board member Dolores Mitchell, who manages health insurance for state workers, said the state has to focus on "wringing the excess costs . . . out of the system. Everybody wants an omelet, but nobody wants to break some eggs."
-
Alice Dembner can be reached at dembner@globe.com.
-
----------
"Plugging health care leaks"
The Berkshire Eagle - Editorial
Monday, March 24, 2008
The increase in premiums and co-payments for the state's poorest residents approved last week by the Health Connector board came about because health insurers, and to a lesser extent state businesses, are hamstringing the state's health insurance reform programs in predictable ways. With insurers granted a payment increase of 10 percent, the state's subsidized health insurance program will cost substantially more than the $869 million budgeted by Governor Patrick, and those who can least afford to pay will be called upon to help make up the difference. The program is also struggling because far more businesses than anticipated decided that rather than provide insurance for their employees they would instead pay the penalty for not insuring their employees. The shortfall in revenue for the program is also causing the state to dip into the free-care pool used to reimburse hospitals for treating those who can't afford insurance. Countries with national health care programs must look on in amazement as the well-meaning custodians of the state's health reform effort scramble to plug ever-widening leaks.
----------
-

-
Jessica Kuznick of Arlington, whose husband has been laid off from work and who is seven months' pregnant with the couple's second child, wonders how proposed changes to Massachusetts' subsidized health insurance program will affect her family. (Essdras M Suarez/Globe Staff)
-
"Healthcare cost increases dominate Mass. budget debate: Controlling them said key to keeping universal coverage"
By Alice Dembner, (Boston) Globe Staff, March 26, 2008
When Massachusetts launched its landmark universal health insurance initiative nearly two years ago, the state put off addressing rising costs so it could expand coverage immediately. Now those costs are dominating the discussion as the state faces a recession and pivotal funding decisions that could make or break health reform.
A short-term funding problem - closing a budget gap of about $100 million by July 1 - may be solved quickly if the state approves an increase in the cigarette tax and devotes the money to healthcare reform, as is widely expected.
A larger issue will also come to a head by July 1: the need to secure a new three-year commitment from the federal government to pay for half the soaring cost of insurance subsidies. Massachusetts is seeking up to $1.5 billion, but the Bush administration has been cutting back federal payments to the states.
Even if the state garners enough money from those two sources, the plan's future rests on slowing the growth of healthcare costs in general, a task many analysts say is far more challenging than shaping the complex health reform law in the first place.
"If we don't grapple seriously with the cost of healthcare, the support for reform will erode and the perception will become broader that it is unaffordable," said Jon Kingsdale, executive director of the Commonwealth Health Insurance Connector, which oversees much of the reform effort.
The state's political leadership and the broad coalition of insurers, hospitals, businesses, and consumer advocates that worked to pass the first-in-the-nation initiative remains committed to ensuring its success.
So far, more than 342,000 people are newly covered since the initiative began, probably about half of the state's uninsured, although the exact number is unknown. Of the total, 176,000 are getting government-subsidized insurance - far more than expected by the second year, which is driving up the cost. Another 55,000 are newly enrolled in Medicaid.
"We have done a remarkable job signing up people for insurance," said Senate President Therese Murray, a Plymouth Democrat. "I don't think anyone wants to go backward on that."
"Everyone understands that the eyes of the nation remain on us," added Andrew Dreyfus, executive vice president at Blue Cross and Blue Shield of Massachusetts.
Yet the financial pressures provide new ammunition for those who have opposed the initiative from the start.
"We've said from the beginning that the basic problem with the reform is that if you don't restructure the system, it becomes rapidly unaffordable and the commitment to cover people begins to fade," said Dr. David Himmelstein, an associate professor at Harvard Medical School and a founder of Physicians for a National Health Program, which advocates for a government-run health system like Canada's. "We're seeing that begin to happen."
Among those who have supported the law, there is as yet no move to change the fundamental provisions of the plan: requiring nearly everyone to obtain insurance, providing free or subsidized coverage for those with low and moderate incomes, and changing the insurance market to make private coverage more affordable.
But the state's top budget official, Leslie Kirwan, last week suggested that the financial pinch might require increases in the contributions from coalition partners as well as "revisiting some of the original assumptions of healthcare reform." Through a spokesman this week, she declined to elaborate, saying only that "the administration remains fully committed to healthcare reform."
Murray also suggested the state should review the health law's provisions as part of a "look at everything." But House Speaker Salvatore F. DiMasi said he believed it was too soon to significantly modify the blueprint.
The Patrick administration has asked coalition members for suggestions on how to raise money and cut costs, and dozens of proposals have been submitted.
Advocates are pressing the administration to expand the number of companies subject to a penalty for not insuring their workers, a step the administration could take without legislative approval but which would probably draw strong opposition from businesses. The penalty raised only about $6 million this year, far less than originally expected. DiMasi said he thinks the administration should consider this option.
DiMasi has also proposed another alternative - a $1-per-pack increase in the cigarette tax earmarked for healthcare reform - that could raise $152 million a year. Murray supports the increase.
Kirwan said the state expects to spend substantially more for insurance subsidies than the $869 million Governor Deval Patrick proposed in his 2009 budget just two months ago, because of increasing enrollment and higher payments to insurers. In private briefings, she has told coalition members that the cost could be $100 million more, according to several who were present. The administration declined to confirm that number.
The gap is part of an estimated $1.3 billion shortfall in the $28 billion state budget. A recession could also bring layoffs at private companies that increase the ranks of the uninsured.
The subsidized program, called Commonwealth Care, accounts this year for about one-third of the $1.9 billion price tag for healthcare reform. About half of that total is picked up by the federal government.
Over the next three years, the Patrick administration has projected, Commonwealth Care will double in size and cost. Some analysts suggest that the cost projections, produced last fall, may have been inflated in an attempt to get more funding.
Spending on other components of healthcare reform are expected to decline over the next few years, but probably not enough to pay all the bills.
Meanwhile, healthcare costs statewide are rising by about 10 percent a year. A council established by the health reform law has developed some proposals to reduce cost growth, and several bills are pending in the Legislature. But the task is daunting.
"Expanding coverage is easy compared to controlling healthcare costs," said Nancy Turnbull, a Commonwealth Health Insurance Connector board member and associate dean at the Harvard School of Public Health. "Nobody has to give much up to expand coverage, but in controlling cost there will always be losers."
-
Alice Dembner can be reached at dembner@globe.com.
-
----------
(A Boston) GLOBE EDITORIAL
"Managing care the right way"
March 26, 2008
MANAGED CARE got a bad reputation in the 1990s. At its best, though, this method of organizing healthcare saves money while enhancing the quality of patients' lives. In Massachusetts, the Commonwealth Care Alliance, which bills itself as a nonprofit care delivery system, is succeeding in its five-year-old experiment on whether treatment can be coordinated and improved for people with complicated medical histories.
"I wouldn't be here. I'd be stuck in a nursing home or a chronic care hospital," said Paul Kahn, 62, of Newton, as he praised the care that enables him to lead an active life at home despite being crippled by a neuromuscular disorder since childhood. For the last few years he has been dependent on a ventilator to breathe. Yet because of a coordinated care system akin to what the alliance offers, he has been living independently since 1979, has married, and has written 20 plays. He has rarely spent time in the hospital.
Kahn has been the beneficiary of coordinated care systems established by Dr. Bob Master. Years ago Master realized that the best way to treat chronically ill patients is to provide them with nursing and social-work services where they live, and only send them off for complicated medical procedures when strictly necessary.
Master cofounded Boston's Community Medical Group in 1988 to provide this kind of care, using a team of physicians, nurse practitioners, social workers and physical therapists. Kahn is a patient.
Payments to treat the chronically ill, many of them very poor, come from a variety of sources, not all of them geared to Master's early-intervention approach. The Commonwealth Care Alliance (no relation to the state's Commonwealth Care insurance plan) is intended to make payment as seamless as treatment. Master helped set up the alliance as part of an effort called Senior Care Options, which combines Medicaid and Medicare funds in a single payment stream.
The alliance is one of three health plans in the state involved in Senior Care Options, and it has the most integrated model of care. The alliance generated a $1.3 million surplus in 2005-2006 and would like to use the money to expand the program. This would be a worthwhile investment to serve more patients beyond the current 2,500.
The alliance has generated interest at the Harvard Business School, where Professor Michael Porter had a case study written about its work. "It offers a model for high-quality, high-value care delivery," said Jennifer Baron, the coauthor. Paul Kahn knows that it's helped keep him on the go despite the difficulties of his life.
----------
The Boston Globe, Op-Ed
CHRISTOPHER R. ANDERSON
"Righting healthcare reform"
By Christopher R. Anderson, March 31, 2008
IN A NOVEMBER 2005 letter to the Legislature, more than 20 state business associations declared support for measures that would deliver healthcare cost controls to the state's ambitious reform efforts. After lauding measures like investing in electronic health initiatives and creating cost transparency at hospitals, the business leaders wrote, "Cost, after all, is the single biggest problem we face today in the delivery of health care."
Unfortunately, that statement remains true today. Despite national attention for the 2006 reform plan, healthcare in Massachusetts has reached a crisis point. More residents now have health coverage, but the crushing costs of the program endanger its long-term viability. This crisis has been brought about by the failure to address costs while focusing almost exclusively on access. For companies that have experienced years of double-digit increases for employee health premiums, the exploding cost of the healthcare law is not surprising.
During the debate, businesses successfully pushed for modest cost reforms. But even those appear to be stalling. Last week, the state's most prominent champion of healthcare transparency, Harvard Pilgrim CEO Charles Baker, expressed frustration at the pace of making healthcare data available on the state's website, which was a mandate of the 2006 law.
With its massive cost overruns and missed deadlines, the healthcare reform law is quickly becoming the Big Dig of the next generation, an ambitious and beneficial but deeply flawed public initiative with back-breaking costs to the taxpayers. Unlike the Big Dig, Massachusetts taxpayers, not Congress, will pay most of the healthcare tab.
Senate President Therese Murray deserves significant credit for proposing the first plan to address the serious challenge of controlling health costs without any new broad-based taxes. In particular, the increased investment in electronic medical records will benefit hospital efficiency and patient safety, while at the same time providing economic opportunities for Massachusetts technology employers. Murray also smartly proposed boosting enrollment at the University of Massachusetts Medical School, which already has one of the nation's top primary-care programs. In addition, proposals to encourage doctors to enter primary care and practice in underserved regions of the state have significant merit.
However, the recommendation to ban many forms of interaction with doctors keeps the pharmaceutical companies from effectively educating doctors on life-altering drugs. This counters the stated goal of controlling costs, as evidenced by the lack of specific cost savings projections publicly attributed to this education ban. It is more of a political proposal than a fiscal one.
Marketing bans or restrictions are redundant because of federal law and could impact drug safety if critical information does not reach doctors or patients. Only a small percentage of drug compounds ever reach the consumer, and the state should not impose duplicative red tape that will hinder access to breakthrough treatments. For these reasons, the New Hampshire House of Representatives recently rejected a similar marketing restriction bill.
It would be shortsighted for the Commonwealth to commit $1 billion for the state's life sciences industry while simultaneously undercutting biopharmaceutical employers that are expected to create jobs here. Last year, a High Tech Council study conducted by the University of Massachusetts discovered that from 2000 to 2006 13 of the leading pharmaceutical firms invested more than $13.4 billion in state biotech companies - far outpacing venture capital biotech investment. The study revealed that this investment typically occurs during the early stages of drug development when many drugs fail due to lack of funding. If the state deliberately works against the biopharmaceutical sector, it is hurting the entire life sciences community, and ultimately patient care.
A much better idea would be to reform the state's medical malpractice laws. Creating a system that minimizes frivolous lawsuits and provides protections to doctors would greatly stabilize skyrocketing malpractice premiums, which are driving many good doctors out of state. A 2002 federal study showed that reforming the nation's medical malpractice system would save up to $108 billion in annual healthcare costs. As Baker said, Murray is "doing us a big favor by throwing the gauntlet down" on cost reform. Now all stakeholders in the debate must work together to make sure it is done right.
-
Christopher R. Anderson is president of the Massachusetts High Technology Council.
-
----------
The Boston Globe, "THE OBSERVER"
"Lost in the labyrinth: It's time for the doc to order a dose of healthcare reality"
By Sam Allis, Boston Globe Columnist, March 30, 2008
The mere thought of exploring the labyrinth called Chapter 58 gives me a case of the vapors.
The statute, which mandates health insurance for everyone previously uncovered, went into effect last year in a forest of fine print that has left people wall-eyed.
Most of us, and plenty of Beacon Hill types who passed it, are clueless today about Chapter 58. Which reminds me of the line from the great screenwriter William Goldman about Hollywood: "Nobody knows anything."
The Observer skirted the Chapter 58 policy morass last week and wandered instead to the Codman Square Health Center in Dorchester for a hit of reality. It is in community centers like Codman, along with hospitals, that we first see the new system bite.
I ask Bill Walczak, founder and CEO of Codman, what changes he is seeing after Chapter 58's first year in operation.
"An exponential increase in bad debt so far this fiscal year. It's up from $700,000 to at least $1.3 million," he says, based on projections from the first four months. "We're also losing between $800,000 and $1 million in cash."
So what's the prognosis?
"Our mission is to see people regardless of means," he says. "We can survive a year or two of this kind of craziness, but a couple of years down the line, the safety net will no longer be protected, and we'll have to start dismantling the operations that serve our people. This new system should not hurt the safety net."
"So far, we've been able to insulate the quality of care from the financial damage," he adds, "but that can't go on forever. There are winners and losers in this equation and we're losers."
Walczak says half of his patients were uninsured three years ago, but they were covered by the Massachusetts Uncompensated Care Pool, the old system that handled such people.
The good news is that far fewer patients are still in the pool, now under a different name. More have some kind of insurance today. The bad news is that the safety net is shredding, and 10 percent of his patients have, in Walczak's words, "fallen off a cliff."
Also, the first 50,000 of the uninsured put into the new program last year are completing year one. Over half of them have not signed up again as they're required to do. Many, Walczak notes, never signed up in the first place and have no idea what to do now.
"Health centers like Codman Square and the Dorchester House serve the working poor - people who have bad jobs, low wages, and no health insurance," he says. "The really poor have Medicaid. Medicaid was enlarged last year. This is good. The problem with the new model is that far more people than anticipated don't have insurance."
Chapter 58, he notes, was based on the assumption there were between 300,000 and 400,000 uninsured people in the state. The real figure is somewhere between 600,000 and 700,000, he says, and a lot of people working on the program knew that.
Walczak ran the numbers on a hypothetical 58-year-old woman who earns $32,000 a year. Under Commonwealth Choice, her cheapest option costs her $4,400 a year in premiums. There will also be a co-pay every time she sees a doctor, but she first must exhaust a $2,000 deductible to get anything back at all. If hospitalized, she'll face a 20 percent coinsurance payment.
"This is an entitlement to bankruptcy if someone actually needs healthcare," he continues. "The number one cause of bankruptcy in this country is medical costs."
Everyone in the state must have annual proof of membership in some health insurance program to avoid fines. Without proof, the state will come after you. The fine for not enrolling in a Chapter 58 program can run as high as $912 a year.
Say I'm earning $31,212 - 300 percent of poverty and, like the hypothetical woman, am forced into Commonwealth Choice. But I don't sign up for it because my company has dropped overtime pay, my wife's salary has been cut in half, and my balloon mortgage just ballooned.
So what's going to happen to a criminal like me, or the 26-year-old criminal struggling in a start-up, or the criminal restaurant cook?
Will we be dragged off in the middle of the night by storm troopers and thrown in the clink? Will the state garnish our wages and hasten our descent into bankruptcy?
I figure the young fry will head for Pawtucket because Rhode Island has no mandatory health insurance program, but I have no idea what will happen to families who can't pay and don't want to move. I just don't see where this thing goes.
Walczak says there's plenty to like in Chapter 58: More than 300,000 people now have some kind of insurance who didn't. Medicaid has expanded its rolls by 70,000. There is new Medicaid coverage for eye care and dental coverage for adults. But big problems are emerging.
We now know the estimates of the uninsured, along with the notion that the new system would teem with young, healthy people who wouldn't cost much, were absurd. There is a major cohort of older people as well who need serious medical treatment at significant expense. Who planned this thing?
Don't blame the elderly here. It's not their fault that we've always provided a safety net, however frayed, for them. Just pray that Chapter 58 doesn't take it away.
-
Sam Allis can be reached at allis@globe.com
-
----------
(A Boston) GLOBE EDITORIAL
"Who said it would be easy?"
April 8, 2008
IT MIGHT have made more sense economically if a lower-cost state - say, Utah or Minnesota - had initiated the health insurance expansion that became law in Massachusetts two years ago this week. But the political and economic leadership here had the will and the resources to try what no state, except Hawaii, had ever come close to achieving: health coverage for just about everyone. While the success of this initiative is not assured, Massachusetts should be proud of accomplishing so much, so quickly.
As of Jan. 1, 342,000 people had enrolled in insurance plans fostered by the new law, an impressive achievement. Two-thirds of that number are in Commonwealth Care, which provides subsidized coverage to those just above the poverty line.
According to the Kaiser Family Foundation, healthcare costs much more in Massachusetts than elsewhere: $6,683 per person in 2004, compared with Utah's $3,972, and Minnesota's more typical $5,795. Yet in the short term, this cost disparity meant Massachusetts had more money in the system to expand coverage - notably from a Medicaid waiver by the federal government, which comes up for renewal on July 1.
Support for the Massachusetts initiative has been a major achievement of the US Department of Health and Human Services. Secretary Michael Leavitt, who has the final say, ought to approve an extension.
Even with a renewal, unforeseen costs will become a burden. More people have signed up for Commonwealth Care than anticipated and rates are going up 9.4 percent July 1. Governor Patrick budgeted $869 million for the initiative in the fiscal year that begins July 1, but his administration now believes that figure is low by $100 million.
If only this were Utah, where the healthy Mormon lifestyle keeps costs down, or Minnesota, which is not so dominated by expensive teaching hospitals and specialists. But Massachusetts has one great advantage over other states - the coalition of groups that put the healthcare package together two years ago. This includes businesses, health insurers, hospitals, unions, healthcare advocates, and political leaders. They now need to figure out ways to control costs, maintain quality, and get new money into the system when absolutely necessary.
A generation ago, Hawaii was praised for requiring employers to provide health insurance to all workers. Companies found loopholes, however, and as of 2006, its uninsurance rate was 10 percent, a little less than Massachusetts's 11 percent.
The Massachusetts initiative will fray more quickly unless the coalition reenergizes itself.
----------
Massachusetts
"Two years later, health care law hailed"
By Cara Hogan, Eagle Boston Bureau
Friday, April 11, 2008
BOSTON — North Adams resident Jennifer Cohen didn't have dental insurance, but needed her wisdom teeth taken out. After years of worry, she applied for state subsidized insurance from Commonwealth Care.
"I was able to get my wisdom teeth out," Cohen said. "I could have had a lot of complications if I didn't get it done. It saved me."
But even as Gov. Deval L. Patrick and the Legislature celebrated the second anniversary of Massachusetts' universal health insurance law that allowed Cohen to get care, the widely hailed program is threatened by rising health care costs and the falling economy.
In the past two years, 340,000 residents have been added to the ranks of the insured; 176,000 of those have joined Commonwealth Care, the state-subsidized insurance plan for low-income residents. Patrick said the program has exceeded expectations and shows that Massachusetts is making real changes in health care.
"What we've done here is not necessarily the formula for the rest of the country, but at least we are trying," Patrick said at a news conference celebrating the anniversary.
The state predicts there will be 50,000 more applicants for subsidized insurance in the next year, which could place a strain on public funds. The governor's budget allots $869 million for subsidized health insurance, but some legislators predict expenses could rise to as much as $1 billion.
"Making this initiative work is even more important as we face a slowing national economy," Patrick said. "Nothing comes easy. We have to join together to reign in costs."
Rep. Denis E. Guyer, D-Dalton, said though the situation seems tough, there are possible solutions to continue expanding health care.
"The most effective way to control health care costs is getting as many people coverage as we can," he said. "So we're treating high blood pressure in the doctor's office instead of advanced heart disease in the emergency room. Emergency room care is far more expensive than preventative care."
Although Guyer acknowledged concern that greater participation would cost more, he said he believes the state will eventually reap benefits from the program.
"I'm very optimistic that we're providing a model for health care for other states to follow," he said. "It will help us contain the costs of health care in Massachusetts and help attract businesses to move to the state, since we will have lower health care costs."
Senate President Therese Murray has proposed various cost-saving programs such as switching from paper medical records to electronic and strengthening preventive care.
Rep. Patricia Walrath, D-Stow, the chair of the Joint Committee on Health Care Finance, supports Murray's bill and is focused on the need for more primary care physicians to produce lower costs.
"There is a shortage of primary care physicians, and we're looking to subsidize the education of physicians that stay in Massachusetts after graduation," Walrath said.
But Senate Minority Leader Richard R. Tisei, R-Wakefield, is less optimistic. He released a statement saying the Massachusetts experiment has produced "mixed results."
--
Reader's Comment:
"leffhill", April 11, 2008 -
From the standpoint of a self-employed individual who does not qualify for state assistance and now must pony up an additional $850 PER MONTH (for something I don't consider necessary), it's real hard for me to see what's so great about this law - which, let's be honest, is not about 'providing care for the people', but is all about making sure that the medical industry and the state are fully compensated.
--
Reader's Comment:
"GMHeller" - April 11, 2008
Read between the lines, what Rep. Denis Guyer is saying is that the new health care law is an unmitigated disaster!
"Although Guyer acknowledged concern that greater participation would cost more, he said he believes the state will EVENTUALLY reap benefits from the program.
'I'm very optimistic that we're providing a model for health care FOR OTHER STATES to follow,' he said.'It will help us contain the costs of health care in Massachusetts and help ATTRACT businesses to move to the state, since we will have lower health care costs.'"
So what Guyer is actually saying here is that if other states, especially surrounding states, don't pass similar health care regulations soon -- or as doctors like to say, "STAT!" -- then patient Massachusetts is going to go terminal -- as in DEAD -- because businesses will have no alternative to stay competitive but to move out!
I'm beginning to think maybe some of Mass. expatriate Jonathan Melle's dismal assessments of Mr. Guyer may actually be correct!
SEE: www.guyerwatch.blogspot.com
GMHeller
Monterey,MA
www.berkshireeagle.blogspot.com
--
Reader's Comment:
"pat the painter" - April 11, 2008
I wonder if our elected officials had to pay for healthcare out of their own pockets would they hail such a 'mandatory law'?
Amazing how our elected 'Public Servants' can spend other people's hard earned money, when they live well and on the taxpayers money. They flourish while the middle class suffers yet again.
--
Reader's Comment:
"Jake" - April 11, 2008
Wouldn't it be nice if we got the same healthcare as our leaders? We get smacked all the time. New tax package passed should really help people move out faster than they planned.
--
----------
"Healthcare affordability figures updated: Governor hails insurance plan"
By Alice Dembner, (Boston) Globe Staff, April 11, 2008
A state board yesterday updated standards that will be used to decide who faces fines this year for failing to have health insurance.
The vote occurred on the same day officials and community members gathered to celebrate the second anniversary of the healthcare law that has resulted in more than 340,000 people getting insurance so far.
"This is a wonderful, wonderful experiment, and it is showing great results," Governor Deval Patrick said at a State House ceremony. "But nothing this ambitious or important comes easy."
To sustain the initiative, Patrick said, the state must reduce expenses.
"Our first priority," he said, "is to rein in costs."
The state faces a rapidly rising bill to cover insurance subsidies and is searching for ways to reduce expenses and raise revenues.
The first person to receive insurance through the subsidized program, Madelyn Rhenisch of Brighton, told those at the ceremony that the bill is well worth it, because it has given her and others security and hope.
Meanwhile, officials are stepping up advertising to encourage the hundreds of thousands of people who are still uninsured to obtain coverage. Those who don't will face a penalty of up to $912 if they are uninsured for the entire year and if the state deems insurance affordable for them.
The Commonwealth Health Insurance Connector yesterday approved new affordability rules that increase the monthly premium considered affordable about 10 percent from 2007 levels. Insurance premiums have been increasing at about that rate statewide, although the connector was able to negotiate an average increase of about 5 percent for the nonsubsidized plans it offers the public.
The rules set out a sliding scale, based on income and family size, that indicates whether the state considers premiums affordable. For example, an individual earning more than $52,500 would be considered able to afford insurance regardless of the premium. But someone earning between $37,501 and $42,500 would be required to purchase insurance only if the premium was $220 or less.
The standards become final after a public hearing and a second vote by the connector.
Consumer advocates said yesterday that they believe the standard requires older people with moderate incomes to spend too much. "We are still concerned that the standard is not genuinely affordable," said John McDonough, executive director of Health Care for All.
----------
The Springfield "REPUBLICAN" Newspaper Online - Editorial, Friday, April 18, 2008
"Universal coverage coming unglued"
It was going to be a new "Massachusetts miracle." But then reality brought everyone back to earth.
The Bay State's plan to provide universal health insurance to the citizens was a new model. Rather than relying solely on the government, the plan was an effort to share the burden. The state, businesses and individual citizens would all do their part.
And everyone would live happily ever after. Or at least be a whole lot better off.
But that's the thing about fairy tales: They are fantastic and otherworldly and only of one's imaginings.
The new Massachusetts miracle may have looked good on paper, but it didn't come to life in the here and now.
While we supported the notion and applauded the effort, we had serious reservations about the plan from the first. The cost estimates never seemed to add up, and there was good reason to believe that like so many government programs before it, the Bay State's health initiative would end up costing vast amounts of taxpayer money. Guess what? The program isn't even a year old, and costs are out of control.
Gov. Deval L. Patrick is looking for an additional $153 million just to make it to the end of the fiscal year on June 30. And that's on top of the $472 million that the state had appropriated for the program for the current fiscal year.
The picture doesn't get any rosier in fiscal 2009. Officials are budgeting $869 million, but say even that much won't be enough.
It won't be very long before we're talking about a billion dollars - and more - for a program that was being touted as a model for other states, and perhaps for the entire nation. Instead of a model, the Massachusetts system should serve as a warning: If you're having thoughts about universal health coverage, you'd better think again.
We are in no way happy to see this program falling to pieces, but we are most decidedly not surprised.
Our real worry now is that it will continue to bleed the state budget. It may well take a miracle just to keep that from happening.
----------
The NY Times Online - National Briefing, Northeast, April 17, 2008
"Universal Health Care to Cost Massachusetts More Than Was Budgeted"
By KEVIN SACK
In its first full year, universal health coverage in Massachusetts will cost the state $153.1 million more than was budgeted, according to a supplemental budget request released Monday by Gov. Deval Patrick. The state had appropriated $472 million for the fiscal year ending June 30, but enrollment in the state’s subsidized insurance programs for low- and middle-income workers exceeded expectations. About 340,000 of the state’s estimated 600,000 uninsured have gained coverage since Massachusetts began requiring health insurance. The state had projected that 136,000 people would sign up for its Commonwealth Care policies, but 174,000 are now enrolled. Cyndi Roy, a spokeswoman for Mr. Patrick, a Democrat, said this year’s shortfall would be offset by surplus revenues in the state’s general fund. For the coming fiscal year, Mr. Patrick has requested $869 million for Commonwealth Care, but his aides have already conceded that will not be enough as enrollment continues to grow.
-
http://topics.nytimes.com/top/news/national/usstatesterritoriesandpossessions/massachusetts/index.html?inline=nyt-geo
-
----------
THE BOSTON GLOBE, Op-Ed
BARBARA DAWIDJAN AND KATHERINE M. PELULLO
"Filling a gap in Bay State dental care"
By Barbara Dawidjan and Katherine M. Pelullo, April 21, 2008
IMAGINE walking into a dentist's office with a severe toothache and being told by the dentist that there is good news and bad news. The good news is that because you are poor, you qualify for free dental care from the state in the state's Medicaid program, MassHealth. The bad news is that your dentist won't be able to treat your toothache because he or she only takes patients who have private insurance or who can pay out-of-pocket.
Unfortunately, this is not the exception but the norm in the delivery of oral healthcare in Massachusetts. Of the 351 cities and towns in Massachusetts, 69 do not have a single dentist. Of the communities with dentists, 30 percent don't have enough to care for all the people who live there.
And the most disturbing statistic of all: Of the state's more than 5,000 active licensed dentists, more than 80 percent refuse to see even one MassHealth patient, including the more than 460,000 MassHealth-eligible children. A bill now on Beacon Hill would allow dental hygienists to help fill this gap.
Without access to oral healthcare services for all residents, disparities in oral health will continue to plague our state. A 2004 state report found that nearly 50 percent of third-graders had a history of dental disease, and 26 percent live with untreated cavities. Research has linked oral health problems to heart disease, diabetes, and other diseases.
However, unlike these other diseases, dental disease is preventable through the use of fluorides, dental sealants, and access to professional care.
Because current law in Massachusetts prevents a dental hygienist from delivering services except under the supervision of a dentist, low income patients typically have no access to either a dentist or a dental hygienist.
Pending legislation would modernize state law to allow dental hygienists to practice in public health settings without the direct supervision of a dentist. This is not some new-fangled Massachusetts idea. Twenty-two other states have passed similar laws, including Rhode Island, Maine, New Hampshire, and Connecticut. In these states, dental hygienists may go directly to patients in public schools, Head Start programs, and nursing homes to perform the same preventive oral health treatment they do in a dentist's office.
Unfortunately, the Massachusetts Dental Society seeks to block this legislation from becoming law.
Even though the bill requires a dental hygienist to establish a collaborative agreement with a dentist and refer patients to dentists for the kind of care that only a dentist can provide, and specifically bars hygienists from independent practice, the dental society remains vehemently opposed.
At a time when dentists are turning away thousands of Bay State residents who need their services, they choose to spend thousands of dollars on ads meant to scare the public into thinking that dental hygienists are somehow unqualified to treat patients "outside of the traditional practice."
This rhetoric fails to note that under current state law, "supervision" of a dental hygienist does not require the dentist to be physically present in the same location where the dental hygienist provides care. Hygienists are more than qualified to see patients in a dentist's office (and allow the dentist to make a healthy profit from that service) when the dentist is at a continuing education conference or on vacation, out of state or even out of the country.
But when hygienists seek to provide the same care to kids in schools or to seniors in nursing homes, all of whom are now often denied services from the dentist for whom they work, the hygienist is suddenly labeled "unqualified."
The bill has gained the endorsement of the two prominent health-related committees in the Legislature. Also, the state Department of Public Health supports its intent. In a recent report the department endorsed the use of registered dental hygienists to help close the gap in access to oral health care.
It is one thing for dentists to refuse to see poor kids and seniors, but it is quite another for them to stand in the way of other perfectly qualified health professionals who are trying to help.
-
Barbara Dawidjan is president of the Massachusetts Dental Hygienists' Association. Katherine M. Pelullo is chairwoman of the association's Council on Regulation and Practice.
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/04/21/filling_a_gap_in_bay_state_dental_care/
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/04/21/filling_a_gap_in_bay_state_dental_care/?page=full
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/04/21/filling_a_gap_in_bay_state_dental_care?mode=PF
-
----------
The Boston Herald, OPINION, Op-Ed/Letters, Saturday, May 3, 2008, Page 16
"A healthy trend for Massachusetts"
"As You Were Saying..." By John Kingsdale
As we mark Cover the Uninsured Week 2008 across the country, it is appropriate to reflect on what health care reform has accomplished in Massachusetts.
More than 340,000 previously uninsured Massachusetts residents now have coverage. Over one-third of them have purchased insurance on their own without any government subsidies. That is remarkable.
One reason for our success is our aggressive public education & outreach campaign. A complicating factor is the varying estimates of how many uninsured Bay Staters there were in 2006. State & federal government surveys estimated a range from just under 400,000 to more than 650,000. It would seem that the real number was closer to the higher end. At the low end, we would appear to have enrolled most of the uninsured, but at the high end about half of them.
In any scenario, health insurance is a valued commodity. A poll released this week by the Kaiser Family Foundation noted that Americans were more worried about paying for their health care than they were about paying their rent or mortgage or buying food.
Those concerns are well-founded. A Families USA study earlier this year reported that more than 2,000 Massachusetts adults under the age of 64 died between 2000 & 2006 because they did not have health insurance.
Here are a few more eye-opening revelations from that study:
* "Across the U.S., twice as many people died from a lack of health insurance than from homicide."
* "Uninsured adults are more that three times as likely to be diagnosed with a disease in an advanced stage as insured adults."
* "Uninsured patients are often charged 2.5 times what insured patients are charged for hospital services because they are unable to negotiate the discounts on hospital & doctor charges like insurance companies do."
What Massachusetts has accomplished is not just about numbers. It is about people. One woman was showing up in the emergency room for 2 years complaining about a soar throat. We all know how chaotic an ER can be, so it was not surprising that her prescribed treatment consisted of throat lozenges.
When she enrolled in our Commonwealth Care program, her physician diagnosed her symptoms as throat cancer. She has stopped smoking, received treatment and is recovering.
Of course, this brings us back to numbers. More specifically, to dollars. It always does. It is understating the problem to say that health care is not cheap. It is terribly expensive. And while our cost per member is actually less than what we projected, higher enrollment means the program will cost more.
Fortunately, our landmark law has served as an impetus to seriously consider controlling costs. That is not merely a good sign, but is a critical step if health care reform is going to be sustainable in the long run.
About 2 million Americans lose their health insurance every year. This is unacceptable. Massachusetts is one state headed in the right direction. Yes, there is a cost factor, but the cost in human life is even greater if we don't stay the course.
-
John Kingsdale is executive director of the the Commonwealth Health Insurance Connector Authority. We invite readers to contribute 600-word pieces. Email to oped@bostonherald.com. Submissions become Herald property.
-
----------
"COMMONWEALTH CARE WOULD COST 1.1 BILLION NEXT YEAR"
Posted by CommonHealth, Tuesday, May 6th, 2008
THE NUMBER OF MASSACHUSETTS RESIDENTS WHO WOULD QUALIFY FOR SUBSIDIZED HEALTH INSURANCE…AND THE COST OF THAT COVERAGE IS RISING…AGAIN. ESTIMATES FOR THE NUMBER OF RESIDENTS WHO WOULD QUALIFY FOR COMMONWEALTH CARE HAVE RISEN FROM 140-THOUSAND TWO YEARS AGO TO 225-THOUSAND EARLIER THIS YEAR TO NOW…255-THOUSAND. THAT REVISION(PG.28) WOULD INCREASE THE COST OF SUBSIDIZED COVERAGE FROM 869-MILLION TO ONE-POINT-ONE BILLION DOLLARS NEXT YEAR. RICK LORD REPRESENTS BUSINESS INTERESTS ON THE CONNECTOR BOARD.
I’m hoping that state estimate is on the high side because if it’s not, that obviously presents a challenging budget situation in what is already a challenging budget year.
LORD SAYS ENROLLMENT HAS BEEN LEVELING OFF IN RECENT MONTHS AS COMMONWEALTH CARE MEMBERS HAVE BEEN ASKED TO PROVE THEY ARE STILL ELLIGIBLE FOR THE PROGRAM. MOST STATE HOUSE LEADERS SAY IT IS TOO EARLY TO DISCUSS LIMITING COMMONWEALTH CARE ENROLLMENT.
THIS LATEST FINANCIAL FILING ALSO INCLUDES A HIGHER ESTIMATE FOR THE COST OF COMMONWEALTH CARE THROUGH THE END OF JUNE. THE SUPPLEMENTAL BUDGET THE ADMINISTRATION FILED LAST MONTH ASKS FOR AN ADDITIONAL 153-MILLION DOLLARS, BUT HERE THE ADMINISTRATION PROJECTS IT WILL NEED AN ADDITIONAL $175 MILLION…BRINGING THE TOTAL COST FOR FY’08 TO 647-MILLION DOLLARS.
Update (after a conversation with Administration and Finance Secretary Leslie Kirwan):
Secretary Kirwan says the administration does not plan to revise the budget for next year until/unless the new enrollment numbers pan out. She stresses that there is a lot of uncertainty in both the coverage estimates and the budget. The higher numbers for Commonwealth Care and for Medicaid are based on current trends and do not factor in possible job cuts during a recession. Several Connector board members say that the next fiscal year will be particularly difficult because the cost of covering the uninsured is rising and savings from expanded coverage have not yet caught up.
----------
"Senate releases $28B state budget"
By Steve LeBlanc, Associated Press (The North Adams Transcript Online)
Thursday, May 15, 2008
BOSTON -- As Senate leaders unveiled a $28 billion budget Wednesday that relies heavily on new taxes and money from the state's "rainy day" fund, Republicans pledged to file Gov. Deval Patrick's casino bill as an amendment to the spending plan, saying the state needs new revenues.
The move, which could breathe new life into Patrick's plan, comes a week after the governor told a Brookline Chamber of Commerce audience that his legislation to legalize casino gambling in Massachusetts "may yet come back."
The House earlier this year overwhelmingly defeated the casino measure, essentially killing it for the year, but Republicans say they want to give the Senate, which has supported expanded gaming in the past, a chance to vote on the plan.
"We want to fortify the governor's efforts going forward if he intends to refile the bill in the new year," said Republican Sen. Michael Knapik, R-Westfield. "Plus, we need the money."
It's unclear what kind of reception the casino amendment would get during the Senate budget debate, scheduled for next week. Democratic Senate leaders have indicated support for Patrick's plan in the past, but not as a budget amendment.
Patrick gave no indication he would support the Republican amendment.
"It's clear from the House's vote earlier this year that there appears to be little chance of final passage for casino legislation this session," said Patrick spokeswoman Rebecca Deusser. "The governor's focus for the remainder of the session will be on his economic stimulus plan including passage of the life sciences and clean energy initiatives."
Even if the Senate adopts the amendment, it would face opposition from House lawmakers as both chambers hammer out a compromise budget.
Like the House budget, the Senate spending plan relies on hundreds of millions of dollars in new revenues from a proposed $1-a-pack cigarette tax hike and the closing of so-called business tax loopholes. It also raids the state's rainy day fund for nearly $400 million.
Senate Ways and Means Chairman Steven Panagiotakos, D-Lowell, said the budget plan was fiscally responsible.
"These recommendations are a balanced, fair approach to addressing the most pressing needs of the commonwealth while remaining mindful of the declining economy," Panagiotakos said.
Besides the $400 million from the state's rainy day fund, the budget also relies on $175 million in projected revenues from the cigarette tax, $297 in added revenues from the business loophole closings and another $157 million from tighter enforcement by the Department of Revenue.
He also said the budget includes "tens of millions" in cuts.
The Senate plan also includes $5 million for a universal pre-kindergarten program, $5 million for a new program to keep those addicted to opiates out of jail, and $25 million to help create a statewide electronic medical records system.
One of the biggest question marks in the budget is funding for the state's 2006 landmark health care law. Senate budget writers used an estimate of $869 million to cover the law's subsidized health care program known as Com-monwealth Care.
But the administration's own, more current estimates -- based on the unexpected success of the program -- have added about $200 million to the cost. That's in addition to the $200 million above original estimates for Mass Health, the state's Medicaid program.
Critics say the $400 million in higher-than-expected health care costs on top of the $400 million the plan already draws from the rainy day fund and other, smaller cost increases could force the state to draw as much as $1 billion from the rainy day fund.
"If you look at the structural balance, meaning revenues coming in and spending going out, it's about a billion dollar gap," said Michael Widmer, president of the business-backed Massachusetts Taxpayers Foundation.
Panagiotakos defended using the original Commonwealth Care estimate, pointing out the same estimate was used by the House when it drafted its budget. But he also expressed concern about drawing too much from the rainy day fund, meant to help the state weather fiscal slumps.
"We are going to need that rainy day account if we get into any type of major economic downfall," he said.
Panagiotakos, who also supports casino gambling, said there's nothing stopping Republicans from offering Patrick's bill as an amendment.
He wouldn't say whether he thought the amendment would pass.
"There are going to be a lot of amendments and we are going to take them up one by one," he said.
Asked last week during a Brookline Chamber of Commerce address about whether his casino plan was dead or not, Patrick said: "It may yet come back in the Legislature. I acknowledge it's hard."
Besides pushing the casino amendment, Knapik also said he was concerned with the spiraling cost of the health care law, saying it's siphoning money away from other pressing needs.
He said the Senate should consider restricting parts of the law, designed to mandate health care to virtually all Massachusetts residents.
"We ought to have that debate," he said. "We've got to put the entire discussion of the scope of the law on the table."
----------
"Health plans' results in 1st quarter are just mediocre"
By Jeffrey Krasner, (Boston) Globe Staff, May 16, 2008
The state's major health insurers yesterday reported lackluster results for the first quarter that ended March 30.
Blue Cross Blue Shield of Massachusetts, the state's largest health insurance company with about 3 million members, cited high medical costs related to the flu. Its HMO Blue health plan lost $41.7 million on medical operations, partly offset by investment income of $25 million. The company's other health plans lost $3.4 million on operations and earned $21.4 million from investments. Combined, the organization lost $2.2 million on premium income of $1.7 billion.
Blue Cross also said it lost 35,000 members, in part through the continued acquisition of major Boston-based companies. For example, former Gillette employees were integrated into Proctor & Gamble's health plan, resulting in a loss of 17,000 Blue Cross members, the insurer said.
Harvard Pilgrim Health Care said it lost $5.2 million on operations, offset by $9.1 million in investment income, resulting in net income of $3.9 million for the quarter. Revenue from premiums was $642.5 million.
"Harvard Pilgrim's first-quarter financial results are consistent with budgeted expectations as we continue to tightly manage medical and administrative costs," said Charles D. Baker, Harvard Pilgrim's chief executive. "We expect to end the year with a modest operating gain of about 1 percent."
Tufts Health Plan stood out from its peers. The company said it earned net income of $4 million, with investment income of $8.3 million, making up for an operating loss of $3.2 million and an income tax bill of $1.1 million. The results are an improvement from the same period last year, when the insurer earned net income of less than $1 million. Membership in March reached 678,000, an increase of 24,000 from September.
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
-----
"2d-quarter revenue up at Partners HealthCare"
By Jeffrey Krasner, (Boston) Globe Staff, May 17, 2008
Partners HealthCare System Inc. yesterday reported operating income of $30 million on revenue of $1.8 billion for its second fiscal quarter, down from income of $35 million on revenue of $1.6 billion in the year-ago period. Operating margin for the quarter declined to 1.7 percent from 2.2 percent a year ago.
Peter Markell, vice president of finance, said that while revenue growth was in line with projections, more revenue came from medical than surgical cases. In addition, he said, expenses had increased, including fuel and utility costs, contractual nursing wages, and the cost of some medical supplies whose raw materials include oil.
For the year, Partners, the state's largest hospital network, is aiming for a 2 percent operating margin on operating revenue of $6.5 billion to $7 billion, he said.
After posting a $3 million loss on investments during the quarter, Partners had net income of $27 million compared to a net gain of $103 million in the same period last year.
"We think the rest of the year will be somewhat challenging but we hope to hit our budget," said Markell. "It will depend on patient volume and the mix of medical and surgical cases."
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
----------
Forum: "Massachusetts proves the folly of universal health insurance"
Tuesday, May 27 2008, The Eagle-Tribune Online, Sally C. Pipes
Universal health care recently celebrated its second — and perhaps final — birthday in Massachusetts. There's not a lot of cause for celebration. Although a success in the media and a blueprint for other politicians seeking solutions to health care — including Democratic presidential hopefuls Barack Obama and Hillary Clinton — it's proven a failure in its home state. Its father, former Republican Gov. Mitt Romney, has fled the political scene, unable to get traction in the presidential race. His partner, Sen. Edward M. Kennedy, D-Mass., current governor Deval Patrick, and a host of bureaucrats are left to deal with the mess.
The program is in intensive care, surviving only on massive infusions of other people's money. The plan's boosters celebrate that it's covered 342,000 people. Quite an accomplishment until we understand that of these, 176,000 are enrolled in nearly free or entirely free plans — free to enrollees but not state and federal taxpayers. Another 55,000 were simply enrolled in Medicaid.
This is all quite expensive but was supposed to be covered by simply shifting dollars that were already in the system, allegedly being frittered away by free-riders who elected not to purchase insurance and companies who didn't pony up for employees. Projected revenues from business, however, are nowhere to be found. Transfers of dollars from the existing free care pool are lower than expected — even as charity hospitals that rely on these monies report major hardship. Bureaucrats long ago gave up hope of providing universal coverage, even with the mandate. Among their early acts was to exempt 20 percent of the state's uninsured from having to participate in the universal insurance program. Now they are clinging to the hope of merely keeping the massive welfare expansion afloat.
This entire mess was predicted. The original promise of reform — like the promises currently coming from Obama and Hillary — was absurd. As if by magic, the public was told that the state could cover everyone, reduce the cost of health insurance, and save money on health care simultaneously. Free riders were demonized and told to purchase insurance.
A few of us objected loudly at the time. We employed logic, economics, history and a bit of humor. "The elected leaders of Massachusetts have come up with a novel solution for the vexing problem of having to pay for health care," wrote economist and author Arnold Kling in the Wall Street Journal in April 2006. "Abolish the laws of arithmetic." Kling and others pointed out the peril to state taxpayers of offering a new government program based on a $219 penalty for not purchasing a health care plan with a zero dollar deductible and an average cost to taxpayers of $6,000.
The bipartisan brigade marched ahead anyway and put the bill into law in April 2006. The system immediately conformed to our expectations. When premiums came in higher than predicted by politicians, the politicians leaned on the carriers, increased taxpayer subsidies, and exempted people from having to purchase the insurance. People flocked to the free plans, but were a bit slower to reach into their pockets for the plans that required premiums. Those who did, however, proved to be heavy users of the system. The plan was far enough gone that a year ago we penned a birthday op-ed predicting that even as backers had abandoned universal coverage, costs were set to skyrocket.
The next year went from bad to worse. Even as Hillary and Obama travel the country promising to nationalize the Massachusetts experience, the folks in Massachusetts are in Washington begging the Bush administration for more money merely to keep it limping along. Politicians pegged estimates for spending on subsidized plans at $750 million for 2009. The current administration puts them at $869 million, and even this is expected to be $100 million short, an amount that is noticed in a state facing a $1.3 billion deficit.
Meanwhile, even the limited abilities and ambitions of local politicians and left-wing health care advocates have deteriorated. The new imperative, all agree, is cost control. Yet unwilling to employ even the slightest free-market mechanisms and deregulation, they are peddling more of the same medicine that is causing the sickness. The leading state senator, Senate President Therese Murray, is pushing a plan to spend more money on information technology and prohibit pharmaceutical reps from communicating with doctors.
The folks at a popular pro-universal coverage organization are looking to non-human sources of funding. "The costs of CommCare cannot be sustained by taxpayers and enrollees," blogs Health Care for All executive director John McDonough. "It won't work."
This is simply to say that people can't pay for it. So if people can't pay, who can? McDonough and company, still in search of their free lunch, are pushing for price controls on providers and hospitals, as if these costs won't ultimately be borne by people.
The nation owes a great deal of gratitude to Mitt Romney, Edward Kennedy, state representatives, the think tankers and health care activists who produced the Massachusetts plan. In providing a real life experiment in time for it to simultaneously be adopted by Democratic presidential candidates and implode under its own contradictions, it provides a reality check on the promises of today's politicians.
When Hillary and Obama claim to be able to provide universal third-party insurance with only minor disruptions to the current system, voters can look to Massachusetts and understand that they are just making promises they can never keep.
-
Sally C. Pipes is president and CEO of the Pacific Research Institute. She is author of "Miracle Cure: How to Solve America's Health Care Crisis and Why Canada Isn't the Answer."
-
----------
"Lesson on health care"
contracostatimes.com - MediaNews editorial
ONE OF THE BENEFITS of federalism is that it gives individual states the freedom to enact their own government programs, serving as laboratories of democracy. Often programs in one state are copied by others or have even become national policy.
For example, California took the lead decades ago in requiring smog control devices on automobiles. Now such pollution controls are national policy. Wisconsin's welfare reforms laid the foundation for national welfare reform under the Clinton administration.
We now have an opportunity to examine a bold health care reform that was enacted in Massachusetts two years ago and went into effect last July 1. It is providing valuable information on possible similar reforms in California and nationally.
Under the Massachusetts reform, everyone is required to obtain health insurance. The idea is to remove the economic burden on hospitals and other health-care providers of caring for uninsured patients, especially those who use emergency rooms a their primary source of medical attention.
Massachusetts also has set up a state-run health insurance system called Commonwealth Care designed for low-income residents. It uses a sliding scale of subsidies for everyone under 300 percent of the federal poverty level, or about $63,000 for a family of four.
The hope of former Republican Gov. Mitt Romney and the Massachusetts Democratic Legislature was that by eliminating "free-rider" use of emergency rooms, costs and insurance premiums would drop, making coverage more affordable for more people. Also, the insurance mandate was supposed to result in universal coverage. Unfortunately, a considerable gap opened between hope and reality.
While the number of uninsured has dropped from about 660,000 to 350,000, Commonwealth Care has accounted for 60 percent of the growth in individual insurance over the past year.
That means many people are still using the "free" services of emergency rooms. Insurance premiums have not significantly changed and the cost to the state is skyrocketing.
The anticipated cost of operating Commonwealth Care was $472 million, which the Legislature appropriated. However, that figure falls far short and the governor is seeking another $153 million, making the total cost $625 million.
For next year, the governor wants $869 million for the state insurance program, which he believes still will not be enough. Estimates of cost overruns over the next decade are $4 billion.
Also, it is likely that the state program is displacing private insurance for many people as well as providing new coverage for uninsured residents.
What Massachusetts failed to do is help direct uninsured people toward using private insurance providers and HMOs. Instead, the state made it more difficult for private insurers to offer low-cost basic policies by imposing costly mandates on them.
Had the state worked with private HMOs and insurance coverage first and then subsidized low-income people, the results could have been considerably better. Instead, the emphasis was on universal care, which has failed to succeed.
The lesson here is not to give up on health care reform, but to examine what does and does not work.
The Massachusetts experience with health care reform, flaws and all, offers valuable information for state and national policy makers. They should not ignore it.
----------
May 25, 2008
"A healthy start: Changes take hold for how the uninsured obtain medical care"
By Lisa Eckelbecker (Worcester) TELEGRAM & GAZETTE STAFF, leckelbecker@telegram.com
Free medical care for poor, uninsured people dropped slightly at 11 Central Massachusetts hospitals during the first fiscal year the state required residents to obtain health insurance, while the overall cost of that hospital care remained little changed from the previous year, according to health care data from the state.
The changes, which were more dramatic at some hospitals, took place as thousands of people in the region signed up for health insurance and suggest that the state successfully moved some uninsured residents into free or subsidized health plans and checked the growth of charity care at hospitals.
The shifts should become more apparent this year as uninsured people continue to sign up for state-subsidized insurance offered under the name Commonwealth Care, said John G. O’Brien, chief executive of UMass Memorial Health Care, which operates hospitals in Worcester and has affiliations with four community hospitals.
“We now are starting to see, each month, greater Commonwealth Care use, and now we are starting to see a drop in the number of people in the free care pool,” Mr. O’Brien said.
The amount and cost of free care at Massachusetts hospitals is one of the barometers of the state’s health insurance initiative, which was signed into law in April 2006 and mandates that all residents obtain health insurance. The law also created the Commonwealth Connector, an entity responsible for spearheading subsidized health plans for people unable to afford coverage on the open market.
More than 300,000 uninsured people have signed up for insurance since mid-2006, according to state and industry sources. About 110,000 have enrolled in private plans, including 18,122 who had signed up as of May 1 for Commonwealth Choice, an unsubsidized option developed by the connector authority. Commonwealth Care had signed up 176,879 people for subsidized plans as of May 1. Another 72,000 had enrolled as of March 31 in MassHealth, the Medicaid health plan for the poor that is funded by the state and federal governments.
Massachusetts has traditionally paid for free hospital care through a fund called the uncompensated care pool. Now known as the health safety net, the fund takes in money from hospitals and adds state money, then sends payments back out to hospitals that submit claims.
The state has reported that the use and cost of free care at hospitals has dropped since 2006. Earlier this year, the Massachusetts Hospital Association calculated that uncompensated care dropped 11.7 percent and uncompensated medical costs qualifying for reimbursement from the state fund dropped 7.5 percent, mostly because of shifts at big Boston and Cambridge hospitals.
In Central Massachusetts, hospitals reported 78,396 free inpatient hospital stays and outpatient visits during the fiscal year ended Sept. 30, 2007, down 5.09 percent from 82,601 inpatient and outpatient visits in the previous fiscal year, according to data provided by the state Division of Health Care Finance and Policy.
The state determined the cost for those visits was $47.7 million in 2007, less than 1 percent more than the $47.4 million in costs in 2006. Over roughly the same time period, 11,748 people in Worcester County enrolled in Commonwealth Care subsidized health insurance, according to the Commonwealth Connector.
Some hospitals reported dramatic changes in free care. The number of times that patients checked into Harrington Memorial Hospital in Southbridge or visited for outpatient treatment dropped 66 percent in 2007, and costs were down 50 percent. Use was down 13 percent at Milford Regional Medical Center in Milford, including the medical center’s rehabilitation, radiology and Whitinsville centers, and costs fell nearly 26 percent.
“We certainly have experienced a reduction in the number of claims we are writing off as free care, and that is continuing this year,” said Jeanne P. Lynskey, chief financial officer of Milford Regional.
In Worcester, free care use dropped 6 percent at St. Vincent Hospital, but costs went up 4 percent. Use fell less than 1 percent at UMass Memorial Medical Center, including the University, Memorial and Hahnemann campuses plus the Tri-River, Barre and Plumley Village centers. Free care costs at UMass Memorial increased 8 percent, according to the state.
The reason some hospitals have seen big drops in free care while others have noticed little change remains unclear, said Brian Rosman, research director of Health Care for All, an advocacy organization.
“Some have been going down pretty sharply. Some have been steady, and some have had an increase,” Mr. Rosman said. “And I don’t think anybody knows why.”
The largest organizations may have been better equipped than smaller hospitals to guide uninsured residents to insurance options, said James T. Kirkpatrick, vice president of health care policy for the Massachusetts Hospital Association.
“Just getting a patient into the hospital doors, getting them set up to provide service, that’s a big enough job for most hospitals,” Mr. Kirkpatrick said.
State grants, which are up for reconsideration in the Legislature, allowed some health systems to aggressively enroll people. HealthAlliance Hospital in Leominster and Heywood Hospital in Gardner participate in a grant-funded enrollment effort, and use of free care dropped modestly at both hospitals. Reimbursements for free care constituted 2.5 percent of total revenues at HealthAlliance in 2007, but are down to 1.8 percent so far this year, according to HealthAlliance figures.
Even as free care has dropped, some hospitals have become busier. As St. Vincent Hospital’s uninsured patients enrolled in health plans, they began seeking more care, sometimes for conditions that had been neglected for years, said Stephen R. Gilmore, St. Vincent Hospital chief financial officer.
“Now that these folks are covered, they’re utilizing the services that are out there for them, whereas in the past they may have dealt with their illness” on their own, Mr. Gilmore said.
Demand is also up for primary care doctors.
“The most common question people ask me is, ‘Are you taking new patients?’ ” said Dr. George Abraham, who practices at St. Vincent Hospital’s free clinic on Vernon Hill and is medical director of the Central Massachusetts Independent Physicians Association.
Requests for free care from people who have dropped out of subsidized insurance plans are persisting, too. Some patients sign up for plans, then stop making payments or don’t keep up with paperwork and end up back in hospitals in search of free care, said George W. Fitton, assistant administrator at Hubbard Regional Hospital in Webster.
“People have to be motivated,” Mr. Fitton said. “After they’ve gotten the service, they don’t have a whole lot of motivation.”
The state is trying to motivate them, instituting new requirements last fall that eligible patients sign up for Commonwealth Care instead of seeking free care. The state has also allocated 30 percent less to the health safety net this fiscal year than it did last year.
Health officials said that despite those efforts, they expect the state will continue to need a fund to cover free care at hospitals for those who cannot or do not obtain coverage.
“We know that despite all our best intentions with health reform, it’s to get as close to universal coverage as we can, there are going to be a small number of people who for whatever reason will remain without coverage and the health safety net will remain an important source of financing,” said Sarah K. Iselin, commissioner of the state Division of Health Care Finance and Policy.
-
www.telegram.com/article/20080525/NEWS/805250354/
-
(picture):

-
Dr. George Abraham, right, discusses health issues with patient Micael Brahne, center, at St. Vincent Hospital’s free clinic on Vernon Hill in Worcester. At left is Tam Chang, a physician’s assistant from Family Health Clinic on Queen Street, who also serves at the St. Vincent clinic. (T&G Staff / JIM COLLINS)
-
(graph):

-
"We certainly have experienced a reduction in the number of claims we are writing off as free care, and that is continuing this year."
-
(picture):

-
John G. O'Brien, chief executive of UMass Memorial Health Care
-
----------
-

-
(Getty Images)
-
The Boston Globe, Op-Ed, ANNIE BREWSTER
"The crisis of primary care physicians"
By Annie Brewster, May 29, 2008
MRS. J. LOOKED baffled and hurt. I had just explained that I would no longer be her primary care doctor. I was leaving the field after just three years. "I have had three different primary care doctors over the past 10 years," she said. "You can't leave now. I was just starting to feel comfortable. I am getting older now. I can't keep changing doctors!"
Primary care is in crisis. Current primary care doctors are quitting, and medical students are pursuing other specialties. Primary care has lost its attractiveness as a profession because of poor compensation and plummeting job satisfaction. Primary care physicians are in short supply, and in Massachusetts, this problem has intensified in the wake of healthcare reform, as more than 300,000 previously uninsured individuals have joined in the search for available doctors.
As a former primary care physician, I am most troubled by the antagonistic state of the patient-doctor relationship. The system sets us against each other. Like many in the field, I chose primary care because I love people. I wanted to take care of the whole person, body and mind. I wanted the intimacy that comes with knowing your patients well and following them over many years. These goals are difficult to achieve in primary care today. After two years in my practice, I walked into an exam room one day and introduced myself to a patient. "We have met before," she replied, clearly aggravated. I was horrified and saddened.
Patients are angry, and rightly so. They feel frustrated by the inability to get timely appointments with their physicians, rushed by the 15-minute visits and the seemingly harried doctors, ignored when they do not receive letters with lab results or follow-up phone calls. They feel disrespected when they come to their medical appointments on time and then sit in the waiting room for 45 minutes. All of these feelings are justified. We are not offering high-quality care.
Doctors feel angry, too. We have too many patients. It is not uncommon for a full-time primary care doctor to have upwards of 3,000 patients. It is impossible to know all of these individuals well, to give adequate focus to each person's unique situation, to sift through the piles of paperwork and lab data daily. Our days are divided into 15-minute sessions, back to back. We move frantically from exam room to exam room, trying desperately not to fall behind in our schedule. We are given incentives to see patients as quickly as possible. We live in fear of litigation.
We are drowning, and in this overwhelmed state we lose our ability to take good care of people. Outwardly, we may feel resentful and burdened. Underneath, many of us feel loss, deep sadness, and personal failure.
This rift between patient and doctor is painful and destructive to the core of medicine: the therapeutic relationship. In an environment where patients and doctors don't know each other well and appointments are rushed, it is inevitable that more medical errors occur and that resources are wasted as expensive tests are substituted for communication. By contrast, research indicates that medicine practiced in the context of solid primary care relationships allows for earlier detection of chronic diseases, and, ultimately, better outcomes and monetary savings, to say nothing of patient and doctor satisfaction
In this election year, patients and doctors need to come together to support healthcare reform aimed at revitalizing primary care. To begin, our medical reimbursement system must be restructured. Our payment system values invasive treatments and procedures over time spent talking with your doctor. We need to reset these compensation levels to favor communication, care coordination, disease prevention, and chronic disease management. Doctors should be rewarded for keeping patients well. Incentives should be based on quality outcomes and efficient resource use, not on patient volume.
Most important, primary care physicians should be valued as team leaders and advocates, poised to help patients navigate the complex medical system. There is no reason why so many patients like Mrs. J. need to feel lost and abandoned in a country that spends far more on healthcare than any nation in the world.
-
Dr. Annie Brewster is an urgent care physician at Massachusetts General Hospital.
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2008/05/29/the_crisis_of_primary_care_physicians/
-
----------
"Health insurance gains detailed: Study finds steep increase in coverage"
By Elizabeth Cooney, (Boston) Globe Correspondent, June 3, 2008
The number of uninsured adults in Massachusetts fell by almost half last year, says a study released today, while the state's Revenue Department reports that 86,000 people paid a state tax penalty rather than buy insurance.
Supporters of health insurance reform said both numbers were a sign of success, that not only are more people getting coverage, but that only a fraction of taxpayers contested the health-insurance mandate.
The study found widespread support for the two-year-old law among those who are already insured, with 71 percent favoring the effort. Among the uninsured, who are more likely to be subject to the tax penalty, the level of support dipped to 44 percent.
"This was the first test in the country of an individual mandate," said Drew Altman, president of the Kaiser Family Foundation, a California-based think tank that was not involved in the research. "People didn't know whether the citizens of Massachusetts would go along with it or rebel. They got the program off the ground with broad-based support, they have dealt with implementation problems they have faced so far, and they have covered more than half of the uninsured. So far it seems to be working."
In the first year that state residents had to report their insurance status on their tax returns, roughly 86,000 who filed their taxes on time chose not to buy insurance and gave up their $219 personal tax exemption. Another 6,000 were deemed able to afford insurance, but are contesting the penalty. For about 62,000 filers, insurance was determined to be too expensive, and they were not penalized.
Penalties for those who can afford insurance will be higher this year, totaling as much as $912 for someone who goes all year without coverage.
In enrollment, the biggest improvement has been among the people least able to afford coverage. Among adults whose family income fell below 300 percent of the federal poverty level, the rate of those without insurance fell by almost half. For adults whose income was lower than the poverty line, the numbers dropped by two-thirds, according to the study, which was conducted by the Urban Institute, based in Washington, D.C., and appears in the journal Health Affairs.
The telephone survey of 3,000 working-age adults found that overall, 13 percent of respondents had no insurance in fall 2006, just before the law took effect. The rate fell to 7 percent of adults a year later, after an expansion in Medicaid, the creation of a state-subsidized plan called Commonwealth Care, and the introduction of a private purchasing plan called Commonwealth Choice.
The biggest remaining challenge is reining in the costs of providing care for those who qualify for subsidized insurance. The state has budgeted $869 million this year, nearly $150 million more than it anticipated, because of high enrollment, and expects costs to rise even higher.
"The long-run success of Massachusetts' efforts will hinge in part on sustaining support for the new policies in the face of these higher costs," according to the study.
Continuing medical inflation combined with a slower economy are also worrisome. And another glitch: The jump in insured people has not been matched by a rise in the number of doctors.
"There are 355,000 newly insured people over last year," said Jarrett Barrios, president of the Blue Cross Blue Shield of Massachusetts Foundation, one of the funders of the Urban Institute survey. "In that year there were not enough new primary care practitioners coming online to accommodate these folks. In many important ways, health reform has been a victim of its own success."
But Brian Rosman, research director of Health Care For All, a local advocacy group, said he hears what coverage means to the 700 people who call a help line each week.
"Again and again we find formerly uninsured people who were ignoring serious medical needs now have coverage and now say the program is literally saving their lives," said Rosman, who helped write a second paper in Health Affairs.
The survey also allays one early concern: A fear that businesses would cut benefits once the state began offering subsidies. Employers did not appear to have reduced the insurance they offered to their workers, judging from the stable levels of adults who said they could get coverage at work both before and after the law took effect.
More low-income people went to a doctor or a dentist for a check-up in the past year, but people still had trouble finding a primary care provider, the survey found. Emergency room visits didn't budge from their high levels before the healthcare law passed, suggesting unfamiliarity with the healthcare system or reflecting a nationwide shortage of doctors available to treat prospective patients, said Sharon K. Long, the survey's author.
The survey found that last year, out-of-pocket spending on healthcare, mostly for prescription drugs, fell, as did the proportion of adults saying they were having problems paying their medical bills.
"Clearly the drop in the uninsured rate is an impressive first-year drop and a significant finding," Long said. "It's not just the gain in insurance coverage, but access to care and affordability of healthcare for individuals that has improved with insurance coverage. This is a broader change than just expanding coverage."
-
www.boston.com/news/local/articles/2008/06/03/health_insurance_gains_detailed/
-
www.boston.com/news/local/articles/2008/06/03/health_insurance_gains_detailed/?page=full
-
www.boston.com/news/local/articles/2008/06/03/health_insurance_gains_detailed?mode=PF
-
----------
“Dose of bias is unhealthy”, The Boston Herald, Saturday, May 31, 2008, Page 16, Op-Ed, By John Abramson
I recently testified at a hearing in federal court concerning the activities that resulted in overpayment of several billion dollars for the drug in question. The judged opened the hearing by quoting the highly respected American Law Institute’s statement that the fundamental purpose of a corporation is to maximize profits and return those profits to its shareholders.
Though the pharmaceutical industry does an excellent job of convincing doctors and the public that its fundamental mission is to improve our health, don’t be fooled – its real job is to sell the most drugs for the highest price. And they do so by capitalizing on every opportunity to influence our beliefs about the need for and benefit of their products.
Providing gifts to physicians and financial support to hospitals for continuing medical education are an integral part of the drug industry’s strategy to achieve this goal. If these were the only sources of bias in what doctors believe is the best way to treat their patients, the legislation to ban these activities – courageously passed by the (Massachusetts) State Senate and pending in the House – would still be vital, but not of such critical urgency.
Unfortunately, they are just the tip of the iceberg. It is what is beneath the surface that is the real problem.
Over the past 30 years, the funding of clinical trials has been largely removed from the National Institutes of Health and taken over by the drug and medical device industries. Consistent with their fundamental mission, these industries design their research to maximize their return on investment. Medical knowledge itself has become a commodity, produced for its business value rather than its health value.
It is not just the commercially biased “educational moments” that are the quid pro quo that come with the gifts to doctors. No, the problem starts with the “scientific evidence” that we doctors read in our most respected journals.
More than two-thirds of the clinical trials that are published in our most trusted medical journals are commercially sponsored. And the odds are five times greater that the commercially sponsored studies will conclude that the sponsor’s drug is the treatment of choice compared to non-commercially funded studies of exactly the same drug. (Wouldn’t it be nice to take those odds to the casino?)
In other words, what we naively think of as objective science is more often than not as extension of marketing – an infomercial.
This is an enormous problem and goes a long way toward explaining why Americans pay twice as much for health care as the citizens of the next 21 wealthiest countries, but actually live two and a half fewer years in good health than the citizens of those countries.
The drug industry has so much money and power that even raising these issues is a third rail for American politicians. The head of U.S. operations for drug-maker Glaxo-Smith-Kline recently attempted to wield some of that power when he threatened decreased investment if the proposed ban on gifts in passed.
So if you want your doctor to be as independent of commercial influence as possible when deciding the best treatment for you and your loved ones, the gift ban is a necessary first step.
But we citizens also must be ready to exercise our power as consumers. The drug and medical device companies should know that blocking this legislation or not participating in a voluntary ban on gifts to doctors could result in a consumer boycott of their drugs and devices that have me-too therapeutic equivalents made by companies that are honoring the ban. This is the way to help the medical industry serve its shareholders by better serving the public interest.
-
John Abramson, author of “Overdosed America: The Broken Promise of American Medicine” is a clinical instructor at Harvard Medical School.
-
----------
A Boston GLOBE EDITORIAL
"Health reform is working"
June 4, 2008
THE 350 PEOPLE who packed into the main conference room of the John F. Kennedy Library yesterday were in a good mood. They were about to hear a report that implementation of the Massachusetts health reform law had, in less than two years, cut the number of uninsured people of working age nearly in half. Then they got the bad news from House Speaker Salvatore DiMasi, one of the progenitors of the law: "The third year . . . will be the most difficult."
The law has resulted in health insurance coverage for 355,000 people, but it is costing more than expected, and it was mainly funded by two uncertain revenue sources: money that would otherwise go to hospitals to treat the uninsured, and a special waiver of federal Medicaid rules. The waiver, which freed up money to expand insurance coverage, expires in less than a month. A renewal seems likely, but it's unclear how much money the state will receive.
And the law hasn't done anything to alter treatment patterns that have burdened Massachusetts with some of the nation's highest medical costs. "We must contain costs," said Senate President Therese Murray. "We must stay together and be fully committed to the second phase of healthcare reform."
A far-reaching cost containment bill supported by Murray has cleared the Senate and is awaiting House action, which DiMasi promised is coming soon. Among other things, the bill calls for more transparency by insurance companies, a statewide system of electronic health records, better recruitment of primary-care doctors, and a ban on gifts from drug companies to physicians.
This last item has provoked opposition from the catering industry. Drug companies would no longer be able to roll out free lunches to attract physicians to informational meetings. But a doctor's prescription patterns should not be swayed, even a little bit, by food or other gifts. Murray's proposal should become law.
A ban on free lunches is nothing compared to the other changes that will be required to make health reform work. Hospitals will need to make sure that expensive procedures actually produce results. Insurers will need to devise payment systems that reward quality, not just quantity of care. Patients will need to be more cost-conscious, especially about unnecessary visits to emergency rooms.
In 2004, when the Blue Cross Blue Shield of Massachusetts Foundation convened the first meetings to solve the unemployment problem in Massachusetts, few would have thought the state could have advanced so far, so fast. The task is still daunting, but the commitment remains strong.
----------
"Checkup for healthcare law"
Updated: 06/05/2008 07:07 AM
By: Ryan Burgess, Capital News 9
NORTH ADAMS, MA -- The phone in Chip Joffe-Halpern's office has been ringing off the hook because he helps to get thousands of people health insurance in Massachusetts. A new law requires every adult to have coverage, or risk losing their $219 tax exemption. So far, Halpern says the new system is healthy.
"It works. We have covered probably half the uninsured in a year and a half's time. That's remarkable. Over 335,000 people who were previously uninsured now have health insurance in Massachusetts because of this law," said Joffe- Halpern.
Joffe-Halpern serves on the committee that just released the first major study on this new healthcare overhaul. He says although there were some initial problems with funding and the length of time it took to sign people up, this checkup passed with flying colors.
"Of individuals who filed their taxes in Massachusetts, 95 percent had health insurance. Only 2.5 percent will be penalized for not having health insurance. And another two percent got a waiver because they really couldn't afford it," said Joffe-Halpern.
A hospital official says one of the biggest advantages of this new healthcare overhaul isn't just that fewer patients are uninsured. It's also that more people are showing up to doctor's offices and hospitals to get preventative care.
"Individuals who have historically not had access to healthcare because they haven't been covered by health insurances, will start getting preventative care [and] will start utilizing the emergency department less frequently for primary care," said Northern Berkshire Healthcare Revenue Cycle Director Gary Smith.
It's just one more healthy reason to have health insurance coverage.
--
Checkup for healthcare law
A report on Massachusetts' new landmark healthcare law that requires every adult to have health insurance has just been released. Our Ryan Burgess talked to an official who helped to write that report to find out how it is working.
--
http://capitalnews9.com/content/headlines/117430/checkup-for-healthcare-law/Default.aspx
--
----------
"A partial cure"
The Berkshire Eagle - Editorial
Thursday, June 05, 2008
The state's health reform measures have cut the number of uninsured adults nearly in half, most of them residents who have been unable to afford coverage. That's great news, but the trouble ahead lies in rising costs threatening the viability of a noble effort that attempts to skirt rather than solve the basic problems plaguing the nation's health care system.
Coverage for an additional 350,000 people has come courtesy of the law, and about half of them are adults well below the federal poverty level. That so many people with so few resources are receiving health care that was previously denied them is a clear victory. That only 86,000 residents chose not to buy health insurance and give up their $219 personal tax exemption indicates general support for the state's pioneering health-insurance mandate.
Unfortunately, the program is more costly than expected and additional revenue sources are largely speculative. If too much of a financial burden is placed on business, economic growth in the state will be threatened. A bill before the Legislature calling for greater transparency among insurance companies and measures to bring more primary-care doctors to the state is laudable but doesn't really address the state's high medical costs.
The state and nation are being dragged down by a profit-driven health care system in which the burdens of bureaucracy and exorbitant executive salaries are driving up costs while tying the hands of physicians. If that doesn't change, no reform measure no matter how imaginative or well-intended will address all of the system's many failings.
----------
A Boston GLOBE EDITORIAL
"Better care is primary"
June 3, 2008
DR. JOSEPH PEPPE is happy to get help in repaying his medical school loans. He and 46other primary care doctors received this benefit in exchange for agreeing to work at a Massachusetts health center for two to three years. "I very much enjoy the work I do," he said a few days ago at the South Boston Community Health Center.
Loan repayments total up to $75,000 over three years. The program is a recognition that physicians need incentives to practice in primary care instead of a higher-paid specialty. A year or two longer in residency to become a specialist can result in a doubling of income, from perhaps $150,000 to $300,000.
Primary-care physicians are in short supply in high-cost Massachusetts. The state Medical Society reported last year that 51 percent of internists were accepting new patients, compared with 66 percent in 2005. Primary care ought to be widely available to cope with the influx of people newly insured under the 2006 Health Reform Law.
The health centers are in particular need because they usually pay less than physicians can earn in private practice. The Massachusetts League of Community Health Centers figures that its 52 centers, with 700,000 patients, have a 10 percent vacancy rate for primary-care positions.
The loan-relief program is a joint effort of the League; state government; Neighborhood Health Plan; Partners Healthcare; the Blue Cross Blue Shield Foundation; and the Bank of America Charitable Foundation, which contributed the largest share, $5 million. Local interventions like these, while welcome, don't get at the root of the problem afflicting medicine throughout the United States: a piecemeal approach to reimbursement that elevates individual procedures by specialists over care coordinated by a primary-care doctor.
Medicare, the largest single payer of healthcare services in the country, inadvertently encourages uncoordinated, excessive care. In 1992 Congress established a physician payment system intended to limit costs, but the federal government gave advisory authority to a committee weighted in specialists' favor. This committee offers payment recommendations for more than 7,000 different procedures, and the more physicians do, the more money they make.
To improve primary care, the federal government wants to add a management fee to the usual visit payment. An informal coalition of primary care providers favors an approach that does away with piecemeal reimbursement, which has led to rushed visits, reduced access, unhappy patients and demoralized physicians. The coalition is trying to get insurers in Massachusetts interested in a "Medical Home" model, in which primary-care practices would receive a comprehensive payment in return for high-quality, patient-friendly care.
A patient's Medical Home would include a multidisciplinary team (say a nurse practitioner, nutritionist, and social worker), enhancing patient support while allowing the physician more time to take a patient's history, diagnose his or her condition, devise a treatment plan, and provide unhurried explanations. In exchange for achieving better outcomes, the primary-care practice would get a higher overall payment from the insurer than under the current system.
This sounds a bit like the old managed care model, which physicians and patients decried in the 1990s for its inadequate payments and frequent denials of care. However, the coalition would make the payments higher and adjust them depending on how medically needy the patients are and how well the practice achieves good results. Last month the Capital District Physicians' Health Plan, in Albany, announced a two-year trial in which they will implement the comprehensive payment plan.
Dr. Bruce Nash, medical director of the Capital District plan, said the Albany area is experiencing the same primary-care shortage as Massachusetts. For the Albany experiment to succeed, it must produce savings without diminishing the quality of care. "We can't pay physicians more unless they create value," Nash said.
The United States spends more per capita on healthcare than any other nation, yet doesn't produce the best outcomes, and leaves 47 million Americans without health insurance. Specialists aren't the villains here. They are essential for treating complicated conditions, but they benefit from a system that is badly out of whack.
Community health centers like the one in South Boston have been trying to provide a medical home for patients, many of them with low incomes, since the late 1960s. The US healthcare system has resisted extending a comprehensive model of care to all segments of society. The Albany experiment offers hope that incentives can be changed to improve the quality of medicine and provide more physicians with the job satisfaction that Peppe enjoys.
----------
(A Boston) GLOBE EDITORIAL
"Keep health reform moving"
June 19, 2008
IN JULY 2006, US Health and Human Services Secretary Michael Leavitt praised the Massachusetts health insurance plan as a national model. He was in Boston then to announce the extension of the special Medicaid funding that enabled Massachusetts to expand coverage to nearly everyone. Leavitt needs to quickly extend this money, which is available through a waiver of Medicare rules, so that the state's landmark initiative can continue.
Governor Patrick is meeting with Leavitt tomorrow to discuss renewal of the waiver, which expires June 30. Patrick might recall the words of his predecessor, Republican Mitt Romney, who told Leavitt in 2006: "Massachusetts is now at the forefront of a revolution in the way we think about healthcare." He added, "The reforms we crafted bring coverage to all our citizens."
Romney was indulging in a bit of hyperbole. The state hasn't managed to cover everybody, but a study by the Washington-based Urban Institute found that 93 percent of the working population had health insurance as of last fall. Sharon Long, researcher on the study, figures that if children and the elderly are included, the total insured population in Massachusetts exceeded 95 percent, an extraordinary figure given that the national rate was about 84 percent in 2006, the year with the latest Census figures.
"None of us should expect perfection here," Leavitt said in 2006. "Mistakes are going to be made."
The Legislature has provided an adequate share of money. The new healthcare connector authority has created subsidized coverage for those just above the poverty line. Private companies have written policies for these people, and for those who can afford unsubsidized insurance. The experiment has gone well, with one exception: The state underestimated the number of people who would enroll in subsidized plans.
It's unclear how much money is involved in the waiver renewal negotiations, but the amount is sure to exceed the $625 million annual federal contribution under the current plan. The governor and Legislature are ready to provide money to accommodate extra enrollment, but they need help.
Many people contributed to the passage of the healthcare law in 2006, notably Romney, Leavitt, and his predecessor Tommy Thompson - all Republicans - along with Senator Edward M. Kennedy and the Democratic legislative leadership. Leavitt said then that "every component of our society" needs to contribute to providing access to affordable, basic healthcare. Massachusetts has shown it can be done. The Bush administration, led by Leavitt, needs to help maintain progress toward this bipartisan goal.
-----
The Boston Globe - Letters
"Paid sick days must be part of prescription"
June 24, 2008
YOUR EDITORIAL "Keep health reform moving" (June 19) justly praises Massachusetts for its landmark healthcare initiative. More than 93 percent of the working population in Massachusetts has health insurance. This is laudable. But another statistic tells a different side of healthcare access. Almost half of Massachusetts workers don't have a single paid sick day. If they miss work to see a doctor, they lose a day's pay and may lose their job. What good is insurance coverage if you can't afford to take time to visit the doctor?
Senate Bill 1073 would guarantee paid sick days to all Massachusetts workers to be used for illness, doctor visits, or care for a child, spouse, or parent. When people go to work sick, they often pass the disease to co-workers. Paid sick days reduce the spread of disease, and decrease outbreaks among vulnerable groups such as nursing home residents and children. They could also lower healthcare costs by speeding recovery.
Paid sick days are the missing piece of healthcare reform. Without them, many of the same workers we congratulate ourselves on covering can't access the healthcare they need.
PATRICIA JEHLEN, State senator, Somerville, Massachusetts
------------
The Boston Globe, Saturday, June 21, 2008, Page B2, City & Region
“Patrick reaches deal on Medicaid waiver”
Governor Deval Patrick has reached a deal with the Bush administration to give Massachusetts a 2-to-4-week extension of a critical Medicaid waiver. An official familiar with a meeting between Patrick and Health & Human Services Secretary Mike Leavitt said they reached an agreement yesterday, Friday, June 20, 2008. The extra time will let the parties negotiate a further extension to a $400 million Medicaid waiver that has powered the state’s universal healthcare program. Senator Edward M. Kennedy called Leavitt on Thursday, June 19, 2008, to push for the extension. (AP)
------------
Columnists
Tisei: Federal Medicaid waiver has big implications for state
By Sen. Richard Tisei/A View from the Hill
Friday, June 27, 2008
Malden -
All eyes are on Washington this week, as Massachusetts officials anxiously await news about the fate of the state’s expiring federal Medicaid waiver, and whether federal officials will agree to extend it for another three years.
The looming decision by the Bush Administration is an important one, because it will have broad financial implications on the state budget for Fiscal 2009 which starts July 1. The decision will also go a long way towards determining what direction the two-year-old Massachusetts Health Care Reform Law will take moving forward.
The current Medicaid waiver, which helped pave the way for the landmark 2006 law, is due to expire June 30. Last Friday, Massachusetts earned a temporary reprieve when U.S. Health and Human Services Secretary Michael Leavitt agreed to grant a two-to-four week extension of the waiver as talks continue to take place between state and federal officials.
The stakes are high in these negotiations. Without significant increases in federal funding, the commonwealth’s health insurance program would have to be curtailed to prevent its collapse. The alternative would be to reduce funding for other important state programs and divert that funding to health care.
Securing a waiver extension is critical to the continued viability of health care reform. In the past, Medicaid funding was restricted primarily to reimbursing hospitals that care for the poor and uninsured and administering the state’s MassHealth program.
Under the soon-to-expire federal waiver, a large portion of that money is now being spent on Commonwealth Care, the state-run health insurance program that provides coverage for low- and moderate-income residents.
Over the last three years, Massachusetts has received more than $600 million annually in federal funding, at least $385 million of which is used to subsidize health insurance coverage. Another $225 million goes toward hospital payments and Medicaid program expansion.
The state is not only seeking a three-year waiver extension, but also is counting on a 14 percent increase in federal matching funds to support Commonwealth Care and what remains of our free care program. However, federal officials may not be willing to agree to such an extension, or to commit to such a large funding increase.
The State House News Service reported last week that the Bush Administration is concerned about the slow pace by which the state is reducing use of the free care pool. In Fiscal 2006, free care cost the state $647 million, but even with reductions in the number of uninsured residents, that figure is expected to drop to only $453 million for Fiscal 2009.
Federal officials are also considering tightening Medicaid eligibility standards to limit subsidized coverage to individuals earning up to 200 percent of the federal poverty level. The state’s Commonwealth Care program permits subsidized health care coverage for those earning up to 300 percent of the federal poverty level, which means some individuals could end up losing subsidized coverage if the changes go through.
Amidst all this uncertainty, the state is hoping for a quick resolution to the waiver negotiations. Conference committee members are hard at work trying to resolve the differences between the House and Senate versions of the Fiscal 2009 budget. They have been working under the assumption that the waiver will be extended and an increase in federal dollars will flow into Massachusetts.
The Fiscal 2009 budget has been built on a house of cards. If federal Medicaid funding is not forthcoming, the budget will be thrown out of balance, and the Legislature and the Governor will be forced to make some tough choices. The longer we go without a decision from the federal government, the more difficult it will be to make cuts if they become necessary.
Since the health care law went into effect, more than 340,000 previously uninsured residents have signed up for coverage, a level of participation the state did not anticipate reaching until 2011. The problem is, the vast majority of enrollees are in subsidized plans, with nearly 75 percent of Commonwealth Care enrollees making no monthly premium payments.
For Fiscal 2008, the state had anticipated spending $618 million on Commonwealth Care, but that number recently increased to over $771 million due to a funding gap of $153.1 million. Only $869 million has been budgeted for Commonwealth Care in Fiscal 2009, but the true costs are anticipated to easily top $1 billion.
This is the legacy of health care reform: Nearly 95 percent of residents now have some form of coverage, but the vast majority of that coverage is subsidized and the state is quickly being burdened with rising costs, with no end in sight.
The Legislature hopes to soon finalize a health care cost containment bill championed by Senate President Therese Murray, who has been at the forefront of efforts to address this problem. But even with these cost-saving measures, the state still needs a commitment from the federal government for a renewed Medicaid waiver if the health care reform law is to have any chance of succeeding.
------------
"Mailing Error Left 16,000 Commonwealth Care Beneficiaries Unaware Of Coverage Cancellation, How To Appeal Decisions"
26 June, 2008
Massachusetts state officials on Monday said a mailing glitch last month left 16,000 residents without proper notice that they could lose their health coverage under Commonwealth Care and information about how to appeal the decision, the Boston Globe reports. The notices were mailed last week, about a month later than they should have been sent, according to the Globe. MassHealth, the state's Medicaid program, said it would cover out-of-pocket medical expenses incurred by beneficiaries who lost coverage as a result of the late notices. Commonwealth Care offers coverage to state residents whose incomes make them ineligible for MassHealth but who are unable to purchase private insurance. The Massachusetts Health Insurance Connector Authority administers Commonwealth Care, but MassHealth determines who is eligible for the program.
Of the 16,000 residents affected by the glitch, 1,000 had their coverage canceled because they did not contribute monthly premiums; 6,200 were eligible to enroll in health plans offered by employers; and 8,700 should have received health coverage from other sources. Dick Powers, a spokesperson for the Massachusetts Health Insurance Connector Authority, said, "These people should have received an initial notice telling them why they were ineligible for Commonwealth Care and a follow-up notice in a matter of days telling them how to appeal the decisions."
Residents whose coverage was terminated have 30 days to appeal the decision, and those whose coverage ends on June 30 are encouraged to submit their appeals as soon as possible, MassHealth CEO Philip Poley said.
"We are deeply concerned about the potential havoc that this bureaucratic error will have on thousands of Massachusetts citizens," Barbara Anthony, executive director of Health Law Advocates, said. Brian Rosman, research director of advocacy group Health Care for All, said, "We hope the state finds a way to provide retroactive coverage so people do not interrupt their medical care when they've been terminated through no fault of their own" (Krasner, Boston Globe, 6/24).
-
Reprinted with kind permission from http://www.kaisernetwork.org. You can view the entire Kaiser Daily Health Policy Report, search the archives, or sign up for email delivery at http://www.kaisernetwork.org/dailyreports/healthpolicy. The Kaiser Daily Health Policy Report is published for kaisernetwork.org, a free service of The Henry J. Kaiser Family Foundation.
-
Article URL: www.medicalnewstoday.com/articles/112836.php
-
Main News Category: Health Insurance / Medical Insurance
-
------------
-

-
Volume 358:2757-2760, June 26, 2008, Number 26.
-
"Health Care Reform in Massachusetts — Expanding Coverage, Escalating Costs"
By Robert Steinbrook, M.D.
-
http://content.nejm.org/cgi/content/full/358/26/2757
-

-
Growth in Health Insurance Coverage in Massachusetts after Health Care Reform.
Panel A shows the health insurance coverage among the 352,170 Massachusetts residents (5.5% of the 2007 state population of 6.4 million) who are newly insured. An estimated 550,000 to 715,000 residents (8.6 to 11.2%)1 were without health insurance before reform. Data for Commonwealth Care enrollees are from the Commonwealth Connector as of May 1, 2008. Medicaid data are from MassHealth as of February 29, 2008. Data for private insurance are from the Massachusetts Association of Health Plans, representing the increase in the number of people enrolled in commercial insurance between January 1, 2007, and January 1, 2008. New private-insurance enrollment includes coverage through Commonwealth Choice, an unsubsidized offering of approved private health plans that has been available through the Commonwealth Connector since July 2007; as of May 1, 2008, a total of 18,122 people had purchased insurance through Commonwealth Choice. Panels B and C show the numbers of residents enrolled in Commonwealth Care and Commonwealth Choice, respectively.
-
ARTICLE:
The far-reaching health care reforms that Massachusetts enacted in April 2006 are often cited as a model for other states.1 After 2 years, the good news is that the new programs have ramped up rapidly, the number of people without health insurance has been substantially reduced, and overall public and political support remains broad. Early data suggest that access to care has improved, especially among low-income adults; there have also been "reductions in out-of-pocket health care spending, problems paying medical bills, and medical debt."2 As of May 2008, about 350,000 residents — 5.5% of the state's population — were newly insured (see figure: ABOVE). About half of them are enrolled in Commonwealth Care, a subsidized insurance program for adults who have no access to employer-sponsored insurance, Medicare, Medicaid, or veterans' or student insurance programs and who earn no more than 300% of the federal poverty guidelines. About a third have purchased private insurance or gained employer-sponsored coverage, and the rest have enrolled in Medicaid. About 72% of the approximately 25,000 people with new individual policies have purchased them through Commonwealth Choice, an unsubsidized offering of private health plans approved by the Commonwealth Health Insurance Connector Authority, which administers many aspects of the reforms. In addition, the individual and small-group insurance markets have been merged, markedly reducing the cost of individual premiums.
Not all the news is good, however. Perhaps 5% of the state's population — the exact figure is a matter of conjecture and may be higher — is still uninsured, the financial burden of the reforms is increasing, and the challenges of sustaining the subsidized program have been exacerbated by the economic downturn. The features of plans that decrease the cost of premiums also increase out-of-pocket costs for those who obtain care. Although adults reported lower levels of health care needs that remained unmet because of cost in the fall of 2007 than in the previous year, those with low incomes reported increased difficulty in getting appointments or in finding a doctor or other provider who would see them.2 And the state ultimately decided that not all residents must actually carry health insurance, as the legislation originally intended: exemptions are available for adults who make too much money to enroll in the subsidized insurance program but are deemed unable to afford policies in the private market; others can be exempted on religious grounds or when unusual financial circumstances arise. If more residents were eligible for subsidized insurance, fewer would qualify for hardship exemptions, but such an approach would further increase the cost of the new programs. Already, enrollment in Commonwealth Care is growing faster than was projected. Annual state spending would be $1.08 billion for fiscal year 2009 if 255,000 residents are enrolled, an increase of about 80,000 enrollees from the current number.3 If 225,000 residents enroll, as an earlier estimate suggested, spending would be $869.4 million. By comparison, spending for Commonwealth Care was $132.9 million in fiscal year 2007 and is projected to be $647.4 million in fiscal year 2008. Moreover, as compared with the national average, the per-capita cost of medical care in Massachusetts is high.
"To maintain public and financial commitment to the new programs, controlling costs is 110% of the challenge for the next several years," according to Jon Kingsdale, executive director of the Commonwealth Connector. The monthly cost per member in the subsidized insurance program is $352.43, which is about what was budgeted and considerably less than the median cost of employer-sponsored coverage in the state. There are no monthly premiums for adults earning less than 150% of the federal poverty guidelines (in 2008, $15,612 for an individual and $31,812 for a family of four); premiums for those who earn 150 to 300% of the federal poverty guidelines are set according to a sliding scale, with a maximum premium for an individual of $105 a month. About 70% of those who have signed up pay no premiums. People who are eligible for Commonwealth Care are deemed to have access to affordable coverage; Medicaid covers the children of adults enrolled in Commonwealth Care.
The requirement to carry insurance is enforced through the state income-tax return. In general, the Massachusetts Department of Revenue uses the affordability schedule adopted by the Commonwealth Connector and other financial and insurance information to verify the self-reported information on tax returns and to determine eligibility for hardship exemptions. In 2008, the maximum penalty for not having insurance is $912. In 2007, it was $219. Revenue from this penalty is expected to be $8.5 million for fiscal year 2008.3
In June 2008, the Department of Revenue released preliminary data about the health insurance information reported on 2007 tax returns, covering 86% of the tax filings that are eventually expected. Of the taxpayers required to file insurance information, only 1.4% failed to comply. About 168,000 of 3.34 million adults (5.0%) reported that they did not have health insurance coverage at the end of the year. On the basis of the affordability schedule, about 97,000 were deemed "able to afford" insurance — 86,000 who paid the penalty and 11,000 who have appealed it. About 62,000 were deemed "unable to afford insurance" and are thus eligible for an exemption. In addition, about 9,000 taxpayers claimed a religious exemption, and about 200 had already obtained a "certificate of exemption," for financial reasons, from the Commonwealth Connector. About 10% of residents either do not file tax returns or are not accounted for as dependents on the returns of others, so the actual number without health insurance is probably higher.
As of January 1, 2009, people with health insurance must have plans that provide "minimum creditable coverage." Among other requirements, such plans must cover at least three doctor visits for an individual or six for a family before charging any deductible, and they must offer prescription-drug coverage (with a limit on any separate deductible of $250 for an individual and $500 for a family). However, annual deductibles (capped at $2,000 for an individual and $4,000 for a family) and out-of-pocket spending (capped at $5,000 for an individual and $10,000 for a family) can be very high.
In 2008, health insurance in Massachusetts is considered affordable — regardless of the premium — for individuals with incomes above $52,501, for couples with incomes above $82,501, and for families of any size with incomes above $110,001, according to the Commonwealth Connector. For people with lower incomes, the affordability schedule, which is revised annually, is used to determine whether residents can pay for health insurance, regardless of whether it is obtained through the Commonwealth Connector or directly from an insurer. According to the 2008 schedule, affordable policies typically require no more than 7.5% to 10.6% of income to be paid for premiums; the percentages vary according to income and type of household. People with preexisting medical conditions are not charged more for individual policies. However, because premiums increase with age, people with incomes below the affordability thresholds are considered to have no affordable private insurance options after a certain age — currently, 55 years for individual coverage, 50 years for couple coverage, and 30 years for family coverage. Income-based categorical exemptions apply mostly to adults who are not offered employer-sponsored insurance. Until a more detailed analysis of tax returns is completed, state officials will not know how many of the people deemed unable to afford health insurance fall into these categories. And, of course, people who use medical care have additional expenses for copayments, deductibles, prescription charges, and other out-of-pocket costs.
Premiums for the unsubsidized Commonwealth Choice program will increase by an average of 5% for fiscal 2009, which begins on July 1. Government payments for premiums in Commonwealth Care will increase by an average of 9.4%. The state's cost for Commonwealth Care is partially offset by federal reimbursement — projected to be at $268.3 million in fiscal year 2008 and for $360.6 million in fiscal year 20093 — and a decrease in payments to community health centers and hospitals that treat the uninsured, which has caused difficulties for some centers and hospitals. Other revenues are limited. Revenue from the "fair share contribution," an annual per-employee charge of $295 paid by businesses that have 11 or more full-time–equivalent employees but do not provide or contribute to health insurance, is projected to be $6.7 million in fiscal 2008, as compared with the $50 million per year that was estimated when the reform was enacted.1,3 The difference could reflect inaccurate or incomplete reporting or an inaccurate initial estimate of the number of employers that would be subject to the assessment. More people, including low-income adults, have employer-sponsored insurance than did before the reform.
Massachusetts has thus far avoided legal challenges to its reforms that might have been brought under the federal Employee Retirement Income Security Act, which prohibits states from setting plan standards for self-insured employers. Possible explanations are that the requirement for maintaining a minimum standard of coverage is placed on individuals rather than employers, that businesses largely support the reform,4 and that their obligations are modest. An employer's requirements are met if at least 25% of its workers enroll in the company health plan or if it offers to pay at least one third of the premium for individual coverage. Employers are not required to provide health insurance to part-time employees. So far, employers have blocked efforts to make them pay more of the costs of the reform.
Health care reform in Massachusetts is not a panacea for the many shortcomings of the health care system.5 It is worth remembering that California, for example, has more people without health insurance (6.7 million) than Massachusetts has residents (6.4 million) and that the financing and delivery of medical care have not changed.1 Having health insurance is not having health care.5 There are still many difficulties with access to primary care and other services. However, Massachusetts has made some strides, and given sufficient resources, more can be done. This includes identifying and reaching people who are still uninsured and helping them gain coverage, expanding employer-sponsored insurance, and improving the options for part-time employees, for low-paid workers who are offered insurance by their employers but who earn less than 300% of the federal poverty guideline and cannot afford it, and for others with hardship exemptions. The state legislature is considering new cost-control measures, and there is interest in a plan from Blue Cross–Blue Shield of Massachusetts, the largest carrier in the state, which pays doctors and hospitals according to a combination of capitation and pay-for-performance approaches. As a practical matter, the improvements in health insurance coverage can continue indefinitely as long as public and political support remain strong and the state is willing — with the substantial help of the federal government through the renewal of a Medicaid waiver agreement — to keep paying the ever-increasing bill.
-
"Source Information"
Dr. Steinbrook (rsteinbrook@attglobal.net) is a national correspondent for the Journal.
An interview with Jon Kingsdale can be heard at www.nejm.org.
-
References
1. Steinbrook R. Health care reform in Massachusetts -- a work in progress. N Engl J Med 2006;354:2095-2098. [Free Full Text: http://content.nejm.org/cgi/content/full/354/20/2095?ijkey=be18fa260ef44985876f72d0341bf16c915d8852&keytype2=tf_ipsecsha]
2. Long SK. On the road to universal coverage: impact of reform in Massachusetts at one year. Health Aff (Millwood) 2008;27:W270-W284.
3. The Commonwealth of Massachusetts. Information statement. April 16, 2008. (Accessed June 6, 2008, at http://www.dacbond.com/GetContent?dctm_r_object_id=0900bbc7800c82b4.)
4. Gabel JR, Whitmore H, Pickreign J. Report from Massachusetts: employers largely support health care reform, and few signs of crowd-out appear. Health Aff (Millwood) 2008;27:w13-w23. [Free Full Text]
5. Angell M. Health reform you shouldn't believe in. The American Prospect. April 21, 2008.
------------
The Boston Globe, Op-Ed, SUZANNE GORDON
"Nursing ratios save money and lives"
By Suzanne Gordon, July 9, 2008
BEFORE ITS legislative session ends in July, the Massachusetts Senate has an opportunity to protect hospital patients as well as the nurses who care for them by approving the Patient Safety Act that was passed overwhelmingly in the House a month ago.
The ratios bill would require that the Massachusetts Department of Public Health implement enforceable limits on the number of patients a registered nurse can be assigned, thus providing patient protection in all acute care hospitals. As the Senate debates this measure, it should consider the positive effects that legally mandated nurse-patient ratios have had where they've already been enacted - in California and Australia.
In California, since 2005, no nurse on medical surgical floors can be assigned more than five patients at a time. On equivalent units in Victoria - the second largest state in Australia - the minimum required staffing for every 20 patients is five RNs, backed up by a "charge nurse" who has no patient load of her own and is thus free to assist other RNs.
In both California and Victoria, ratios were originally introduced because excessive RN workloads were putting both nurses and patients in jeopardy, while adding to overall healthcare costs. More than 60 studies have documented that hospital understaffing results in more patient deaths, plus more preventable complications like pneumonia, urinary tract and catheter infections, and medication errors. A study done in 2005 by Michael B. Rothberg in the journal Medical Care put a price tag on these problems, concluding that a nurse who had time to prevent a case of pneumonia "saved $22,390 to $28,505, or $4,225 to $5,279 per additional hospital day." When nurses prevent an adverse drug event, they save the patient from an "added 2.2 hospital days at a cost of $3,344." On the other hand, if understaffing leads to complications after surgery, the resulting patient stay can be 8.1 days longer than normal, adding nearly $11,000 to the total expense.
Unmanageable workloads have also created an exodus of nurses into other fields or nonpatient-care jobs. According to a study by L.J. Hayes that appeared in the Journal of International Nursing Studies, hospital nurse turnover in 2006 - outside of California - ranged from 15 to 36 percent per year.
A study by economist Joanne Spetz, just published in the nursing journal Politics, Policy, & Nursing Practice, finds that ratios in California have increased RN job satisfaction and reduced turnover. According to Spetz, nurses are happier at work because they now get to spend more time at the bedside - particularly on patient education - which has a positive impact on nurse turnover and thus on the quality of care.
Researchers at the University of Pennsylvania have compared nurses in California with those in Pennsylvania and New Jersey - states without minimum staffing requirements. California RNs reported greater job satisfaction, leading to less burnout.
Ratio foes claim that ratios will cripple hospital functioning and force ERs to shutter their doors, because not enough RNs are available to meet the new requirements.
The hospital industry in California cited similar dire consequences in its bid to thwart full implementation of ratio legislation. In 2005, however, the state supreme court found no evidence that any hospital or ER there had closed due to new staffing mandates as opposed to the usual reasons for a shutdown (poor management, precarious finances, and consolidation of several nearby facilities).
Easing the nursing workload gives RNs who have dropped out of the active nursing workforce an incentive to return and encourages those already employed to stay. In Victoria, the government lured more than 7,000 inactive nurses back into the workforce. In California, nurses in hospitals that have fully complied with the new standards say ratios have had the same effect and many of those who reported they wanted to leave the profession say they will now stay.
Further legislative inaction on the issue of safe staffing in Massachusetts will only prolong an unacceptable status quo that drives nurses out of their profession, leaving too many hospital patients under-protected. If we want there to be enough nurses to care for the waves of baby boomers who will soon fill our hospitals, the time to act is now.
-
Suzanne Gordon is co-author of "Safety in Numbers: Nurse-to-Patient Ratios and the Future of Health Care."
-
------------
"Group warns Massachusetts state budget could spell financial doom"
Boston Business Journal - Boston Business Journal - Thursday, July 10, 2008 - 2:58 PM EDT
The Massachusetts Taxpayers Foundation wants Gov. Deval Patrick and State Legislators to cut hundreds of millions of dollars from the recently approved fiscal 2009 state budget to avoid what it said will be “an enormous threat” to state finances.
In an analysis released on Thursday, the MTF said it was worried the shortfall would affect Medicaid and ongoing efforts to expand health insurance coverage under the state’s new law mandating coverage.
According to the MTF, the budget is at least $1 billion out of balance, closed only through the use of the state’s stabilization reserves. But that money, the MTF warned, reduces those reserves almost by half.
Also a point of concern, according to the MTF, a potentially sharp drop in capital gains tax collections that amounted to nearly $2 billion in revenue for fiscal 2008.
Without the state stabilization funding, the MTF said that the Commonwealth Care subsidized insurance program is underfunded by $75 million and that MassHealth is behind $150 million.
------------
"Business balking at health changes: Many firms and insurers oppose $100m price tag; Public backs Patrick idea to close gap in funding"
By Kay Lazar, (Boston) Globe Staff, July 15, 2008
Governor Deval Patrick's proposal to ask businesses, insurers, and hospitals to kick in about $100 million to close a gap in funding for the state's landmark health insurance law is threatening to fracture the fragile coalition whose support was instrumental in passing the measure.
Business and insurance industry leaders are opposed to Patrick's plan, saying it is unfair to ask them to pay more, especially during an economic downturn. But consumer groups praised the proposal, saying patients were asked to pay more when copayments and deductibles for subsidized health plans were increased earlier this year. Now, they say, it is time for others to step up and pay their share.
Meanwhile, a new poll indicated there is broad public support for asking businesses and insurers to pay more to keep afloat the state's health insurance law, which seeks to cover almost all residents.
But a lobbyist with the state's largest business group said Patrick's proposal is likely to undermine key support for the two-year-old law, which passed only after more than a year of sensitive negotiations and compromises involving hospitals, insurers, employers, and con sumer groups.
"It was a real delicate balance that was achieved two years ago to bring everybody on board," said Rick Lord, president and chief executive of Associated Industries of Massachusetts, an association of business groups with 7,000 members.
"This jeopardizes the support of the business community, and that's one of the reasons reform has been so successful so far," he said. "Any reform that has been tried anywhere else - when the business community opposed it, reform has not been successful."
The law requires most employers to offer health coverage or to pay an annual penalty of $295 per worker. But a crucial compromise was struck to win the business community's support: companies would be in compliance even if a minority of their workers were covered. Employers with more than 10 workers had the option of paying at least 33 percent of workers' premiums within their first 90 days of employment or having at least 25 percent of their workers covered by an employer plan.
Patrick's proposal would raise $33 million in additional penalties by requiring employers to meet both requirements.
Lord said the proposal would hit retailers especially hard, because many of them face such high turnover that they do not typically offer health insurance to full-timers until after 90 days.
The governor announced the plan Sunday as part of a supplemental budget request, which must be voted on by the Legislature. In a letter to legislators, Patrick described the proposal as modest and as "companion contributions to those already made by consumers." House Speaker Salvatore F. DiMasi promised yesterday there will be a "full examination" of the proposal.
Patrick's plan would raise another $33 million from an assessment on insurance companies' reserve accounts. But Dr. Marylou Buyse, president and chief executive of the Massachusetts Association of Health Plans, said that the money is needed by the companies to cover catastrophic health costs in the event of a flu pandemic or a terrorist attack.
"This is taxing healthcare to pay for healthcare and is not solving the basic problem, which is healthcare costs too much," said Buyse, whose group represents most of the state's health insurers.
The state's largest private health insurer, Blue Cross Blue Shield of Massachusetts, hasn't taken any position on the proposal. A spokesman said the governor needs to release more details before the company could assess the full impact.
The state's hospitals are supporting the request for more money - $28 million from hospitals - with a caveat. Hospitals are willing to pay more to make near-universal healthcare work, said Lynn Nicholas, chief executive of the Massachusetts Hospital Association, but she tied the organization's support to the defeat of an unrelated measure pending in the Senate. That bill would set minimum nurse staffing requirements and require hospitals to hire more nurses.
The cost of Patrick's plan "pales in comparison to the prospect of having government-mandated nurse staffing ratios, which could cost in excess of $200 million a year," Nicholas said.
Most of the extra money from hospitals would go to a pool that covers hospital costs of residents who remain uninsured. Currently, the hospitals contribute $160 million to that fund.
Consumer groups are enthusiastically supporting Patrick's plan. "Consumers have already stepped up to the plate," said the Rev. Hurmon Hamilton, president of the Greater Boston Interfaith Organization, a consortium of religious and civic groups. "I would strongly urge the business community, insurance, and hospitals . . . to come forth and do their part."
Patrick also wants to plug the funding gap by shifting $35 million from the Medical Security Trust Fund, which is used to pay health insurance for the unemployed. Consumer groups were skeptical of that part of his plan.
"Unemployment is going up as the economy worsens, and we want to make sure there is enough money left to pay unemployment to people who are entitled to the money," said Brian Rosman, research director for Health Care for All.
Asking businesses and insurers to pay more toward healthcare is popular. A poll being released today by the Harvard School of Public Health and the Blue Cross Blue Shield of Massachusetts Foundation found that nearly three-quarters of those surveyed supported requiring businesses with more than 10 employees to pay more toward the system. And 61 percent said they favored requiring insurers to contribute more to a fund that would subsidize coverage. The poll of 1,015 Massachusetts adults was conducted June 10 to 23.
-
Kay Lazar can be reached at klazar@globe.com. Globe writer Eric Moskowitz contributed to this report.
-
------------
"Support for law varies, poll shows"
The Boston Globe, July 15, 2008
More than two-thirds of Massachusetts residents support the state's two-year-old, near-universal health insurance law, according to a new poll, but consumers most directly affected by the law are significantly less enthusiastic.
The survey by the Harvard School of Public Health and the Blue Cross Blue Shield of Massachusetts Foundation found that 69 percent of those polled backed the law, an increase from the 61 percent who said they favored it two years ago when it was first adopted.
Yet when pollsters asked the same question of residents who have bought health insurance or changed policies because of the law, support dropped to 52 percent.
The survey also found that increasing numbers of residents believe the law is hurting some groups that it was designed to help, such as the poor, uninsured, and small businesses.
For instance, the percentage of those who think the uninsured are being hurt by the new law nearly doubled from 17 percent last year to 33 percent this year.
Still, respondents do not want to abandon the landmark law. When asked whether it should be repealed, continued as is, or continued but with changes, 70 percent opted to continue, but with changes. The poll did not ask what changes should be made.
Survey author Robert Blendon, professor of health policy and political analysis at Harvard, said the findings show a sophisticated understanding of a complex law.
"They are basically saying it's better to have people covered, even though there are problems here," Blendon said. "People are aware there are costs to this thing, yet they still hang in because they think it's the right thing to do."
The poll also asked respondents how the state should cover a projected $150 million shortfall in the insurance program this year. The most popular options were to increase the tax on cigarettes (which the Legislature did last month) and penalize businesses with many part-time employees who are using state-subsidized care.
The least-popular ideas were to increase the sales tax or limit the number who could receive subsidized healthcare.
KAY LAZAR
------------
A Boston GLOBE EDITORIAL
"Patrick makes a tough choice"
July 15, 2008
THE GOOD news is that enrollment in the state's new subsidized health insurance program has greatly exceeded projections. The bad news is that this has raised the first-year cost of Commonwealth Care from an expected $472 million to $630 million. To fill the gap, the Patrick administration has devised a plan that spreads the pain relatively equally among health reform's major stakeholders, from providers to employers to insurers and the state itself.
The most important stakeholders - the individuals and families who have signed up for the state's pioneering effort at universal coverage - have already done their bit. In April, their premiums rose 10 percent and their co-payments also increased. The Legislature should approve the governor's proposal or come up with a better one before it adjourns at the end of this month.
Under the governor's plan, an employer would have to pay an annual assessment of $295 per uninsured worker unless it offers a health plan enrolling at least 25 percent of its workers and pays at least 33 percent of its employees' health premiums. Until now, employers have been able to avoid the assessment if they met either criterion. The state calculates this change would hike employer assessments by $33 million. Insurers would face a one-time assessment of $33 million, and providers would have to kick in $28 million. The state would draw up to $35 million from a surplus in a fund for health insurance for the unemployed.
If lawmakers do not act, the alternatives are sobering. The state could reduce spending for other programs or further increase charges to subscribers, putting coverage beyond the reach of some. Or it could cut off enrollment in Commonwealth Care. But this would not only leave consumers without access to affordable coverage, it would also probably make it impossible for the state to enforce the mandate on individuals to get insurance. Thanks to Commonwealth Care, the mandate, and other elements of the state's reform plan, a recent survey found that the percentage of uninsured in the state had fallen from 13 percent in the fall of 2006 to 7 percent last fall.
A poll released today by the Harvard School of Public Health and the Blue Cross Blue Shield of Massachusetts Foundation found strong public support for health reform and a 66 percent majority against capping enrollment in Commonwealth Care to limit its costs. To keep that backing, legislators should quickly find a way to pay for Commonwealth Care's success without gutting other state programs or putting an undue burden on the newly insured. The Patrick plan to achieve this is a good start.
------------
"Health plan's rising cost"
The Berkshire Eagle - Editorial
Wednesday, July 16, 2008
The state's innovative health care program met its first financial crisis in April and weathered it by raising premiums and co-payments for participants. Now the wolf is at the door again, and it is the business community that Governor Patrick wants to dig deep to help close a $100 million funding gap. In a sense the program is a victim of its own success, but it is more clearly the victim of flaws in our health care system that its architects failed to or couldn't steer clear of.
The admirable goal of the state-subsidized Commonwealth Care program is to provide insurance for everyone in the state, and it has done an impressive job of lowering the uninsured rate in Massachusetts to just 7 percent. Families at or below the poverty level are now getting health care. Predictably, however, costs have increased, and at an estimated $630 million, the program's first-year costs are now about $150 million higher than planned.
The governor wants to raise $33 million by subjecting businesses that don't meet requirements for insuring employees to penalties they were not subjected to when business leaders originally signed off on the plan. The state's hospitals will agree to pay an additional $28 million as requested but only if Beacon Hill agrees to abandon an unrelated bill requiring minimum nursing requirements. Blue Cross Blue Shield is pondering the governor's proposal that insurers pitch in more money. The governor wants to shift $35 million from health insurance for the unemployed, a risky idea in this dismal economic climate.
It's unfortunate that Commonwealth Care funding pits consumers and businesses and hospitals against one another when they are all in the same bind. But because the plan doesn't address the insurance companies at the center of our broken health system, that was the unfortunate and inevitable result.
------------
The Boston Globe, Op-Ed, JIM STERGIOS
"Doing the math on healthcare"
By Jim Stergios, July 22, 2008
ALMOST WITHOUT exception, policy makers find 1+1 = 2 an easier proposition to understand than 2-1 = 1. Just consider the ease with which earmarks are "sold" in the political marketplace and the difficulty of trying to stay focused on providing high-quality core services.
The politics of addition seem to be absorbed through the palms of politicians' hands during their swearing-in ceremonies. Democrats have their share of egregious examples, most notoriously the Clinton healthcare reform effort, with its cast of hundreds of policy makers and thousands of pages. But congressional Republicans have proven this is not a matter of party affiliation.
Here at home, there was the less memorable Romney climate change plan, with its litany of 73 "action items." When folks trumpet action items (and worse, the gross misuse of the English language "actionable items"), be prepared to be less than impressed with the results. They will collapse under their own weight and land in the inactive file.
Governor Patrick's readiness project is the latest in this line of policy-making, crafted by a cast of hundreds, with 24 action items, numerous other recommendations, and, ahem, no way to pay for any of it. Moreover, it was beyond even the governor's noteworthy oratorical ability to summarize it. He was wise to take three days to roll it out because, well, it took all of that.
There are complex pieces of legislation that start with an idea and are not premised on the politics of addition. The Education Reform Act of 1993 was conceptually simple: more money in exchange for high standards, accountability, and innovation.
The same was true for the Healthcare Reform Act of 2006. However complex, its basic proposition was unambiguous: shift subsidies away from institutions and toward healthcare consumers. That elegant formula was interesting enough to get left and right, federal, and state leaders on board.
We are already well into the new fiscal year, and negotiations with the federal government continue over whether it will renew the waiver that facilitated the Commonwealth's healthcare experiment in the first place. It might be useful to remember that no matter how conceptually interesting, even idea-based reforms face the logic of mathematics. They have to be affordable.
The Education Reform Act of 1993 required the grit of legislators and the governor to make good on the promised massive funding increase needed to make it viable. And now we must remain faithful to the idea of the Healthcare Reform Act, or the federal government will kill it.
The government wants reform, and it doesn't want it to affect federal coffers. Reform is happening; we have successfully signed up hundreds of thousands who were previously uninsured. One has to assume that the reduction in the number of people showing up to emergency rooms without insurance is translating into less of a burden on hospitals, especially those that previously provided care to a disproportionate share of the uninsured - specifically Boston Medical Center and Cambridge Health Alliance.
To remain cost-neutral to the federal government, we have to address this year's shortfall of $153 million and a minimum shortfall of $184 million next year. In the long term, there are several things we can do to contain healthcare costs, including perhaps a hard look at certain benefits mandated in the law and increasing the transparency of cost and quality data useful to consumers.
But there is really only one way to address the costs of the legislation in the immediate term: reduce the level of extra payments to Boston Medical Center and Cambridge Health Alliance, which were granted special annual payments that began at $200 million and ratchet down by $20 million a year. These special institutional payments were meant to ease the hospitals into the new regime. They were also very much a political deal.
However important Boston Medical Center and Cambridge Health Alliance are, they must play by the same rules as other hospitals and must not put the entire reform at risk. It is no doubt true that hospitals like Bay State Medical in Springfield, among others, face the same challenges. And there is a larger reason: the whole point of the healthcare reform was to focus on people. So let's do that.
-
Jim Stergios is executive director of Pioneer Institute.
-
------------
The Boston Globe, Op-Ed, ALAN SAGER AND DEBORAH SOCOLAR
"Make doctors agents of health cost controls"
By Alan Sager and Deborah Socolar, July 21, 2008
THE STATE'S new healthcare law was the best law that could be passed, and has proven a blessing to more than 350,000 newly insured people, though a similar number remains uninsured.
Often, however, the law that can pass can't work as enacted. This law's individual mandate requires big public subsidies to make insurance affordable. It sharply boosts Medicaid payments to hospitals. It has no controls on healthcare costs. It redistributes modest sums previously used to help vulnerable people instead of squeezing out waste to finance care for all.
The law's proponents underestimated costs and overestimated revenue. Redeeming the law's promises has therefore obliged the state to spend more to subsidize insurance. This obligation imposes unsustainable financial and political stresses amid a growing budget deficit. Many health reform advocates therefore now declare cost controls crucial to the law's survival.
But what is crucial here has been unattainable throughout the United States. Since the 1970s, virtually all cost controls - using market competition or government regulation - have failed. And powerful caregivers still seek more money for business as usual.
Current cost control proposals - like publicizing hospital prices, adopting electronic medical records, or promoting prevention - will do little to cut costs. That's why they are politically feasible: they don't upset insurers or hospitals, doctors, other caregivers, and drug makers. The state isn't even canceling unwarranted Medicaid rate hikes that help the richest hospitals most.
Not yet able to lower underlying costs of healthcare, the state will seek new revenue. Methods include recent hikes in premiums and co-payments for families, higher cigarette taxes, proposed new payments by insurers, providers, and employers, and more federal Medicaid dollars. These steps may preserve the law's gains and buy time for fundamental cost containment, but not much time. Rising health costs may crash through the windshield of a stalled economy.
Today, US health costs per person are double those in other wealthy nations that cover everyone and live longer.
In Massachusetts, health spending this year will reach $10,500 per person, one-third above the US average. Today's spending is easily enough to finance medical security for all. But to make this promise real requires addressing the three main reasons for past controls' failure.
First, half of all spending is wasted and most cost controls have ignored central causes of waste. Clinical waste stems largely from caregivers' financial incentives to over-treat, defensive medicine, and lack of evidence on what care works. Waste also includes excess prices, theft, and paperwork, which is imposed partly by complexity but mainly by deep mistrust between payers and doctors or hospitals.
Second, hospitals, doctors, other caregivers, and drug makers have become increasingly specialized and uncoordinated, and their political power defeats efforts to cut their revenue.
Third, doctors' decisions essentially control almost 90 percent of health care spending. That's why shifting costs to patients can't work. Yet cost controls have ignored, marginalized, or sought to manipulate doctors instead of working with them.
Given doctors' power and their unique ability to squeeze out waste, the challenge is to put our healthcare dollars in their hands under conditions that verifiably let us trust them to spend it well. That entails dramatic but carefully coordinated bottom-up reforms in how care is given and financed. Microregulated pay-for-performance or a few more dollars for care management won't work.
Only by persuading doctors to be fiduciaries, not entrepreneurs, can we craft healthcare that is self-regulating, covers everyone, extirpates waste, and spends only what's affordable. This requires a financial, legal, and clinical peace treaty between payers and doctors. Different ways to do this should be tested quickly.
One approach: We urge development of small clusters of primary care doctors and other professionals that live within budgets, accepting capitation payments calibrated to patients' health. Raising primary care doctors' incomes by half would sharply increase their supply and their time to listen to patients and coordinate care.
Payment-related paperwork will be slashed. Doctors could not gain financially by giving unnecessary care - or by withholding needed care. Savings will be recycled to expand coverage and benefits and fulfill the promise of the state's reform law.
-
Alan Sager and Deborah Socolar direct the Health Reform Program at the Boston University School of Public Health.
------------
"Coalition fights fee plan for insurers: Urges alternative of mandatory managed care"
By Kay Lazar, (Boston) Globe Staff, July 24, 2008
A coalition of business and insurance groups is vigorously lobbying lawmakers against Governor Deval Patrick's plan to collect millions of dollars from them to help close a $130 million gap this year in funding of the state's landmark health insurance law.
The coalition is pushing an alternative that would require all Massachusetts Medicaid patients to join managed care plans, which try to achieve savings in part by restricting patients' choice of providers and services. The coalition says mandatory managed care would save the state $160 million this fiscal year and between $690 million and $1 billion by 2013.
The proposal for placing all patients in managed care plans was originally advanced in December in a report commissioned by the four health plans that now serve about 400,000 of the 1.1 million people in the state's Medicaid program, also known as MassHealth.
"There is potentially hundreds of millions of dollars in savings in this plan, and I have been perplexed as to why the administration has backed away from doing this in the midst of saying there is a shortfall in healthcare," said Michael Widmer, president of the Massachusetts Taxpayers Foundation, a business-funded public policy group.
Last night, the Patrick administration disputed the contention that the managed care proposal would save money. A statement from the Executive Office of Health and Human Services said its analysis showed that the plan would be more expensive than the current program. The managed care plans "have served the healthiest members of MassHealth and have not yet demonstrated the capacity to serve large numbers of disabled members," the statement said.
The issue is expected to come to a head in the coming days when lawmakers vote on the governor's supplemental budget request, which includes his plan to keep the health insurance law afloat.
Widmer's group is among the two-dozen that sent a strongly worded letter yesterday to House Speaker Salvatore F. DiMasi and Senate President Therese Murray, urging them to reject the governor's financial bailout plan.
"With the Commonwealth facing a bleak fiscal reality and employers and consumers struggling with rising healthcare costs, the governor's proposal is the wrong approach," the letter states, adding that the governor should be focusing on ways to control healthcare costs.
Patrick's proposal would tap an additional $28 million from hospitals this year and $66 million more from employers and insurance companies to finance the near-universal health insurance law.
He said earlier this month that consumers were already asked to pay more this year in higher health insurance premiums and copayments, and that it is only fair to ask other members of the coalition that originally supported the state's two-year-old law to contribute more, too.
The state pays the Medicaid managed care plans a fixed monthly fee per patient, and these plans in turn typically pay physicians and other providers in their networks lower rates than they would receive from other health plans.
Requiring thousands of Medicaid recipients to enroll in managed care, however, may not be a popular idea, especially among those who are disabled, said Brian Rosman, research director of Health Care for All, a consumer group.
"The current plan gives choices to consumers," Rosman said. "Particularly, people who are disabled really need a health structure that focuses on their needs, and a lot of disabled people we know pick the [other plans] because of the freedom from strict constraints."
He also questioned whether such a massive overhaul of the Medicaid system could be done quickly enough to raise the $130 million the governor said is needed this year to cover a funding shortfall.
The December report by the health plans pointed out that a number of other states have retooled their Medicaid programs to require most of their residents to enroll in managed care plans. It concluded that a similar shift in Massachusetts could help persuade federal officials that the state is pursuing cost controls.
That is one factor the federal government is considering as it decides, probably by early next week, whether it should continue to pay the state hundreds of millions of dollars per year to help fund its insurance experiment.
In the statement last night, the Patrick administration pointed to $340 million in MassHealth savings that are contained in the budget for the fiscal year that started July 1.
On Beacon Hill, spokesmen for House and Senate leaders said they are reviewing the coalition's letter and proposal.
"As we move forward with quality and cost-control measures, we remain open to all ideas that could improve the Commonwealth's healthcare system and help ensure the success of healthcare reform," said David Falcone, the Senate president's spokesman.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Insurers to cover drugstore clinic visits: Copayments to be lower than for hospital ER care; CVS, Walgreens may become major providers"
By Jeffrey Krasner, (Boston) Globe Staff, July 24, 2008
Some of the state's largest health insurers say they will cover visits to the retail health clinics expected to open in CVS and Walgreens drugstores later this year, making the clinics attractive options for the treatment of everyday ailments.
Harvard Pilgrim Health Care and Tufts Health Plan have signed contracts with CVS Caremark, the Woonsocket, R.I., company that operates more than 6,000 pharmacies nationwide. The chain plans to open as many as 28 MinuteClinics in its Massachusetts stores this year and 100 statewide within five years. CVS also is negotiating coverage for clinic services with Blue Cross and Blue Shield of Massachusetts, the state's largest insurer. Together, the insurers have nearly 5 million members.
The endorsement by insurers is likely to turn retail clinics into major healthcare providers in the state because, for many patients, they will be less expensive than hospital emergency rooms, with less waiting time. Under the contracts signed and being negotiated, retail clinic copayments range from $10 to $25, compared with the $50 to $150 copays most insurers assess for emergency room care.
In addition to its talks with CVS, Blue Cross-Blue Shield is negotiating with Take Care Health Systems, the medical clinic subsidiary of Walgreen Co. of Deerfield, Ill., which plans to open in-store clinics in Massachusetts this fall. Tufts Health Plan is considering extending coverage for the Take Care clinics, as well, and Fallon Community Health Plan said it is negotiating to give its members coverage for retail clinic care, but didn't specify at which clinics.
"We have already contracted with some insurers and are in final stages of discussions with others," said Carolyn Castel, a spokeswoman for CVS Caremark. "We see all of these negotiations moving positively."
Retail clinics in Massachusetts will feature weekend and evening hours. Services will include vaccinations and treatment of common ailments such as ear infections, poison ivy, and minor burns. Without insurance, prices range from $59 to $69 at CVS's MinuteClinics, and from $59 to $74 at Walgreen clinics.
Major insurers provide coverage for treatment at MinuteClinics in all 25 states where they operate, according to CVS.
The state's powerful physicians' group, the Massachusetts Medical Society, opposed the clinics when they were proposed by CVS last year, saying they raised concerns about safety, oversight of caregivers, and spread of germs. Dr. Bruce Auerbach, president of the medical society, said yesterday the physicians organization still believes patients are "best served" by doctors in primary care practices, which provide "comprehensive care that is continuous and not fragmented."
Boston Mayor Thomas M. Menino has decried the notion of retailers profiting from illness and said clinics would "jeopardize patient safety."
But despite the medical establishment's objections, the state Public Health Council in January approved the MinuteClinic plan, saying expanding access to healthcare outweighed concerns about patients using the clinics as a substitute for an ongoing relationship with a physician.The oversight and safety issues raised by the medical society have been addressed by new state regulations that govern how the clinics are run.
Dr. Neil Minkoff, Harvard Pilgrim's medical director of network medical management, said the need for the retail clinics is especially intense in Massachusetts, where there is a shortage of primary care physicians.
"We're helping our members get access into a medical system and reduce inappropriate use of the hospital emergency room," he said. "We believe that contracting with MinuteClinic will allow for some reasonably simple, high-volume care to occur in this different setting. Right now, this stuff is unnecessarily clogging up emergency rooms."
Minkoff added, "What's really driving this is that the cost of care performed in a retail setting is significantly lower than when it is done in an emergency room."
Paul Dreyer, director of healthcare safety and quality at the Department of Public Health, said he expects licenses for the clinics to be granted in the fall.
While the clinics could ease crowding at hospital emergency rooms, a significant shift of patients away from emergency rooms could also hurt community hospitals that are strapped for cash and depend on steady revenue from emergency visits.
Lynn Nicholas, chief executive of the Massachusetts Hospital Association, said she still supports the retail clinics.
"Given the shortage of access to primary care, this can only be a good thing in the long run," Nicholas said.
CVS now operates about 500 MinuteClinics. The closest ones are in Connecticut. Walgreen has 189 Take Care clinics in 14 states. The clinics proposed by both chains for Massachusetts are typically staffed by nurse practitioners, registered nurses with advanced degrees who are trained to diagnose and treat common conditions and perform many of the same functions as physicians. The nurses can prescribe medications for the uncomplicated ailments treated at the clinics. If they detect more serious conditions - such as heart attacks - the patients are sent to a doctor or emergency room. Nurse practitioners also will have telephone access to doctors who can provide immediate advice.
"We want to make sure our members get access to simple care when they need it in the evening and on weekends," said Dr. Allen Hinkle, chief medical officer for Tufts Health Plan. "We'll save money, and the member saves money because the copayment for an emergency room visit is much higher."
Hinkle said Tufts has reviewed the track record of retail clinics in Minnesota, where they have been long established, and was satisfied that patients sought care at clinics for the proper type of ailments.
Lauren Tierney, a spokeswoman for Take Care Health System, said its clinics help ease some of the burden on primary care physicians by treating simpler cases. In addition, she said,
Take Care nurses and consulting doctors have contacts in the communities they serve and can refer patients to primary care physicians who have room in their practices for additional patients.
"About 30 percent of the patients we see don't have a primary care physician," she said. "Our goal is to connect them with the system."
-
Stephen Smith of the (Boston) Globe staff contributed to this report.
&
Jeffrey Krasner can be reached at krasner@globe.com.
-
------------
"Hospital payments central to federal health care negotiations"
By Kyle Cheney/State House News Service
Wednesday, Jul 23, 2008, www.wickedlocal.com/cambridge/news, Cambridge, Massachusetts -
Annual state government payments to two Boston-area teaching hospitals are increasingly at the epicenter of a local and national firestorm over the affordability of Massachusetts's health insurance access laws.
Cited by some as a potentially ruinous drain on funds for health care reform and defended by others as critical support to care for the poor, the payments to Boston Medical Center and Cambridge Health Alliance are a major point of contention between Massachusetts and the Bush administration as they negotiate over hundreds of millions of dollars in federal funds for state health care programs.
Calls for the state to end such payments are growing - the right-leaning Pioneer Institute head Jim Stergios called for their elimination in a Tuesday Boston Globe op-ed - with some fiscal watchers convinced that powerful political support from figures such as Sen. Edward Kennedy and Mayor Thomas Menino are keeping them intact.
In fiscal 2009, the payments will reach $160 million, the second year of a scheduled phase-out of such payments, laid out in the state's Chapter 58 health care reform law of 2006.
But to some observers, the phase-out can't come quickly enough.
"We need to be on an aggressive schedule to eliminate those special payments," said Michael Widmer, president of the Massachusetts Taxpayers Foundation. "Politically, it's a very powerful institution with powerful backers. I'm sure it's a thorn in the side of waiver negotiations."
Widmer said redirecting those payments toward other health care costs would eliminate the need to raise new revenue. Massachusetts implemented a $1-per-pack cigarette tax at the beginning of July in an effort to offset rising costs for Commonwealth Care, the taxpayer subsidized health care program for low-income residents. That program insures more than 170,000 residents, many who pay no premiums but were uninsured prior to the 2006 implementation of health care reform. Gov. Deval Patrick this month also offered new plans to raise $130 million in assessments on insurers, providers and employers.
Greg D'Angelo, a researcher for the conservative Heritage Foundation, noted that the state and federal governments already reimburse BMC and Cambridge Health for services provided, not to mention the two organizations were given near-exclusive access to sign up uninsured residents as health care reform and insurance access laws were implemented.
"They got a pretty good deal," he said, arguing the additional lump sum payments simply amounted to "sustaining their revenues."
"They're both getting paid to enroll people in health insurance and provide services to that same population. They were double-dipping," he continued. "If there are budgetary challenges, this is low-hanging fruit."
But supporters of the payments contend they are necessary to ensure that the two institutions can continue to provide high-quality care to the neediest Massachusetts residents.
"I have and will always support the mission of Boston Medical Center," said Mayor Thomas Menino in a statement emailed by his office. "When children, elderly, low income families, and underserved patients are sick, they know that Boston Medical Center will provide quality care, regardless of their ability to pay. In return, BMC needs the support of the City and the state to continue to fulfill its mission."
U.S. Sen. John Kerry registered his support for the payments, telling the News Service in a statement issued through his spokeswoman saying "While we work to ensure that as many individuals as possible get private insurance, we will not sit idly by if a hospital faces financial ruin."
"If the payments are reduced to BMC and Cambridge Health Alliance, the likely consequences are reductions in services to people who are vulnerable," said Alan Sager, a professor of health care policy at Boston University.
Sager said those who advocate for rapidly eliminating the payments are "thinking more in theoretical terms than in real world terms." He described their argument as, "'Let's just move the money around without examining the consequences.'"
Asked how the state should respond to the federal government's emphasis on eliminating the special payments, Sager said, "If someone has a gun to your head, it's important to listen to them. That doesn't mean it's right."
Sager said that the state should propose to reduce Medicaid reimbursement rates to wealthy hospitals such as Massachusetts General Hospital. Those rates went up dramatically under the Chapter 58 reform law.
Boston Medical Center defended its payments, noting that, in addition to being the largest Massachusetts hospital of its kind, half of its patients earn less than $22,000 a year.
"Recognizing its uniqueness and central role in providing health care to the low income and underserved, as well as wanting to ensure that access to services for these patients continued without interruption, the Commonwealth made commitments to its two major safety net hospitals at the inception of the program," Boston Medical Center officials wrote in a statement issued in response to a News Service inquiry.
Similarly, Cambridge Health Alliance cited its role in helping insure thousands of low-income residents.
"We are doing our part and believe we demonstrate the value of our highly public mission in our daily work providing medical and mental health care to the needy and most vulnerable among us - including a growing number of patient care visits under health reform," said Doug Bailey, a spokesman for the hospital.
With the divergent viewpoints about the payments, the Patrick administration is seeking to find a middle ground.
"Safety net hospitals pay a critical role in our health care system," said Jennifer Kritz, a spokeswoman for the state Executive Office of Health and Human Services. "What we're working on now is striking a balance between supporting safety net hospitals while keeping our commitment to transitioning from institutional payments to coverage for individuals."
The payments to BMC and Cambridge Health, approved in the fiscal year 2009 budget signed last week by Gov. Deval Patrick, were among the drivers behind the state's ambitious health care reform law. In 2005, the federal government refused to continue funding payments directed at the two institutions as they grew and thrived. Rather than forfeit federal funds for the hospitals, the state pledged in 2005 to redirect those payments to insure low-income residents.
But when Gov. Mitt Romney signed the state's 2006 health care reform act into law, rather than eliminate the payments, it put them on a phase-out schedule, starting at $200 million in fiscal 2007 and declining by $20 million for each of the next three years.
Now, federal negotiators are weighing their level of continued support for Massachusetts health care programs, with the hospital payments at the center of the debate as talks drag on between the Patrick and Bush administrations. Negotiations on a three-year federal waiver involving hundreds of millions of dollars in Medicaid funds for Massachusetts were set to expire on July first but state officials received two two-week extensions, moving the deadline to July 28.
Officials are reluctant to discuss the substance of the negotiations, but sources familiar with talks have told the News Service that another central issue in negotiations is the speed with which Massachusetts reduces spending on so-called free care for the uninsured. Draws on a pool used to reimburse providers of care to the uninsured have dropped significantly since the advent of health care reform, but some observers question whether it has been a precipitous enough decline.
Negotiations on the federal side have been largely controlled by President Bush's Office of Management and Budget, which has tightened its grip on federal coffers in the waning days of the Bush administration. State officials, including Gov. Deval Patrick, have met with OMB leaders as well as federal Medicaid officials but still contend there are myriad issues to work through.
If the state fails to receive funds it is requesting, it could find itself hundreds of millions of dollars out of balance, clouding the future of health care reform efforts and putting pressure on officials to cut other areas of state spending.
The hospital payments became the subject of dueling blog entries this month between Sen. John Kerry and the Heritage Foundation, as well as a post from Beth Israel Deaconess Medical Center CEO Paul Levy.
An unsigned July 11 entry on Sen. John Kerry's campaign blog blasted the Heritage Foundation for caring more about "profit margins" than "health care for sick people." In a Monday response on the Heritage Foundation blog, D'Angelo compared federal support for Massachusetts to proposed bailouts for embattled Freddie Mae and Fannie Mac.
Levy, on his blog called Running a Hospital, criticized Jim Stergios's Tuesday Globe op-ed, equating it to prior "attacks" on BMC and Cambridge Health Alliance. In a comment on Levy's blog, Brian Rosman, research director of consumer group Health Care for All, pointed to the 1,450 large companies in Massachusetts that fail to insure upward of 50 employees, arguing that they should be asked to help pay for increasing expenses.
------------
(A Boston) GLOBE EDITORIAL
"Checks on the state's to-do list"
August 6, 2008
VOTERS ARE said to like divided government, with one party heading the executive branch while another controls the Legislature. This is supposed to provide checks and balances, but just as often it can result in gridlock. The session just completed shows that much can be accomplished when the two branches work together - provided everyone agrees to share the credit.
Deval Patrick was the first Democrat elected governor in 16 years, but the Democratic Legislature did not march in lockstep behind all his policy proposals. The defeat of casino gambling and criminal justice reform, stalled property tax relief, and $122 million in budget vetoes are proof of that.
Rather, Patrick, legislative leaders, and especially their staffs did the unsexy policy work needed to cobble together strategies for the big issues facing states today. The result: A $1 billion life sciences initiative; a sweeping energy bill with a focus on conservation and renewables; a $3 billion bond to accelerate repairs on deteriorating roads and bridges; $500 million in new revenues; an intact health reform law with 340,000 new patients enrolled in insurance plans. "Green" causes fared particularly well, with the biggest environmental bond bill ever, and commitments to carbon reduction and open-space preservation.
Personality clashes sometimes substituted for ideological differences, however. The governor got off to a rocky start with the House Speaker Salvatore DiMasi and Senate President Therese Murray, themselves fairly new to the job. But in an interview yesterday Patrick said, "we play the long game." Over time, the three focused on getting to yes.
Some in the business community have complained of rising costs in these initiatives, pointing to tax loophole closings, new environmental regulations, and increased contributions to the healthcare law. But Patrick was scrupulous about seating business representatives at the table while the big changes were hammered out, to the benefit of corporate interests. For example, the tax loophole closings and cigarette tax hike were partly offset by an overall reduction in the corporate tax rate.
Plus, as the state GOP likes to boast, taxes were cut more than 40 times by four successive Republican administrations. Given plunging revenues and the press of healthcare and other needs, the fairly modest tax hikes are more a course correction than a radical shift.
Former Governor Weld, who started the 16-year run of Republicans in the corner office, liked to say that government should "steer, not row." But this past session suggests what is possible when most oars are pulling in the same direction.
------------
"Fourth delay in care plan sought: US balks at hike proposed in yearly Medicaid funding"
By Kay Lazar, (Boston) Globe Staff, August 9, 2008
Federal regulators are balking at the state's proposal to increase Medicaid spending by up to $1 billion a year over the next three years, and this and other sticking points prompted Massachusetts yesterday to request another two-week extension of its healthcare funding package.
The federal payments, which are crucial for keeping the state's landmark health insurance law afloat, were set to expire June 30, but the state has received three extensions, and a fourth would postpone the deadline for reaching an agreement until Aug. 25.
At stake in the negotiations between state and federal officials is more than $11 billion in federal funds over three years, money earmarked for dozens of healthcare programs in Massachusetts in addition to the state's crown jewel: its two-year-old near-universal health coverage law that has provided insurance to more than 350,000 residents.
Medicaid is a state and federally funded program that provides healthcare assistance to low income people. Over the past decade, Massachusetts has been granted waivers from Medicaid rules to expand assistance to residents who wouldn't otherwise be eligible for coverage.
Federal rules require that the expanded coverage not cost more than would have been spent without the waivers, and the figure itself is one area of disagreement, according to a key legislator and other people familiar with the talks.
"If we don't get everything we are looking for in the waiver, we would either have to come up with the money through [state] reserves, or we would have to cut benefits," said Senator Steven Panagiotakos, chairman of the Senate Ways and Means Committee.
Panagiotakos, who has been regularly briefed by the administration of Governor Deval Patrick, declined to discuss specifics but said state negotiators seemed cautiously optimistic about the progress of the discussions. But he said that the two sides are still in disagreement over funding for several key programs in the massive spending blueprint, and that if Massachusetts did not get what it requested for any one of those programs, it could have a large impact on the state budget.
Several others familiar with the talks said that the state is pushing for higher spending because it expects at least 50,000 more residents to sign up in the next year for Commonwealth Care, a subsidized health insurance program for lower-income residents ineligible for Medicaid.
The higher-than anticipated enrollment in Commonwealth Care has stretched state funds, and the dispute with federal regulators comes at a time when Massachusetts has little wiggle room, with a tight budget and declining revenues.
Yet the state's Medicaid proposal for the next three years shows a growth in spending each year that is roughly double what it had been in years past.
Another critical point of disagreement between state and federal negotiators, people familiar with the talks say, is the way Massachusetts has counted the number of children enrolled in MassHealth, the name of the Massachusetts Medicaid program. They said federal regulators believe the state has, for years, incorrectly listed many children under MassHealth when they should have been counted under a program called the State Children's Health Insurance Program, which is not funded by Medicaid.
The difference made it appear that Massachusetts had a much larger number of children in MassHealth, and that made the state eligible for more federal reimbursement in its Medicaid program.
The Patrick administration has declined to discuss details of the sensitive negotiations. But late Wednesday, a federal government spokeswoman released a statement that indicated the talks were nearing completion.
"The US Department of Health and Human Services has extended an offer to the State that is faithful to the intent of the original . . . Medicaid [waiver]," said the written statement from Christina Pearson, agency spokeswoman.
"The offer continues HHS' commitment to the shared principles of health care reform under the (Medicaid waiver) program and maintains its support for the Commonwealth as the State continues to be an innovator in this endeavor," the statement continued.
But Patrick administration officials denied that any offer had been extended. Shortly after that, Pearson backed off the statement that an offer had been extended.
"There is not a formal offer on the table," Pearson said in an e-mail on Thursday. "What we did provide recently was more feedback, specifics, and ideas on how to proceed. Since it is an ongoing dialogue, we will not have further comment on our discussions."
-
Kay Lazar can be reached at klazar@globe.com.
-
www.boston.com/news/local/articles/2008/08/09/fourth_delay_in_care_plan_sought/
-
------------
-

-
MORE DOCTORS NEEDED The law, based on a plan pushed by Senate President Therese Murray, seeks to increase the number of primary-care doctors.
-
"Leaders nip, tuck healthcare policy: Limits enacted on drug firm gifts"
By Scott Allen, (Boston) Globe Staff, August 11, 2008
Governor Deval Patrick yesterday signed into law one of the nation's strictest limits on gifts given to medical professionals by drug salespeople, the most contentious measure contained in a broad package intended to improve healthcare safety and curb skyrocketing costs.
The new law also provides $25 million to promote electronic medical record-keeping in doctors' offices, requires the state university to graduate more primary care doctors, and gives regulators the power to hold hearings when health insurers want to raise premiums.
Critics of the pharmaceutical industry had hoped to ban gift-giving altogether, arguing that the drug company largesse interferes with doctors' judgment in deciding which drugs to prescribe. But the bill that the Legislature sent the governor bans only certain types of gifts such as sports tickets and free travel, and requires that pharmaceutical and medical device-making firms publicly disclose gifts worth more than $50.
"The good news is that it prevents some of the most abusive gift-giving," said Senator Mark Montigny, a New Bedford Democrat who has pushed for years to ban gift-giving. "If I didn't feel that it was beyond a half a loaf of victory, I would not have signed on."
The changes come amid intense focus on the cost and quality of healthcare, which consumes one in every six dollars spent in Massachusetts. Two years ago, landmark legislation required almost everyone in the Commonwealth to have insurance. But the law has been so successful - prompting an estimated 345,000 people statewide to obtain insurance - that it has been far more expensive than expected, forcing Patrick to sign a bill last week raising more than $100 million in state funds and fees on private companies to help foot the bill.
Patrick's Human Services Secretary JudyAnn Bigby said that while universal health insurance is an important goal, the current system is lacking if everyone cannot get access to quality care, or premiums and out-of-pocket costs become too costly for patients.
"We have to make sure that people have access to high quality care and that we are being efficient in the way we pay for that care and that we are paying for the right things," Bigby said in an interview. The law Patrick signed yesterday "puts the challenge to those of us who have to implement it to do more planning."
The new law, based on legislation championed by Senate President Therese Murray of Plymouth, contains several initiatives intended to increase the number of primary-care doctors, who make the initial decisions as to how patients will be cared for. Although Massachusetts has the most primary-care doctors per capita in the country, Bigby said there is evidence that there aren't enough to handle the workload, especially as the number of people covered by insurance swells.
In response, the law directs the University of Massachusetts Medical School in Worcester to increase class size so that it can graduate more primary care doctors, Bigby said. In addition, the law calls for better training of primary care doctors and aids some of them in repaying medical school loans.
The law also establishes an institute to award grants to doctors and hospitals seeking to increase their use of computer technology. Electronic medical records systems typically cost $30,000 or more, which has slowed the healthcare industry's adoption of technology that most people agree improves both safety and efficiency.
In addition, the law gives the state more oversight of health insurance rates than regulators have had in more than a decade. Now, both the Division of Insurance and an office under Bigby's control can require health insurers to publicly justify rate increases.
But the limits on drug industry gift-giving drew the most attention.
Montigny had hoped that, after failing twice, he might succeed in banning gift-giving between salespeople and healthcare professionals altogether. However, representatives of the drug and medical device industry successfully argued that the measure went too far, potentially banning money paid to doctors and hospitals to conduct medical research. Though the Senate passed the full ban, the House backed only restrictions.
Still, the limits in the law put Massachusetts at the forefront of states in cracking down on the use of financial incentives to persuade doctors to prescribe particular drugs or medical devices. In addition to banning some gifts and requiring disclosure of others, it calls for the state to develop a code of conduct for industry representatives that includes a $5,000 fine for each violation.
"I commend the governor for standing firmly on the side of the patient and the taxpayer," said Montigny.
But the pharmaceutical industry's trade group, called PhRMA, said state leaders could one day regret the limits, especially the public disclosure of gifts. The group said in a statement that researchers could be discouraged from doing important drug research if they fear their research grant will be put on a public list of gifts from industry.
"Governor Patrick's decision to sign [the limit on gift-giving] is deeply disappointing - and very likely damaging for medical partnerships, clinical research, and patients in Massachusetts," said PhRMA senior vice president Ken Johnson.
-
www.boston.com/news/local/articles/2008/08/11/leaders_nip_tuck_healthcare_policy/
-
------------
"Businesses rip healthcare proposal: Trade group declares higher costs will lead to dropped coverage"
By Kay Lazar, (Boston) Globe Staff, August 12, 2008
Businesses are balking at a proposed state regulation that, a leading retail group says, will force small companies to spend thousand of dollars more in health insurance for their workers, and could lead many employers to drop coverage altogether.
Proposed rules, issued yesterday by Governor Deval Patrick's administration, are intended to help close a gap in funding the landmark healthcare law.
The regulations, if adopted, would take effect Oct. 1, and raise about $45 million this fiscal year, according to documents made public yesterday. A public hearing is scheduled for Sept. 5.
Current law requires most employers with more than 10 full-time equivalent employees to offer health coverage or to pay an annual "fair share" penalty of $295 per worker. It gives companies an option of paying at least 33 percent of full-time workers' premiums within the first 90 days of employment or making sure that at least 25 percent of their full-time workers are covered by an employer plan.
But the new regulations would require employers to meet both requirements, or pay the penalty.
"I think there is going to be a revolt over this," said Jon Hurst, president of the Retailers Association of Massachusetts, a trade group with 3,000 members. "This is tough economic times, and I don't think they fully understand how many small businesses are going to be hit hard by this."
Hurst said hundreds of seasonal businesses, especially on Cape Cod, would be hurt, because the proposed changes would also require reporting workers' health coverage on a quarterly basis, instead of annually, prompting more paperwork. He predicted many small retailers would find it cheaper to just drop health coverage and pay the annual fine instead.
The new proposal comes just two weeks after lawmakers approved a supplemental funding request by the governor to raise about $100 million for the healthcare law. That package added an assessment on health insurance companies' reserve accounts, required additional payments from hospitals, and shifted money from the Medical Security Trust Fund, which is used to pay health insurance for the unemployed.
Rick Lord, president and chief executive of Associated Industries of Massachusetts, said employers are already paying more than their fair share to fund the state's near-universal health system - an additional $500 million a year to cover 85,000 more workers since the new healthcare law went into effect. He said members of his organization, the state's largest business trade group, would lobby the Patrick administration against the proposed changes.
But Health Care for All, one of the state's largest consumer groups, applauded the proposals. Brian Rosman, the group's research director, said consumers were required this year to pay higher premiums and deductibles to help cover the funding shortfall.
"We think this implements the shared responsibility concept that was the hallmark of healthcare reform," he said. "It makes sense to us to say to companies that offer minimal or no benefits, 'You have to make a small contribution.' "
When the healthcare law was signed two years ago, the Legislature estimated the "fair share" penalty on businesses would bring in $45 million in the first year and $36 million in the fiscal year that just ended. But the state collected no payments the first year, and state officials said employers made penalty payments of only about $7 million in the past year.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
-

-
"Dental benefits widen, waiting lines grow: Some balk at giving care, call subsidized rates too low"
By Kay Lazar, (Boston) Globe Staff, August 7, 2008
Two years into the state's bold healthcare experiment, its early success in expanding dental coverage may be threatened by a shortage of dentists willing to treat newly insured patients.
Since getting free or subsidized dental coverage in 2006, more than 200,000 low-income adults have climbed into Massachusetts dentists' chairs for work on their long-neglected teeth. But increasing numbers of patients are expected to seek care, and advocates fear the wait for appointments, now three months at community health center clinics, will grow.
The problem is that just 17 percent of dentists statewide have been willing to see these newly insured patients, despite reforms intended to boost their ranks. Even some of these dentists are limiting the number of state-subsidized patients they will treat.
Dentists say the state's reimbursement rate for adults covers only about half their costs, and they also cite payment delays and burdensome paperwork.
Without more dentists, said Kerin O'Toole, spokeswoman for the Massachusetts League of Community Health Centers, patients will not be able to get timely preventive care and "we risk treating people with more expensive and serious health issues."
As part of the healthcare law's goal of extending insurance to nearly everyone, dental benefits were restored to roughly 540,000 low-income adults who had lost nearly all dental coverage under Medicaid budget cuts in 2002. The law also expanded eligibility, prompting another 140,000 to sign up through Medicaid or the newly created Commonwealth Care subsidized program for the previously uninsured.
Suddenly, thousands of patients who had not opened wide in years were calling for appointments, and the number of Medicaid patients who saw a dentist more than doubled in the first full year, from about 15 percent of adults to 35 percent, state data show.
Among the newly insured is Pam Anasoulis, a 48-year-old telemarketer from Beverly who has also wired helicopter engines and fixed conveyor belts to make ends meet. For her, entree to the dentist after years of oral neglect was bittersweet. The mother of two grown children, she had broken a front tooth in 2004 and had gone to a dentist who filed down several of her front teeth to make a temporary bridge.
But Anasoulis said she couldn't afford health insurance and could not afford to go back to have the work completed. The bridge broke, decay set in, and Anasoulis was left with stubs for front teeth.
"You really don't think, when you look at someone with missing teeth, how much they're hurting inside," she said. "I got so depressed I didn't go out."
When she finally found her way to the Lynn Community Health Center dental clinic in 2006, many of Anasoulis's front teeth had to be extracted. But Dr. Herlivi Linares, the clinic director, was able to save some of her teeth and make her a partial denture.
Thanks to insurance, Anasoulis got her smile back.
Healthcare advocates expect that thousands more patients will, like Anasoulis, seek care in coming months as community health centers and other groups launch education programs about the need for regular preventive care for children and adults. They say that the one-third of Medicaid patients who saw a dentist in the past year is substantially less than the rate for adults statewide. By the federal government's counting, about three-quarters of all Massachusetts adults go to the dentist at least once a year.
"People who have been chronically uninsured may not understand the nature of primary and preventive medical and oral healthcare, simply because they have never had an ongoing relationship with a physician or dentist," said O'Toole, of the Community Health Centers group.
As part of the healthcare law, the state changed a rule to encourage dentists to treat at least some patients covered by Commonwealth Care or its Medicaid program, called MassHealth. The old rules mandated that dentists who accepted even one subsidized patient had to accept all such patients. Now, the state allows dentists to limit the number of poor patients they accept. That has helped increase the number of practicing dentists who are willing to see poor patients from about 10 percent to 17 percent, according to a Globe analysis of public records.
Of that 17 percent, one in five have already closed their doors to new subsidized patients, said Dr. Catherine Hayes, a professor at Tufts University School of Dental Medicine.
"We need dentists to understand there have been significant improvements in the program," said Hayes, who is also a court-appointed monitor of the state's dental program for children.
But the state's reimbursement rate for treating adults remains at only about 50 percent of what private insurers typically pay, despite small increases in both 2006 and 2007. Dentists contend that makes it financially unfeasible for them to accept many subsidized adults. (Rates for children are more generous, because of a 2005 federal court ruling requiring improved dental care for poor children in Massachusetts.)
"With children, I think the reimbursement is pretty fair now, but the adult fee is still very poor," said Michael Wasserman, a Pittsfield dentist who treats some subsidized patients. "I think if a dentist is going to treat these patients he or she should not be forced to lose money."
Dentists say that in addition to low reimbursements, they are still encountering mountains of paperwork to join the program and delays in getting paid. Jennifer Kritz, spokeswoman for the state Executive Office of Health and Human Services, said the agency is trying to ease the claims and enrollment process, but cannot currently pay dentists higher rates.
The Massachusetts Dental Society has been urging members to join, saying it is the responsible thing to do. But it's been slow going. "It has gotten a little better," said Karen Rafeld, assistant executive director of the dental society, "but it's still a bureaucratic nightmare."
For Dr. Barry Aston, a dentist with offices in Watertown and Hudson, accepting subsidized patients has been a mixed blessing. He signed up about a year ago and was so swamped that he stopped accepting additional needy patients 10 months later. Today, about 40 percent of his caseload is Medicaid or Commonwealth Care.
"I am making more money, but it's a nightmare for my administrative staff," he said. His aides often spend substantial time on the phone with Doral Dental, the company that manages the state's subsidized dental program, to track down lost paperwork.
The dental society's Rafeld said that until the state works out more of the bugs and raises the rates, persuading more dentists to join will be a hard sell. "It comes to a point when you throw up your hands," she said. "People thought instantaneously it would be solved. But it's a process."
-
Kay Lazar can be reached at klazar@globe.com.
-
-----
WIDENING ACCESS TO ORAL HEALTHCARE
The Boston Globe - Letters
"The problem is a broken system"
August 12, 2008
WE APPLAUD the Globe for bringing to light the many obstacles faced by those trying to access oral healthcare in Massachusetts ("Dental benefits widen, waiting lines grow," Page A1, Aug. 7, 2008).
While it is true that a lack of dentists participating in the MassHealth program is one factor, there are many others, not the least of which is the system itself. What business could possibly survive by spending an inordinate amount of time on administrative paperwork just to serve a certain segment of customers, and then lose money on each person they finally get to see?
The Massachusetts Dental Society has made great progress in recruiting more of our members to participate in MassHealth. In fact, we've doubled the number in the last 18 months. But we know that more needs to be done.
The problems in providing access to care are both chronic and systemic, dating back for decades. And the solutions won't be achieved overnight. By the dental profession and the state working together, we will be able to meet the growing demand of all those seeking high-quality oral healthcare.
MILTON A. GLICKSMAN
Southborough, Massachusetts
The writer is president of the Massachusetts Dental Society.
-----
WIDENING ACCESS TO ORAL HEALTHCARE
The Boston Globe - Letters
"Don't forget care for poor children"
August 12, 2008
THE GLOBE'S coverage of the dental crisis in Massachusetts among low-income adults was excellent ("Dental benefits widen, waiting lines grow," Page A1, Aug. 7), but there is another part of the story: a lack of dental care for poor children.
Like the adults profiled in the story, children from low-income families are also less likely than affluent children to receive adequate dental care, and the problem is exacerbated by private caregivers who decline to offer treatment for kids receiving Medicaid assistance. Nationwide, fewer than 20 percent of dentists treat Medicaid kids.
As an educator and pediatric dentist, I have seen first-hand the impact of poor dental health among younger patients. Chronic tooth decay in young children can lead to a variety of other health and developmental challenges including pain, poor nutrition, distraction from learning, and other activities.
Raising Medicaid reimbursement rates is a good first step toward increasing access to care, but it doesn't address issues on the patient side of the equation.
Much more needs to be done to educate parents about dental disease. Effective treatment for the nation's poorest patients will require innovative approaches from the dental community, policy makers, social workers, and others involved in the dental care of children and adults alike.
DR. STEVEN ADAIR
Nashville
The writer is chief dental officer of FORBA Dental Management, which manages dental clinics in Massachusetts for children whose families receive Medicaid.
-----
The Boston Globe - Letters
"Money is the key to early dental care"
August 15, 2008
ONCE AGAIN, poverty is equated with healthcare ignorance. In "Don't forget care for poor children" (Letters, Aug. 12), Dr. Steven Adair, writes, "Much more needs to be done to educate parents about dental disease. Effective treatment for the nation's poorest patients will require innovative approaches from the dental community, policy makers, social workers, and others involved in the dental care of children and adults alike."
Adair is assuming that poor parents do not know their children need dental care early in their lives. Being uninformed is not the problem. The issue, as he states earlier, is the lack of financial conviction by private dental practitioners and state and local government alike.
What would be "innovative" is if those in the middle and upper classes stopped claiming unawareness among the poor as the issue. Have they never heard of "genteel poverty?" The issue is money.
DEBORAH SAN GABRIEL
Lynn, Massachusetts
-----
WIDENING ACCESS TO ORAL HEALTHCARE
The Boston Globe - Letters
"Early prevention can save lives"
August 12, 2008
KAY LAZAR'S story ("Dental benefits widen, waiting lines grow," Page A1, Aug. 7) shines an important spotlight on a situation that has long needed attention. Thousands of Massachusetts residents do not have access to the oral healthcare they need to remain healthy, productive members of our society. To solve this problem, we must take a prevention-oriented approach to changing the systems we currently have in place. Expanded dentist participation in MassHealth must be coupled with increased access to oral health education and care.
The widespread nature of dental disease in children and adults is a solvable public health concern. Dental decay is an infection that can inhibit learning, speech and eating and, left untreated, can lead to pain and serious health problems, including heart disease and diabetes. Fortunately, when communities have access to the oral healthcare they need, we can almost entirely prevent this disease. The key to this effort is to start early.
No one group can accomplish this alone. We must act together and ensure that all residents have access to the preventive services and treatment so vital to overall health.
FRANK ROBINSON
Springfield, Massachusetts
The writer is chairman of the Oral Health Advocacy Taskforce.
------------
"Rate hikes help boost Partners' profit 25%: Healthcare group increases salaries for key executives"
By Jeffrey Krasner, (Boston) Globe Staff, August 15, 2008
Partners HealthCare System yesterday reported a third-quarter profit from its hospitals of $54 million, 25 percent more than in the same period last year, driven by wider margins, rate hikes, and an increase in high-paying, complex cases.
But the healthcare giant's profits from nonoperating activities - principally investments - dropped significantly. During the third quarter last year, Partners' Massachusetts General Hospital received a onetime royalty payment of $206 million, pushing nonoperating profits to $250 million. For the third quarter this year, which ended June 30, nonoperating profits were $64 million.
Overall, surplus of revenues was $118 million for the quarter compared with $293 million in the same period last year.
The nonprofit system, made up of Mass. General, Brigham and Women's Hospital, and an array of community and specialty hospitals and other entities, said it lost $167 million from treatment of Medicare and Medicaid patients, because government payments don't cover the full cost of treatment, and from insufficient state reimbursement for the care of uninsured patients.
Also, several key Partners executives received substantial raises last year, according to statements filed with the state yesterday. Dr. Peter Slavin, president of Mass. General, earned $1.17 million in salary, deferred compensation and benefits in the year that ended Sept. 30, an 11.6 percent increase from the previous year. Dr. Gary Gottlieb, president of Brigham and Women's, earned $1.19 million, including salary, deferred compensation and benefits, an increase of nearly 16 percent.
Partners officials said salaries for senior executives at smaller hospitals in the Boston area have risen substantially, making it necessary to give the heads of two of the largest academic medical centers in Boston raises "to ensure that compensation is appropriate relative to smaller hospitals in the region."
The increase is intended to retain the "physician leaders" and keep them from being recruited to other parts of the country, Partners said.
Dr. James Mongan, chief executive of Partners, earned $2 million, an increase of about 3 percent.
The system's top earner was Dr. Lawrence H. Cohn, a cardiac surgeon at Brigham and Women's, who earned $3.1 million in fiscal 2007. The figure includes about $2.4 million in deferred compensation - money earned in earlier years that isn't paid out, but is invested, an arrangement available to many high wage earners that provides tax benefits and other advantages. Including the deferred compensation, Cohn's annual compensation increased nearly fourfold from the previous year.
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
------------
JON B. HURST, The Boston Globe, Op-Ed, August 18, 2008
"Small businesses pay for plan's shortcomings"
By Jon B. Hurst
'No good deed goes unpunished." This phrase passed over the lips of many small businesses owners in Massachusetts last week, as the Patrick administration moved to increase penalties on small businesses in its effort to raise money to fund the state's healthcare law.
Why increase penalties on small businesses? This move would be explainable if they had not embraced reform and not offered their employees affordable, reliable healthcare options. But in reality, they have done both.
When the law was crafted, the proponents estimated that the state would collect $45 million in the first year and $36 million this year in penalties from business that refuse to offer healthcare to their employees. Instead, businesses overwhelmingly embraced the law and offered healthcare benefits to their employees. So the state collected no payments in the first year and only $7 million this year.
The result is that we find ourselves with a great success story on access and coverage. The law has delivered in expanding coverage - a very good thing.
So why punish the small business owner by changing the rules when she's been doing everything that has been asked of her? Doing so is completely unfair. Should the administration's change be implemented, fewer businesses, not more businesses, will offer their employees health benefits.
The proposed change is a disaster waiting to happen. Current law requires employers of 11 or more full time equivalent employees to offer health benefits or pay a penalty of $295 per worker. To avoid paying the penalty, businesses must cover 33 percent of the cost of the premiums or have 25 percent of their full-time workers enrolled in their company's plan. The new policy simply changes that "or" to an "and." But the consequences are enormous.
Many small employers - including stores, restaurants, services, tourism entities, and nonprofit organizations - have work forces composed of retirees (on Medicare) and secondary wage earners (on parents' or spouses' plans). So it is very difficult for them to achieve a 25 percent participation rate because their employees are covered elsewhere. But by meeting the requirement to pay 33 percent of premiums, they can avoid paying a penalty. The new policy makes it almost impossible for those business to avoid paying the penalty - for reasons that are completely out of their control.
These small business owners are frustrated for another reason: The law has had no impact on the endless increases in annual premiums for those buying health insurance. Family health insurance policies for small businesses with little bargaining power cost as much as $23,000 today. Those rates are unaffordable. There is no indication that relief is in sight.
The difficult truth is that small businesses pay far more for the same coverage than do big purchasers, thus creating a disproportionate funding of the healthcare system by smaller businesses than by large companies or by government payers. Unfortunately, group purchasing discounts are available for public employers but are prohibited for small businesses. The state's Commonweath Connector still hasn't delivered on the promise of low-cost small business plans, focusing to date only on taxpayer-subsidized plans for individuals.
Add to that the effects of the soft economy, pessimistic consumers, the highest electricity rates in the continental United States, and current gasoline, fuel oil and food prices, and it is easy to see why many small businesses are struggling in Massachusetts.
Barely staying in the black, they get frustrated when they're told that "employers are not doing their fair share." So now, rather than steps being taken to ease their health care costs and mandates, they are now looking at a far greater likelihood of state imposed health care tax assessments on top of the growing premiums.
For those affected, the consequences will range from dropping their offer of coverage altogether and just paying the tax, to discriminating in the hiring process, to giving up and closing their doors.
In the real world, government mandates can determine winners and losers in the competitive marketplace. The Patrick administration's proposal will do exactly that. The result will be small business losses, diminished support for healthcare reform in the business community, fewer jobs for our citizens, and fewer offers of health insurance by small employers.
-
Jon B. Hurst is president of the Retailers Association of Massachusetts.
-
------------
-

-
"439,000 more get health coverage: State shows big gains in landmark program"
By Kay Lazar, (Boston) Globe Staff, August 20, 2008
Nearly three-quarters of previously uninsured Massachusetts residents now have medical coverage under the state's landmark campaign to extend health insurance to virtually all Bay Staters, according to a report released yesterday by Governor Deval Patrick's administration.
Since the program's launch in June 2006, 439,000 more people have enrolled in health insurance, and nearly half of them signed up for private insurance not funded by taxpayers, says the report from the Division of Health Care Finance and Policy. Before 2006, studies had estimated that about 600,000 Massachusetts residents lacked health insurance.
The dramatic expansion has spurred a substantial drop in patients seeking routine care in hospital emergency rooms, where treatment is much more expensive. The reduction is already saving the state millions of dollars, the quarterly report said.
In the past two years, Massachusetts has embarked on a closely watched experiment to become the first state requiring virtually all residents to have health insurance. The figures released yesterday provide some of the most compelling evidence so far that the experiment is working.
"This shows a cultural shift in public attitude, where people understand that as a community, by everyone getting health insurance, we are improving the health of everybody," said Brian Rosman, research director of Health Care for All, one of the state's largest consumer groups.
Still, the economics of the ambitious campaign remains uncertain. Massachusetts is locked in delicate negotiations with federal authorities to determine if the state will continue getting billions of dollars in special assistance to help make the experiment work.
Dr. JudyAnn Bigby, the state's secretary of Health and Human Services, said that the latest enrollment figures should bolster the state's case with the federal government.
"It shows them that it's a good model for Massachusetts," Bigby said in an interview. "The intent of healthcare reform was that if people were getting coverage," then the number of patients relying on the state and hospitals to pick up the tab for their care would decline, she said.
That appears to be happening. For example, from July through September 2007, the most recent period for which data is available, the number of visits to hospitals and community health centers by the uninsured declined by 37 percent, compared with the same period a year earlier, the report said. That drop translated to a $68 million savings in the pool of money the state sets aside to cover the uninsured.
Massachusetts has requested more than $11 billion in federal support during the next three years to pay for dozens of healthcare programs, including its crown jewel, its nearly universal health coverage system. The federal payments, which are crucial to keeping the landmark program afloat, were set to expire June 30, but the state has received four extensions. The deadline for reaching an agreement with the Centers for Medicare & Medicaid Services is now Monday.
Bigby said that during negotiations, federal regulators have asked for data to determine whether the number of uninsured was declining. They have also wanted to see whether employers were dropping coverage and dumping employees on the state's subsidized system, she said.
The new report debunks those fears. In fact, a substantial share of the newly uninsured are opting for private coverage that does not cost the state money. Nearly half of the newly insured are enrolled in private health insurance and the largest group, 159,000 people, signed up for employer-sponsored health coverage from June 2006 through March 2008, the report said.
"That 159,000 is almost twice what was projected. It translates into almost $1 billion more spent by employers on premiums," said Michael Widmer, president of the Massachusetts Taxpayers Foundation, a business-funded public policy group.
The business community has been sparring with the Patrick administration over proposed state regulations intended to help close a gap in funding the healthcare law. Those rules, scheduled to take effect Oct. 1, would raise about $45 million this fiscal year.
The rules would require businesses with 11 or more full-time employees to pay at least one-third of full-time workers' premiums and make sure that at least 25 percent of their full-time workers are covered by an employer plan. Employers who fail to meet this requirement face an annual penalty of $295 per worker.
Widmer said the new report, showing that 159,000 residents have gained insurance through their employers "makes a mockery of the state's allegation that employers have not done their fair share."
In the final months of 2007, state officials and healthcare advocates launched an advertising blitz, reminding residents that the law now required nearly everyone to have insurance or face a $219 tax penalty. Data released by the state yesterday indicate that the ad campaign paid off: More people signed up in the second half of 2007 than in any other six-month period since the healthcare law took effect.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Opening wider for oral health"
Editorial - Posted by The (Springfield) Republican, August 18, 2008
There's something to smile about - and frown about - on the dental health care front in Massachusetts.
Worth a smile is the news that since free or subsidized dental coverage became available in 2006, more than 200,000 low-income adults have paid a visit to the dentist - many of them for the first time in years. Deserving a frown, however, is the fact that the system can't handle the influx of patients.
While thousands of patients have found their way to the dentist's chair, there are thousands more who are calling for appointments. The average waiting time is about three months and the lag between making the call and seeing the dentist is expected to get even longer.
There just aren't enough dentists willing to see the newly insured patients. Despite efforts to enroll more dentists in the program, just 17 percent are participating. Those shunning the program cite as their reasons what has become a familiar refrain among health care providers: low reimbursement rates, burdensome paperwork and bureaucratic delays.
The state's reimbursement rate for treating adults is about half of what private insurers typically pay. And while rates for children are more generous because of a federal court ruling requiring better dental health care for poor children, there's still some bridge work needed before the system is working as it should. Good childhood dental care translates into lower costs down the road.
In a letter to The Boston Globe, Milton A. Glicksman, president of the Massachusetts Dental Society, said the organization has made progress in recruiting more of its members to participate in MassHealth - doubling the number of participants in the last 18 months. But, he added, "What business could possibly survive by spending an inordinate amount of time on administrative paperwork just to serve a certain segment of customers, and then lose money on each person they see?"
Therein lies the problem. The commonwealth's effort to improve access to dental health care is admirable, but much more needs to be done before Bay State officials can break out in a big smile.
------------
The Boston Globe - Letters
"Many employers not doing fair share for health reform"
August 23, 2008
MASSACHUSETTS HEALTH reform has been successful thanks to the confluence of the interests of businesses, healthcare providers, insurers, government, and consumers who together have borne additional costs, allowing Massachusetts to reduce the number of uninsured by more than 439,000.
Jon Hurst, president of the Retailers Association of Massachusetts, claims that the recent changes in the Fair Share regulations put an unfair burden on small businesses ("Small businesses pay for plan's shortcomings," Op-ed, Aug. 18). Hurst is correct that most businesses are doing their part to support health reform and offer their employees healthcare coverage, and they should be commended. However, many employers are not doing their fair share.
Business revenues to the state under the Fair Share assessment were expected to be $171 million in the first three years. Instead, after about a year and a half, they are less than $15 million. Governor Patrick's plan to refine the definition of "fair and reasonable" contributions by businesses, resulting in additional business contributions next year, is still much lower than the original estimates that the business community signed on to in agreeing to support health reform. All stakeholders are being required to make additional payments, respecting the original concept of shared responsibility.
PHILIP J. EDMUNDSON
Boston, Massachusetts
The writer is chairman and CEO of William Gallagher Associates, a Boston-based insurance brokerage firm, and is chairman of Massachusetts Affordable Care Today, a coalition of healthcare providers, insurers, business, and consumer groups.
------------
"Errors leave some without insurance: State's complex system blamed"
By Kay Lazar, (Boston) Globe Staff, August 23, 2008
Tens of thousands of people insured under the state's universal healthcare system have had their coverage terminated since the start of the year, state enrollment figures show. In some cases, patients were terminated because of mistakes they made themselves and in other cases because of errors by the state.
The state figures, however, do not show how many of the people later re-enrolled, nor do they track how many were wrongfully terminated. But lawyers and community advocates said they have seen a "steady stream" of enrollees whose insurance was unilaterally canceled by the state through no fault of their own. State regulators acknowledge that some have been mistakenly cut from the system but put the number at fewer than 100.
The terminations reflect growing pains in the state's first-in-the-nation law requiring virtually every resident to have coverage. Earlier this week, the state reported that since the law's launch in 2006, nearly three-quarters of previously uninsured Bay Staters had gained medical coverage; roughly half are covered under private health plans.
But about 173,000 of the newly insured are enrolled in Commonwealth Care, which is insurance for people who don't qualify for employer-sponsored health coverage and earn too much to qualify for Medicaid. Those enrollees must renew their insurance annually and must also report to the state every time they change jobs.
The state's eligibility documents are complex, advocates said, leading some patients to have their insurance terminated - even though they are eligible for coverage - because they made mistakes filling out the forms. Mail sent by the state to the wrong address is also cited as another reason coverage is dropped.
In other instances, the state misinterprets information on the forms and mistakenly bounces people out of the program, advocates said.
Patients terminated by the state can unknowingly rack up thousands of dollars in medical bills only to discover that those expenses will not be reimbursed. The only way they can get the money back is to sue the state.
"We get a steady stream of people who were erroneously dropped," said Barbara Anthony, executive director of Health Law Advocates, a nonprofit that has sued the state on behalf of some Commonwealth Care members who were mistakenly terminated. Health Law Advocates did not have exact figures.
"This is an issue of fairness," she said. "I think there would be a huge outcry by state government if a private insurance plan behaved that way."
Melissa Boudreault, director of Commonwealth Care, estimated there have been fewer than 100 wrongful terminations brought to the attention of the Commonwealth Health Insurance Connector board, the state agency that regulates Commonwealth Care.
"If we are made aware of an instance where medical debt was incurred, or someone needs to see a doctor, we work on a case-by-case basis to resolve those issues," Boudreault said. "We are really trying to get this right."
Boudreault said that state regulators are aiming by January to overhaul the massive computer system that runs Commonwealth Care and the state's Medicaid program, known as MassHealth. That upgrade, Boudreault said, should ease the wrongful termination issue and allow the state to reimburse those whose coverage was erroneously canceled.
Consumers caught in the middle said the experience can be maddening and expensive.
"It's confusing and frustrating, and who's got the time to deal with this?" said Elizabeth, a 55-year-old part-time midwife in Springfield who signed up for Commonwealth Care in January. Elizabeth asked that her full name not be used because she does not want her family to know she is receiving subsidized healthcare.
Elizabeth is not eligible for insurance at the hospital where she works because she is part-time, but the hospital agreed to deduct monthly premiums from her paycheck and send it to Commonwealth Care. Unbeknownst to Elizabeth, though, her employer was getting the premium bill on the day it was due, so even though the bill was being paid, Elizabeth was marked as delinquent.
So Elizabeth said she was bumped from coverage for four months. Although she continued to pay her $400 monthly premiums, Elizabeth said, her insurance card was rejected when she went to the drug store to pick up allergy medication. The pharmacy billed her the full $125 each month.
Maritza Smidy, the office manager at the hospital where Elizabeth works, helped sort through the mess.
"I would consider myself a fairly educated person," Smidy said, "and I got confused."
A prime source of confusion, Smidy and others say, is that consumers are directed to the Connector Authority to sign up for Commonwealth Care and for questions about the insurance. But they must work with a separate state agency, MassHealth, to prove they are eligible and for yearly renewals.
Leaders of two of the health insurance companies that cover most of the Commonwealth Care customers, BMC HealthNet and Network Health, say members frequently seem to be terminated by the state and then re-enrolled several months later.
"The paperwork is complicated material from the state," said John Cragin, a top BMC HealthNet executive.
Jennifer Kritz, a spokeswoman for MassHealth, said the state is refining its mailing system. But she said that because a significant number of Commonwealth Care members fail to notify the state when they move, her agency is trying to work with advocates to come up with a reminder system. Kritz said the state also is developing a more easily understood document to simplify the annual renewal process.
"MassHealth is keenly aware of this issue and has a shared interest with members, providers and advocates to prevent disenrollments whenever possible," Kritz wrote in an e-mail.
------------
Massachusetts Health Law
"Massachusetts tops in health insurance coverage"
Posted by Gideon Gil, August 26, 2008, 11:27 AM
By Stephen Smith, (Boston) Globe Staff
Massachusetts has the lowest percentage of residents without health insurance in the nation, according to a US Census Bureau report released this morning that provides evidence that the state's bold experiment to insure nearly everyone is succeeding.
Averaging data from 2006 and 2007, the study found that 7.9 percent of Bay Staters did not have health insurance. From 2004 through 2005, the rate was 10.3 percent.
By comparison, one-quarter of residents lacked health insurance in Texas, the state that fared worst. Nationally, about 15 percent of Americans were uninsured in the 2006-07 period.
The Census report likely understates the effect of the law in Massachusetts requiring virtually every resident to be insured because the law did not go into effect until June 2006 and penalties for not enrolling did not kick in until the end of 2007.
------------
"Census: Mass. has lowest rate of uninsured in U.S.", 08/27/2008,
By: AP Wire Service, (Capital News 9, Ryan Burgess has the details).
BOSTON (AP) - A new U.S. Census Bureau survey shows Massachusetts has the lowest rate of uninsured residents in the country.
The average uninsured rate dropped from about 10 percent in 2004-2005, when it was seventh lowest in the U.S., to about 8 percent in 2006-2007
The drop coincides with the launch of the state's new universal health care law, which expands free government programs but also requires subsidized or private coverage for workers who can afford it.
Some 444,000 people have added health insurance since the program was launched in June 2006. More people signed up for insurance than expected, adding $130 million in costs that will be covered by insurance companies, health care providers and businesses.
A spokesman for Gov. Deval Patrick issued a statement Tuesday saying the findings were "another indication of the tremendous success of health care reform."
------------
"State could be sued, healthcare giant warns: Fears proposed rules will face federal action"
By Kay Lazar, (Boston) Globe Staff, September 6, 2008
Partners HealthCare, the state's largest private employer, is warning that Massachusetts may face a federal lawsuit if it proceeds with plans to raise the amount some companies must contribute to their workers' health insurance.
The proposed new rules, designed to help close a $130 million gap in the state's pioneering healthcare law, are opposed by several trade groups because, they say, businesses are already contributing millions more under the new law and the regulations would hit smaller firms especially hard.
Partners was one of dozens of business and consumer groups that testified yesterday at a public hearing on the issue. The healthcare giant's testimony stood out because it has long been a prime supporter of Massachusetts' landmark law.
Partners' vice president for community health, Matt Fishman, said he was concerned that if the regulations were adopted, it would prompt a federal court ruling that would throw out a key portion of the state's healthcare law.
"That would say to the nation that Massachusetts' health reform law is perhaps not as successful as many thought, even though the coverage numbers are so strong," Fishman later said in an interview.
He also said Partners does not object to the changes because of its potential impact on the healthcare chain, which includes Massachusetts General Hospital and Brigham and Women's Hospital. Rather, Fishman said Partners is concerned that a successful lawsuit would undermine the substantial progress the state has made.
The current law requires most employers with more than 10 full-time employees to offer health coverage or to pay an annual "fair share" penalty of $295 per worker. It gives companies an option of paying at least 33 percent of full-time workers' premiums within the first 90 days of employment or making sure that at least 25 percent of their full-time workers are covered by an employer plan.
But the proposed new regulations would require employers to meet both requirements, or pay the penalty. The rules, if adopted, would take effect Oct. 1 and raise about $45 million this fiscal year, according to state documents.
Courts have thrown out state laws that directly impose requirements on companies' health benefit plans, and Fishman said the proposed regulations bring Massachusetts dangerously close to such a challenge. He said, however, that Partners did not intend to file a legal challenge to the law. He said he did not know whether another company planned such a suit.
Sarah Iselin, commissioner of the Division of Health Care Finance and Policy, said her agency is aware of the potential legal risk and carefully considered that before proposing the new regulations.
"We heard many concerns expressed, as well as support by many parties, all of which we will take under advisement as we move forward," she said.
Iselin also said her agency estimates that nearly 90 percent of companies with 11 or more full-time employees will comply with the proposed new rules. She also said her agency's survey last year of all Massachusetts companies showed that 72 percent of businesses were offering some sort of health coverage.
In July, legislators passed a law, requested by Governor Deval Patrick, that requires hospitals to contribute an additional $28 million to help finance the new healthcare law and that also raises another $33 million from an assessment on insurance companies' reserve accounts. Earlier, administrators raised additional money by boosting premium payments for consumers who receive partially subsidized insurance.
Consumer groups who testified yesterday said it's time for businesses to step up and pay their fair share.
"We cannot balance health reform on the backs of the most vulnerable," said the Rev. Hurmon Hamilton, president of the Greater Boston Interfaith Organization, a coalition of religious, community, and civic groups.
"We need to make sure that the less than 30 percent of employers who do not cover their workers do not freeload," he said.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Across Mass., wait to see doctors grows: Access to care, insurance law cited for delays", By Liz Kowalczyk, (Boston) Globe Staff, September 22, 2008
The wait to see primary care doctors in Massachusetts has grown to as long as 100 days, while the number of practices accepting new patients has dipped in the past four years, with care the scarcest in some rural areas.
Now, as the state's health insurance mandate threatens to make a chronic doctor shortage worse, the Legislature has approved an unprecedented set of financial incentives for young physicians, and other programs to attract primary care doctors. But healthcare leaders fear the new measures will take several years to ease the shortage.
Senate President Therese Murray, who championed the legislation, said that many of the roughly 439,000 people who obtained health coverage under the 2006 insurance law are struggling to find a doctor. "You can take a look at the whole state and you are not going to find a primary care physician anytime soon," she said in an interview. "It became apparent very quickly that we needed to do something."
Access to internists and family practitioners is especially difficult in the western counties and on Cape Cod, doctors said, but Boston, too, is feeling the squeeze. Doctors and patient advocates report growing stress for patients trying to get care, and for physicians trying to squeeze them in:
In Williamstown, one doctor said he is working up to 60 hours a week to handle the increased patient load.
In Amherst, a physician began accepting new patients this year, but was so inundated by newly insured people that she had to shut her doors to new patients again six weeks later.
And in Great Barrington, Volunteers in Medicine, a clinic for the uninsured, is for the first time treating insured patients. It has taken weeks for newly insured residents to find doctors who will accept new patients, and months longer to get an appointment.
"We've been covering them because of the long time lag between getting insurance and getting established with a doctor," said Lynne Shiels, clinical care coordinator.
Access to care is not just a problem for the newly insured. Herman Berkman of Adams fell down some stairs a couple of months ago. But his primary care doctor, Robert Jandl, and an orthopedist's office were busy, Berkman said, so the 85-year-old went to the emergency room. Recently, when his blood sugar soared, Berkman had to see another doctor in Jandl's practice. He has a routine appointment with Jandl next month, made last February, but "if something happens in between, that's a different ball game," said Berkman, who added that he is very satisfied with Jandl's medical care.
Jandl has watched his colleagues in the Berkshires retire, move away, and quit high-stress practices to work predictable shifts in a hospital. With few new physicians replacing them, he had taken on so many patients that earlier this year, he closed his practice to new patients.
"This is a small community, so we've really extended ourselves trying to provide for these folks," said the 55-year-old Jandl, who belongs to Williamstown Medical Associates and works 55 to 60 hours a week. "But it's at the expense of everyone's personal lives. The hours are just not tenable for us right now."
A national primary care shortage has been looming for several years as doctors retire or leave the specialty, which requires long, unpredictable hours and pays less than most other medical specialties; some larger practices pay $170,000 to $190,000, but smaller rural practices can pay as little as $110,000.
At the same time, fewer new doctors are entering the field. According to a survey published this month in the Journal of the American Medical Association, 2 percent of students graduating from medical school plan to practice primary care.
In its annual survey of physicians, the Massachusetts Medical Society, the state's largest physicians group, found that among 100 internists the average wait time for an appointment for a new patient was 50 days, with some reporting waits of up to 100 days. In 2004, the average wait time was 47 days and the longest wait was 87 days. The waits for appointments with obstetrician/gynecologists and family practitioners also have generally increased.
Jandl said patients wait 65 to 85 days for a routine appointment with him, but two other internists he practices with have four-month waits. Patients with urgent problems or who are willing to see a nurse practitioner can get in sooner. He said a survey he conducted of other internists in the Berkshires showed generally shorter wait times.
The medical society also found that fewer primary care doctors are taking on new patients; 42 percent of internists surveyed have closed their practices to them, compared with 33 percent in 2004.
Amherst family physician Kate Atkinson decided to open her practice to new patients in January partly so she could take on the newly insured, especially since, by her count, 18 doctors in the area had closed their practices over the last two years. Most of those physicians have become hospitalists, caring for patients in the hospital, she said.
"There were so many people waiting to get in, it was like opening the floodgates," Atkinson said. "Most of these patients hadn't seen the doctor in a long time so they had a lot of complicated problems." She closed her practice to new patients again six weeks later. "We literally have 10 calls a day from patients crying and begging," she said.
Legislators hope the law passed in July to control the cost and improve the quality of healthcare will draw more primary care doctors into the workforce. Richard Cauchi of the National Conference of State Legislatures said no other state has passed so many initiatives in a single year to increase access to primary care.
The Massachusetts law includes $1.5 million this year to help the University of Massachusetts Medical School expand its class size - from 103 students to as many as 125 - and to waive tuition and fees for students who agree to work as primary care doctors in Massachusetts for four years after they finish training.
The state also is spending $1.7 million this year to repay medical school loans of doctors who agree to work in community health centers, and at least $500,000 to pay off debt for doctors who agree to work in primary care in underserved areas for at least two years; the average medical school student graduates with about $150,000 in debt. A new healthcare workforce center will identify underserved areas.
The law also directs state officials to develop a housing grant or loan program that will help doctors buy houses, including money for down payments, mortgage interest buy-downs, and closing costs.
Legislators don't know how many primary care doctors the package will attract to the state, but they believe it could be a significant number.
A loan repayment program started last year with a $5 million grant from Bank of America - the state also contributed $1.7 million last year - has attracted 45 doctors and 19 nurse practitioners. They will work in community health centers for two to three years in exchange for $20,000 to $75,000 in loan repayment.
"One of the things that concerns me is so many of the [legislative] initiatives have a long lag time," said Dr. Bruce Auerbach, an emergency room physician and president of the Massachusetts Medical Society. "There are things we could do more immediately and aggressively in terms of payment reform and reducing the administrative burden on doctors. Those are the things that are really driving people out of practice."
-
Liz Kowalczyk can be reached at kowalczyk@globe.com.
-

-
------------
"Massachusetts obtains extension of Medicaid waiver"
Associated Press, Tuesday, September 30, 2008
BOSTON (AP) — The state has reached an agreement with the federal government on a three-year extension of a Medicaid waiver needed to provide critical funding for the state's landmark health care law.
People close to the negotiations told the Associated Press today that the agreement secures billions of dollars more in spending authority for the state over the previous waiver and preserves eligibility and benefit levels. The Patrick administration is expected to announced the agreement this afternoon.
The waiver allows Massachusetts to bypass rules about spending its federal money for Medicaid, a state and federally funded program that provides health care assistance to low-income people. The state needs the waiver to continue using federal money as it shifts coverage from free emergency room care for the uninsured to a mix of private and government-sponsored insurance for all workers.
The federal payments were set to expire June 30, but Massachusetts received a series of extensions to continue negotiations.
Under the deal, overall spending over three years will jump by $4.3 billion over the previous three-year agreement to $21.2 billion, according to people with knowledge of the agreement who requested anonymity because it had not been formally announced.
The deal also allows the state to continue to offer subsidized health plans under the Commonwealth Care program to adults earning three times the federal poverty level. Children enrolled in the Children's Health Insurance Program whose families earn up to three time the poverty level also will be covered.
Federal negotiators had hoped to drop the eligibility level to two times the federal poverty level.
The agreement comes as Massachusetts continues to see increases in the number of insured residents as it works toward near universal coverage under the law. Between Jan. 1 and March 31, those with insurance increased from 340,000 to 439,000.
A total of 191,000 people have gotten private insurance since the law took effect in June 2006. Another 176,000 purchased subsidized insurance, while 72,000 have been insured through government programs.
The deal is the result of intense negotiations between the state and federal officials.
Sen. Edward Kennedy and Gov. Deval Patrick met with Health and Human Services Secretary Michael Leavitt in February and talks continued through the year. Kennedy spoke with Patrick on Sept. 21 to discuss the deal and then with Leavitt on Sept. 24 to make a final push.
------------
"Massachusetts gets $10.6b for healthcare insurance"
By Kay Lazar, Boston Globe Staff, October 1, 2008
At a time when many states are facing substantial cuts in federal financing, Massachusetts will be able to expand its first-in-the-nation healthcare law because of a federal promise of $10.6 billion over the next three years, Governor Deval Patrick said yesterday.
The deal, struck after months of delicate negotiations, gives Massachusetts about $2.1 billion more than it received from the government in its last round of negotiations three years ago for its Medicaid waiver package. The waiver allows Massachusetts to provide subsidized health insurance to some residents with incomes higher than would typically be allowed under traditional Medicaid rules.
While Massachusetts did not get everything it had requested, it did get all of the money it expected to receive for this fiscal year, Patrick said, easing anxiety among state leaders who are grappling with a budget shortfall.
"The American economy is in turmoil and the future is uncertain," Patrick said. "Thanks to this agreement, we can keep our healthcare commitments."
Patrick said the agreement also gives the state flexibility, allowing it to spend $5 billion over the next three years, about $1 billion more than previously allowed, on its newly created programs. The state had lobbied to get the spending cap lifted altogether.
Dr. JudyAnn Bigby, state secretary of health and human services, acknowledged that federal authorities turned down some requests by Massa chusetts but declined to specify what was denied, saying only that they were not "significant" items.
Although the amount granted the state was $2 billion less than requested in December, it was seen as sufficient, especially given that expected health insurance enrollment has lagged in recent months.
Several state leaders characterized the agreement as a federal stamp of approval for Massachusetts' historic healthcare law, which was enacted in 2006 and requires nearly every resident to have coverage.
"This is a signal from the federal government that they support what we are trying to achieve here," said state Senate President Therese Murray.
Yesterday's agreement is unusual. It comes at a time when many states are fighting with federal officials for the right to extend subsidized health insurance to people with incomes higher than is traditionally allowed under Medicaid rules.
Massachusetts was granted permission in its 2006 law to provide subsidized coverage to individuals making up to 300 percent of the federal poverty level, or roughly $31,000 for a single person and $63,600 for a family of four.
That has meant thousands more residents are eligible for health coverage that is at least partially subsidized by the government. Federal authorities agreed to continue that provision in the state's waiver package.
Senator Edward M. Kennedy, who played a pivotal role in behind-the-scenes negotiations, said the agreement allows the state to continue blazing a path for healthcare reform.
"We've made major progress in the program's first two years, cutting the number of uninsured in half and increasing employer-sponsored coverage," he said in a written statement. "Our experience with health reform in the Commonwealth argues well for our debate on national health reform next year."
Since the state launched its healthcare law two years ago, nearly 440,000 more residents have obtained coverage, with about half enrolling in their employer-sponsored programs. Several months ago, state officials said they faced at least a $130 million gap this fiscal year in paying for the newly insured, and they required hospitals and insurance companies to contribute more to the fund. The state also boosted premiums and copayments for consumers who receive subsidized coverage.
At the time, the Patrick administration also said it would require employers to pay more toward their workers' coverage under complex new rules that were to start today. But yesterday the administration, facing an uproar from businesses, said it would delay the rules until Jan. 1 and exempt many small companies from the proposed changes. Several business leaders had warned that the rules would force many companies, already reeling from the soured economy, to drop health coverage all together.
Bigby, the state's human services director, said in an interview that the concerns raised by businesses were "compelling" and that the state's intent was not to "penalize small businesses."
To soften the impact, state officials said yesterday, they would not only delay the new rules but apply them only to businesses with 50 or more full-time or equivalent workers - rather than businesses with 10 or more such workers, as was originally planned. Under the new rules, the larger companies would have to pay 33 percent of their workers' premiums within 90 days of hiring and make sure that at least 25 percent of their workers are covered by the plan. Otherwise, the employer must pay a $295 fine per worker.
Businesses with fewer employees would still be allowed to follow the old rules, Bigby said, and meet only one of the two requirements to escape the penalty.
-
Kay Lazar can be reached at klazar@globe.com
-
------------
"Small businesses are exempt from new increase in health care insurance requirements: Those with 50 or fewer employees exempt from health care requirement"
By Jon Chesto, The Patriot Ledger, October 02, 2008
BOSTON —
Business groups won a partial victory when Gov. Deval Patrick’s administration decided to exempt companies with 50 or fewer full-time employees from a new health care coverage requirement.
The Patrick administration on Wednesday unveiled the change, which would collectively cost businesses in the state about $30 million a year under the state’s “Employer Fair Share” rules.
That’s a big increase from the previous cost of $7.5 million a year in Fair Share fees. But the changes would have cost about $45 million a year under the Patrick administration’s original draft proposal, which drew widespread criticism in the business community.
The central issue in the Fair Share rules, which were put in place as part of the state’s 2006 health care reform law, involves deciding which employers are liable for a $295-per-worker annual fee for not making a reasonable contribution toward their workers’ health care.
Companies with fewer than 11 employees have been exempt since the program’s start.
Other employers have been able to avoid paying the fee if at least 25 percent of their full-time workers participate in an employer-sponsored health plan or if they offered to contribute at least 33 percent to the premium cost for a group health plan for full-time employees who had worked at least 90 days.
The Patrick administration is changing the rules to require employers meet both requirements to be exempt from the fee.
Business groups complained loudly, saying that many companies – especially small businesses – could be encouraged to drop their health plans and just pay the fees.
“We had quite a few responses from our members on this ... and I think the Patrick administration heard them,” said Bill Vernon, the Massachusetts director for the National Federation of Independent Business. “A number of employers have added health insurance since the law took effect. It’s important to (encourage) them to keep insurance.”
The administration’s Division of Health Care Finance and Policy said on Wednesday that it decided to allow employers with 50 or fewer full-time equivalent employees to continue to take advantage of the old rules. But companies with larger work forces would be forced to meet both requirements to avoid the $295-a-year fee – unless they can prove that more than 75 percent of their employees participate in their health plans.
The rules change would require about 1,100 companies to pay the per-employee fee, up from about 850 companies. However, about 3,000 companies would have been liable under the administration’s draft rules.
Jon Hurst, president of the Retailers Association of Massachusetts, said small businesses would have been particularly hurt under the draft rules because health insurance generally is more expensive for smaller companies and a greater portion of their employees get health insurance from another source.
“In general, we’re very pleased with the impact on small businesses,” Hurst said. “However, some of our arguments that we were relaying on the fairness of how this assessment would work certainly applies as much to big business as it does to small business.”
Eileen McAnneny, senior vice president for government affairs at Associated Industries of Massachusetts, said her organization’s members had hoped the Patrick administration would decide not to go forward with the regulation changes. She cited the administration’s success this week in negotiations with the federal government over Medicaid payments, as well as the arguments made by companies at a Sept. 5 hearing that the Patrick administration held to discuss the change.
“The employer community showed up in force at the hearing, and we made some compelling arguments, and we were hoping it was enough that these reg changes wouldn’t go forward,” McAnneny said.
-
Jon Chesto may be reached at jchesto@ledger.com
-
------------
"Kennedy ties helped secure waiver: Boosts Bay State healthcare law"
By Kay Lazar, Boston Globe Staff, October 7, 2008
It was the dog days of summer, and secret negotiations between Massachusetts leaders and federal officials had dragged on for months. The word was that future funding for the state's first-in-the-nation healthcare law looked bleak.
But then, something shifted in the talks. And now, four months later, state leaders are jubilant that Washington will send more money than most had dreamed possible to keep the state's pioneering program afloat. News of the $10.6 billion in federal aid arrived last week.
At a time when many other states are lamenting the lack of support from Washington for health programs, how was it possible for a state known for its liberal leanings to win such backing from a conservative administration?
An unlikely bond forged years ago between Senator Edward M. Kennedy of Massachusetts, an icon of the left, and US Health and Human Services Secretary Mike Leavitt, a conservative former governor of Utah, is part of the answer. The friendship set a collegial tone for the negotiations. It was crucial in salvaging talks when the White House threatened to slash nearly $2 billion from the state's health financing package, key players familiar with the negotiations said in interviews last week.
The package, known as a Medicaid waiver because it offers not only money but flexibility in federal regulations, allows Massachusetts to provide subsidized health insurance to some residents with incomes higher than would typically be allowed under traditional Medicaid rules. It authorizes Massachusetts to spend up to $21.2 billion, half of it federal money, over the next three years on health programs. That's an increase of $4.3 billion over the state's last Medicaid waiver package.
Leavitt, who oversees the agency that negotiated the waiver with Massachusetts, said he has privately sought Kennedy's advice on reconciling Democrats and Republicans over health insurance issues.
"What I appreciate about him is he is unvarnished on what the political pressures on his side are and what needs to happen to progress," Leavitt said.
He traces their friendship to 2003, when President Bush nominated Leavitt to head the Environmental Protection Agency. Leavitt asked for Kennedy's support, to which the Senator suggested Leavitt come to New Bedford to tour some polluted sites. Leavitt agreed and, after winning confirmation, visited the city.
"We are in different parties and have different ideas on the issues, but no one can fail to admire his devotion and that day, and others, formed the basis of our relationship," Leavitt recalls.
That friendship was tested in early June, when the Office of Management and Budget stepped into the waiver negotiations because, the regulators said, they discovered that Massachusetts for 10 years had incorrectly listed many children in its Medicaid program when they should have been counted under a program called the State Children's Health Insurance Program, which is not funded by the waiver. The state's way of counting those children had, by Washington's estimate, given Massachusetts about $2 billion more than it was entitled to over the last decade.
"We are talking about having to write a check for $2 billion and having to send it to the federal government," said Governor Deval Patrick. "It was a big problem."
The clock was ticking. Federal funding for Massachusetts' last waiver package was set to expire June 30. Negotiations had hit an impasse. That's when Leavitt went to bat for Massachusetts, said a source familiar with the negotiations, calling Joshua Bolten, President Bush's chief of staff and former director of the Office of Management and Budget, to argue the state's case.
Kennedy also called Bolton from his cellphone on June 19, while en route to Hyannis Port from Boston, where he was receiving cancer treatments.
"We were all very conscious of his very personal challenges," said Dr. JudyAnn Bigby, Massachusetts secretary of Health and Human Services, who helped negotiate the state's waiver. "We wanted to respect the fact that even though he was very committed to this and we wanted to make sure he was kept informed about what was going on, that we would only use him when we needed him," Bigby said.
In his conversation with Bolton - and with $2 billion on the line - Kennedy suggested that if Massachusetts universal healthcare initiative was successful, it could be a model for the rest of the country, and a legacy for the Bush White House.
"The senator and Josh definitely did talk," said White House deputy press secretary Tony Fratto. "And Josh communicated to OMB the interest, and then they were able to work out their agreement in a way that was mutually satisfactory."
That agreement on the $2 billion difference came after several more weeks of tense talks, with Washington agreeing to extend the June 30 deadline. During that stretch, the normally restrained Leavitt posted on his blog a candid entry about a phone conversation he had with Kennedy.
"He sounded great! We talked briefly about his health. He was forward looking, crisp and as passionate as always," Leavitt wrote. "There wasn't a single hint of negativity or worry. I'm sure he has moments when both creep in, but the call was an unexpected lift to my spirits."
Ultimately, Washington allowed Massachusetts to keep the disputed $2 billion but insisted that it change its accounting method.
So why was Washington so generous with the Bay State?
"We are all going to learn from what Massachusetts is doing," said Leavitt of the state's innovative attempt at near-universal health coverage. "We will learn from things that don't work and do work, and every state will benefit from what is going on in Massachusetts."
Kennedy was not available last week to talk about his role in the negotiations, but heralded the outcome in a statement: "Any reduction in commitment would have put our reforms at risk."
Final details of the agreement are being worked out and officials say a signed deal is expected soon. Health policy specialists underscored the unusual nature of the agreement, in the context of shrinking federal dollars.
"You have bad relationships between the states and the administration around Medicaid recently, and in the middle of an economic meltdown and an environment where the federal government is not looking to spend money, Massachusetts' waiver stands out as truly unusual," said Drew Altman, president and CEO of the Kaiser Family Foundation, a nonprofit that researches and analyzes health policies.
Several other states are cutting back their programs to reform healthcare, Altman said, because of a lack of funding.
"That's the reason Massachusetts, from a national perspective, is so significant," he said. The new waiver "allows the most sweeping health reform plan in the country to continue."
-
Kay Lazar can be reached a klazar@globe.com.
-
------------
"Two safety-net hospitals hit hard by budget cuts"
By Kay Lazar and Stephen Smith, Boston Globe Staff, October 17, 2008
State budget cuts will hit two of the state's safety-net hospitals particularly hard. Boston Medical Center has been notified it will not be reimbursed $64 million for care delivered to low-income Medicaid patients last fiscal year, and Cambridge Health Alliance will lose out on $40 million it had been expecting, state and hospital officials said yesterday.
An executive at Boston Medical, where 150,000 Medicaid patients receive care each year, said the hospital will be forced to cut services. Tom Traylor, vice president of federal and state programs, said the hospital is mulling which programs for low-income patients would be cut; options include interpreter services, transportation to the hospital, and asthma, diabetes or primary care.
Traylor said the cut is in addition to $12 million the hospital will lose this year as part of the sweeping reductions announced Wednesday by Governor Deval Patrick to close a $1.1 billion budget gap.
The medical center is a priority of Mayor Thomas M. Menino's administration, and the mayor said he is concerned about the potential effect of the cuts on residents.
"Regardless of changes in health insurance, there will always be many, many people who are not covered at all or not adequately and BMC continues to be the safety net for all those people," he said. "We would like to see the state work closely with the medical center to ensure their mission is protected."
Officials at Cambridge Health Alliance, which treated more than 50,000 Medicaid patients in the last fiscal year, said yesterday they had not yet been notified of the cuts. Earlier this year, the Globe reported that the hospital was on track to lose $26 million in the fiscal year that ended June 30.
Juan Martinez, a spokesman for the Patrick administration, said the cuts are part of more than $200 million slashed from Medicaid payments to providers "that allowed us to preserve all currently funded MassHealth populations and services. We understand the important role these hospitals play and remain committed to supporting them as best we can through this difficult economic time for everyone."
Lawmakers earmarked the Medicaid money for the hospitals as part of Massachusetts' 2006 health insurance law because they treat a disproportionately large number of low-income patients, but other hospitals have complained about being left out.
The payments are slated to end next year. Any cuts to the payments before that time must be approved by state lawmakers, and Traylor said BMC is considering asking legislators to rescind the cuts.
The governor's decision to cut Medicaid spending means Massachusetts will lose matching federal money.
In other healthcare cuts, the Department of Public Health is trimming nearly $6 million from its immunization program. Massachusetts has long been a national leader in buying vaccines for children and then distributing them to doctors, a policy that yielded the highest vaccination rates in the United States.
In an interview, John Auerbach, the state's public health commissioner, said his agency has not decided how much of the spending reduction will be carved from childhood immunizations and how much from adult programs, although he said all could come out of the adult program. The state had committed about $51.5 million for immunizations this budget year, with the federal government kicking in a comparable amount.
-
Donovan Slack of the Globe staff contributed to this report. Kay Lazar can be reached at klazar@globe.com and Stephen Smith can be reached at stsmith@globe.com.
-
------------
"Blue Cross-Blue Shield to cut administrative costs: Insurer says it must adjust for expected drop in enrollment"
By Jeffrey Krasner, Boston Globe Staff, October 17, 2008
Blue Cross and Blue Shield of Massachusetts, anticipating further deterioration of an employer-based health insurance system and more competition from out-of-state, needs to rein in administrative costs, according to an internal e-mail obtained by the Globe.
The 18- to 24-month effort is intended to keep the state's largest health insurer competitive as employers become less willing to absorb hefty annual premium increases.
No major layoffs are planned at the Boston firm, which has 3,800 employees. But Blue Cross-Blue Shield wants to keep payroll costs down by reducing its headcount through attrition, by boosting productivity through increased use of technology, and by allowing some employees to work from home to save on office space.
Blue Cross-Blue Shield is telling its workers the cost-cutting is part of an effort to fundamentally change the way it does business.
"Our current business model has served us very well over the past decade," said senior vice president Carole Waite, who will head the project, in an e-mail to employees. "This initiative I'm leading is about preparing our company for where the market is headed."
Blue Cross-Blue Shield is the state's dominant health insurer, with just over 3 million members. Harvard Pilgrim Health Care covers about 1 million members, and Tufts Health Plan has about 650,000. Several other Massachusetts health plans and some out-of-state, for-profit insurers also sell coverage in Massachusetts.
Since becoming president of Blue Cross-Blue Shield in 2003, Cleve L. Killingsworth has consistently criticized hospitals and other healthcare providers for offering too much or too little care to patients, and for providing too much care in emergency rooms instead of doctors' offices. He has also scolded hospitals for driving up medical costs, which account for 90 percent of Blue Cross-Blue Shield's spending.
But the new effort is instead focused on internal spending. Although the insurer's annual spending on administrative expenses has stayed roughly constant since 2001 on a percentage basis - between 10 and 12 percent of premiums - spending has soared because premiums have grown dramatically. In 2002, Blue Cross-Blue Shield spent $406 million on administrative expenses. Last year, it had grown to $705 million.
"Most of our time is spent trying to manage the 90 percent piece of the pie," said Stephen R. Booma, senior vice president of sales, marketing, and service. "This is about managing our own administrative costs."
Administrative costs can include salaries, the price of administering claims, marketing, computer systems, and other basic functions.
Booma said the plan to streamline spending is driven in part by fundamental changes happening in the nation's healthcare system. In recent years, the number of Americans who get their healthcare from employers has steadily declined. Only 60 percent of companies now offer healthcare coverage to employees, down from 69 percent in 2000, according to the nonpartisan Drum Major Institute for Public Policy.
Booma predicts more companies will give workers a fixed dollar contribution toward healthcare coverage, instead of a specific health plan. As a result, more coverage will be sold on an individual, retail basis, instead of through group plans. That means customers will become more aware of prices, he said. Blue Cross-Blue Shield predicts premiums for members renewing coverage in January will rise 11 to 13 percent, unless their employers trim benefits.
"Over time, there will be steady erosion of employers paying for healthcare," said Booma.
But still, he said, "If we manage our costs well, there's still a chance to grow market share in our core business," despite the state's stagnant population.
Blue Cross-Blue Shield is undertaking the cost-cutting plan while it is strong, Booma said, rather than waiting for a financial crisis. But despite its size, the insurer faces tough challenges. As Massachusetts companies have been acquired by out-of-state firms, more employees are switching to insurance provided by headquarters located elsewhere. Blue Cross-Blue Shield expects to lose about 40,000 members this year, falling to 3.02 million, in part because former Gillette employees now receive health benefits from parent firm Procter & Gamble Co., based in Cincinnati. It will be Blue Cross-Blue Shield's first membership decline since 1998.
The company also faces new competition in its lucrative business providing health plans to Massachusetts cities and towns. Under new rules, the municipalities are free to purchase insurance from the Group Insurance Commission, which arranges coverage for state employees and their families. Blue Cross-Blue Shield doesn't participate in the GIC's health plan.
And some question how much effect reining in administrative costs will have on the insurer's overall rates, given that they represent a small part of overall spending.
Jim Burgess, an associate professor of health policy and management at the Boston University School of Public Health and a consultant who has worked for Blue Cross-Blue Shield, said he views the effort to change the company's business model as a way of sending a coded message to customers and investors.
"Rather than trying to save significant amounts of money, Blue Cross is trying to tell employer groups and potential bond borrowers that they are a safe place to put money," said Burgess.
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
------------
"State tweaks health insurance rules: Base requirements for policy coverage will be tightened"
By Kay Lazar, Boston Globe Staff, October 18, 2008
Starting Jan. 1, residents who do not have health insurance that meets minimum standards set by state regulators could face a hefty tax penalty.
A state board voted unanimously yesterday to proceed with the new requirements, drafted in 2007. But the panel added exemptions for an individual, union, or employer who can show that their plan - while not one authorized by the state - has comparable benefits.
In general, to meet the test, a plan must offer coverage for prescription drugs, preventive and primary care, hospitalization, mental health and substance abuse services, and emergency services.
Plans for an expanded list of required minimum benefits was put on hold. The Commonwealth Health Insurance Connector Authority board voted to delay until Jan. 1, 2010 implementation of rules that will mandate radiation and chemotherapy; maternity and newborn care; and diagnostic imaging and screening tests. The delay is to give employers more time to overhaul their policies.
Leslie A. Kirwan, the board's chair and state secretary of Administration and Finance, said that regulators' goal is to make sure that nearly everyone in Massachusetts not only has health insurance, but decent coverage.
"Our intent is to help, not hurt people," she said. "We will continue to track implementation . . . to revisit thorny issues as they arise and to make mid-course corrections where necessary."
All health insurance companies licensed in Massachusetts will be required to notify customers about whether their plans meet state standards. However, the rules put the onus on individuals to make sure their coverage meets the state's minimum standards, because it will be individuals, and not employers, who are assessed the penalty.
Currently, the state's universal healthcare law requires most residents to have insurance or face a tax penalty of up to $912 per year. But the rules do not mandate what the coverage must include.
Regulators said yesterday that the penalty in 2009 would probably be higher than $912.
During the past year, board members have grappled to design minimum standards that give consumers vital insurance coverage to protect them from bankruptcy if they get sick, but are not so sweeping they make the insurance unaffordable.
"We're trying to make sure people have real insurance that means something," board member Celia Wcislo, a vice president of 1199 SEIU Health Care Workers East, said yesterday.
Despite months of public debate, some board members said they are concerned that employers might still not understand how to determine whether their policies comply with the rules, or how to appeal if they do not. The Board's executive director, Jon Kingsdale, said there will be presentations for employers across the state the next several months to sort through those issues, and mailings to insurance carriers and employers will explain the new requirements.
Brian Rosman of Health Care for All, one of the state's largest consumer groups, said he was pleased with the final package.
-
Kay Lazar can be reached at klazar@globe.com
-
------------
-

-
"Medical costs still burden many despite insurance: Massachusetts survey finds people in debt, skimping on care"
By Kay Lazar, Boston Globe Staff, October 23, 2008
Although far more Massachusetts residents have health insurance coverage than residents nationwide, a significant portion of Bay Staters are still struggling to pay for needed healthcare, a new survey shows.
Some are postponing treatments, and others are not filling prescriptions, because of high costs or an inability to pay bills from earlier procedures, according to the survey by The Boston Globe and the Blue Cross Blue Shield of Massachusetts Foundation.
A third of those surveyed said the cost of care is their biggest health concern, and 39 percent ranked it among their top two health concerns. No other concern came close.
Thirteen percent of residents with insurance said they were unable to pay for some health services in the past year. The same percentage of insured people said they did not fill at least one prescription because it was too expensive or their insurance copayment was too high. The numbers rise to 14 percent if both insured and uninsured residents are considered.
Two years into the state's pioneering healthcare experiment to insure nearly everyone, coverage is almost universal, with 97 percent of Massachusetts adults reporting they have some sort of insurance, according to the survey. Yet for some that did not translate into getting needed care.
"Basic things, like getting Flonase, [a sinus medicine] are a luxury," said Diane Schilder, a 44-year-old Arlington mom and adjunct college professor of education who has two children, a doctorate, health insurance, dental insurance, and about $800 of medical debt on her credit card.
Schilder is one of 506 adults surveyed in the telephone poll conducted Oct. 12 to 17 by the University of New Hampshire Survey Center. The margin of error is plus or minus 4.4 percentage points. Schilder is divorced, but still covered under her former husband's insurance, which carries a $500 family deductible for prescriptions and then covers only 50 percent of the costs for many drugs, she said.
Such insurance coverage is not unusual. "Many of the policies out there have such huge copayments and deductibles that people can't afford care," said Dr. David Himmelstein, associate professor of medicine at Harvard Medical School and a primary care doctor at Cambridge Health Alliance.
Himmelstein is cofounder of Physicians for a National Health Program, an organization that pushes for national health insurance. He studied personal bankruptcies nationwide in 2001 and found that about half of them were linked to a medical issue, and in three-quarters of those cases, the debtor was insured.
While medical debt is burdening a sizable number of Massachusetts residents, the pain is greater nationally, where the percent of uninsured is about five times greater, according to the latest US Census.
A national poll released this week by the Kaiser Family Foundation, a California-based nonprofit that researches health policy, found that about a third of Americans surveyed reported that their family had problems paying medical bills in the past year and that almost one in five said they had medical bills of more than $1,000.
Healthcare leaders say the state's first-in-the-nation law, which requires nearly everyone to have health insurance or face a tax penalty, has mitigated some cost concerns for consumers.
"It may be that while you are seeing those problems in Massachusetts, they are not as high as what we are seeing nationally because in Massachusetts people do have access to healthcare," said Drew Altman, Kaiser president and chief executive officer.
Dr. JudyAnn Bigby, Massachusetts secretary of health and human services, said prescription costs can be prohibitive, especially for low-income residents who have chronic health problems and need several medications. She said the state is considering eliminating or greatly reducing the $1 copayments for thousands of residents on Medicaid who need medications to treat diabetes or high blood pressure or cholesterol.
"It would make it more affordable for people with chronic medical conditions to take multiple medications and . . . manage their conditions better," she said.
Still, she said, fewer residents overall are struggling with medical bills since Massachusetts overhauled its healthcare laws two years ago. She cited a recent survey by the Urban Institute, which found that the share of people with skimpy health insurance that left them with huge medical bills has dropped two percentage points since the state's new law started.
It also found that such inadequate insurance is a problem for three times the number of people nationally, compared with Massachusetts. Starting in January, the insurance coverage mandated by the state will have to include prescription drugs.
The Globe-Blue Cross survey found that income has a direct correlation to a household's ability to afford care. People with household incomes less than 300 percent of the federal poverty level, roughly $31,200 for a single person, were more than twice as likely to report problems affording prescriptions or other care. People who are divorced or who never went beyond high school were also more likely to report healthcare cost problems.
Among those reporting difficulty was Harvard University graduate student Justin Vincent, 26, a brain researcher who was stuck with a $3,000 bill last year after breaking his leg because his health insurance did not cover the physical therapists recommended by his doctor.
"After the leg surgery, I generally refuse medical care because they don't tell you what the prices are," he said. "It's not like Walmart, where they tell you what the prices are."
The Globe/Blue Cross survey found that 8 percent of people with insurance and 9 percent overall reported avoiding or postponing medical treatment because they already owed money for health services. In Blackstone, Robert Ravenelle, 20, a private security guard who makes about $10 an hour, said he is still paying off a $1,400 emergency room bill from last year for a knee injury because he doesn't have health insurance. Ravenelle said he has received warnings from the state about facing a tax penalty for not having coverage, but has decided paying the penalty is less expensive than buying insurance.
"Unless they want me to live on the street," he said, "I can't do it."
The Blue Cross Blue Shield Foundation recently launched a project studying how state residents get care.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Healthcare network says it may lay off hundreds"
By Kay Lazar, Boston Globe Staff, October 25, 2008
Cambridge Health Alliance, a key part of the Boston area's healthcare network, is warning that it may have to lay off hundreds of workers and consolidate operations because of deep cuts in state funding.
The healthcare network - which includes hospitals in Cambridge, Somerville, and Everett, as well as 20 community health centers - serves a disproportionately large share of the area's poor. It is operating on a $22 million deficit budget this year.
In a stark memo to staffers, alliance CEO Dennis D. Keefe wrote that the Patrick administration's plan to slash $55 million from the organization's budget would "translate to a reduction of more than 20 percent of our workforce." The memo noted that the alliance is about two-thirds of the way through a previously announced plan to cut expenses by reducing staff by the equivalent of 300 full-time jobs.
"Unless the financial picture improves or we find other ways to trim costs further, there will be more reductions," Keefe wrote. "It is important to note that we are doing everything possible to try and impress state officials on the impact these cuts will have."
Governor Deval Patrick last week announced sweeping cuts that include nearly $300 million for healthcare spending to help close a $1.4 billion state budget gap. The alliance and Boston Medical Center were especially hard hit.
Now, officials at both healthcare facilities are scrutinizing their operations for potential savings while lobbying lawmakers in hopes that they will reverse some of the governor's proposed cuts.
Keefe declined to comment, but Alliance spokesman Doug Bailey said the network is doing everything it can to lessen the impact on patients. Earlier in the week, the Alliance announced that over the next three months it would close its Oliver Farnum Senior Health Center in Cambridge, where patient volume was down 25 percent this year.
"The intent is to not to reduce our level of service at all, but to combine access points," Bailey said. "Whether that can be done in light of these cuts is questionable."
Senator Anthony D. Galluccio, a Democrat whose district includes Cambridge, Somerville, and Everett, said he is organizing a meeting early next week of lawmakers whose communities also are served by the Alliance's many health centers. He is urging those legislators to fight the cuts.
"We all understand the give and take of budget cuts," Galluccio said. But dismantling the largest public health authority geographically in the Commonwealth, which serves the most vulnerable residents of the Commonwealth, should not be part of that game plan."
Dr. JudyAnn Bigby, state secretary of health and human services, said she understands the tough road the Alliance faces, but said its leaders have not told her in private discussions that they feared a dismantling of the network's core services.
"It's difficult for everyone to go through this, and we will continue to work with Cambridge as much as we can to work through this issue," Bigby said. "But we have no way to lessen any of the cuts we announced."
Even if the Alliance wins a reprieve from state cuts, it will still face difficult decisions next fiscal year because it is set to lose $94 million in Medicaid funding it has been receiving under the state's 2006 healthcare law. Lawmakers earmarked money for the Alliance and Boston Medical Center because both treat a disproportionately large number of low-income patients. But other hospitals have complained about being left out. The payments are slated to end next year.
The governor said he will not reimburse Boston Medical Center for $64 million in services it delivered to low-income Medicaid patients last fiscal year and will also cut $30 million in Medicaid rates for this fiscal year.
BMC spokeswoman Ellen Berlin said that if those cuts stand, the facility is projecting a deficit in the tens of millions of dollars for this fiscal year. She also said that it has not made any decisions about what areas to cut but expects to leave currently vacant management and administration positions unfilled until its budget situation becomes clear.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Massachusetts hospital network cuts jobs due to deficit"
By Associated Press, Wednesday, November 5, 2008, www.bostonherald.com, Local Coverage
SPRINGFIELD - The western Massachusetts healthcare network that runs Baystate Medical Center in Springfield says a $37 million deficit is forcing it to cut 55 jobs and eliminate 120 vacant positions.
Baystate Health said today that it will also enact a hiring freeze for non-clinical positions and wait until the economy improves before moving ahead with financing for a major expansion.
Baystate says it’s been hit hard by the economic downturn, reductions in Medicaid reimbursements and falling numbers of patients. The deficit represents about 2.3 percent of its budget for the current fiscal year
The company, which employs about 10,000 people, also operates hospitals in Ware and Greenfield and runs several regional health centers.
------------
"A healthcare system badly out of balance: Call it the 'Partners Effect:' Elite hospitals are paid much more for care that is often no better than average. It is the best kept secret in Massachusetts medicine"
The Boston Globe, November 16, 2008
This story was reported by Globe Spotlight Team members Scott Allen, Marcella Bombardieri, Michael Rezendes, and editor Thomas Farragher, as well as Liz Kowalczyk and Jeffrey Krasner of the Globe staff. It was written by Allen and Bombardieri.
As his patient lies waiting in an adjacent exam room, Dr. James D. Alderman watches while an assistant reaches into a white envelope and pulls out a piece of paper that will determine where the man will be treated. Big money is on the line.
Alderman, an interventional cardiologist, plans to open the patient's clogged coronary artery by inserting a flexible tube with a tiny balloon at the tip. Usually he does the procedure, called angioplasty, at MetroWest Medical Center in Framingham. But he sometimes operates in Boston as part of a research program. One time of every four, by the luck of the draw, Alderman and his patient go to a big teaching hospital in the city.
If the white slip of paper directs him to do the procedure in Framingham, the insurance company will pay the hospital about $17,000, not counting the physician's fee. If Alderman is sent to Brigham and Women's Hospital in Boston, that hospital will get about $24,500 - 44 percent more - even though the patient's care will be the same in both places.
"It's the exact same doctor doing the procedure," said Andrei Soran, MetroWest's chief executive. "But the cost? It's unjustifiably higher."
Call it the best-kept secret in Massachusetts medicine: Health insurance companies pay a handful of hospitals far more for the same work even when there is no evidence that the higher-priced care produces healthier patients. In fact, sometimes the opposite is true: Massachusetts General Hospital, for example, earns 15 percent more than Beth Israel Deaconess Medical Center for treating heart-failure patients even though government figures show that Beth Israel has for years reported lower patient death rates.
Private insurance data obtained by the Globe's Spotlight Team show that the Brigham, Mass. General, Children's Hospital, and a few others are, on average, paid about 15 percent to 60 percent more than their rivals by insurance companies such as Blue Cross Blue Shield of Massachusetts and Harvard Pilgrim Health Care. The gap is even more striking for many individual procedures, which can be two or three times more expensive in one hospital than in another.
This payment pattern has become a driving force in the state's galloping healthcare costs, and it raises hard questions about why certain hospitals and physicians receive premium pay for care that is no better than that of their competitors. Until now, the growing pay gap has not been subject to public scrutiny because contracts between insurers and hospitals typically include confidentiality agreements.
But an ongoing Spotlight Team investigation of healthcare in this state found scores of payment disparities for routine procedures in which there is no obvious difference in quality. Consider:
Children's Hospital typically gets about $1,100 for making an MRI of an ankle or a knee, not counting the physician's fee. Insurers pay Boston Medical Center $490 for the same procedure, using a similar high-tech machine.
The technician who makes a simple chest X-ray to help diagnose pain or an insistent cough brings in $75 at Anna Jaques Hospital in Newburyport. Mass. General earns more than twice as much, $160, for producing the same image.
The cost of Catherine Murphy's care was $5,309.15 for two days in Winchester Hospital to treat the pneumonia she contracted soon after her wedding earlier this year. Had she gone to Brigham and Women's instead, similar care would have cost more than $9,000, according to a Spotlight Team analysis of insurance records.
The dramatic payment gaps have emerged over the last decade as hospitals pushed, with varying levels of success, to offset federal budget cuts by boosting their income from insurance companies, health executives say. The resulting wide range of payments for the same services reflects a healthcare system in which deregulation and lax government oversight have allowed the hospitals with the most clout to extract big increases from insurers while everyone else falls behind.
"The same service delivered the same way with the same outcome can vary in cost from one provider to the next by as much as 300 percent," said Charles Baker, president of the state's second-largest health insurer, Harvard Pilgrim Health Care. "There is no other sector of the economy anywhere in this country in which that kind of price variability with no appreciable difference in service or product quality can sustain itself over time."
Health insurance premiums paid by the average Massachusetts family have jumped 78 percent since 2000, and Baker believes that a significant portion of the rise has been driven by hefty insurance payment increases to dominant providers, who use the extra income to install the latest technology and expand, often on rivals' turf.
At the same time, the pay gap undermines less powerful hospitals, whose officials say that they steadily lose doctors to those that can pay more, and that they constantly struggle to keep pace with advances in costly medical technology. For instance, while Mass. General is spending $686 million on the single most expensive hospital expansion in state history, the state's second-largest hospital chain, Caritas Christi, had to borrow money this year to pay for basics, like oxygen tanks.
"The playing field is dramatically unlevel," said Dr. John Chessare at a conference in June, when he was acting chief executive of Caritas Christi. He noted that nearly all Massachusetts hospitals are nonprofit charities - exempting them from having to pay millions in taxes - and argued that those that receive higher insurance payouts should not be in the business of snaring patients away from the less well paid.
"They are using that not-for-profit status to make a profit and to build more capacity for things we don't need," he said.
A powerful hand
Most patients don't think about the payments their insurance company makes to hospitals and doctors, but they should: Inflation of those payments is the main reason insurance premiums increased by an average of $1,800 per family during this decade. More than 85 cents of every dollar in insurance premiums goes to pay the bills in hospitals, doctors' offices, and other medical facilities. Five years ago, those bills were rising mainly because of growing patient demand for care, Blue Cross data shows, but now the escalating prices that hospitals and doctors charge is far more important. A recent Massachusetts study concludes that the price of inpatient care at hospitals is rising by 10 percent a year, while overall use of hospital beds is declining.
The hospitals that are paid at the highest rates all share one trait: They have the bargaining clout to demand higher insurance payments. Often, that clout is based on a powerful brand name and elite reputation. Children's Hospital has negotiated the highest insurance payments in the state, arguing that its work with children is uniquely expensive. The high rates have allowed the hospital to consistently report profit rates three times the median for Massachusetts hospitals; still, insurers pay to keep Children's happy because they know parents won't buy insurance that doesn't include access to one of the world's most prominent pediatric hospitals.
The other source of bargaining power is geographical isolation. Sturdy Memorial Hospital in Attleboro, for example, commands high insurance payments for outpatient procedures because local residents have no convenient alternative, insurance executives say.
But no company has thrived more in this sharply competitive world - or has had more impact on the cost of medicine here - than Partners HealthCare, a company formed in 1994 to fight back against what its founders saw as the stinginess and lopsided power of insurance companies, which had brought many hospitals to their knees. By bringing together two of the most prestigious hospitals in Boston - the Brigham and Mass. General - Partners became what some called the "800-pound gorilla" of Massachusetts healthcare, able to bend insurers to its will.
Almost from the start, Partners played its powerful hand with conspicuous - rivals would say relentless - aggression and skill. No other city can boast two of the top 10 hospitals on US News and World Report's honor roll, and every insurance company is vividly aware that its members want access to their famed halls.
Partners' dominance became clear in 2000, when executives of Tufts Health Plan had the temerity to refuse Partners' demand for a substantial rate increase. Partners countered by declaring it would no longer accept Tufts insurance at its hospitals. Within days, as thousands of Tufts customers threatened to change insurance rather than lose the right to treatment at the two famous hospitals, Tufts gave in to Partners' demands. Since then, Partners has negotiated one big pay increase after another from insurance companies fearful of a similar humiliation.
Today, the Brigham and Mass. General are paid an average of 30 percent more than similar nonpediatric hospitals statewide for each procedure, based on payment rates of Blue Cross obtained by the Spotlight Team. The health official who provided the information asked not to be identified for fear of professional retaliation. Though Partners' rates are not the highest - that would be Children's - Partners has more effect on statewide costs because its revenue is five times larger.
"We were willing to take the risk of challenging payers," said Partners chief financial officer Peter Markell, adding that Partners should not have to apologize for a successful strategy. "If you are never willing to challenge them, of course they are going to jam it down your throat."
That willingness to get tough turned Partners' main insurance contracts from money losers a decade ago to the company's largest source of profit, Partners officials say. Extrapolating from Partners' internal tally of its insurance revenues, the Brigham and Mass. General receive at least $500 million a year more from the three biggest insurers than if they were paid at the lower rates typical of their rivals. Likewise, Partners' 6,000 physicians are paid 15 percent to 40 percent more than most other Massachusetts doctors, based on Blue Cross rates, while the company's community hospitals earn at least 10 percent more than their peers.
Altogether, those higher rates add up to at least $800 million more for Partners hospitals and doctors than if they were paid at rates similar to competitors, based on Partners' insurance income. That is the equivalent of $170 a year for every member of the three leading insurers - Blue Cross, Tufts, and Harvard Pilgrim.
Partners officials reject the idea that their insurance payments have driven up healthcare costs significantly, arguing that costs in Massachusetts are part of a national problem and not caused by any one company. They note that insurance premiums here are rising at about the same rate as the national average.
"Boston is experiencing the same premium increases as the rest of the country," Partners said in a prepared statement to the Globe.
Likewise, the state's insurers are divided on Partners' responsibility for the current price run-up. Blue Cross officials discount Partners' role, while Baker at Harvard Pilgrim says there is a meaningful but hard-to-measure "Partners effect" on statewide insurance costs. And Partners officials themselves have said in the past that their goal was to "reset the prices" paid to hospitals even if it drives up insurance premiums.
Partners' favorable insurance contracts have helped the company to reap $1.7 billion in profits since 2004, reflecting a profit rate that is average compared with the nationally known hospitals the company considers its peers. But it's high by Massachusetts standards: Partners collected 35 percent of statewide hospital profits last year, even though it owns only 16 percent of the beds.
Those earnings have allowed Partners to launch a five-year $4 billion construction program that includes the addition at least 180 new hospital beds and several outpatient facilities. Though the current recession is expected to slow expansion considerably, Partners officials say it won't affect projects already underway.
While Partners prospers, 24 Massachusetts hospitals are losing money. Many of them would be profitable if they had even a fraction of Partners' contract clout. Caritas Norwood Hospital, for instance, could erase the $242,347 deficit it reported through the third quarter of this fiscal year if the hospital were paid Partners rates for the babies it delivers. Instead, the hospital is losing money and bracing to lose more next year, when Partners opens a new outpatient center at Gillette Stadium in Foxborough.
"Some are able to spend more than others," said Jack Connors, Partners' longtime chairman of the board. "It's our fortune that we're probably in the lead on those investments. And several hospitals aren't able to keep that pace. And that's what I, as a businessman, call market forces, if you will."
But market forces don't do much for some other highly regarded hospitals. A few years ago, when an executive for Beth Israel Deaconess Medical Center asked then-Tufts HMO boss Harris Berman why Beth Israel, a Harvard teaching hospital, wasn't paid as well as Partners, Berman said he had a simple response: "You are not Partners."
One influential researcher found that Beth Israel's overall mortality rate was lower in 2005 than the mortality rates at both the Brigham and Mass. General, but the hospital and its doctors still earn 15 percent to 20 percent less for the same work, according to the Blue Cross rates obtained by the Globe.
"Shouldn't there be some correlation between what you get paid for doing something and the quality of what you do?" asked Beth Israel chief executive Paul Levy last month in remarks at the Massachusetts Medical Society.
Curtain of secrecy
Michelle Faulkner got lucky.
The self-employed marketing consultant sprained her right ankle last Memorial Day weekend for the second time, and in August, when she still felt pain while running, she went to see an orthopedist. Fortunately for her, the doctor, affiliated with Winchester Hospital, did not send her into Boston for an MRI. That choice saved her about $500.
Faulkner is one of thousands of Massachusetts residents who save money on insurance by purchasing lower-cost plans that require patients to pay a higher deductible before insurance kicks in. Faulkner had to pay the $526.84 MRI bill herself, which hurt, but the bill at Winchester Hospital was far more affordable than what she would have paid for care at the Brigham ($987) or Mass. General ($1,091), insurance claims data show.
"People don't shop around," said Faulkner, 39. "That's why insurance is so high."
One reason patients don't shop for care is that, as a practical matter, they can't. The pay rates of different caregivers have long been treated as confidential data, veiled by nondisclosure agreements between insurers and hospitals. As a result, there has been no public notice or debate as an insurance system that a decade ago paid hospitals and doctors similar amounts for the same work has grown into one that disproportionately rewards a few.
The insurance data obtained by the Globe, drawn from millions of medical claims collected by the state Health Care Quality and Cost Council, is a byproduct of the state's sweeping healthcare reform law of 2006. Because some hospitals treat sicker people, the data has been adjusted to reflect the cost of care for an average patient.
The law calls for the council to post insurance claim information on the web so that the public can see the disparities. But a year and a half after the law was passed, the council has still not published its findings because of disputes with medical groups about how the numbers should be presented and whether they are accurate in every detail.
"Apparently, this subject is the equivalent of the third rail," said Gregory W. Sullivan, the state's inspector general and a member of the Quality and Cost Council.
However, council officials say privately that the data, after months of review by the hospitals, is generally accurate. Partners said it has raised concerns "about the data and methodology" with the council. But other hospitals contacted by the Globe either confirmed the data's accuracy or would not comment on it.
The Globe also checked the state numbers against detailed payment rates for Blue Cross; the two closely track. The Blue Cross data show that about 10 hospitals - four Boston teaching hospitals and six community hospitals - are paid at least 30 percent above the state average, while 12 hospitals make at least 20 percent below average, including Cambridge Hospital, which earns about half as much per procedure as the Brigham and Mass. General.
Partners officials say that they don't know exactly how their pay compares to others, though they know they are paid more. That added revenue is going for good purposes, they say, such as research and doctor training. Insurance profits also subsidize unprofitable lines of business, such as psychiatric care and the burn units at the Brigham and Mass. General. In addition, Partners employs 50,000 people, more than any other private company in Massachusetts.
Partners officials also say they are building a massive integrated system that could become a model for how to reduce errors and waste. The company's computer networks, for example, will eventually be used to bar-code every single pill, so that each can be double-checked at bedside.
"We are different," said Dr. Thomas H. Lee, chief executive of Partners' physicians network, "I would say it is like 70 percent potential and 30 percent reality in terms of how different. But we have the pieces of a system that are increasingly actually working together."
Lee, however, admits that existing measures of quality do not prove Partners is consistently better. In fact, he argues that the science of measuring medical quality remains so limited that it can't determine which is the best among Massachusetts' very good hospitals. He offers an analogy: If the Boston marathon were judged using tools as imperfect as current medical quality measures, researchers could identify the Kenyan runners at the front of the pack, but they could not predict the winner.
Partners hospitals, he said, "are running with the pack of Kenyans at the front of the country. And it's great to be one of those Kenyans, but there's a fair amount of angst about us because we are being paid more than the other Kenyans, and they aren't particularly happy about it."
Brand name medicine
Karen Dahl, 31, lives less than 2 miles from Mount Auburn Hospital in Cambridge, but when she became pregnant with her first baby last year, she decided to go to a Boston teaching hospital to deliver.
"I talked to women in the area who had babies in Boston," said Dahl, a self-described nervous patient who gave birth to son Henry by Cesarean section at the Brigham last November. "I also looked at the US News rankings for female care. The Brigham was rated very high."
State health officials have tried to encourage women like Dahl to reconsider their flight to Boston, pointing out in a 2003 study that community hospitals are generally just as reliable as teaching hospitals for normal births. In fact, they had a slightly lower complication rate - and they're a lot cheaper. Dahl's care cost $8,282.14 at the Brigham, while the cost at Mount Auburn would have been about $5,700, according to state insurance data.
But Dahl, who had a complicated pregnancy, has no regrets: "I felt this was the safest place to be if anything happens."
Massachusetts patients love brand name medicine, going to teaching hospitals 2.5 times more often than patients across the country, according to a 2005 report for the Massachusetts Council of Community Hospitals. It is a habit that carries a heavy cost: We spend about $1.7 billion more per year than we would using community hospitals at the national rate.
Partners' Lee, a cardiologist who still sees patients in addition to his management job, argues that patients are voting with their feet.
"There's a very fair question of can we afford that as a society, but there's no question in our market that people want this," Lee said. "I have people come and see me from New Hampshire and Rhode Island for their blood pressure, and I tell them, 'You don't need to come here,' and they say, 'But I want to,' and I think they're sometimes offended because I'm trying to chase them away."
The growing dominance of Partners - and Children's Hospital for pediatrics - is a microcosm of the national trend in the last 15 years, as government has increasingly allowed the market to decide what healthcare will be available and at what price. Hundreds of unprofitable hospitals closed, while many others merged to gain more negotiating power with insurance companies, which, by the mid-1990s, were aggressively denying claims and shortening hospital stays to hold down costs.
The balance of power between insurers and providers did need to shift. But the realignment has had costly side effects: After a decade of stable insurance rates in the 1990s, medical inflation began to soar across the country, something economists attributed partly to the increased clout of merged healthcare systems like Partners. And healthcare specialists agree that the price run-up did not lead to a similar improvement in quality.
At a Federal Trade Commission workshop on healthcare in April, the moderator asked a panel of healthcare leaders, "Is price a signal of quality in healthcare markets?"
A professor quickly offered a one-word answer: "No."
There was a pause. Then someone else chimed in, "There's a universal no on that."
The moderator concluded, "That was pretty easy," and moved on to the next question.
Behind the rankings
To walk the gleaming corridors of Partners' flagship hospitals is to tour a Hippocratic Hall of Fame: Dr. William Morton first demonstrated the use of anesthesia in surgery at Mass. General in 1846. Dr. Joseph Murray carried out the first successful organ transplant at the Brigham in 1954. Today, the two hospitals manage one of the largest biomedical research budgets in the country, carrying out cutting-edge studies on everything from AIDS to arthritis and attracting patients from all over the world.
But the high-end procedures that make the Brigham and Mass. General so famous are not their bread and butter. Eighty-five percent of the time their doctors are performing the same less glamorous medicine that occupies most other hospitals: delivering babies, repairing hernias, treating pneumonia.
And it is there, in the workaday world of hospital care, that the hospitals' reputation for unmatched excellence fades - and with it much of the rationale for the higher payments they receive for such treatments. The growing, if still inadequate, body of data available about hospital quality paints a fairly consistent picture of the care at the Brigham and Mass. General: often good, but rarely extraordinary, and sometimes inferior to the care available at other hospitals.
The two hospitals have inconsistent performance on routine care, according to data collected from nearly all US hospitals by the Centers for Medicare & Medicaid Services on how often hospitals give the right drug or test on time. Using a method of comparison commonly employed by government officials and researchers, the Globe determined that the two hospitals finished ahead of the other Boston teaching hospitals overall for four areas of treatment in a recent 12-month period, but both scored lower on caring for pneumonia patients than half of American hospitals. A quarter of American hospitals outperformed Mass. General on heart failure care.
Hospital accreditors faulted Mass. General after a surprise inspection in December 2006. They saw staff members fail to wash their hands after touching patients, and the hospital could not document that its staff had consistently followed routine safety checks that can prevent doctors from performing the wrong procedure on patients. At the Brigham earlier this year, the rate of one common - but dangerous - infection that sometimes enters the bloodstreams of intensive care patients was about twice as high as that at Beth Israel Deaconess. Brigham officials said their infection rate has since dropped.
When it comes to saving lives, the Brigham and Mass. General do not rate the highest even in Massachusetts. A review of 42 individual mortality ratings produced by the state and federal governments for Massachusetts hospitals from 2002 to 2007 found that three other hospitals - Beth Israel Deaconess, Partners' own Newton-Wellesley Hospital, and Beverly Hospital - had the highest average scores.
The mortality rankings - adjusted for the relative sickness of patients at different facilities - graded hospitals as either average, above average, or below average for ailments and procedures from pneumonia to coronary bypass surgery. The vast majority of the ratings for all hospitals were average, but Beth Israel earned a dozen above-average scores, and none below average. The Brigham received seven above-average scores and one below-average score. Beverly and Cape Cod hospitals each earned five top scores and no low scores. Mass. General had four high scores and one low score.
In sum: When all scores are averaged, the Brigham ranks high, though not among the very best; Mass. General was part of the broad middle, or average, tier.
Partners officials said some of the ratings are based on untrustworthy data that should not be used for scoring. In general, they said, the statistical methods used to adjust for the sickness of the patients at different hospitals are not sophisticated enough to recognize how much more vulnerable their patients are.
They also noted that even as governments are making more data public, many of the existing measures are controversial and often fairly crude.
"I think a consumer that relies on the cross-section of information that's out there and available to them, it's akin to being a cork floating in the ocean," said Dr. David F. Torchiana, head of the Massachusetts General Physicians Organization. "You'll be driven in random directions by the randomness of the information that you will obtain."
But Dr. Atul Gawande, a surgeon who juggles his practice at the Brigham with writing soul-searching books and magazine articles about his craft, said the reality is that no hospital, not even his own or Mass. General, can be good at everything.
"We aim to deliver more than 2,000 different kinds of surgical procedures, and there are more than 10,000 different diagnoses we take care of," Gawande said of the Brigham and Mass. General. "There is no way we are the best at all of them. I'd be surprised if you didn't find that there are particular areas of incredible excellence, but for the larger share of them we are probably floating around in the middle, and I would not be surprised if on a portion of them we are down toward the bottom."
And it is by no means clear that a big teaching hospital is safer or better than a well-run community hospital for a wide variety of procedures, including some that are fairly complex.
Cape Cod Hospital in Hyannis, for example, reported no deaths among 741 angioplasty patients from July 2007 to June 2008, an extraordinary feat that hospital officials attribute partly to the fact that theirs is not a teaching hospital. The care also costs less: $20,020 for angioplasty, on average, compared with $27,242 - 36 percent more - at Mass. General, according to the insurance records collected by the state.
"When you go to a teaching hospital you have residents and interns caring for you, which is different from our hospital," said Dr. Richard Zelman, the hospital's director of interventional cardiology, referring to doctors who have not completed medical training. "When you come into Cape Cod Hospital at three in the morning having a heart attack, you have an attending cardiologist with 20 years of experience that will take care of the patient every step of the way."
Many community hospitals say they are willing to cede some of the most complex, technology-assisted care to the large teaching hospitals. They can't compete in that arena. And they don't try to.
But for more ordinary procedures - the vast majority of care - community hospital officials say the existing data on quality supports what they've been arguing for years: They're as good. Or better. And considerably cheaper.
At Caritas Norwood Hospital, where he scrubbed floors as a teenager, Dr. Adam Glasgow said it's unfair that the Brigham and Mass. General make so much more for some procedures, even factoring in the expense of teaching and research.
"We're doing the same work," said Glasgow, a surgeon. "It doesn't make any sense for that institution and that physician to be paid more for doing the same work. It just drives up the cost of healthcare. It's unfair, and it's unnecessary."
-

-
------------
A Boston Globe Editorial
"Unkindest cuts in healthcare"
November 21, 2008
FROM the day Massachusetts embarked on its pioneering healthcare reform law, all its supporters crossed their fingers that no recession would come along to derail the plan's delicately balanced finances. Now, the economic downturn is taking a toll on the two healthcare centers that serve the largest share of the state's poor and uninsured, the Cambridge Health Alliance and Boston Medical Center. Governor Patrick's budget cuts last month in response to the state's declining revenues hit the two institutions hard.
The stability of Boston Medical Center, and of the three hospitals and more than 20 community health centers of the Cambridge Health Alliance, is crucial to the new law's success. Together they serve more than 200,000 Medicaid patients as well as many who shift back and forth between the ranks of the uninsured and the state-subsidized Commonwealth Care plan.
Cambridge Health Alliance, in particular, provides care to many illegal immigrants, who are excluded from public programs, and to many patients suffering from mental illness or substance abuse. Cambridge attracts these patients because it offers interpreters and other specialized services. Although the healthcare law has been successful statewide in enrolling the uninsured, the alliance has seen its uninsured patients decrease by just 21 percent.
When the Patrick administration last month saw the recession shrinking revenues, it focused on cuts in Medicaid for the same reason Willie Sutton gave when asked why he robbed banks: That's where the money is. But the $55 million it is taking from the Cambridge alliance and the $114 million from Boston Medical Center will seriously hurt the institutions' ability to serve patients.
Even before the latest cuts, the Cambridge alliance was operating at a deficit and had begun to close a senior health center in Cambridge. More consolidation is in order. But the health alliance CEO, Dennis Keefe, said the most recent cuts have turned what was supposed to be a "glide path" toward reduced state support into a "crash landing." The alliance is facing a reduction of 20 percent of its work force.
One short-term alternative to the cuts would be to assess all the state's hospitals and insurers an equivalent amount for the State Health Safety Net fund. A congressional stimulus package with increased federal Medicaid spending, as Representative Barney Frank has proposed, could help. But the state should find a way to ensure this year and in years to come that healthcare for all - the promise of the new law - does not fall victim to the recession.
------------
A BOSTON GLOBE EDITORIAL, "Code blue on healthcare costs", November 26, 2008
IN THE EARLY 1990s, Massachusetts shifted from hospital reimbursement rates set by a state agency to a deregulated system in which insurers and hospitals negotiated with each other. As a recent Globe Spotlight report detailed, two big winners have been Partners HealthCare's Massachusetts General Hospital and Brigham and Women's. They command disproportionately high reimbursements partly because they are highly regarded teaching hospitals that subsidize unique and costly facilities like their burn units, and partly because of sheer market muscle. No health insurer would dare to offer a plan that did not include them.
The deregulated system creates problems of equity and affordability. In some specialties, other teaching hospitals with medical outcomes just as good as the Partners hospitals must make do with lower reimbursements. For example, the Spotlight team found Mass. General charged nearly twice as much for an MRI of the brain as Tufts Medical Center.
Since 2000, insurance premiums in the state have increased 78 percent, while the cost of living has gone up 28.3 percent. Over-generous payments to Partners have also helped fund its outpatient empire-building in the suburbs, which is likely to exacerbate the equity imbalance as these newly minted Partners facilities presumably will garner higher reimbursements than local competitiors.
Other states have also seen substantial premium increases, but only Massachusetts has a new universal-coverage law that requires individuals to purchase insurance. The state needs a better rate-setting system to ensure that the reform law does not become the Big Dig of health insurance.
One alternative is to shift from the private dealing between insurers and hospitals to a more transparent system of performance-based reimbursements. These would have to account for complicated medical procedures. Or the state could set an allowable range for the cost of each procedure.
Ideally, rate-setting would move toward a single payment system: a gallbladder removal would be reimbursed at the same rate by a private insurer, Medicaid, or Medicare. Currently, Medicare pays somewhat less than actual cost, Medicaid much less, and the insurers subsidize both programs. Ending this disparity would benefit the hospitals with disproportionate shares of Medicaid and Medicare patients. A saner rate-setting system would also pay more for primary care and less for the interventions by specialists that inflate overall costs and lure medical students away from basic care.
A state health-cost bill this year set up a payment commission that will report next fall. It should recognize that the present system is not working, and devise a new one that controls cost and treats providers fairly.
------------
"Healthcare groups push for federal bailout funds"
By Kay Lazar, Boston Globe Staff, January 2, 2009
With a leafleting, lobbying, and letter-writing blitz, healthcare groups are urging Governor Deval Patrick to use expected federal bailout money to shore up health programs slashed this fall because of the state's budget crisis.
A coalition of three dozen social service, healthcare, labor, and legal groups - dubbed Put Patients First - is mailing 100,000 Boston area voters a flier about the specific effect of recent cuts to Boston Medical Center and Cambridge Health Alliance. The two institutions serve a large share of the region's low-income residents and, hospital officials say, are suffering from disproportionate state budget cuts.
The hospitals' troubles are just one example of how patient care will suffer from cuts, past and future, to the state's Medicaid budget, which funds health programs for children, the low-income, and the elderly, the coalition warns.
The jockeying for a share of the federal stimulus package, expected soon after President-elect Barack Obama takes office Jan. 20, comes as the recession tightens its grip on Massachusetts and Patrick prepares up to $1 billion in additional state budget cuts.
It also comes as Patrick is hinting that he may shift some funds the state previously earmarked for Medicaid programs to other ailing areas of the state budget - if, as hoped, Massachusetts receives additional Medicaid money in the federal package. At a press briefing this week, Patrick signaled the possibility that stimulus funds could free up state Medicaid money that could then be used elsewhere.
"We can displace that money for other needs," Patrick said to reporters during a Tuesday news briefing, after he explained the gist of discussions with federal officials about Medicaid.
"So then you could spend that money on something else in the budget to preserve other programs?" a reporter asked.
"Correct," the governor said.
An administration spokeswoman later said nothing definitive has been decided.
"At this point, it's premature to speculate about a stimulus package, how much support Massachusetts might receive, and how we might use those funds," Jennifer Kritz, spokeswoman for the Executive Office of Health and Human Services, said in an e-mailed statement. "We are awaiting details about a stimulus package, including [the Medicaid portion]. Until we know the details, it's simply too early to say."
Using earmarked Medicaid money in the stimulus package to justify transferring similar amounts of state Medicaid money to other uses would, coalition members say, mean little or no net increase to restore earlier cuts to health programs. That includes cuts to struggling community health centers, which depend heavily on state financing. Many centers are seeing an increasing number of patients who have lost jobs and their employer-paid health insurance, they said.
"Healthcare centers are reporting the impact of the cuts is forcing them to look at cutting core services, such as interpreters and front-line staff that make sure patients are being enrolled in health insurance they are eligible for," said coalition organizer Mike Fadel, who is executive director of 1199SEIU United Healthcare Workers East, a union that represents many community health center and hospital workers.
"At the end of the day, the governor is facing tough choices and too often the Medicaid budget has been looked at in a knee-jerk fashion as a large piece of the state's budget that could be cut," Fadel said. "As the economic crisis is taking its toll, this is not the moment to fray the safety net."
In addition to mass mailings and phone calls to the governor, the Put Patients First coalition is planning a State House rally on Jan. 15, five days before Obama takes office.
Cutbacks to healthcare, among the state's largest industries, could produce a "ripple effect, extending to nursing agencies, equipment suppliers, and other businesses that support hospitals," the Massachusetts Hospital Association warned in a recent letter to the governor. The letter noted there are 479,000 healthcare and social service jobs in Massachusetts.
Joe Kirkpatrick, the association's vice president for healthcare finance, said patients, particularly those with mental illnesses, will feel the effects of continued hospital cutbacks.
"Hospitals look at mental health because hospitals already take a loss in delivering this care and, if they are going to survive, that's where a lot of the cutbacks are going to occur. It's the less profitable areas that tend to get cut," he said. "And it's those behavioral problems that increase in times of recession."
-
Globe staff writer Matt Viser contributed to this story.
-
------------
-

-
The governor called the rise in rates unsustainable. (Globe Staff Photo / David L. Ryan)
-
"Patrick intensifies state's push to curb soaring health premiums"
By Marcella Bombardieri, Boston Globe Staff, January 6, 2009
Governor Deval Patrick yesterday accelerated his administration's efforts to control spiraling statewide healthcare costs, warning that rising premiums threaten to crush families and businesses and doom Massachusetts' groundbreaking experiment with universal insurance.
Patrick said officials are considering using state insurance regulations to block excessive healthcare premiums. He is also summoning leaders of insurance and hospital companies for meetings as soon as this week to ask for their "vigorous cooperation."
In response to stories by the Globe's Spotlight Team about the role of Partners HealthCare and Blue Cross Blue Shield of Massa chusetts in driving up costs, Patrick convened a panel of senior administration figures yesterday to coordinate new and existing state cost containment efforts, which he said should produce action by summer. He also said he expects to file new legislation.
"The increases at this rate over time [are] just not sustainable, not for families, not to business, not for government," Patrick said at a news conference after the summit.
Inspector General Gregory W. Sullivan also said he wants providers and insurers to delay signing new contracts until the administration has implemented new, as-yet-undetermined policies to limit premiums.
The Spotlight Team has reported, quoting officials directly involved in the negotiations, that the leaders of Partners and Blue Cross made a deal in 2000 in which Blue Cross significantly boosted its payments to Partners in exchange for Partners' insistence that all other insurers pay at least as much for the care of their members by Partners doctors. That prevented insurance companies from competing on price, and helped to drive up consumer prices statewide. Individual insurance premiums in Massachusetts have risen nearly 9 percent a year since 2000, twice the annual rate increase of the late 1990s.
The Spotlight Team has also reported that Partners hospitals are paid significantly more than other, comparable facilities.
Partners and Blue Cross say they did nothing improper. Both companies contend that payments to hospitals had been too low before the 2000 agreement, and Partners said its CEO promised only to treat all insurers equally.
Both companies also said yesterday that they look forward to participating in Patrick's discussions. Partners spokesman Rich Copp said in a statement that cost increases nationally "have been mirrored almost exactly" in Massachusetts. He also noted that Partners' latest contract with Blue Cross, settled over the summer, "resulted in rate increases well below those experienced in prior years." The contract calls for increases in payments of about 5 to 6 percent a year, roughly equivalent to medical inflation.
Blue Cross CEO Cleve L. Killingsworth Jr. expressed support in a statement for one proposal the administration is considering: reforming the payment system to compensate hospitals for patient outcomes, rather than for the number of procedures or visits.
Yesterday, Patrick declined to comment specifically on the role of either Partners or Blue Cross. He said he wants to examine cost containment from all angles. But he added: "We have to get at cost containment because these kinds of premium increases and the unevenness in the way various providers are compensated for similar services have to be addressed in order to assure the long-term viability of this grand experiment," a reference to healthcare reform.
Patrick also said that while a number of the cost containment measures he discussed yesterday have been underway for months, the Globe series "made me feel like I ought to make sure we're all on the same page, that we're taking account of all of the contributors, real or perceived, to cost increases. And I'm satisfied from the conversation we had that there's a lot of good work and it will come to fruition soon."
Among the ongoing efforts to examine costs Patrick cited are a study commissioned from the RAND Corporation, a think tank, on the feasibility of various reforms, and work by the state Health Care Quality and Cost Council, a body created by the healthcare reform law.
Patrick also highlighted the healthcare cost containment bill he signed in August, which was championed by Senate President Therese Murray. It created a payment reform commission, which he said will hold its first meeting next week.
However, Murray said yesterday that she is frustrated that Patrick has been slow to appoint members to that commission, which she said was supposed to start meeting Sept. 15. "I don't think the governor needs to reinvent the wheel," said Murray. "We established this commission on healthcare payment reform because it was already evident to us that Massachusetts had higher healthcare costs than everybody else."
State Senator Richard T. Moore, Senate chairman of the committee on healthcare financing, also wrote to Patrick last week, after the Globe reported the plan for yesterday's meeting, commending him for examining the role of Partners on the cost of healthcare. But Moore said that no official with recent ties to Partners should be part of the review team. Patrick's secretary of health and human services, Dr. JudyAnn Bigby, previously worked at Partners affiliate Brigham and Women's Hospital, and attended yesterday's meeting.
-
Jeffrey Krasner of the Globe staff contributed to this report.
-
------------
-

-
At the State House yesterday, Governor Deval Patrick spoke after conferring with officials about financing the state's healthcare system. He wants to examine cost containment from all angles. (Globe Staff Photo / David L. Ryan)
-
"Tufts to break with Blue Cross: Hospital takes high-risk step over doctor pay"
By Scott Allen and Jeffrey Krasner, Boston Globe Staff, January 6, 2009
Tufts Medical Center has begun warning thousands of patients that Tufts doctors will no longer accept Blue Cross Blue Shield HMO coverage after Jan. 31, asserting in a letter that the state's largest health insurer refuses to pay Tufts doctors at a "reasonable rate."
The medical center is asking its patients to contact Blue Cross directly to "express your frustration."
The unusual move carries enormous risks for Tufts as well as for patients, who may be faced with the difficult choice of changing insurance coverage or changing hospitals in the next few weeks. The last time a hospital took the drastic step of canceling a major insurance contract, in 2000, worried patients were caught in the middle and thousands switched insurance carriers so that they could stay with their doctors.
But Tufts officials said they had no choice but to begin phasing out Blue Cross coverage after 11 months of what Tufts described as fruitless negotiations with the company. Ellen Zane, Tufts Medical Center's chief executive, said that Blue Cross pays her doctors and hospital 20 to 40 percent less than other major teaching hospitals even though she said Blue Cross ranks Tufts among the top three teaching hospitals in Massachusetts for overall quality. Unless Blue Cross offers Tufts a major payment increase before the end of the month, the Blue Cross HMO contract with Tufts doctors will end on Feb. 1.
"We hope that Blue Cross comes to their senses," said Zane, adding that her hospital has lost $25 million treating Blue Cross patients over the past five years and is on a course to lose $10 million more this year. "The place has been grossly underfunded."
A spokesman for Blue Cross Blue Shield of Massachusetts, Jay McQuaide, called Zane's termination threat a "negotiating tactic" that puts patients in the crossfire. He said Blue Cross has offered Tufts pay increases similar to other hospitals and physician groups, but Tufts wants a much higher increase.
"We're disappointed the doctors have chosen to go in this direction," said McQuaide. He said termination of the contract would affect patients treated by about 210 Tufts doctors. However, Tufts officials said at least 475 Tufts physicians would stop accepting Blue Cross HMO coverage under Zane's plan.
Robert Laszewski, a national healthcare consultant, said such "scare-downs" will be more common as communities grapple with spiraling medical costs that now consume more than 16 percent of the national economy. Blue Cross officials have made similar predictions in the past.
"Boston is the highest healthcare cost market in the US, so something's got to give," said Laszewski, president of Health Policy and Strategy Associates LLC of Alexandria, Va., "You either keep talking about it or you start dealing with it."
But Stuart Altman, a healthcare economist at Brandeis University and a member of the Tufts board of trustees, said the dispute reflects the failure of the free market to assure high quality, affordable healthcare. He said all hospitals should be paid the same rate, adjusted for the quality of their work and the complexity of their patients' care. Instead, pay is largely determined by negotiating power.
"Tufts barely survives," he said. "Sure it could do a better job and be more efficient, but the reality is we're paid significantly less than other teaching hospitals."
Tufts Medical Center, founded in 1796 by Bostonians including Paul Revere and Sam Adams, is the principal teaching hospital for Tufts University School of Medicine. Located in Chinatown, the hospital treats a higher number of low-income patients than most other teaching hospitals in the city and, partly as a result, it has struggled financially. The hospital lost $21 million in 2004, but posted a $13.5 million profit the next year after Zane became CEO.
Tufts Medical Center has been one of the losers in the deregulation of healthcare over the last decade, lacking both the size and political clout to negotiate favorable insurance contracts that would give the hospital a financial cushion. Blue Cross rates obtained by the Globe show that Tufts Medical Center is paid about 32 percent less than Brigham and Women's and Massachusetts General hospitals in Boston and 19 percent less than Beth Israel Deaconess Medical Center. All three are Harvard Medical School teaching hospitals.
But doctors at Tufts Medical Center say that their hospital deserves more respect, noting that the hospital runs one of the region's largest heart transplant programs, trains more primary care doctors than any other hospital, and treats more low-income patients under the state Medicaid program than any other hospital except Boston Medical Center.
And they say that Blue Cross's own quality measures show Tufts performs better than many teaching hospitals that are paid much more. A Blue Cross report on hospital quality released last month ranked Tufts Medical Center along with Beth Israel Deaconess and Baystate Medical Center in Springfield at the top among 12 academic medical centers statewide, Tufts officials said. Other statistics show that, on average, Tufts cares for sicker patients than the other teaching hospitals.
Blue Cross officials say that there are a wide variety of ways to measure quality and they questioned whether Tufts should be considered part of the elite. "We have not seen data to support their contention that they are a high-quality provider," said McQuaide.
The showdown between the two sides has been building for nearly a year as Blue Cross tried to persuade Tufts to sign a new type of contract under which the doctors have to meet aggressive quality and cost-control goals to earn their full payment. Tufts officials said they embraced the idea of the contract, but needed significant claims information from Blue Cross to identify the best ways to save money - help that Tufts said was not forthcoming.
Blue Cross had hoped to keep talking, but, by yesterday morning, Zane had had enough. She phoned Blue Cross chief executive Cleve L. Killingsworth Jr. to inform him that she planned to terminate the Blue Cross HMO contract unless Blue Cross offered significantly more money. Patients covered by a type of Blue Cross insurance called "preferred provider organizations" could continue to see Tufts doctors after the termination, but might have to pay a higher copayment.
Zane acknowledged that the decision to end the Blue Cross contract was a "heavy moment," but it's one she has been through before. In 2000, as chief negotiator for Partners HealthCare, owner of Mass. General and the Brigham, Zane oversaw the cancellation of Partners' contract with another insurer, forcing the company to give Partners a big rate increase within a matter of days.
This time, Zane represents a smaller hospital without the resources of Partners. But doctors at Tufts Medical Center are hoping that Zane still has the upper hand in the battle for public support that lies ahead. As Dr. Paul Summergrad, chairman of the medical center's physician organization, said, "As far as I know, no one has ever been cured in the executive offices of Blue Cross Blue Shield."
------------
"Tufts Medical, Blue Cross negotiations break down: Patients face being rejected by doctors Feb. 1"
By Jeffrey Krasner, Boston Globe Staff, January 7, 2009
The breakdown in contract talks between Tufts Medical Center physicians and Blue Cross and Blue Shield of Massachusetts has thousands of patients fretting they may not be able to see trusted doctors, and scrambling to come up with alternate caregivers.
Tufts Medical Center and its physicians group Monday said they had been unable to reach an agreement with Blue Cross, the largest health insurer in the state, after 11 months of talks. Unless a solution can be quickly crafted, Tufts doctors will no longer accept Blue Cross members as of Feb. 1.
The hospital's contract with Blue Cross lasts through September. Tufts had sought to renew both at the same time, and for many patients, the inability to see a Tufts doctor effectively locks them out of the hospital.
"I am very, very upset," said Nick Azzolino, 57, who had a heart transplant at Tufts Medical Center in July 2006. Blue Cross "is saying to me if they can't come to terms with the doctors, then I'm on my own. They don't have patient care at the front of their priorities."
Azzolino, who runs a day care center in Carver with his wife, said he spent 10 days in the hospital last month when his body began retaining huge amounts of water. He is scheduled to meet with his cardiologist again Jan. 22.
But when he called Blue Cross yesterday, he said, he was told he could only get an extension to see his doctor for an additional three months - and only if the appointments were set up before the contract terminates at the end of the month.
"These are the people who foster my care," he said. "I need to be with them. If this thing doesn't get resolved, I'm going to have to just get the bills as they come in and submit them myself to Blue Cross."
A Blue Cross spokesman confirmed that HMO patients whose doctors' contracts end this month will have to pay medical bills out of their pocket or seek alternate care. The three-month extension applies only to those HMO members with special medical needs - such as the terminally ill or those with chronic conditions.
After that, "if the physician feels like he or she needs more time with the patients, he or she can call us and we can review it," said Jay McQuaide.
Members of Blue Cross's preferred provider organization, a more flexible type of insurance, can continue to see doctors who are terminated, but will have to pay 20 percent of the bill.
For some, that's not an option.
Elise Gardner of Winchester said she takes her four children to Woburn Pediatrics, a practice that is part of the Tufts doctors group.
"Twenty percent of an office visit is a lot," said Gardner. "Plus we're paying the monthly premium. With four kids, the last thing I want to worry about is my insurance company throwing a tantrum and not playing fair, which is what I try to teach my children."
Talks between Tufts and Blue Cross broke down Monday. The hospital and its affiliated doctors claim they are paid 20 to 40 percent less than comparable teaching hospitals in Boston. Tufts said it is asking for a 9 percent annual pay increase for three years for its doctors, to bring their rates more in line with the other hospitals.
Blue Cross did not dispute that Tufts is paid less.
"We have acknowledged there is an imbalance in rates paid to providers that can be because of market clout," said McQuaide. But Tufts can only get relief, he said, by signing up for the insurers' new payment system, in which hospitals get a basic payment for each patient and can earn additional revenue by meeting quality targets.
Both companies have set up hotlines to field calls from customers. Blue Cross's number is 888-404-9846; Tufts Medical Center's number is 888-953-3763. Tufts also has a website for patients, www.keepmydoc.org.
-
Jeffrey Krasner can be reached at krasner@globe.com.
-
------------
A BOSTON GLOBE EDITORIAL
"High stakes in health battle"
January 9, 2009
THE KNOCKDOWN fight between Tufts Medical Center and Blue Cross Blue Shield of Massachusetts over the reimbursement rate for doctors at the hospital is Exhibit B of the dysfunction of the state's health insurance system. Exhibit A, of course, is the much better rate that Partners HealthCare muscled Blue Cross into granting to its teaching hospitals, Mass. General and Brigham and Women's, in 2000. Two sides of the same coin, these deals cry out for reform.
Doctors who meet quality standards while handling complex cases at academic centers should get uniform reimbursement - not just from private insurers but from Medicaid and Medicare as well. Reformed rates should also better reward primary care.
But comprehensive changes will have to await action by a payment reform commission that the Legislature called for last year. Lamentably, that panel has yet to meet. In the meantime, Tufts said Monday that talks with Blue Cross, the state's largest insurer, had reached a stalemate. Starting Feb. 1, Tufts doctors will no longer take part in the Blue Cross HMO plan.
This is a drastic step for a hospital to take, with an impact on patients. Also, with the recession cutting into employers' and workers' ability to afford insurance of any kind, Tufts's bid for a Blue Cross rate increase well above the rate of inflation could be seen as the last thing the state needs.
But Tufts CEO Ellen Zane makes a good case that her hospital, with rates lower than the two Partners hospitals and Beth Israel Deaconess, treats difficult cases more efficiently than the other three. If Blue Cross's current rates for Tufts, which Tufts says are 32 to 35 percent below rates for Partners, cause doctors to switch - with their patients - to the other hospitals, the overall cost to the system would also rise.
Not all insurers do as Blue Cross does. Zane argues that the state's second-largest insurer, Harvard Pilgrim, reimburses more fairly. Blue Cross pays Tufts below the average for teaching hospitals in Boston, she says, and not enough to cover her costs. Blue Cross denies that.
Blue Cross has said it is willing to pay Tufts more if the hospital would sign its new alternative quality contract, which bases a portion of payment on performance quality and not just fee for service. However, the insurer has not imposed such a condition on the higher rates it pays to doctors at Partners.
Performance-based contracts are still relatively new in this state, and might become more attractive to Tufts - and a major part of a reformed payment system - if they prove themselves in the future. Until then, Tufts deserves a better deal from Blue Cross. And the state deserves a better payment system than the current one - a monument to inequity and inefficiency.
------------
"Patrick weighs insurance hearing: Healthcare leaders told to rein in costs"
By Marcella Bombardieri, Boston Globe Staff, January 13, 2009
Governor Deval Patrick yesterday asked the state's most prominent hospital and health insurance leaders to take quick action to hold down rapidly rising healthcare costs, suggesting that if they did not take steps on their own, they might face new government regulation.
Meeting with healthcare industry executives in response to recent articles by the Globe Spotlight Team about the cost of medical care, Patrick said he is considering holding hearings on health insurance premiums and the primary driver of premium increases - the rates hospitals charge insurers for members' medical care. Last week, he said the state Division of Insurance has the power to reject rates it deems excessive.
"Other governors haven't used this power, but he's telling them, 'I have this and tell me why I shouldn't use it,' " said state Inspector General Gregory W. Sullivan, who attended yesterday's meeting in Patrick's office.
Insurance executives at the meeting said they would welcome such an investigation, according to Charles D. Baker, chief executive of Harvard Pilgrim Health Care, the state's second-largest health insurer.
Sullivan asked the executives to refrain from signing new contracts that cover patient care beyond this year until the government has time to consider potential reform measures. The inspector general singled out the largest private contract in Massachusetts healthcare, between the state's dominant provider, Partners HealthCare, and its largest insurer, Blue Cross and Blue Shield of Massachusetts.
The two agreed last summer to a multiyear contract that calls for annual rate increases of about 5 to 6 percent. Spokesmen for Partners and Blue Cross said yesterday the agreement was final.
Still, Sullivan said he believes unforeseen circumstances - such as state insurance hearings - would be grounds for the two companies to revise or suspend their deal.
After the meeting, several executives said they will support a new payment reform commission about to begin meeting, but they did not promise any other immediate action or changes. The commission, created by legislation Senate President Therese Murray spearheaded last year, will examine alternatives to the traditional payment model in healthcare. Many insurance executives and healthcare reformers argue that providers should be paid for healthy outcomes, not as they are now - based on the number of tests and procedures they perform on patients.
Dr. James J. Mongan, chief executive of Partners, said Patrick "understands [healthcare costs] are national issues, but the state of Massachusetts showed it could lead on national issues with [healthcare] coverage and it's going to try and lead on national issues with costs."
Baker said Patrick "made clear that this is sort of a today issue, not a tomorrow issue, but in a room with 30 people it's hard to pursue specific commitments in front of everybody else."
"It was more about expressing urgency and seeking aggressive participation," he added. "I think he got the right answers from everybody."
The Spotlight Team reported recently that Partners and Blue Cross made a deal in 2000 that called for major increases in what Blue Cross would pay for the services of Partners, the parent company of Brigham and Women's and Massachusetts General hospitals. In exchange, Partners would insist on receiving payments from other insurers that were at least equal. Healthcare costs have risen dramatically since that time.
Tufts Medical Center said last week it would soon stop accepting Blue Cross insurance because the company will not pay reasonable rates, while Blue Cross says demands for higher payments by Tufts would increase healthcare costs. Blue Cross rates obtained by the Globe show Tufts is paid about 32 percent less than Mass. General or Brigham and Women's.
-
Marcella Bombardieri can be reached at bombardieri@globe.com.
-
------------
"Drug costs soar for seniors: Cut in state funding boosts copayments"
By Kay Lazar, Boston Globe Staff, January 14, 2009
Tens of thousands of Bay State seniors are facing steep increases in the cost of their prescription drug copayments, the result of an $11 million cut in a state-funded program that, until Jan. 1, helped to defray their pharmacy costs.
More than 44,000 senior citizens are affected by the cuts in the Prescription Advantage program, with many seeing their copayments double or triple, officials said.
As a result, some seniors are simply leaving their prescriptions on the pharmacy counter, rather than pay a price they feel they can't afford, said Mary Sullivan, a pharmacist and director of MassMedLine, a nonprofit organization run by the Massachusetts College of Pharmacy and Health Sciences.
"I am selling everything I can on eBay to help pay for these drugs," said Ralph F. Van Dean, a 77-year-old Swampscott resident who said he was hit with a $793 copayment Jan. 4 for four medications for his wife, Nina, who suffers from a chronic lung disease. Previously, he said, the copayment for the four drugs would have been about $50, because the Prescription Advantage program covered what Medicare did not.
The cuts in the Prescription Advantage program were part of the $1 billion cut the Patrick administration made in October, as the recession began eating into state revenues.
Kristina Barry, a spokeswoman for the Executive Office of Health and Human Services, said it was a "difficult decision" to make the cuts, but a necessary one.
Many seniors apparently did not realize how they would be affected by the program cuts, despite mass mailings by the state and outreach by advocacy groups in November and December.
"They are calling us when they reach the pharmacy and realize their [prescription] plans are not what they expected," said Sulllivan, of MassMedLine. Calls to the organization's hotline are running at double the normal volume, she said.
For years, the state-funded Prescription Advantage program has helped seniors who met income-eligibility requirements with copayments for their medicines. That aid has been available with no requirement that seniors first pay a set amount out of pocket before the assistance kicks in. But now state assistance with copayments will not be available until $2,700 has been spent yearly on covered prescription drugs by the enrollee and Medicare, combined.
"The pain will go away once they reach the $2,700, but it will be a heck of a lot of pain until then," said Deborah Banda, state director of AARP Massachusetts. "The vast majority of these people are on fixed incomes."
The Executive Office of Elder Affairs has been trying to ease the effects of higher copayment by sending out information to seniors statewide. The state will hold "over 100 statewide informational seminars about the changes, as well as briefing senior centers, pharmacists, and senior counselors," said Barry.
With the state still facing a substantial budget gap and Governor Deval Patrick warning that another round of cuts is likely, advocates for seniors say most can not shoulder more increases in medication costs.
"We know this is a difficult time all across the board, but we just feel this program has taken the biggest hit it can right now without jeopardizing the health of some of our most vulnerable residents," said Banda of AARP.
"Prescription drugs keep people healthy and away from more expensive care," she said. "If people are cutting back because they can't afford these costs, they may stop taking their prescriptions, and they may end up at emergency rooms all over the state."
Van Dean, the Swampscott senior who is caring for his wife, is himself fighting prostate cancer and recovering from a stroke, so he, too, is taking several medications. He gets help from the Veterans Administration with his prescription copayments.
Faced with cuts in the Prescription Advantage program, Van Dean called MassMedLine to help him switch to a Medicare plan with better coverage for his wife's medications, reducing that $793 copayment to about $150. That switch was made last week.
But, he said, he and his wife will still be scrimping to cover the higher copayments for her medications for about three months, until they hit the $2,700 limit. Then, her copayments with Prescription Advantage assistance will revert to $7 for generic medications and $18 for brand name ones.
"We live on our Social Security now, and that barely covers what our expenses are, especially with the heat," he said, adding that the cost of medications "can wipe us out."
Massachusetts residents can call MassMedLine at 866-633-1617 for free assistance with questions about drug coverage.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Health care tinkering"
The Berkshire Eagle, Editorial, Thursday, January 15, 2009
We appreciate Governor Deval L. Patrick going to the bully pulpit in an effort to hold down rapidly rising health care costs, but we don't see the health insurance industry responding to threats, and reform measures are self-limiting because of the inherent flaws in a system tied to the profit margins of insurers. The way in which we pay for health care requires a complete overhaul.
The governor is considering holding hearings on skyrocketing health insurance premiums and the rates hospitals charge insurers for members' medical care, which is driving higher premiums. In a meeting with industry executives Monday, Mr. Patrick indicated he would introduce tougher regulations and/or urge the state Division of Insurance to reject rates it regards as excessive, a power the executive office rarely exercises, if the industry doesn't bring down costs itself.
The meeting hosted by the governor came in the wake of a Boston Globe report that Blue Cross and Blue Shield of Massachusetts, the state's largest insurer, agreed in 2000 that it would pay more for the services of Partners HealthCare, the state's largest provider, if Partners in turn insisted on receiving comparable payments from Blue Cross' smaller rivals. This cozy arrangement has helped fuel health care costs for residents for nearly nine years.
There is only so much tinkering that can be done to fix a broken health care system that has been sabotaged by corporate providers and insurers experienced at gaming that system to benefit their bottom lines — and the bank accounts of overpaid CEOs. Introduction of a single-payer, government-run but privately administered health care system that puts the interests of patients before the profit margins of bureaucrats is the only meaningful reform.
------------
"Partners, insurer under scrutiny: AG seeks details on agreement; Possible collusion over prices cited"
By Scott Allen and Thomas Farragher, Boston Globe Staff, January 23, 2009
Attorney General Martha Coakley has launched an investigation into whether the state's largest health insurance company and its largest healthcare provider may have illegally colluded to increase the price of health insurance statewide over the last nine years, according to several legal and government sources.
The attorney general sent formal demands for information to Blue Cross and Blue Shield of Massachusetts and Partners HealthCare late last week, the sources say, calling for a detailed account of their contract negotiations in recent years.
Since 2000, Blue Cross has boosted the rate it pays for medical care by Partners doctors and hospitals by 75 percent, dramatically more than the increases given to most other Massachusetts hospitals. Blue Cross now pays $2 billion a year to Partners, parent company of Massachusetts General and Brigham and Women's hospitals.
Coakley's investigation comes just weeks after the Globe Spotlight Team reported that the leaders of Partners and Blue Cross made a private agreement in 2000 under which Blue Cross would give Partners a significant increase in payments as long as Partners obtained similarly big pay increases from Blue Cross's competitors. The deal - never written down because Partners lawyers feared that the agreement was legally risky - required Blue Cross and its competitors to raise insurance premiums to pay Partners, ushering in a decade of rapidly escalating healthcare costs.
State Inspector General Gregory W. Sullivan called the attorney general's probe "historically significant."
"The attorney general is fulfilling an important role by examining the concentration of market power by major medical providers and insurers on the cost of healthcare to consumers in Massachusetts," said Sullivan, who has pushed for a public review of whether hospitals and insurance companies use market power to increase prices.
A spokeswoman for the attorney general declined to comment on the investigation, but Coakley has increased oversight of hospitals and insurance companies since assuming office in 2007, saying she was concerned about the market power of some insurers and hospitals. After the Spotlight story appeared late last month, Coakley said: "We will continue to monitor Partners' expansion plans and will take action as appropriate regarding Partners' market behavior."
Partners and Blue Cross officials say they have done nothing wrong and that the real drivers of the 78 percent increase in Massachusetts insurance premiums since 2000 are factors such as new medical technology and the growing incidence of chronic diseases such as diabetes. Both acknowledge that Partners price hikes in 2000 helped start a trend toward rising insurance rates, but say the higher pay to Partners and other hospitals was necessary so that the company could meet its own rising costs.
Dr. James J. Mongan, Partners chief executive, denies that Partners has driven up healthcare costs disproportionately, arguing that his eight hospitals and more than 40,000 employees are caught in a national trend toward higher costs. Mongan has said that insurance rates in Massachusetts have gone up at roughly the same rate as the national average.
Yesterday, Blue Cross and Partners officials declined to comment on the investigation.
But the report by the Spotlight Team in November that Blue Cross typically pays Partners' flagship hospitals, the Brigham and Mass General, 30 percent more than other teaching hospitals that mainly treat adults has focused debate on the disproportionate cost of Partners, which treats 1.7 million patients. Though the Partners teaching hospitals have excellent reputations for quality, quality data does not show they consistently achieve better results than other, less well paid hospitals such as Beth Israel Deaconess Medical Center.
Partners now makes hundreds of millions of dollars from its contracts with insurers while some other hospitals say they actually lose money every time they treat a Blue Cross member. Underscoring the point, doctors at Tufts Medical Center had announced plans to stop accepting Blue Cross HMO insurance after Jan. 31, but relented when Blue Cross agreed to a significant payment increase to offset what Tufts said were big losses.
Donald J. Thieme, executive director of the Massachusetts Council of Community Hospitals, said the 23 hospitals he represents welcome Coakley's investigation. . Thieme said his organization submitted legislation seeking a formal review by the attorney general's office into anticompetitive behavior between hospitals and insurers.
Though the agreement was never disclosed publicly, its consequences were clear: a few months later, Partners announced plans to stop accepting Tufts HMO insurance after Partners negotiators determined the offer to Partners was not enough to "match Blue Cross," according to a 2000 Partners memo reviewed by the Globe.
"Everybody wished they had the same handshake," Thieme said. When the difference in rates paid to Partners and others was reported by the Globe and then by the state Health Care Quality and Cost Council website, he added, "A lot of our members were shocked at the degree of difference that existed."
The type of agreement that Partners and Blue Cross forged in 2000, known as a "most favored nation" agreement, is not automatically illegal, but such deals so often lead to higher prices that most-favored-nation agreements have been banned in several states, including New Hampshire and Rhode Island.
In this case, Blue Cross chief executive William Van Faasen feared that if he gave Partners the extra $193 million the company wanted over three years, Blue Cross insurance might become more expensive compared to the competition. But Dr. Samuel O. Thier, then the Partners chief, promised to seek similar increases from Blue Cross rivals, easing Van Faasen's fear about price competition.
Keith Hylton, a law professor at Boston University who has written a book on antitrust law, said that Coakley would have the option of taking legal action under either federal antitrust or state consumer protection law, which should worry Blue Cross or Partners. He said the federal law governing anticompetitive behavior by companies, know as the Sherman Act, allows prosecutors to recover three times the damage caused by the anticompetitive behavior.
"The concerning thing here is that antitrust laws are so serious in this country," said Hylton, who believes Coakley did the right thing by launching the investigation. He had this advice for Partners and Blue Cross: "They need to talk to lawyers."
Skyrocketing healthcare costs are under more scrutiny than ever in Massachusetts, partly because the success of the state's new health insurance mandate depends on controlling medical costs. The state has budgeted $869 million this year to pay for subsidized insurance. The governor and several groups have begun attacking the problem in the last month and are hoping to recommend solutions this year.
Governor Deval Patrick called a meeting of providers and payers on Jan. 12, during which he said he could resume state regulation of health insurance rates if people in the industry could not resolve the cost crisis.
-
Jeffrey Krasner, Marcella Bombardieri, and Liz Kowalczyk of the Globe staff contributed to this report.
-
------------
The Boston Globe, Op-Ed, REGINA HERZLINGER
"Creating a real healthcare market"
By Regina Herzlinger, February 18, 2009
MASSACHUSETTS healthcare costs are a problem. The state has virtually the highest costs in the country and insurance premiums that rise more rapidly than national rates. The state's near-universal health coverage shows that no good deed goes unpunished: As the state lowered the number of uninsured, costs increased.
After the Globe reported that Partners hospital system attained higher prices based primarily on its clout with insurers, Attorney General Martha Coakley began an anti-trust investigation. But the remedies will be a long time coming should she decide to prosecute and then win her case.
To spur more immediate solutions, a memo written last summer by former governor Michael Dukakis urged the return of the halcyon days of the 1970s and 1980s, when Massachusetts regulated hospital fees for services and construction. Although most economic reviews of this regulation had reached negative or uncertain conclusions about its impact, and these regulatory schemes have been mostly dismantled, some argue that the problem may not have been with the regulation per se, but rather in its limitation only to hospitals. The memorandum advocated that the state regulate all health insurance premiums - essentially a single payer system. It concluded that ". . .it should be unmistakably clear by this time that market forces don't work in healthcare."
Nothing could be further from the truth.
Real markets, like those for computers or cars, feature many competitors who offer differentiated products, and consumers who search for the best value. Innovators easily enter the market. Consumers separate the good from the bad with readily available information about quality and prices. They use it to reward the good guys and penalize the bad. That is why the Digital Equipment Corporation is no longer among us.
These conditions are absent in the Massachusetts healthcare market. Boston hospitals form an oligopoly, dominated by an almost monopolist Partners Healthcare, which last year earned around half a billion dollars in profits. As for health insurance, many employers offer a choice of one - or a choice of firms with virtually identical policies. And if you need an operation, there's no way to learn about histories and prices of potential surgeons.
If this is a market, I am Angelina Jolie.
In the long run, the appropriate role for governments in controlling healthcare costs is to use their existing powers to correct these problems through vigorous prosecution of antitrust and the provision of relevant information.
There is a more immediate solution, however. Insurers could require integrated hospital systems to give fixed price bids for providing all the care needed for specific chronic diseases or disabilities, such as Type II diabetes and high-risk pregnancies. Insurers would offer these bids to consumers. They could, for example, choose hospital A's diabetic team in preference to hospital B's, which costs $500 more a year. The effectiveness of such integrated networks is illustrated by Duke Medical Center's congestive heart program. In one year, it lowered costs by an astonishing 40 percent by improving the health of its patients through innovative procedures that decreased the number of hospital visits.
Our oligopolistic hospitals could create these teams. After all, they own all the resources needed to provide this care, and they have sprawled into convenient neighborhood locations. These integrated facilities (which I call focused factories) are feasible even in small areas. For example, if 10 percent of a town is diabetic and the average diabetic costs $10,000 a year, an area of only 50,000 residents could support $50 million of competitive diabetes-focused factories. In addition, transparency about the quality of care for a disease or a disability could be more easily attained from these focused teams eager to demonstrate the competitive excellence of their care. Accordingly, consumers, armed with relevant information, would pick those facilities that give them the best value for their money.
And here's another bonus. Because these teams would effectively and efficiently treat those with chronic illnesses, which normally account for at least 75 percent of healthcare costs, this would give the Commonwealth a shot at finally controlling expenses while improving quality - a potent combination.
What do you prefer: giving more power to the state government, which fiddled while Massachusetts healthcare burned, or a transparent consumer-based healthcare system based on real market forces?
-
Regina Herzlinger is a professor of business administration at Harvard Business School and author of "Who Killed Health Care?"
-
------------
"US state health system is tested by recession"
By Steve LeBlanc, Associated Press Writer, February 23, 2009
BOSTON --Massachusetts' pioneering health care system, which requires nearly everyone to carry insurance or face fines, is about to be put to the test by the bad U.S. economy.
Unemployment in the state has climbed over the past three years from around 4.8 percent to close to 7 percent, meaning 72,000 more people are out of work now than when the law was signed in 2006. Many of the newly jobless may have to buy their own insurance.
Will they do it? Will the state penalize those who don't? And will this recession-battered state be able to bear the added costs of supporting the program?
With the Obama administration hoping to expand health care nationally, the fate of Massachusetts' program is being watched closely.
"People are going to be watching how it fares in the recession and how resilient it is and whether people will continue to be able to afford health care when they face other economic pressures," said Drew Altman, president of the Kaiser Family Foundation, a health policy think tank.
Officials said they are confident those who have lost their jobs will do the right thing and obtain insurance. The law guarantees virtually free insurance for the poorest of the poor, creates subsidized plans for those making up to three times the poverty level, and offers lower-cost private coverage for those earning more.
"The fact that Massachusetts has so many options for people to obtain and maintain health care is a great comfort," said Leslie Kirwan, head of the Health Care Connector Authority Board, which oversees the law.
For example, a family of four earning $42,400 in the Boston area could get a subsidized health care plan for a premium of $39 a month. A Boston family of four who earn too much to qualify for a subsidy can get a basic private plan for about $766 a month.
Also, for some people who have lost their jobs, the state covers nearly the entire cost of maintaining their insurance as long as they are collecting unemployment, which lasts up to 46 weeks in Massachusetts.
People who fail to obtain insurance can be hit with fines that could top $1,000 for an individual during the 2009 tax year. The fine is deducted from the individual's annual tax refund. If the refund isn't enough to cover the fine, the state bills the taxpayer for the balance.
About 60,000 people had to pay a penalty for not having insurance in tax year 2007, according to the state Revenue Department. The penalty for that year was $219 for an individual.
A report by the Revenue Department in December found that in 2007 only 1.4 percent of tax filers required to have insurance failed to have it.
In this economy, the state is getting ready for an increase in the number of people relying on subsidized plans.
The current budget projected spending of $820 million to cover 164,000 people in subsidized plans. Democratic Gov. Deval Patrick's proposed budget for the fiscal year that starts on July 1 would increase spending to $880 million to cover up to 180,000.
The governor and the top two leaders in the Legislature have said they are committed to maintaining the program, despite the need for billions in spending cuts in other programs to bring this year's budget and next year's into balance.
But others in Massachusetts say it is time to rethink the mandate, given the rising number of unemployed.
-
On the Net:
Massachusetts Division of Unemployment Assistance: http://www.mass.gov/dua
Massachusetts Health Care Connector: http://www.mahealthconnector.org
-
------------
"Study: Massachusetts Health Reform is a Failed Model"
Les Masterson, for HealthLeaders Media, healthplans.hcpro.com, February 19, 2009
The single-payer healthcare system was once the reform flavor of the moment, but it has been largely pushed to the rear and replaced by talk of a public insurance option and individual mandate.
Massachusetts' healthcare reform, which included an individual mandate that required residents to purchase insurance, has increased coverage, but critics charge that the plan has not decreased costs or improved access to care.
In a study released Wednesday, two organizations say the Massachusetts health system is a failure and national policymakers should not look to that model as a possible solution. Instead, they propose a single-payer "Medicare for all" system as a better alternative.
Physicians for a National Health Program and Public Citizen, which support a single-payer health system, charged the Massachusetts project has not covered as many people as claimed, not contained costs, and hurt safety-net providers like public hospitals and community clinics.
In fact, the individual mandate is merely a "new tax on the uninsured," according to the study.
"We are facing a healthcare crisis in this country because private insurers are driving up costs with unnecessary overhead, bloated executive salaries, and an unquenchable quest for profits--all at the expense of American consumers," says Sidney Wolfe, MD, director of Public Citizen's Health Research Group in Washington, DC, at a press conference announcing the study Wednesday. "Massachusetts' failed attempt at reform is little more than a repeat of experiments that haven't worked in other states. To repeat that model on a national scale would be nothing short of Einstein's definition of insanity."
The reform law, which was enacted in 2006 with unanimous support from the Democratic-controlled Massachusetts Legislature and then Republican Governor Mitt Romney, requires residents to have health insurance and fines businesses that do not provide coverage.
In the study, the two groups said the individual mandate meant more business for health insurers, but didn't address administrative costs associated with private health insurance. In fact, the Massachusetts Connector, which was created to promote the program and help link people to the health plan options, adds 4-5 percentage points to private insurer policies, according to the study.
Though the reform has added to the number of insured residents in the commonwealth, the study's authors said the total is not as high as promoted. The Urban Institute found that 2.6% of Massachusetts respondents said they were uninsured in a mid-2008 phone survey. However, two other sources claim the percentage is about twice that number, according to the study.
Jon Kingsdale, executive director of the Massachusetts Connector, says Wednesday the state is confident with the 2.6% figure because they went "to great lengths" to accurately survey the uninsured.
"This low level of uninsured is consistent with the stated goal of health reform to achieve near-universal coverage and is only a point or so above the uninsurance rates reported by many European countries with so-called universal access," says Kingsdale.
.
Rising costs
The study's authors say another problem with the initial Massachusetts reform is that it did not address rising healthcare costs. Healthcare costs, in turn, will increase from $1.1 billion in fiscal 2008 to $1.3 billion in fiscal 2009.
On the flip side, if the state had created a public single-payer system, it could save about $8-$10 billion annually through reduced insurer administrative costs, which could go to covering uninsured residents and improving coverage for those with health insurance, according to the study.
The major problem is that policymakers created incremental healthcare reform while maintaining the same private health insurance system, says Rachel Nardin, MD, president of the Massachusetts chapter of Physicians for a National Health Program, assistant professor of neurology at Harvard Medical School, and study co-author.
"It is very hard to have effective cost control in incremental reform because it's piecemeal," says Nardin. "I think that is an extremely important lesson for national reform that comes from Massachusetts."
Kingsdale disagrees with that analysis. He says the $1.3 billion projection is from an outdated financial statement and is not actual costs. In fact, the state now projects costs to come in at about $800 million in the current fiscal year—not the $1.3 billion figure cited.
.
Barriers to care
To help offset state budget constraints and fund the rising costs of the health reform, Governor Deval Patrick last fall reduced funding to safety-net providers, such as public hospitals and community clinics. This has forced at least six community clinics to close and hospitals to cut the number of inpatient psychiatry beds.
This is an example of why insurance does not equal universal access to care, says Nardin.
"These safety-net services, which often lose money for hospitals even when patients have good insurance, include emergency care, chronic mental healthcare, and primary care. The public hospital where I work is busier than ever, but has just announced that it will close six community clinics, and about half of its inpatient psychiatry beds—despite critical shortages of primary care and psychiatric services," says Nardin.
Many Massachusetts residents are still underinsured. In fact, those who once used the free care system now must pay copays for medication and care, says Nardin.
One reason why the Massachusetts system, and previous state plans, failed is that the reforms maintain the private health insurance system. The reforms are incremental and merely add new public subsidies or expand Medicaid. "It is time to wake up from this insanity and enact single-payer health insurance for all," says Wolfe.
Canadian model
While opposing the Massachusetts model, the study's authors also promoted the United States National Health Care Act, which is a bill in Congress that would implement a single-payer system without private insurers.
The single-payer advocates support a system similar to the one in Canada. By eliminating private insurance overhead while spending the same amount on healthcare, the U.S. would avoid waiting lists and shortages that have been an issue in our neighbor to the north, which spends much less on healthcare, says Steffie Woolhander, MD, co-founder of Physicians for a National Health Program, associate professor of medicine at Harvard Medical School, and study co-author.
In announcing its findings, the two groups also presented an open letter to Sen. Edward Kennedy that was signed by more than 500 Massachusetts physicians and other health professionals to urge him to reject the Massachusetts model and support the single-payer system.
Responding to the study, Ian Duncan, FSA, FIA, FCIA, MAAA, a board member of the Commonwealth Health Insurance Connector Authority Board and founder and president of Solucia Inc., a Hartford-CT based consultant for the healthcare financing industry, tells HealthLeaders Media the scale of the health system problem is so great that he is not surprised that Massachusetts' experiment has faced obstacles.
Duncan adds the reform has created a "remarkable collaborative achievement on the part of the stakeholders."
"Massachusetts has achieved a remarkably low rate of uninsurance while encouraging the best aspect of the market (private bargaining between employers, employees, providers, and government payers) without some of the faults that we see too often in government systems," says Duncan.
-
Les Masterson is senior editor of Health Plan Insider. He can be reached at lmasterson@healthleadersmedia.com.
-
------------
"Sickened by healthcare executives' pay"
The Boston Globe, Letters, March 6, 2009
ALL WE have to do is take one look at health insurance executive pay to understand why healthcare in America is not available to all ("Blue Cross CEO's pay rose 26%," Business, Feb. 28). I had to drop my COBRA plan with Blue Cross last year, and switch to an indemnity plan with less coverage, because the monthly payment would have resembled a mortgage payment. When will politicians understand that healthcare for all is not something you mandate with the threat of a fine, but rather an equitable service administered fairly across the board?
Does Cleve Killingsworth, chief executive of Blue Cross and Blue Shield of Massachusetts, really work 50 times harder than I do? I doubt it. I'm holding down three jobs to pay the bills (health insurance being one of the largest), leaving me with still enormous out-of-pocket expenses.
The burden of ballooning healthcare costs is bleeding the American worker dry, and the folks responsible for its excesses are being rewarded to the tune of millions.
Is this America? Perhaps it is time to move back to France.
Jean Dunoyer
Watertown, Massachusetts
-
Link to news article: www.boston.com/business/healthcare/articles/2009/02/28/blue_cross_ceos_pay_rose_26/
-
------------
"Boost to health coverage planned: State seeks to assist ranks of unemployed"
By Elizabeth Cooney, Boston Globe Correspondent, March 9, 2009
Massachusetts will combine federal stimulus money with an existing state assistance program so that thousands of unemployed residents will be able to get health insurance at a small fraction of the usual cost, state officials are expected to announce today.
A program called COBRA has long allowed people to keep their employer-provided health coverage when they lose their jobs, but without the employer picking up part of the tab, many workers were unable to pay the premiums. To make insurance more affordable for the unemployed, the federal stimulus package signed into law last month pays nearly two-thirds of the cost of health insurance for nine months.
Massachusetts already has its own program to help cover COBRA costs for low- and some middle-income unemployed people. Now Massachusetts will combine its program with the federal initiative, using state money to offset the remaining one-third of a family's premium costs not covered by the federal benefit.
The net effect is that the COBRA benefits will be stretched farther. Payments for families earning no more than $84,000 will be as low as $70 a month for family insurance plans that begin at $1,000.
With the move, Massachusetts continues as one of the most generous states in providing health insurance assistance to laid-off workers. "We think this is going to be a tremendous benefit to unemployed folks who had a health plan subject to COBRA," said Suzanne M. Bump, state secretary of Labor and Workforce Development. "Even under the Medical Security Program there were a lot of folks who still couldn't exercise their COBRA options. This can really help bridge the gap."
The 20-year-old Medical Security Program - funded by a tax on employers - is a separate program that helps unemployed people whose income does not exceed $84,000, or 400 percent of the federal poverty limit of $21,000 for a family of four. As of January, 17,803 workers and family members get their health insurance this way, nearly double the number in January 2008.
Although some of those families had the option of continuing their workplace coverage through COBRA, they could not afford the upfront premiums of $1,000 or more and turned to the Medical Security Program for help. The new subsidy plan being announced today is expected to put healthcare under COBRA within reach, said Gerald A. McDonough, general counsel of the state labor department.
Families will be able to stay covered under their former workplace insurance plans by paying as little as $350 a month in advance, with $280 of that reimbursed later.
A spokesman for the Boston-based advocacy program Health Care For All applauded the newly combined efforts of the state and federal COBRA programs.
"We are really pleased with the decision to layer both the federal assistance with state assistance to provide maximal benefits to low-income people who are struggling to find jobs after being laid off," said research director Brian Rosman. "One thing we know is that when people lose their jobs, their medical needs don't go away."
He said his office has been inundated with calls from people losing their jobs who want to know more about the Medical Security Program and the new COBRA assistance. The state's 2006 law mandating near universal health insurance coverage imposes a penalty on people who go without insurance for more than three months.
The federal COBRA program is designed to avoid interruptions in coverage by allowing workers and their families to keep their health insurance after leaving an employer's plan for a variety of reasons, including an employee's job loss, death, or divorce. The subsidy created by the federal stimulus package covers people losing their jobs between Sept. 1, 2008, and before Dec. 31, 2009.
It comes with some income limitations: Benefits begin to decrease for individuals starting when their income hits $125,000 a year, and for couples when their income reaches $250,000. The benefits are not available for individuals with incomes over $145,000 and couples with income over $290,000.
The benefit is not retroactive, but it does reopen the 60-day window for selecting COBRA coverage. Employers will be required to send letters offering COBRA again to laid-off workers who may have declined it, dating back to September. People on COBRA will also be notified by their former employers.
-
Elizabeth Cooney can be reached at lizcooney@gmail.com
-
------------
"State may not boost healthcare premiums"
By Kay Lazar, Boston Globe Staff, March 12, 2009
Tens of thousands of residents who receive state-subsidized healthcare will avoid any increase in monthly premium costs this year, and some may even pay less, under a plan to be voted on today by state regulators.
Secretary of Administration and Finance Leslie Kirwan confirmed late yesterday that her staff will recommend that the Connector Authority board approve the no-increase measure because of the "severe economic environment."
The proposal has wide backing by board members, Kirwan said.
"This is bucking a trend that has been a really serious concern," she said. Last year, regulators approved a 10 percent increase.
If approved by the 10-member board, consumers in the Commonwealth Care program, roughly 164,000 low-income people, will not pay more for their health insurance, starting July 1, if they choose the lowest-cost plans in the program.
Many who choose higher-cost plans may even see their monthly bills decrease, Kirwan said.
The state's landmark health insurance initiative requires nearly everyone to have insurance, if they can afford it. The law allows exemptions for some residents who make too much to qualify for state-subsidized care but not enough to afford private coverage.
The board is expected to address these consumers as well today. It will decide on a formula that would be more generous this year than last in determining who qualifies for that exemption. People who do not have an exemption and who fail to buy health insurance, face a stiff tax penalty.
One of the state's largest consumer groups applauded the news.
"There is only so much of a burden folks in this economic category can afford, and the administration is paying attention," said the Rev. Hurmon Hamilton, senior pastor of Roxbury Presbyterian Church and president of the Greater Boston Interfaith Organization.
The affordability proposal before the Connector Authority board today is one of two major issues it will face. The other is a proposed joint venture by Caritas Christi Health Care network, affiliated with the Catholic Archdiocese of Boston, and a nonreligious company, Centene Corp., to provide insurance in the Commonwealth Care program.
The venture has drawn fire from both sides of the political spectrum because of questions about how the Catholic-affiliated entity will handle reproductive services, such as abortion, contraception, and sterilizations.
Abortion foes have decried the venture as an "appalling betrayal of Catholic principles," while abortion rights and civil rights groups expressed concerns about hurdles low-income women may face in getting reproductive care after studying problems at a similar, though not identical, Catholic-affiliated managed care system in New York.
Caritas issued an initial statement saying its venture would cover a full range of "confidential family planning services," but declined to elaborate. The Archdiocese later said it would not "in any way participate in actions that are contrary to Catholic moral teaching."
Late yesterday, a spokeswoman for the Caritas-Centene venture issued an additional statement that explained how Centene handles similar situations in other states.
"If a provider does not perform certain medical services, that provider directs patients back to the health plan. Our health plans have local staff and 1-800 numbers available 24/7 for access to information on all services provided," it said. "This number and information about all services are readily available online and in printed materials. In Massachusetts, we will apply these same procedures."
-
Kay Lazar can be reached at klazar@globe.com
-
------------
"State bans drug firm gifts to doctors: Disclosure of fees for consulting mandated"
By Liz Kowalczyk, Boston Globe Staff, March 12, 2009
State officials gave final approval yesterday to regulations banning pharmaceutical and medical device companies from providing gifts to physicians, limiting when companies can pay for doctors' meals, and requiring companies to publicly disclose payments to doctors over $50 for certain types of consulting and speaking engagements.
Drug, biotechnology, and device companies, the hotel and convention industry, doctors and consumer groups had pushed for changes to the rules, but the final language is close to what the staff of the Department of Public Health proposed in December.
There are two substantive changes, however. Companies will have to disclose payments to doctors and hospitals for research designed to promote a particular product, sometimes called "seeding trials"; funding for research aimed at answering a scientific question will still not have to be disclosed.
Also, the department eliminated a provision allowing companies to provide financial assistance for medical residents and other trainees to attend conferences and education courses.
Health officials said the rules are the most comprehensive in the nation; Massachusetts is now the only state to require disclosure by device makers, as well as drug companies, and just one of two states to make disclosures public, officials said.
"We think this is a victory for consumers," said Amy Whitcomb Slemmer, executive director of Health Care For All, a Boston-based consumer advocacy group. "They will know more about the full relationship between industry and their provider."
The regulations, approved by the Public Health Council, are intended to implement a law passed last summer to restrict interactions between physicians and drug and device companies. Legislators have said the regulations are intended to control costs by reining in unnecessary prescribing of expensive drugs and to make doctors' potential conflicts of interest transparent to the public.
Any company doing business in Massachusetts must comply with the regulations.
After the Public Health Department staff proposed the regulations, objections were raised by dozens of interest groups and lawmakers. Consumer groups and some legislators wanted even stricter restrictions on the behavior of companies and their salespeople, such as requiring disclosure of all research payments.
Many companies said the proposal went too far and would discourage firms from doing business in Massachusetts. Convention and hotel executives said the rules would scare away companies from sponsoring continuing medical education courses for physicians, which bring millions of dollars into Boston.
The Public Health Department clarified that the rules allow for industry-sponsored conferences at hotels and convention centers that include meals.
Still, some industry executives are disappointed by the new rules.
"Massachusetts is now seen as the most unfriendly state in the nation toward industry," said Robert Coughlin, president of the Massachusetts Biotechnology Council. "In these tough economic times, you don't want to send a chilling message to an industry that's a growth industry."
The rules passed by a vote of 10 to 0. Three council members, all medical doctors, were not allowed to participate in the discussion or vote on the measure, in accordance with conflict-of-interest laws, because they owned stock or had some other financial interest in a drug company or other business regulated under the new rules.
The regulations will take effect July 1, and the first public reporting by companies will be due by July 1, 2010.
The information will be posted on the Public Health Department website and will be searchable by company and by healthcare provider.
-
Liz Kowalczyk can be reached at kowalczyk@globe.com.
-
------------
The Boston Globe, Op-Ed, JAMES J. MONGAN
"4 steps to cure surging health costs"
By James J. Mongan, March 16, 2009
IN MASSACHUSETTS, we have much to be proud of when it comes to healthcare. We have a highly successful health coverage law that is financially sound and viewed as a national model. Second, the quality of our medical care is arguably among the best in the nation, and major advances in the understanding and treatment of disease, discovered here in Boston, are transforming the lives of patients. Finally, healthcare is an economic engine providing jobs for some 300,000 residents, and spurring a growing biotech industry that is the envy of other states.
Progress costs money, and that has many citizens, elected officials and business leaders worried. The federal Agency for Health Research and Quality reports that healthcare costs rose an average of 8.8 percent per year between 1996 and 2006 nationally, and 8.7 percent average annually in Massachusetts. So we are not the only state experiencing healthcare cost increases; this is a national issue, and there are no villains or easy answers to the problem.
What can we do to control healthcare costs? We could take a blunt approach, adopted by other nations, which sets specified rates for all providers. This heavily regulatory approach can control costs, but it can also lead to indirect rationing and limiting services to patients. If the economic crisis forces steps this severe, it should be done nationally so we all share in the sacrifice.
States, however, can also successfully assume leadership roles in solving national problems. We are fortunate to have had extraordinary leadership among elected officials and from the healthcare, business, and advocacy communities in enacting health coverage reform.
I believe we should take a rational approach to control costs, and recommend these four steps:
Reimbursement reform. Our current, open-ended fee-for-service reimbursement system is an engine for inflation - the more you do, the more you are paid, and there are no explicit incentives for quality or efficiency. Partners HealthCare has pay-for-performance in its contracts with all the major payers in Boston and with Medicaid. These goals have enabled Partners to reduce inpatient and pharmaceutical utilization in the pay-for-performance contracts. The important work begun under Senate President Therese Murray's bill, which established the Special Commission on the Health Care Payment System, has the potential to make Massachusetts a national leader in rewarding prevention and efficiency.
Electronic medical records. Building and using a system of electronic records with decision support features to prompt and guide physician behavior is critical to controlling costs and improving quality and efficiency. At Partners, all primary-care physicians use electronic medical records; they are already seeing some results in reducing unnecessary medical expenses. For example, software is being piloted at Massachusetts General Hospital that automatically searches for a similar exam when physicians order a high-cost radiology test. In early experience, this decision support has reduced follow-up tests by 10 percent.
There is more to do in utilizing the full cost-control capabilities of this technology and in working with other hospitals and physicians to expand the use of electronic records and make systems interoperable.
Disease management. Guided by the knowledge that 10 percent of patients account for 70 percent of costs, we must do more to focus on these sickest patients. Early efforts at Partners HealthCare hospitals with diabetes and congestive heart failure have achieved measurable success in reducing emergency department use and readmissions, and must be expanded to other conditions.
Effectiveness review. The national Commonwealth Fund Commission and President Obama have recommended an approach to review the effectiveness of drugs and procedures as they are used in the healthcare system. Ultimately this may work best at a national level, but there is no reason why Massachusetts could not begin this work now.
At Partners, the Center for Drug Policy uses evidence-based guidelines on appropriate use of new and existing medications. This has enabled Partners to eliminate or restrict the use of some drugs in its register of approved medications, and an estimated $4 million was saved last year alone. Encouraging physicians to prescribe generic drugs has resulted in savings to Partners hospitals of about $2 million per year and to patients of up to $300,000 annually in co-payments.
Achieving success in each of these four areas will not be easy, but Massachusetts has never been afraid to take the lead on challenging issues. Working together, we can lead the way on coverage - and cost.
-
James J. Mongan MD is president and CEO of Partners HealthCare and chair of the Commonwealth Fund Commission on a High Performance Health System.
-----
-
www.boston.com/news/local/articles/2008/11/16/a_healthcare_system_badly_out_of_balance/
-
HEALTHCARE PRESCRIPTIONS
"Insurance at issue"
The Boston Globe, Letters, March 23, 2009
DR. JAMES Mongan dismisses governmental rate-setting as a "blunt approach" that could lead to limiting services. But the current system already limits services - it allows access only to those who have insurance. The insured, who have relatively unbridled access to healthcare, have to recognize that the only way that healthcare will be provided to the uninsured is by placing some limitations on services. There has to be sacrifice that is spread around. It can't just fall into the laps of the working poor any longer.
These wonderful four steps that Mongan describes - reimbursement reform, electronic medical records, disease management, effectiveness review - divert attention from the fact that there will need to be pain if we are to provide universal healthcare, and that this sacrifice needs to be felt in all quarters.
Dr. Deborah Bershel
Somerville, Massachusetts
-
"Principled approach"
The Boston Globe, Letters, March 23, 2009
IT IS surprising that Dr. James Mongan, president and CEO of Partners HealthCare, is such a staunch supporter of our Massachusetts healthcare law, Chapter 58 ("4 steps to cure surging health costs," Op-Ed, March 16). Mongan was one of the architects of the five principles for healthcare reform issued by the Institute of Medicine in 2004, yet Chapter 58 doesn't meet any of these principles.
Health insurance should be "universal." Chapter 58 does not cover all residents.
Healthcare should be "continuous." In Massachusetts people who have health insurance through employment may be one serious illness away from losing their job and their coverage.
Healthcare coverage should be "affordable to individuals and families." Premiums have been rising many times faster than wages, even since 2006 when the new law was enacted.
"Health insurance strategy should be affordable and sustainable for society." The cost of the subsidies to low-income people is higher than anticipated, and the contributions from the business community are much smaller than what was needed.
"Health insurance should promote care that is effective, efficient, safe, timely, patient-centered, and equitable." Chapter 58 is based on ability to pay, which creates medical disparities. The individual mandate is punitive, forcing people either to buy insurance that often has unaffordable out-of-pocket costs or to be fined.
Mongan should be supporting single-payer healthcare, which meets all the five principles.
Dr. Patricia Downs Berger
Brookline, Massachusetts
The writer cochairs Mass-Care.
-
"Primary care gap"
The Boston Globe, Letters, March 23, 2009
DR. JAMES Mongan's prescription for curing "surging health costs" omits what is, for many, at the core of this so-called disease: The primary care workforce nationally and in Massachusetts is significantly understaffed in comparison to that of specialists.
Increased quality and decreased costs can be directly correlated to the number of primary care physicians in relation to specialists. Many Western healthcare systems have understood this and worked to achieve a ratio close to 50-50. In the United States it is more like 30-70. Today fewer than 10 percent of US medical students have expressed an interest in the primary care disciplines, and few internal medicine residents choose general medicine as a career. Boston, with its numerous academic medical centers, may have an even greater imbalance.
Thankfully, the Obama administration has identified the primary care shortfall as critical. To get more primary care doctors in the pipeline, we need to pay them more (and probably pay some specialists less), redesign practice sites to resemble patient-centered medical homes, fund medical school programs in primary care, and create a federal institute of primary care research. Until every person in the Commonwealth has a personal physician, we can never hope to cure surging healthcare costs.
Dr. Robert L. Dickman
Newton, Massachusetts
The writer is a professor at Tufts University School of Medicine.
------------
The Boston Globe, Op-Ed, LESLIE KIRWAN AND JON KINGSDALE
"Healthcare victory for consumers"
By Leslie Kirwan and Jon Kingsdale, March 21, 2009
GOVERNOR PATRICK'S call for a major effort to control healthcare costs registered a significant victory last week with the approval of new bids for the state's Commonwealth Care program. The contracts hold the line on government spending, without reducing benefits or increasing costs for members.
In fact, both the average rates that government pays the five health plans in Commonwealth Care and the average monthly contributions from members will decline slightly from current levels beginning in July. This is what insurance experts call negative or downward "trend," and it's virtually unheard of in healthcare. Since the inception of the Commonwealth Care program in 2006, the average annual rate of increase in premiums for enrollees has been held under 5 percent, well below typical "trend" for the same period.
There are other benefits of the new agreements. Members will have more choice with the addition of a fifth health plan. This new health plan represents one of very few new entrants to the Massachusetts health insurance market in decades, and it provides Commonwealth Care members access to nearly 100 new primary-care doctors.
Massachusetts now enjoys near-universal coverage. With 97.4 percent of citizens insured, the Commonwealth enjoys the highest rate of coverage in the nation. As a result, residents report far fewer financial barriers to accessing care, seeing their doctors, and filling prescriptions than the rest of the nation.
Expanded coverage is being financed by all of us - by government, by individuals buying insurance directly, and by employers. Under health reform, over 40 percent of the newly insured are enrolled in private plans, not subsidized by the state, and almost one-third of Commonwealth Care enrollees - while they receive a subsidy from the state - also pay monthly premiums. And nearly everyone recognizes that to sustain this historic achievement, we must control medical spending.
Last week's wins in the Commonwealth Care program are a result of prudent purchasing, strong financial oversight, and high-quality, cost-effective health plans. Collectively, the five participating health plans are answering the governor's call and bringing improved health as well as value to the citizens of Massachusetts. Now we need to move beyond this win to a comprehensive cost-containment strategy for all businesses and households.
In Massachusetts, the coalition of hospitals, doctors, employers, advocates, and health plans that came together to pass the landmark legislation of 2006 remained committed to its implementation. Now they must coalesce again to fight medical inflation. We must continue to build on last week's victory and find ways to bring continued innovation and value to the market.
The Obama administration is right in saying that fixing the way that healthcare is delivered and financed in the United States is one key to fixing the nation's economy. It is projected that healthcare will consume 17.6 percent of the gross national product this year - far more than America spends on education, transportation, construction, food, or any other vital economic activity.
Escalating healthcare costs not only bust government budgets, but sap workers' wages and hobble our international competitiveness. Over the past decade, health insurance premiums have risen 18 times faster than workers' earnings nationwide. Most workers have not seen wage increases above inflation because all their productivity gains go to pay for the increasing premiums of employer-sponsored health insurance. If getting more of our citizens covered is key to a healthy America, then getting medical inflation under control is key to a prosperous America.
As President Obama and Congress embark on the complex task of structuring national healthcare legislation, our experience in Massachusetts is receiving increasing attention. The structure of the law, policy decisions made during its implementation, and the public education campaign that helped drive enrollment are all being analyzed and discussed. Let us hope that as the spotlight continues to shine on us, we can continue to reform healthcare.
-
Leslie Kirwan is state secretary of administration and finance and chairwoman of the Massachusetts Health Insurance Connector Authority. Jon Kingsdale is executive director of the Authority.
-
------------
"State's Health Care System Gets Shot of Stimulus Funds"
iBerkshires.com - March 25, 2009
BOSTON — Some $764 million in federal stimulus funds will be injected into the state's Medicaid system as part of the nationwide effort to stablize the economy and save jobs.
"These additional FMAP funds are critically important to Massachusetts during these challenging economic times," said Gov. Deval Patrick. "Through thoughtful and strategic investments, we will protect and assist Massachusetts residents who will rely on the state for key services and supports now more than ever."
The federal American Recovery and Reinvestment Act provides a temporary boost in the Federal Medical Assistance Percentage, increasing federal matching dollars for the state's Medicaid program from 50 percent to between 56.2 percent and 61.6 percent, depending on unemployment levels in the state during the stimulus period.
Approximately $764 million in additional FMAP funding will be available to Massachusetts in fiscal years 2009 and 2010, supplementing the $1.2 billion announced in January as part of the governor's Emergency Recovery Plan.
"Shoring up our health care system is a responsible and proper use of stimulus funds," said U.S. Rep. John W. Olver, D-Amherst. "This extra infusion of capital will help to ensure that modest-income people have access to health care in these difficult economic times. In addition, these funds will directly contribute toward maintaining high-paying jobs in the health sector."
As part of the governor's budget, some $255 million will go to securing jobs and supporting health care services, including $160 million for hosptials and $45 million for nursing homes; $222 million for health care reform to maintin coverage for existing MassHeath and Commonwealth Care members; $97 million for for "safety net" initiatives, including $45.6 million toward aiding mental health clients and developmentally disabled citizens.
"By making these key investments now, we are continuing to preserve insurance coverage and eligibility for vulnerable populations to avoid capping program enrollment and eliminating services just when they are needed most," said Secretary of Health and Human Services Dr. JudyAnn Bigby.
For more information: www.mass.gov/recovery.
------------
The Boston Globe, Op-Ed
GENEVIEVE PREER AND CHÉN KENYON
"Defining, funding quality healthcare for the poor"
By Genevieve Preer and Chén Kenyon, March 28, 2009
AS THE nation looks to Massachusetts as a model for healthcare reform, decision makers must keep in mind that the most vulnerable patients often cannot advocate for themselves. As pediatric residents at Boston Medical Center and Children's Hospital Boston, we see the promise of exceptional healthcare. Yet we are concerned that funding decisions being made now will adversely affect the promise of healthcare reform for poor children and their families.
Quality healthcare requires health insurance that provides equitable reimbursement. Unfortunately, not all hospitals and providers are reimbursed fairly for the services they provide. Based on current rates and incorporating proposed cuts for next year, the governor's proposed budget would reimburse BMC only 64 cents for every dollar it costs the hospital to deliver care to our predominantly low-income Medicaid patients.
No healthcare provider can remain viable, much less continue to provide excellent care, while being paid 64 cents for every dollar spent. The White House recently announced that $15 billion in immediate Medicaid relief from the stimulus bill is being sent to the states. The money is federal matching funds given annually to states to pay for Medicaid and other related expenditures.
Fortunately, Massachusetts will be getting approximately $3 billion over the next two years and more than $594 million of that is expected soon. The money should be used as an immediate remedy to restore equal Medicaid reimbursement so that vulnerable patients at hospitals like BMC can continue to receive the services they desperately need.
According to a 2008 report issued by the Boston Public Health Commission, the neighborhoods in which our patients live have some of the highest rates of low birth weight babies, asthma hospitalizations for children under the age of 5, tuberculosis, substance abuse treatment hospitalizations, infant mortality, and overall mortality.
For these patients, quality healthcare means that the smallest premature baby, weighing less than a pound at birth and requiring life support to survive, will receive cutting-edge care in BMC's neonatal intensive care unit and will one day come back to visit the doctors and nurses who cared for him or her as a mischievous, energetic 2-year-old.
Quality healthcare means that when a parent brings a child for a well visit, the youngster will receive vaccines and other routine care, as well as a book to take home to prevent future learning problems. And the family will receive food from BMC's food pantry to prevent malnutrition and free legal assistance to prevent them from being evicted or having their power shut off.
Quality healthcare means that a teenager suffering from a severe asthma attack will be treated aggressively in our pediatric emergency room and will be cared for by critical care specialists in the pediatric intensive care unit, and will walk out of the hospital able to breathe again.
Our patients, who carry such an unequal burden of disease, desperately need the unique, high-quality medical services that BMC offers. But if BMC does not receive fair Medicaid reimbursement, we cannot continue to provide our complicated and vulnerable patients with the services they deserve. Simply carrying an insurance card does not guarantee good healthcare. BMC requires equitable funding if it is to continue to deliver high quality, comprehensive medical services to our patients.
As President Obama seeks to reform the healthcare system he is looking to Massachusetts. Our state now leads the country in expanding coverage. We must also continue to lead in providing the best care to patients living in poverty. The Patrick administration can increase Medicaid rates to a fair and reasonable amount. This needs to be done soon. The nation is watching.
-
Dr. Genevieve Preer and Dr. Chén Kenyon are senior pediatric residents at Boston Medical Center and Children's Hospital Boston.
-
------------
"Subsidized care costs state $794m: Companies relying on Commonwealth for health coverage"
By Kay Lazar, Boston Globe Staff, April 2, 2009
The state's bill for providing healthcare to employees and their families who work for large companies increased 24.6 percent to $793.7 million in the last fiscal year, according to a report released yesterday.
The report showed that while the state's landmark 2006 health initiative extended coverage to thousands of Massachusetts residents, many employers - particularly large retailers - continue to rely on state subsidy programs to provide health benefits to workers.
Wal-Mart, the world's largest retailer, tops the new list with 4,796 workers receiving public health coverage, followed closely by Stop & Shop, with 4,731. The rankings, which include only companies with 50-plus employees, are largely similar to last year's.
Overall, the number of employees and their dependents covered by state programs increased 12 percent in 2008, compared to 2007.
That jump is likely to reignite the debate about whether employers should pay more to the state for their workers who are receiving subsidized care.
"Increasingly, employers are getting tremendous benefits under health reform," said Lindsey Tucker, policy manager at Health Care for All, a large consumer group that helped create the 2006 law.
"The question is not whether employers are doing their fair share for the employees they are covering," Tucker said, "it's whether they are doing their fair share for their employees the state is covering."
The law sets a minimum standard for company contributions toward healthcare coverage, requiring companies with 10 or more full-time employees to have 25 percent of workers enrolled in a company plan or pay 33 percent of workers' premiums. Companies with more than 50 employees must meet both requirements. Those that don't meet the thresholds must pay $295 per employee into a pool for the uninsured.
Health Care for All is backing legislation that would require employers to contribute more, a proposal criticized by the state's largest business trade group, Associated Industries of Massachusetts, which also played a large role in shaping the state law.
"When we designed healthcare reform, we tried to strike a balance in terms of what employers responsibilities should be, and also tried to make sure we weren't placing Massachusetts employers at a competitive disadvantage," said AIM's chief executive, Richard Lord.
"We have seen that healthcare reform is supported by most employers," Lord said. "I worry that if we start tinkering with the law, that support could erode."
The law requires nearly everyone to have health insurance or pay a tax penalty. But third on the list of employers with the most workers enrolled in public health coverage is the Commonwealth of Massachusetts, with 3,785 employees - up 465 from last year.
Sarah Iselin, commissioner of the Division of Health Care Finance and Policy, the agency that produced the report, said the state provides generous health benefits, compared to many employers, and that overall, the percentage of workers not covered by state plans is less than 5 percent of the employees.
-
Kay Lazar can be reached at klazar@globe.com.
-
Related Links:
www.mass.gov/Eeohhs2/docs/dhcfp/r/pubs/09/50_plus_employees_04-09.pdf
-
www.mass.gov/?pageID=eohhs2modulechunk&L=4&L0=Home&L1=Government&L2=Departments+and+Divisions&L3=Division+of+Health+Care+Finance+%26+Policy&sid=Eeohhs2&b=terminalcontent&f=dhcfp_researcher_all_dhcfp_publications&csid=Eeohhs2#50_plus
-
------------
"Massachusetts groups sharing burden of health insurance"
By Associated Press, April 6, 2009, - www.bostonherald.com - Local Politics
BOSTON — A new study affirms one of the key principles of Massachusetts’s landmark health care reform law: employers, individuals and the government are proportionately sharing the burden of paying for insurance.
Overall spending on health care increased 23 percent after the new law’s passage, from $20.8 billion in 2005 to $25.5 billion in 2007. But the spending distribution among the three groups hardly changed.
The report, released by the Blue Cross Blue Shield of Massachusetts Foundation, found that employers paid about half of the total health care spending in both 2005 and 2007. Individuals and the state and federal government split the other half, with 25 and 27 percent respectively.
Officials are holding panel today to discuss the findings.
------------
"State mandate not driving health coverage costs: Report: Increases due to inflation"
By Kay Lazar, Boston Globe Staff, April 7, 2009
On the third anniversary of Massachusetts' landmark health insurance overhaul, a new report shows that employers, consumers, and state government paid the same, proportionately, for health coverage after 2006 as they did the year before the initiative started.
The study, released yesterday from the Center for Health Law and Economics at the University of Massachusetts Medical School, found that employers contributed about half (48 percent) of the overall spending on coverage in Massachusetts in 2007. Individuals accounted for about a quarter of the total, and government - divided between the state and federal level - contributed about 27 percent.
"With all the criticism from the left and the right before health reform started - that individuals will have to pay more or that government will have to pay too much - this says both of the concerns are unfounded," said Michael Widmer, president of the Massachusetts Taxpayers Foundation, a business-funded public policy group. The foundation played a key role in creating the 2006 law.
The report, commissioned by the Blue Cross Blue Shield of Massachusetts Foundation, found that overall spending on healthcare coverage increased $4.7 billion, or 23 percent. Nearly $21 billion was spent on coverage in 2005, while $25.5 billion was spent in 2007.
But the majority of the increase, the report found, was not from the new law. Sixty percent of the rise was due to healthcare inflation unrelated to the law. Another 31 percent was linked to new enrollment in already-existing programs, such as employer-paid healthcare or Medicaid, according to the report.
More consumers have coverage, the study found, but they are paying more than previously.
The 2006 law requires nearly everyone to have coverage or face a tax penalty. It also requires most employers - those with more than 10 full-time equivalent employees - to provide coverage or pay a penalty for uncovered workers. The study found consumers were paying a lot more in penalties for failing to have coverage - approximately $16 million - than employers, who paid $7.7 million.
A state report released last week noted that 72 percent of Massachusetts employers offer health insurance to employees, whereas nationwide, that figure is only 60 percent. Still, the report noted that many large retailers continue to rely on state subsidy programs to provide health benefits to their workers.
Leaders at Health Care for All, a large consumer group that helped shape the state's 2006 law, are backing legislation that would require employers to contribute more to coverage.
"Our challenge moving forward is to ensure health reform's continued affordability for the state, employers, and individuals," said Lindsey Tucker, a policy manager at Health Care for All.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
The Boston Globe, Op-Ed
JAMES ROOSEVELT JR.
"Healthcare: Let's build on what we know"
By James Roosevelt Jr., April 9, 2009
AN ARTICLE in The New Yorker earlier this year by Dr. Atul Gawande explained the rationale for creating a national healthcare system based upon the fundamentals of existing programs. Gawande provided a terrific overview of the origins of healthcare systems in other parts of the world, and it is instructive for us as we embark upon our own journey toward universal healthcare. His premise is that every nation that has a successful national health plan has built it upon what existed in its own borders - imperfect and patchworked, but foundational nonetheless. I agree with him that that is what America must do rather than create a government-run health plan, or any system that reproduces what is done in Canada or Great Britain, or elsewhere. Building upon employer-based, private health insurance has proven merit.
The advocates of a government-run plan claim that it will control costs. I am not convinced. The allure of a government-run health plan is distracting and unproven, and brings a high risk of unintended consequences such as reducing competition and consumer choice. Moreover, even if a government-run plan could be designed in a way that preserves choice for most Americans, it would delay the start of universal coverage for years. As a nation, we simply cannot afford to wait for the kind of accessible, portable, universal healthcare coverage that we have available to us today in Massachusetts, or to employees eligible for coverage through the Federal Employees Health Benefits Plan, which was touted during President Obama's campaign.
Our experience offers a real-time example of what can be achieved when there is a successful public/private partnership. The Commonwealth's citizens have long enjoyed the promise that healthcare won't be denied due to a prior health condition. We haven't had to make the choice between bankruptcy and treatment for serious disease; endure waiting periods before receiving healthcare coverage; or pay hospitals upfront for life-or-death care. The lack of this protection elsewhere contributes to the sense of urgency felt in most of the country.
We have already learned that for healthcare reform to be successful, individual mandates encourage widespread adoption; that timing and a united will can create a workable solution; and that incentives must be aligned. This public/private partnership has successfully met the needs of more than 97 percent of the state's citizens and could be a blueprint for private market reform, as we understand what can be reasonably accomplished in a set time frame, what can be improved upon, and where the focus should be for achieving sustainable change while maintaining choice, quality, and affordability.
In addition, there is much that we do here in Massachusetts that the president wants the rest of the nation to adopt, such as: our leadership in electronic medical records; our commitment to quality through innovative payment models for providers; and our adherence to evidence-based medicine. Of course, this isn't to say that our state system is perfect, but theoretical perfection should not hold us hostage as we embark upon an idea whose time has finally come.
Evidence that we inhabit a unique moment is that, unlike 1993, we are engaged in a much different discussion. The country's insurance industry is now a key supporter and stakeholder, and has already signaled its willingness to be part of the national solution.
For example, America's Health Insurance Plans, a national trade association on whose board I sit, has submitted its own comprehensive healthcare reform proposal to achieve universal coverage, reduce the unsustainable increase of healthcare costs, and improve the quality of medical care. No less a national healthcare advocate than Senator Ted Kennedy said of AHIP's efforts, "The insurance industry has advanced serious proposals that deserve serious analysis and consideration."
As Gawande suggests, let us learn from the experience of others who successfully crafted healthcare systems built upon existing foundations. We cannot afford to be distracted. Today's confluence of will, momentum, and the coming together of stakeholders is rare and must not be squandered.
-
James Roosevelt Jr. is president and CEO of Tufts Health Plan and co-chair of the policy committee of America's Health Insurance Plans.
-
On 4/9/2009, e67 wrote:
>> “We have already learned that for healthcare reform to be successful, individual mandates encourage widespread adoption;… .”
---
Under coercion of a Department of Revenue penalty, high-priced luxury plans that disallowed anything but all of the fixings were designed by a state legislature convinced that high employment and a bountiful revenue stream were guaranteed certainties. It has contributed to the destruction of the state economy, and the consequent drop in revenue by affected advertisers may result in the closure of a newspaper.
>> "our leadership [according to whom?] in electronic medical records."
---
A shaggy dog (and a mission that has little if anything to do with improved medicine). And one that, if anything, isn't being advanced in eastern Massachusetts at all, but rather between a NY test site and Redmond, WA.
>> "...and our adherence to evidence-based medicine."
---
Like the local work of the celebrated Dr. Joseph Biederman?
>> "reduce [sic] the unsustainable increase of healthcare costs, and improve the quality of medical care. No less a national healthcare advocate than Senator Ted Kennedy said of AHIP's efforts, 'The insurance industry has advanced serious proposals that deserve serious analysis and consideration.'"
---
Reduce? Reduce in the sense that Kennedy was enlisted just recently to help CMS funnel a $10.6 billion, 3-year Massachusetts Medicaid waiver that allowed the state to continue an otherwise unsustainable health insurance law? That kind of expenditure reduction?
-----
On 4/9/2009, johnmayer76 wrote:
Are you uninsured in America? You should check out the website http://UninsuredAmerica.blogspot.com - John Mayer, California
-----
On 4/9/2009, fredbob wrote:
"We have already learned that for healthcare reform to be successful, individual mandates encourage widespread adoption"
OR SAY: Insurance company profits go up when everyone is forced by the government to patronize and insurance company.
"The allure of a government-run health plan is distracting and unproven, and brings a high risk of unintended consequences such as reducing competition and consumer choice."
OR SAY: THe insurance industry - including Mr Roosevelt - findx that any serious consideration of a single-payer health care system is a distraction from the business of increasing insurance company profits. And since when is "consumer choice" important? My brother had to change doctors because his employer changed insurance plans and the new one won't let him see his former doctor who has treated him well and effectively for years. ANd what does "competition" get us? Bigger hospital buildings with more fancy machinery that only drives up the cost of medical care as the hospitals compete with each other to attract the most "customers" and increase their profits and the salaries and bonuses of their executives.
Further, the idea that a government single-payer medical care system is fraught with risk to the population is ridiculous. Exactly that kind of system has been proven to work in many countries already. Look at world health statistics. We, who refuse to adopt a single-payer system because insurance and drug companies and other big businesses have convinced many of us that the Constitution guarantees a right to obscene profits on the misfortune of others, are at or near the bottom of the "developed" world in most statistical categories.
Long live the insurance industry!! Long live Big Pharma!!
-----
On 4/9/2009, fredbob wrote:
"I agree with him that that is what America must do rather than create a government-run health plan, or any system that reproduces what is done in Canada or Great Britain, or elsewhere. Building upon employer-based, private health insurance has proven merit."
OR SAY: "....has the proven merit of maintaining the status quo in which insurance companies and the medical equipment and drug industries make huge profits on the pain of the common people, and in which the common people must be slaves to their employer because they otherwise can't have affordable medical insurance."
The current system has helped to make General Motors and other American companies less competitive in world automobile markets, and penalizes people who work in small businesses or are self-employed who must pay much more for less medical insurance than those who work for large businesses, if their employer even has an insurance plan.
THere is a lot wrong with the employer-based insurance model, and much of what is wrong with it benefits corporate bottom lines and helps to stifle entrepreneurship and innovation in business by keeping many people who would otherwise work in small businesses or start their own business stuck in a corporate job. It also restricts the ability of many Americans to work where they want to work and do the kind of work they might most want to do or be best at because they need to stay where their insurance is.
Mr Roosevelt is blowing up a smoke screen in order to protect his insurance industry's profit margins. He, at least by the evidence of this opinion piece, has NOTHING USEFUL to say about reforming our medical care system.
Our freedom to work where we want and to work at what we wnat to work at, and our right to decent and affordable medical and health care far outweighs any dubious right to large profit margins for capitalists.
-----
On 4/9/2009, feuerbach2 wrote:
"The allure of a government-run health plan is distracting and unproven, and brings a high risk of unintended consequences such as reducing competition and consumer choice."
I started reading this article without knowing what the author did for a living. When I got to the end, I realized where he was coming from. Here are his two main worries about a state-run health system: decreased competition and consumer choice. I'm sure that due to his position, Mr. Roosevelt gets (a) a hefty salary and (b) a generous discount in his health plan premium. What he doesn't understand --or doesn't want to understand-- is that his two main concerns already are a reality in our current privately run health system.
There's a non-profit agency I know that only got 1 (one) quote from the different plans. Tufts, for instance, didn't even bother to give them a quote! The only competition I see is between BMW and Mercedes dealers. I'm sure that there are companies who can purchase their products but what about the rest of us? His other concern: consumer choice. If this guy lived in the real world, he would know that the real choice is between paying your health plan premium OR buying food, paying your mortgage/rent, etc. I know that some agencies in the non-profit world are asking their employees to explore MassHealth and Commonwealth Care as viable alternatives!
The system is broken, Tufts et al. have a mandate from their boards to ensure that the status quo is maintained at any cost, and the Globe gives these companies this space to publish their BS. I love America!
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2009/04/09/healthcare_lets_build_on_what_we_know/?comments=all
-
------------
"Should state be a health reform model?"
The Berkshire Eagle, Op-Ed, By Charles Joffe-Halpern, Wednesday, April 15, 2009
NORTH ADAMS, Massachusetts
A battle is raging whether Massachusetts should be a model for expanding health coverage to the approximately 46 million Americans without health insurance.
Indeed, the lead health reform proposals being moved forward in Congress, with encouragement from the White House, include a variation of the principles of Massachusetts health policy. These principles include: providing subsidies to help individuals pay for health insurance, an individual health insurance mandate, an assessment on larger businesses who do not offer health benefits to their employees, regulating health insurers prohibiting them from denying coverage to anyone, and developing a new federal health insurance plan that individuals and businesses could purchase.
These proposals build on the success we have achieved so far in Massachusetts driving down the uninsured rate to below 3 percent, strengthening employer-provided coverage, and improving access. They would also learn from the challenges still facing Massachusetts, such as how to control costs, which continue to rise for everyone.
To understand why Massachusetts is seen as a potential model, it is important to recognize that any proposed health care legislation in this country has to pass through a gauntlet of special interest groups including: groups representing medical providers, business interests, insurance providers, and patients. These groups have varying amounts of power and influence to either support, or defeat any proposed change in national health policy — and they will fight to keep their interests protected.
— The American Medical Association, the most powerful lobbying force for physicians, wants subsidies to help individuals pay for coverage; choice for individuals in what health plan to join; and insurance market reforms that "protect vulnerable populations without unduly driving up premiums for the rest of the country." The AMA has also come out against the creation of a new public plan, fearing the plan will drive down reimbursements to physicians.
— The U.S. Chamber of Commerce, the influential business lobby, supports a health insurance mandate along with subsidies to help low-income families pay for insurance; understandably it rejects any mandate for businesses to provide coverage. It also wants freedom to offer plans nationally without state-by-state regulations.
— The health insurance industry's lead lobbying group, America's Health Insurance Plans (AHIP), indicates it will agree to be regulated if a mandate for all Americans to have coverage is a part of the deal. It vehemently opposes the creation of a new public health insurance plan, claiming the public plan would have an unfair advantage to compete with their members.
And how about patients, shouldn't their preferences come first? To understand patients, it is important to recognize that 94 percent of all voters have health insurance, and while most voters feel the uninsured should have access to health coverage, most feel that individuals should have to pay for it for at least some of it; it is easy to overlook that we live in a society where the prevailing cultural value is self-responsibility.
There is also the psychological factor that individuals are less fearful of the devil they know to the devil they don't know. While upset at the increased costs of health coverage through higher premiums, deductibles, and co-pays, most people still want choice and prefer to have the option of keeping their employer-sponsored health coverage to an entirely government financed system.
Policy makers are very aware of where these groups stand. President Obama, to avoid frightening the public, says under his plan Americans will be able to maintain their choice of doctors and insurance plans. Other Democratic leaders emphasize the need for quality "affordable" health care over "universal coverage," while at the same time, stressing the need to hold insurance companies accountable.
Commenting on the demise of the Clinton health reform initiative of 1993, Jacob Hacker, writing in "Health Affairs" observes: "The greatest lesson of the failure of the Clinton health plan is that reformers pay too much attention to policy and too little to politics. If real estate is about location, location, location, health reform is about politics, politics, politics." He added: "the problem was that policy development was put ahead of coalition building and building public support."
In Massachusetts, we were only able to implement health reform, because of compromises made among consumer advocacy groups, health care providers, business interests and health insurers. What we have implemented might be considered a political blueprint, rather than a policy blueprint. If we are to learn from the lessons of the past failed attempts to reform health policy, the political blueprint is how we must move forward.
-
Charles Joffe-Halpern is the executive director of Ecu-Heath Care and the president of the Board of Directors of Health Care for All in Boston. He can be contacted at cjoffehalpern@nbhealth.org
-
------------
"ER visits by Mass. residents on the rise"
The Associated Press, Friday, April 24, 2009
BOSTON (AP) — The number of people visiting hospital emergency rooms in Massachusetts is on the rise, and so is the cost of treating them.
The Boston Globe, citing state data, reports today that emergency room visits grew 7 percent between 2005 and 2007, to more than 2,469,000.
The estimated cost of treating those patients — including salaries for caregivers, medical tests, and medicines — jumped to $973 million from $826 million in the same time period.
The rises come despite efforts to direct patients with non-urgent problems to primary care doctors instead.
Some doctors and policy makers say what is needed to reduce emergency room visits are more primary care doctors and nurses, and a new system to better monitor patients with chronic illnesses.
------------
"High healthcare costs taking toll on insured"
By Kay Lazar, Boston Globe Staff, May 2, 2009
Despite Massachusetts' pioneering 2006 health insurance overhaul, healthcare costs are devouring more than 10 percent of thousands of residents' income, according to a new study from Families USA, a nonprofit organization that lobbies for affordable care.
The study, released yesterday, found that more than 1 million Massachusetts residents are in families that will spend more than 10 percent of their pretax income on healthcare this year, even though the vast majority of them - roughly 94 percent - have health insurance. Also of note: Their ranks have increased 46 percent since 2000.
"High healthcare costs are not just a problem of the uninsured," said Ron Pollack, executive director of Families USA. "Increasingly people are finding that healthcare costs are consuming a larger and larger portion of their family budget."
In some families, the study found, healthcare costs eat up far more than 10 percent: Nearly 300,000 Bay Staters are in families that will spend more than a quarter of their pretax income on healthcare, researchers found. Again, the vast majority - 90 percent - have insurance, Pollack said.
In 2006, Massachusetts launched a first-in-the-nation initiative requiring nearly everyone to get health insurance or pay a tax penalty. Because of that law, Massachusetts now has the highest percentage of insured in the country. But soaring monthly premiums, combined with skimpier coverage for services and medications, has burdened many with bills they can no longer afford. And calls to consumer help lines from residents with health insurance are mounting.
"We get calls all the time from people who want to pay their medical bills, their debts are mounting, they have gone through their savings to pay their bills and don't have the resources to cover them," said Carol Pryor, policy director at Access Project, a Massachusetts nonprofit that helps consumers negotiate payment plans.
Much of the rise in healthcare costs nationwide, the study concludes, is linked to increasing use of prescriptions and hospital care, pricey new medical screenings, and an insurance market with few consumer protections.
A state commission is working on strategies to help slow spiraling healthcare costs, which are growing faster than the national average. "Until we do some thing about the way we pay for healthcare and reduce some of the inefficiencies in the system and redesign the way care is delivered, we can't expect anything other than those costs will increase," said Anya Rader Wallack, who cochairs the commission's cost-containment committee.
"Our goal is to have a report by September that will lay out a range of strategies that will hopefully work together to bring down the rate of healthcare costs," Wallack said.
Across the country, 64 million people under age 65 are in families spending more than 10 percent of their pretax income on healthcare, the Families USA study concluded. Nearly 19 million are spending more than 25 percent of their income, and most of them have insurance.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
A BOSTON GLOBE EDITORIAL
"A public plan for healthcare"
May 3, 2009
THE SUCCESS of Massachusetts' three-year-old experiment with universal health insurance has made it a focus of attention as Congress and the Obama administration weigh reform on a national scale. But Massachusetts isn't a model for everything. A case in point: the debate over whether national legislation should include a public insurance plan as an option for consumers who don't qualify for Medicare and Medicaid and cannot get coverage through employers.
The architects of reform in Massachusetts opted not to create such a public plan, and opponents of the idea, such as private insurance companies, make much of that decision. Private insurers fear that a public plan would use its bargaining heft to drive down costs and grab a disproportionate share of the market. Advocates of a public plan, such as President Obama, say it is the best way to ensure affordable coverage and to provide a yardstick for the private plans.
So, does the Massachusetts example clinch the case against a public plan? No.
As noted by speakers at a conference recently at Harvard's Kennedy School, this state could avoid a public option because it already had a highly regulated insurance system that ruled out some of the more unsavory features of laissez-faire private insurance. Companies in Massachusetts could not refuse customers because of preexisting conditions or reject policy renewals after health problems emerge. Insurers could charge higher premiums based on a customer's age or place of residence, but not health history.
The state required that insurers cover many treatments and procedures, such as special screening of newborns, beyond the bare-bones policies offered elsewhere. It had a relatively low number of uninsured residents to start with. And, almost alone among the states, Massachusetts had no for-profit firms among its major insurers.
With a national health reform debate looming, some major private insurers have said they could live with a requirement that they accept all patients if it is paired with an individual mandate, like the one in Massachusetts. This would ensure that the young and healthy join the risk pool and lower its overall costs. But the Massachusetts rules would hamstring the private insurers that specialize in excluding anyone with a preexisting condition and providing as little care as possible to everyone else.
As the debate in Washington swirls over creation of a public plan, its supporters should not be cowed into dropping their insistence on it. Massachusetts is getting along without a public plan, but the national health insurance market is vastly different.
------------
"State seeks to revamp way doctors, hospitals are paid"
By Liz Kowalczyk, Boston Globe Staff, May 7, 2009
Massachusetts soon may embark on another bold healthcare experiment, with a state commission poised to recommend this month that insurers radically change how they pay doctors and hospitals.
Commission members said they will urge Governor Deval Patrick and the Legislature to replace the current system, in which insurers typically pay doctors and hospitals a negotiated fee for each individual procedure or visit, with a set payment for each patient that covers all that person's care for an entire year.
Massachusetts would be the first state to broadly adopt such a system, which would essentially put doctors and hospitals on a budget in an effort to restrain health spending.
A single, yearly fee is intended to discourage doctors and hospitals from providing unneeded tests and treatments, so patients could find it harder to get procedures of questionable benefit. And because doctors and hospitals would have to work together more closely to manage the budget, the hope is they will better coordinate care for patients, which could improve quality.
The "fee-for-service" system "has all the wrong incentives," said Dolores Mitchell, a member of the Special Commission on the Health Care Payment System and head of the state employees' insurance program. "It encourages excessive use and does nothing to discourage waste. People know the system has been dysfunctional for years."
The 10-member commission includes administration officials, key legislators, and representatives of hospitals, physicians, and insurers, boosting chances that Massachusetts will overhaul its payment system.
The Patrick administration strongly supports the change. "We need to move forward as quickly as we can," said Leslie Kirwan, the governor's secretary of Administration and Finance and cochairwoman of the group, "but this is going to take a very thoughtful transition."
Commission members still must work out many challenging and controversial details - such as how quickly to switch systems and how to divide payments among primary care doctors, specialists and hospitals - which could derail the process. The federal government would also have to approve the payment changes for patients covered by the government's Medicare and Medicaid programs.
Legislators created the commission last year, directing it to identify ways to slow soaring healthcare costs in Massachusetts, where spending is growing by more than 8 percent annually, driven largely by the high price and heavy use of hospitals. The members began meeting in January and said they quickly reached consensus that the best way to do this is for the state to move toward dismantling the fee-for-service system, which Massachusetts private insurers use to pay more than 80 percent of doctors and nearly all hospitals.
The system pushes up costs because it encourages doctors and hospitals to do lots of procedures, and do those that are most profitable, even if they're not always necessary, according to health policy analysts. In addition, it results in specialists such as surgeons and cardiologists earning substantially more than primary care doctors, contributing to a shortage of these physicians. And it does not reward the type of coordinated care that is best for patients, analysts said. Commission members estimate that a new payment system could slow the growth of healthcare spending to about 5 percent annually.
"Massachusetts has recognized that its cost trends are unsustainable so something has to be done," said Paul Ginsburg, president of the Center for Studying Health System Change, a Washington, D.C.-based policy group. But he said the proposed changes are "very ambitious."
The commission's work partly grows out of the state's near-universal health insurance mandate, which is being closely watched as President Obama and Congress draft a similar national health insurance program. The escalating cost of caring for newly insured patients could threaten the future of the program, making state subsidies for lower-income residents and their out-of-pocket payments too expensive. Employers and workers in the private market also are struggling with soaring costs.
In January, Patrick also started pressuring hospitals and insurers to cooperate on controlling medical costs, following a Globe Spotlight series showing that some hospitals, most significantly Massachusetts General Hospital and Brigham and Women's Hospital, are paid far more than others for providing similar services. The commission has not yet developed ways to lessen these disparities, but members said they plan to do so.
"Doctors think it's very unfair to be paid different fees for the same services done at different institutions," said Dr. Alice Coombs, vice president of the Massachusetts Medical Society and a commission member.
The new payment system the commission expects to recommend has been tried before; it was known as "capitation" when it initially became popular under managed care in the 1980s and early 1990s. The system broke down when many small physician practices lost millions of dollars on very sick patients with high healthcare costs, and amid widespread concern that the system encouraged doctors to deny patients necessary care so they could stay within their budgets.
But commission members said they believe the state can adopt an improved version - called "global" payments - that protects doctors by providing higher yearly payments for very sick patients or those at risk of needing high-cost treatments. The state could also help make available insurance that covers physician practices in the event of large losses. Patients would be protected from doctors' denying them services, because the new system would monitor the quality of care doctors provide, members said.
It's also possible the group may recommend keeping fee-for-service payments for certain unusual and expensive specialty services - such as heart transplants or the delivery of triplets - or for one-person doctors' practices that can't easily align with a network of specialists and hospitals.
"The devil is in the details," said Dr. James Mongan, president of Partners HealthCare, the state's largest hospital and physician network, which includes Mass. General and the Brigham. Partners is one of a few systems that are already set up to handle global payments, which would require physician practices and hospitals to form networks to share insurers' payments and coordinate care.
"Most of the healthcare system is not structured in a way that could really work out a very rational global payment system," Mongan said.
How long it would take to restructure doctors' practices and hospitals is one of the major points of debate among commission members. Some, like Senator Richard Moore, an Uxbridge Democrat who cochairs the legislature's committee on healthcare financing, believe the cost problem is urgent and are advocating having a new system in place in three years.
But other commission members who represent providers and insurers say even five years may be impossible, because most doctors and hospitals don't have the computer systems or provider networks in place yet to fully coordinate care for patients, which would cost millions of dollars.
"These are not excuses not to change the payment system," said Lynn Nicholas, president of the Massachusetts Hospital Association. "These are infrastructure issues that have to be addressed to enable a hospital to be successful. Three to five years is unrealistic."
Members of the Patrick administration said the cost of healthcare is reaching a crisis point.
"There is urgency, but there also is a sense of realism about who can get there when," said Sarah Iselin, state commissioner of Health Care Finance and Policy and cochairwoman of the payment commission. That the group agreed so quickly that fee-for-service "is not optimal is really encouraging and shows that we have the potential here in Massachusetts to be a model for the rest of the nation on payment reform."
-
Liz Kowalczyk can be reached at kowalczyk@globe.com.
-
------------
"Massachusetts health model inspires key senator: Panel considers creating agency to ease insurance"
By Lisa Wangsness, Boston Globe Staff, May 13, 2009
WASHINGTON - A key Senate leader appears to be leaning toward proposing a new tax on employer-provided insurance benefits and creating a new federal agency modeled on one in Massachusetts to make it easier for individuals and small groups to buy insurance.
The Senate Finance Committee is discussing a series of policy options for sweeping healthcare legislation scheduled to be completed by mid-June. On Monday, the committee released options for insuring the nation's 47 million uninsured, including expanding Medicaid, subsidizing private insurance for low-income people, and creating a public insurance plan - an idea Republicans have flatly rejected.
Yesterday, the committee debated how to pay for subsidizing insurance for the uninsured, which could cost as much as $1.4 trillion over 10 years. The panel's chairman, Senator Max Baucus of Montana, a Democrat, pointed to the tax exclusion, a rich source of cash. Senators will also consider other options, including "sin" taxes on soda and alcohol and limiting tax breaks for other health benefits, such as tax-preferred health accounts.
"The reforms that we are planning are not cheap," Baucus said.
Senator Charles Grassley of Iowa, the ranking Republican on the Finance Committee, said lawmakers should try to eliminate wasteful spending before imposing new taxes.
And starting to tax the health benefits the vast majority of Americans get through their workplace could set the stage for a battle with the White House; President Obama spent millions of dollars during the campaign attacking his Republican rival, John McCain, for proposing to end the tax exclusion, which Obama said amounted to taxing health insurance.
Baucus said yesterday that he does not believe the benefit should be eliminated, but that it should be fairer and less regressive. Under current law, those with the most expensive insurance get the largest benefit.
Limiting the tax exclusion is one of the few options that could provide large amounts of revenue to expand health coverage. Employer-provided insurance is considered part of workers' compensation, but unlike salaries, is not taxed as income.
Kenneth E. Thorpe, chairman of the Department of Health Policy and Management at the Rollins School of Public Health at Emory University, said it is worth "well over $250 billion a year."
The Finance Committee's options for expanding coverage include phasing in new regulations requiring all insurance products to cover basic medical services that the least expensive plans in some states don't cover currently, such as prescription drugs and mental health and substance abuse services. No annual or lifetime limits would be allowed. Insurers could vary premiums based on a few factors, such as age and geographic location, but could no longer refuse to cover someone.
The committee's policy options also explain the workings of the Commonwealth Health Insurance Connector, which helps Massachusetts individuals and small business employees compare and purchase insurance. Based on that model, the proposal calls for creating a national website that would offer one-stop shopping for individuals and small groups. Jon Kingsdale, executive director of the Commonwealth Connector, said policymakers have clearly taken note of the popularity of the Massachusetts website.
-
Material from the Associated Press was used in this report.
-
------------
"Report: Mass. health care law no budget buster"
By Associated Press, Tuesday, May 19, 2009, www.bostonherald.com - Local Politics
BOSTON — A new report says Massachusetts’ landmark health care law has had only a "marginal impact" on state spending while dramatically expanding the ranks of the insured.
The business-backed Massachusetts Taxpayers Foundation, which supported the law, said Tuesday it found state health care spending will grow by $707 million between the 2006 and 2010 fiscal years. Half the increase is reimbursed by the federal government for an annual state increase of $88 million.
That has allowed the state to achieve the lowest uninsured rate in the country.
One reason is that many workers who had previously opted against getting insurance through their jobs have now signed up, at an annual additional cost to business of about $750 million.
------------
"Costs are keeping patients from care: Copayments rise as families struggle"
By Kay Lazar, Boston Globe Staff, June 21, 2009
People with robust health insurance are putting off doctors’ appointments and skimping on prescriptions because they can’t afford the increasing costs of copayments and deductibles, according to managers of patient-assistance hot lines in Massachusetts.
Not that long ago, such dilemmas were typically faced by lower-income families, often on publicly subsidized insurance. But with many consumers struggling to pay rising healthcare costs amid today’s shrinking family budgets, these tough choices are becoming commonplace - even among families with employer-provided health insurance, consumer advocates say.
“Our medical debt resolution program is hearing repeatedly that copayments are a problem,’’ said Mark Rukavina, executive director of the Boston-based Access Project, a nonprofit organization that helps consumers with healthcare issues.
“Previously it was the uninsured,’’ Rukavina said. “Now we are seeing people with insurance, but they are struggling to pay their bills.’’
The problem appears particularly acute for people with chronic illnesses such as diabetes, asthma, and cancer. They make frequent visits to doctors and often take multiple medications.
The issue has become so widespread that state lawmakers have scheduled a hearing Wednesday to address aspects of the problem, including a proposal to allow residents with chronic illnesses to buy prescribed medications and medical devices without facing a copayment or deductible.
As healthcare costs rise and the recession’s grip has tightened, more employers have slashed their health costs by shifting more costs onto their workers, according to Families USA, a Washington-based consumer group. As a result, more employees are shouldering heftier copayments.
In 2004, most patients had copayments of $15 or less for a visit to a primary care physician, according to the Kaiser Family Foundation, a health research nonprofit group. By 2008, a majority were paying $20 or more per visit. Many insurance plans now require even higher copayments for visits to specialists, the doctors typically seen by people with chronic illnesses.
Christina Knowles of Boston said she canceled two appointments with pain specialists this spring because she couldn’t afford the $25 copayments. Despite having what she thought was decent health insurance, the 26-year-old had accumulated more than $2,000 in medical debt from copayments for surgery, frequent follow-up care, and prescriptions, after having a benign tumor removed from deep within her jaw.
“It’s both incredible and sad to think that I am the poster child for the new demographic of people who cannot afford medical care,’’ said Knowles, statewide manager for the Massachusetts chapter of the National Organization for Women. Her annual salary was in the low-$30,000s until she got a raise this month.
The surgery left her with partial facial paralysis and a gnawing pain, but Knowles said she was so cash-strapped that she resorted to frequent ice packs and Advil instead of going to the pain specialist recommended by her physician.
“There were days where it bothered me so much, I had ice on my scar all day,’’ said Knowles, whose pain has since eased.
In Framingham, Dr. James Kenealy, an ear, nose and throat specialist, said his patients increasingly cite copayments as a hurdle to continuing with allergy treatments. The care typically includes weekly shots for several months, with copayments ranging from $20 to $50, per shot, depending on the patient’s insurance plan.
“Probably once a week, there will be a patient deciding to discontinue allergy injections or not pursue that as a therapy because they have high copays,’’ Kenealy said.
Even patients without chronic illnesses are finding themselves in a copayment crunch.
“If you are a family with four or five kids . . . copayments are going to add up,’’ said Worcester family physician Dr. James Broadhurst, noting that children visit doctors frequently for illnesses and preventive care.
Especially in the past year, Broadhurst said he’s encountered more families asking him to treat or prescribe over the phone because they can’t afford the copayment of an office visit.
As part of Massachusetts’ pioneering 2006 healthcare overhaul, the state created the Safety Net program, which helps people of any income pay large medical bills. But it specifically excludes coverage for copayments.
“Oftentimes, these people end up using their credit cards to pay their copays and end up with medical debt,’’ said Kate Bicego, help line manager at Health Care for All, one of the state’s largest consumer groups.
Bicego said calls to the nonprofit group’s helpline are up roughly 65 percent from last year, and many of those seeking help are struggling with copayments and deductibles.
One of the proposed laws, cosponsored by Senator Mark C. Montigny, a New Bedford Democrat, and Representative Charles A. Murphy, Democrat of Burlington, would prohibit insurers from charging copayments or deductibles for any prescribed drugs or medical devices that are “necessary for the treatment or maintenance of a chronic disease, illness or condition.’’
But the trade association that represents most of the state’s insurers says employers and consumers would just end up paying higher monthly premiums, instead, because the costs have to be covered somehow.
“Right now, employers are struggling with increased costs for healthcare in general, and this is not the time to be adding to their healthcare costs,’’ said Dr. Marylou Buyse, president of the Massachusetts Association of Health Plans.
Buyse said the state’s Connector Authority, which oversees the 2006 law that requires most adults to have health insurance, carefully considered the issue of high copayments and deductibles when it crafted rules that define the minimum health plan a resident must have in order to avoid a tax penalty. Those rules generally say out-of-pocket costs - deductibles, copayments and other patient fees - cannot exceed $5,000 for individuals and $10,000 for families, but allow copayments and deductibles for prescription drugs to be excluded from the calculation.
“The state struck a delicate balance to make sure individuals have adequate coverage, while guarding against standards too few could afford,’’ Buyse said.
Jon Kingsdale, the authority’s executive director, said it has taken no position on the bill or on another legislative proposal, also sponsored by Montigny. That measure is aimed at requiring the Connector Authority to consider the total amount of copayments and deductibles a consumer pays when calculating affordability thresholds used to exempt some residents from paying the tax penalty assessed for having no insurance.
-
Kay Lazar can be reached at klazar@globe.com.
-

-

-
------------
"State cuts its health coverage by $115m: Board to slow enrollment in Commonwealth Care"
By Kay Lazar, Boston Globe Staff, June 24, 2009
Overseers of Massachusetts’ trailblazing healthcare program made their first cuts yesterday, trimming $115 million, or 12 percent, from Commonwealth Care, which subsidizes premiums for needy residents and is the centerpiece of the 2006 law.
The board of the Connector Authority made the cuts as officials confronted two side effects of the recession: the state budget crisis and a surge in enrollment by the recently unemployed.
The largest share of the savings will come from slowing enrollment. An estimated 18,000 poor residents who qualify for full subsidies, but who forget to designate a health plan, will no longer be automatically assigned a plan and enrolled and thus could face delays in getting care.
The board also eliminated dental coverage for the poorest residents enrolled in Commonwealth Care, roughly 92,000 people who currently are the only ones in the program who receive that care. Regulators said that would save $10 million. Dental coverage was retained in the budget approved by lawmakers last week, and now it falls to the governor to decide its fate.
Also hanging in the balance is the health insurance status of 28,000 legal immigrants whose Commonwealth Care coverage was dropped in the budget lawmakers approved for the fiscal year that begins July 1. Governor Deval Patrick has until Monday to decide whether to veto any of that budget, which set aside $116 million less for Commonwealth Care than he proposed.
“No decision has been made’’ on restoring immigrant coverage, said Leslie Kirwan, chairwoman of the Connector Authority board and Patrick’s secretary of administration and finance. “It’s certainly going to be at the top of our list’’ of items the governor is considering adding back to the budget, she said.
But Kirwan said the $115 million in cuts the Connector Authority board approved yesterday were merely to deal with shrinking state revenues and the rapid growth in enrollment in Commonwealth Care, which has 177,000 members and was projected to grow to 212,000 in the next year.
These cuts do not provide any wiggle room for adding back the 28,000 immigrants who are facing elimination. If the governor decides to restore coverage for the immigrants, Kirwan said, he would have to find other areas to cut in the already razor-thin budget.
Patrick Holland, the Connector Authority’s chief financial officer, said enrollment spiked during the last three months, from 165,000 to nearly 177,000 members, because so many workers are losing their jobs and, with that, employer-provided health insurance.
The progress of the Massachusetts healthcare initiative is being closely watched in Washington, where Congress is crafting national legislation to extend coverage to more Americans. The Massachusetts law, cited as one model in the national debate, requires nearly everyone to have health insurance or pay a tax penalty.
The residents affected by yesterday’s cuts earn too little to be subject to the penalty. They also would be eligible for free emergency care for three months under the state’s Health Safety Net.
Leaders of Health Care for All, one of the state’s largest consumer groups, said the changes will be especially hard on residents whose first language is not English and who have difficulty understanding the complex enrollment paperwork.
But the group said state officials appear to have made the best of a bad situation. “There’s no other place to go for money,’’ said Lindsey Tucker, the organization’s healthcare reform manager. “. . . My concern is people will not get the care that they need.’’
While the group’s leaders are resigned to that cut, they said they will continue to lobby the governor to restore coverage for legal immigrants. Lawmakers said they cut this class of legal immigrants because they do not qualify for matching federal subsidies. Thus, they are more expensive for the state to insure. The move has enraged advocates for the immigrant community.
Much of the rest of the $115 million in savings, $32 million, comes from slowing payments to the managed-care health insurance companies that won bids to offer insurance through the Commonwealth Care program. Regulators said that by slowing enrollment growth, the companies would receive less money than they had banked on when they submitted their bids earlier this year.
Kirwan stressed that when the economy improves, the changes made by the authority can be revisited. She also said the changes still protect the basic eligibility rules for the program and benefits that members receive, but put the brakes only on enrollment growth during an “unprecedented time.’’
While the emergency changes approved by the Connector Authority go into effect July 1, Kirwan said the board will schedule a hearing, probably in late July, to seek public comments on the issues.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
The Boston Globe, Op-Ed, JOAN VENNOCHI
"The forbidding arithmetic of healthcare reform"
By Joan Vennochi, Boston Globe Columnist, June 28, 2009
THE FUZZY math behind the Massachusetts universal healthcare law is starting to add up - just as Washington studies the law as a possible model for the nation.
Because of a recession-related drop in state revenues and a surge in enrollment by the recently unemployed, the truth is emerging at an inconvenient time. Massachusetts doesn’t have enough money to pay for the coverage envisioned by the law.
In June, state officials announced they are cutting $100 million from Commonwealth Care, which subsidizes premiums for needy residents. The poorest residents, along with the newest - legal immigrants - will take the hit.
This outcome is not surprising, but it is instructive as President Obama pushes for a national healthcare plan.
On the day that Republican Governor Mitt Romney, for once, made Bay State Democrats happy, by signing the sweeping new healthcare bill into law, the Globe headline said it all: “Joy, worries on healthcare. As Romney signs bill, doubts arise about revenues.’’
In Massachusetts, the numbers never added up, as everyone involved in crafting the new law understood. But for a variety of reasons, ranging from Romney’s presidential aspirations to Senator Edward M. Kennedy’s longstanding commitment to healthcare reform, everyone smiled for the cameras and hoped for the best out of this noble experiment.
Today, the current governor, Deval Patrick, a Democrat, is skeptical about the end product. Asked during a televised town hall meeting in March if he believes national healthcare legislation should be patterned after the Massachusetts plan, he said, “I don’t know. I had real misgivings about it as a candidate. . . . I’m proud of it, but I don’t know if it’s a model for the nation.’’
The foundation of the Massachusetts law is the so-called individual mandate. That means everyone must have health insurance. From that perspective, the Massachusetts experiment is a success. The percentage of residents without insurance was down to 2.6 after two years.
But, the law never provided an absolute way to pay for the expanded coverage, and it never addressed how to reduce costs.
“They decoupled the access issue from the cost issue,’’ said Philip Johnston, chairman of the Blue Cross Blue Shield of Massachusetts Foundation, which played a key role in expanding healthcare coverage here. “The lesson is, there needs to be a dedicated revenue source to support health reform.’’
An even bigger lesson is that to make health reform happen, all the players must be invested from the start - and must stay invested. “Getting it done is politics. That means dealing with all the elements that are necessary for near-universal access and cost management, but not overreaching in any one area, so that major stakeholders turn from supporting the effort to opposing it,’’ said John Sasso, who represented Partners Healthcare, the largest healthcare provider in Massachusetts, and Blue Cross Blue Shield, the state’s largest insurer, during the reform process.
The stakeholders are still at the table, trying to make the numbers work better, he points out.
It’s true that Massachusetts built a dream house of a healthcare plan, without knowing the exact cost or how to pay for it. But that doesn’t mean it should be dramatically downsized, as state Treasurer Timothy P. Cahill proposes as he positions himself for a gubernatorial run.
A recent report by the Massachusetts Taxpayers Foundation, a business-funded group that advocated for the healthcare law, found that state spending increased by about $88 million annually since it was implemented. Is that too much to absorb, within the context of a $28 billion state budget?
As Patrick also said about the state’s healthcare law at that town hall meeting, “The great story about Massachusetts is instead of waiting for the perfect solution . . . or doing nothing . . . we tried something.’’
Washington can’t be as adventurous. Costing out a national healthcare plan, and figuring out how to fund it, is the current fault line for Obama. The president insists he can overhaul the healthcare system without adding to the deficit.
He should take this final lesson out of Massachusetts: Be honest about cost in the good times and make sure you can cover it in the bad.
-
Joan Vennochi can be reached at vennochi@globe.com.
-
------------
"Widened mental benefits pose test: Advocates hail law covering 4 disorders; Insurers, employers say costs to be high"
By Kay Lazar, Boston Globe Staff, July 6, 2009
Tens of thousands of Massachusetts patients who grapple with some of the most intractable mental health problems - eating disorders, addictions, autism, and post-traumatic stress - should face fewer barriers to treatment under a state law that went into effect July 1. But the cost of the state’s latest healthcare expansion remains an open question.
The new law, which lifts limits on care, adds the four mental health disorders to nine other common psychiatric conditions that health insurers must cover as they do physical ailments. That means, for example, that a drug addict who previously would have been denied treatment after 24 outpatient sessions and a total of 60 days in a hospital will now get as much care as medically needed to tame an addiction.
While patient advocates hailed the expansion of mental health assistance, the people who will pay the bills - insurers and companies that provide health coverage to their workers - greeted the law with uncertainty, especially about its cost.
The expansion illustrates two of the most pressing issues in healthcare today: equality for mental health services and the price tag for expanding medical care.
“Any step we take that breaks down this artificial divide that exists between mental illness and physical health is a big step,’’ said Matt Noyes, a mental health advocate at Health Care for All, a Massachusetts consumer group.
Medical spending is under scrutiny from Beacon Hill to Capitol Hill, and the cost of expanding mental health coverage, known as “mental health parity,’’ is a matter of disagreement.
Supporters of the change, citing the experience of other states, said they expect parity will add less than 1 percent to overall healthcare costs, while easing the stigma of mental illness.
Insurers’ overall spending in Massachusetts, estimated at about $13 billion a year, will increase by $13 million to $39 million a year because of the new law, according to regulators’ calculations.
But a coalition of employer and insurance groups contends that the costs are likely to be significantly higher. Insurers said that the state’s calculations substantially underestimate the costs. They have not, however, come up with their own estimates.
“We will be able to tell in about two years from actual experience,’’ said Dr. Marylou Buyse, president of the Massachusetts Association of Health Plans, a trade group. “Everything else is an estimate based on what we think will happen. Reality is sometimes different.’’
Employers, also anxious about healthcare costs, say they, too, have not yet calculated how the new law will affect their tight budgets.
“Hopefully, it gets people the care they need, but is also cost-effective,’’ said Jim Klocke, vice president of the Greater Boston Chamber of Commerce. “We have had a cost problem in this state for a while.’’
Last summer, the Chamber of Commerce joined a coalition of business groups that lobbied lawmakers against passage of a more sweeping mental health parity law, which would have required equal coverage for an even broader range of conditions.
Not even the new law will ensure that every person in the state who needs those services will get them. Roughly half of Massachusetts companies are exempt from state insurance laws, meaning that they are governed by federal regulations that call for less-generous mental health services.
A new federal mental health law aimed at closing many of the gaps between state and national rules does not kick in for most of these companies until January, and, even then, the rules exempt some of them.
Ron Bachman, a former principal at PricewaterhouseCoopers who is now a healthcare consultant in Atlanta, calculates that at least 31,000 Massachusetts residents will fall into this enduring loophole.
“Should the advocates be anxious and careful and watchful? Sure,’’ he said. “There will be companies out there that try and find the loopholes. But at the end of the day, the vast majority of people will get improved mental health benefits.’’
There remains one piece of unfinished business. When the state last attempted to overhaul mental health services nine years ago, regulators left untouched the broad range of treatment that falls somewhere between overnight hospital stays and trips to the psychiatrist. That includes such services as residential treatment programs, home-based care, and day treatment programs. In that void, advocates say, patients have often had to battle, frequently failing, to get needed help.
“People with mental illness often have more difficulty navigating the speed bumps that health plans put in place,’’ said Dr. Gregory Harris, a Brookline psychiatrist and chairman of the managed-care committee of the Massachusetts Psychiatric Society.
State Insurance Commissioner Nonnie S. Burnes, who has been meeting for months with leaders from all sides of the issue, said she hopes to issue clear guidelines by the end of summer.
“We are working hard with the Department of Mental Health, as well as insurers and providers,’’ she said, “. . . so the consumers of Massachusetts will get what they are entitled to.’’
-
Kay Lazar can be reached at klazar@globe.com.
-
-----
"More care for 4 common disorders"
boston.com - July 6, 2009
A new Massachusetts law that went into effect July 1 lifted limits on medical care for four common mental health disorders.
Massachusetts law prior to July 1
A two-tiered system allowed health insurers to limit treatment for dozens of mental health diagnoses to 24 outpatient sessions and 60 days of hospitalization per year. But it prohibited such limits on nine specific disorders: schizophrenia, schizoaffective disorder, major depressive disorder, bipolar disorder, obsessive-compulsive disorder, panic disorder, affective disorders, delirium and dementia, and paranoia and other psychotic disorders.
Massachusetts law after July 1
Four additional psychiatric conditions are added to the nine without limitations on treatment: autism, eating disorders, substance abuse problems, and post-traumatic-stress disorders. The law also gives the state mental health commissioner the authority to include any additional disorder to this list.
Source: Massachusetts Division of Insurance
------------
"Massachusetts Panel Backs Radical Shift in Health Payment"
By Kevin Sack, The New York Times, July 17, 2009
BOSTON — A high-level state commission recommended Thursday that Massachusetts seek to rein in health care costs by radically restructuring the way doctors and hospitals are paid.
The commission’s action kicks off the second phase of a health care overhaul that has succeeded in covering nearly every resident of the state but done little to slow the relentless growth of spending.
The recommendations, if approved by the legislature and Gov. Deval Patrick, would make Massachusetts the first state to end the practice of paying health care providers for each office visit, laboratory test or procedure.
Instead, primary care physicians, specialists and hospitals would group themselves into networks that would be responsible for a patient’s well-being and would be compensated with a flat monthly or annual fee known as a global payment.
The 10-member commission deferred many central decisions to the legislature and to a new authority that would be created to establish and oversee the new payment system. In doing so, it preserved cautious support from the state’s hospital association, medical society and leading insurers for a proposal that resembles guiding principles more than bill language.
Representatives of those groups joined in a unanimous commission vote for the recommendations. But they made clear that their continued support might depend on devilish details, the kind that will determine whether their members are net losers and, if so, by how much.
It was only by keeping those stakeholders at the negotiating table that the state succeeded in 2006 in vastly expanding subsidized coverage for the uninsured. Maintaining that coalition is expected to be more difficult as the state tries to slow the growth of costs, an effort that typically translates into less revenue for providers and insurers.
The existing “fee for service” system has been roundly criticized as offering incentives that encourage doctors to provide more treatment than is necessary, a significant contributor to the high cost of health care.
Global payments, it is thought, would reward health care providers for keeping their patients well rather than for merely treating their ailments. If the cost of treating a patient was less than the global payment, the provider networks, called accountable care organizations, would keep the difference as profit.
Changing the payment system has also been central to the health care debate in Washington. Thus far, those discussions have focused more on providing financial rewards for high-quality preventive care than on demolishing the fee-for-service system.
The Massachusetts commission was created last year by the legislature and was led by Mr. Patrick’s chief finance and health policy advisers. But on Thursday the governor, a first-term Democrat, stopped short of endorsing its recommendations, saying only that they “bring an important focus to cost containment and quality.”
Top state legislators said that they recognized the political challenge in enacting such a plan but that Massachusetts’ circumstances demanded it. Senator Richard T. Moore, co-chairman of a joint legislative committee on health care financing, said he expected to hold hearings on the recommendations this fall.
The committee’s other leader, Representative Harriett L. Stanley, said, “It’s going to be a very long haul, but it’s a trip worth taking.”
The commission stressed the importance of changing the way doctors and hospitals are paid not only by private insurers but also by Medicare and Medicaid. That would require permission from the federal government.
Global payments are hardly a new idea, as the concept closely resembles the capitation model that incited a backlash by consumers who accused health maintenance organizations of skimping on care. But members of the Massachusetts commission said their plan would offer financial incentives for performance that would transform physicians into care coordinators rather than gatekeepers.
“This is not about containing costs by sacrificing quality,” said Mr. Patrick’s finance director, Leslie A. Kirwan, a co-chairwoman of the commission. “That’s been tried and rejected, and rightly so.”
The commission recommended that its plan be carried out over five years. The state would not set rates, which would be negotiated by insurers and the new provider networks. But it would require those payment rates to account for variations in the health condition and socioeconomic status of patients seen by individual doctors and hospitals.
The report left the details of such risk adjustments to the new authority that would be established. It also made no projection of what it would cost to set up the new system.
Interest groups with heavy stakes embraced the proposal, but warily.
“Hospitals want to be part of this historic endeavor,” said Lynn B. Nicholas, president of the Massachusetts Hospital Association. But Ms. Nicholas added that “the success of moving to a global payment system is not a foregone conclusion” and expressed concerns about how risks would be adjusted and how start-up costs would be covered.
The president of the state medical society, Dr. Mario E. Motta, also urged caution. “A big transition like this has never been done on such a broad scale,” Dr. Motta said, “so it must be done very carefully, deliberately and thoughtfully.”
The commission issued its recommendations three years after the state enacted one of the most sweeping restructurings of health care in the country’s history. By requiring nearly all residents to have health insurance, and providing subsidies to those earning no more than $66,150 for a family of four, the state has managed to cover 97 percent of its residents.
That is by far the highest rate of any state, and elements of the plan have been adopted by President Obama and Congressional Democrats in their proposals to revamp the national health care system.
But to maintain political support for expanding coverage, Massachusetts political leaders deliberately deferred any serious discussion then about how to control health care costs. Those costs have continued to rise at what state leaders acknowledge is an unsustainable annual rate of 6 percent to 9 percent. Although the state’s new subsidized insurance program, Commonwealth Care, has kept a lid on premium increases, it is now straining the state’s budget for the second consecutive year.
“We are among the highest-cost states,” said Sarah Iselin, Mr. Patrick’s health policy adviser and the other co-chairwoman of the commission. “Without intervention, our projections are that spending on a per-person basis could double by 2020.”
------------
A BOSTON GLOBE EDITORIAL
"How to pay doctors"
July 21, 2009
PAYING FOR healthcare on a fee-for-service basis is an inflation engine that, unless something changes, will cause health spending in this state to double by 2020. A legislative commission wants to replace fee-for-service with per-capita payments that would be handled by groups of healthcare professionals with full responsibility for an individual’s care. One-fifth of doctors in the state are already paid this way. Making it the norm could be the secret to better, less costly medicine.
Ideally, this shift in incentives will mean that a patient, for instance, will leave a hospital with enough discharge support so that she won’t be re-admitted a week later. Or, a primary-care physician checking an overweight patient for a strep throat will have enough time to talk to the patient about exercising more to lose some pounds. A well-crafted “global’’ payment system should pay for such preventive measures in ways that fee-for-service does not.
The commission issued its report on the same day last week that the head of the Congressional Budget Office told Congress that its various health reform proposals, including ones with a public insurance plan to compete against high-overhead private plans, would all raise federal spending. This state’s three-year experience with its health reform supports his conclusion. Less than 3 percent of the population is now uninsured, but costs have escalated.
A switch to global payments in the hands of so-called accountable care organizations with doctors, labs, imaging specialists, and even hospitals could bring costs under control. When health insurers used a capitation system in the 1990s, patients were denied care unfairly. To avoid such problems, the commission calls for rigorous monitoring and a focus on quality.
A first step will probably be legislation to create some kind of public board or authority to work out the specifics of the sticks and carrots that would wean providers from fee-for-service. One carrot will have to be tax credits or outright subsidies to speed up doctors’ and hospitals’ adoption of electronic medical records. Such records are crucial to the coordination that accountable care organizations should be able to provide.
To help ensure that any new payment system produces better care and not just cheaper care, the oversight panel should include at least one representative of a consumer group. The Legislature should also give the board more direction than the report provides. In 2006, lawmakers opted to let the Commonwealth Health Insurance Connector Authority work out many details of new health plans for the uninsured. But totally revamping health payments is a far more complex task that will require more explicit marching orders from Beacon Hill.
------------
The Boston Globe, Op-Ed
MICHAEL J. WIDMER
"Health law costs aren’t the problem"
By Michael J. Widmer, July 23, 2009
WE’VE HEARD the claims repeated from the moment the bill was signed three years ago - Massachusetts’ health reform law is unaffordable. Those claims have come from a wide variety of ideological and political quarters, but what they have in common is a failure to understand how the law works.
The Taxpayers Foundation recently released an analysis of the costs to taxpayers of achieving near-universal access to healthcare in Massachusetts. The “surprising’’ conclusion: Between fiscal 2006 and 2010, the annual incremental cost from the state budget is less than $100 million, a modest sum for this historic achievement. This cost is very much in line with estimates that were made when the bill was passed.
From a base of $1.04 billion in fiscal 2006, the state is projected to spend $1.75 billion on healthcare reform in fiscal 2010, an increase of about $700 miillion, half of which is supported by federal reimbursements. The $350 million state share translates into an average yearly increase of only $88 million.
Compare this with the sweeping education reform law of 1993, that decade’s rough equivalent to the 2006 health reform law in terms of scope and scale. Implementing education reform cost an additional $250 million each year between 1993 and 2000, with an average annual increment of approximately $150 million in the decade since. In recent years there has been much debate about whether that investment has paid dividends, but few claim we should back off the commitment.
The Legislature’s recent decision to cut the fiscal 2010 budget for Commonwealth Care as part of the state’s enormous fiscal crisis has led to renewed claims that health reform is unaffordable. In particular, the issue of Commonwealth Care funding for legal immigrants, while important in its own right, has led many observers and critics to conclude mistakenly that health reform is unraveling.
These critics ignore the fact that the fundamental problem is not the costs of Commonwealth Care, but rather the unprecedented collapse of state tax revenues. With the state facing a structural budget gap of $5 billion in fiscal 2010, virtually every state program has hit the cutting board. And as is always the case during economic downturns, caseload-driven programs like Commonwealth Care experience a temporary increase in enrollment.
Critics also confuse the costs of health reform with spending on Medicaid, which at $8.5 billion accounts for about 30 percent of the state budget. The relentless increase in Medicaid costs has bedeviled state policy makers for the past quarter century as that program consumes an ever larger share of the state budget.
How has Massachusetts been able to reduce the number of uninsured to less than 3 percent of its population while spending so few new public dollars? To a large degree, the answer can be found in the unique way the law’s programs and incentives act in concert to expand access to subsidized coverage for low-income families largely through a reallocation of funds from uncompensated care, while also encouraging enrollment in employer-sponsored and individual health insurance plans.
With individuals required to have health insurance, many have enrolled for the first time in their employer’s plan or purchased private coverage on their own. Employer-sponsored enrollment has grown by 150,000 and individuals’ private coverage by 40,000 since health reform was adopted. The Foundation estimates that the added cost to Massachusetts employers for newly insured employees and dependents is at least $750 million - more than double the $350 million increase in state spending under health reform.
To be sure, Massachusetts, like the nation, must address the escalating costs of healthcare - for government, employers, and individuals alike - and Massachusetts has launched a variety of efforts to deal with this intractable problem. But this persistent problem has little to do with the health reform law. These are extraordinarily difficult times for all of state government, and it is not helpful to advance unfounded allegations about the unaffordability of health reform. We need to stay the course on one of the most important state initiatives of recent times, which has become a beacon for the rest of the nation.
-
Michael J. Widmer is president of the Massachusetts Taxpayers Foundation.
-
------------
"From Massachusetts: Health care reform 'dos and don'ts'"
By Steve Leblanc, Associated Press Writer, Friday, Jul 24, 2009
BOSTON – Three years into its experiment with near-universal health care, Massachusetts has some "dos and don'ts" for the nation as it grapples with the best way to cover tens of millions of uninsured Americans.
Do require that virtually everyone have health insurance, the overriding goal in Massachusetts. Don't ignore rising costs, the single greatest threat to the law's long-term affordability.
Those who designed and implemented the nation's most ambitious health care overhaul make those suggestions and more: get employers to help pay for the plan, ask taxpayers to subsidize insurance for the poor, and embrace some new regulation.
The landmark 2006 law requires every Massachusetts resident who can afford health insurance obtain it, either through their employer, a private plan, or — for low-income residents — through a new subsidized state program. Those who don't are fined.
The law allowed Kathy Riley, 59, to get a state-subsidized plan for $51 a month after losing her insurance when she cut back her hours to care for her ailing mother.
"This was absolutely perfect," the Wilmington resident said. "Otherwise I wouldn't have any insurance."
The law has been a success in getting 97 percent of residents in health plans, compared with 94 percent before it took effect. But costs to the state have been climbing, thousands have paid tax penalties for being uninsured, and some of the newly insured are struggling to find doctors.
"As we look at health care reform nationally, it's very important to look at what has worked on the ground," Health and Human Services Secretary Kathleen Sebelius said during a recent visit.
A key part of the state plan, and an element federal lawmakers are considering, is the "individual mandate" — the requirement that everyone who can afford health care be insured or face a penalty.
President Barack Obama, who has made universal health care his top domestic priority, said Wednesday he favors an individual mandate as long as it includes a hardship exemption. Massachusetts exempts those who can't find affordable plans.
And like Massachusetts' law, Obama said he hopes his plan will end up covering nearly everyone.
"The overwhelming majority of Americans want health care, but millions of them can't afford it," Obama said. "The basic idea should be that in this country, if you want health care, you should be able to get affordable health care."
The individual mandate has irked some Massachusetts residents who argue they shouldn't be fined for being uninsured. The penalty is now about $1,000 for those who are uninsured for an entire year.
But backers say the mandate distributes risk over a wider population and ensures everyone has a stake in their care.
"Clearly there are some things here that we think have worked and can work nationally," said Jon Kingsdale, executive director of the Massachusetts Health Care Connector, which oversees the law. "One is the whole concept of shared responsibility."
That includes asking employers to contribute to their workers' coverage and asking taxpayers to help cover low-income people, he said.
But Massachusetts' plan has been dogged by rising costs.
In its first year, the budget for Commonwealth Care, the subsidized insurance, soared from $472 million to $628 million as the uninsured flooded into the program faster then anticipated. After leveling off, enrollment has begun creeping up again as the state's jobless numbers grow.
"We have never really been able to put the program on autopilot," said Connector Authority Board Chairman Leslie Kirwan, adding the state "clearly made the decision to go forward with access before wrestling with cost."
The law is starting to show other signs of strain.
The Connector board has been forced to make some budget cuts and a major Boston hospital has sued, claiming the state illegally reduced the amount it pays the hospital for treating a Medicaid patient to help cover the cost of the health care law.
Michael Tanner, a senior fellow at the Cato Institute, faulted Massachusetts for not addressing costs early on, and said the nation should avoid the same mistake.
"The goal of health care reform at the national level shouldn't be measured in whether we can get a piece of paper in everyone's hand saying they are insured," he said.
The business-backed Massachusetts Taxpayers Foundation said health care costs are not out of control. In a recent report, the group said the cost of the law has been "relatively modest and well within early projections."
To control costs, Massachusetts is now weighing a change in the system it uses to pay doctors, so they would be rewarded for keeping patients healthy, not performing more tests.
Former Gov. Mitt Romney, who signed the law, said one important lesson was Massachusetts' decision not to create a separate government insurance plan — an option Obama strongly favors to compete with private insurers to reduce costs.
"That's the biggest flaw in President Obama's proposal," said Romney, a former Republican presidential contender who is mulling a 2012 run.
Instead, Massachusetts created a subsidized insurance program for those earning up to three times the federal poverty level. A second, non-subsidized program lets those earning more to choose from an array of lower cost private plans.
Commonwealth Care, the subsidized plan, now covers about 181,000 adults.
Romney also said any national plan should also avoid mandating specific benefits, such as prescription drug or mental health coverage, something Massachusetts does. Romney said insurers should instead be allowed to offer a wider range of benefits in their plans.
Massachusetts's experience also shows the importance of regulating the insurance market, according to Sen. Edward Kennedy, who said insurers shouldn't be allowed to avoid covering the sick, while competing for the healthy.
A final lesson from Massachusetts was the decision not to nail down every last detail before forging ahead.
"This is a gargantuan task. It cannot all be thought out in one piece of legislation," Kingsdale said. "Three years into it, we're still learning."
------------
"Massachusetts medical leaders wary of healthcare overhaul’s cost"
By Robert Weisman, Boston Globe Staff, July 28, 2009
If you want to know how the proposed overhaul of the US healthcare system may play out nationally, talk to top executives at the biggest medical and life sciences companies in Massachusetts.
As the heads of leading hospitals, insurers, and biotechnology companies, they have dealt with the complexities of near-universal healthcare since 2006, when Massachusetts became the first state to mandate insurance coverage. That gives them a unique perspective on the national effort to overhaul healthcare.
As the debate in Washington heats up, local executives warn that two goals of the Obama administration - expanding insurance coverage and controlling spending - may prove incompatible. And as Massachusetts strains to deal with the increasing costs of its successful healthcare program, they raise questions about who will pay for the projected $1 trillion cost on the federal level.
“Healthcare isn’t free, and if more people want an MRI on demand, that isn’t going to reduce costs or improve care,’’ said Ellen M. Zane, president of Tufts Medical Center in Boston. To make reform work on such a big scale, Zane said, the burden will have to be shared by providers, insurers, employers, and patients.
Most Massachusetts business leaders agree the healthcare system needs major surgery. But they have their own particular concerns about the impact of proposed healthcare changes on their organizations’ health, underscoring how difficult it will be to reach consensus.
Hospitals and doctors say that lower federal reimbursements could hurt the quality of medical care, while insurers chafe at a proposed government-run health plan they argue would put them at a competitive disadvantage.
At the same time, biotech and medical-device makers say the focus on cost savings could hinder their ability to develop life-saving drugs and innovative devices.
Details have yet to emerge on the healthcare plan, but some provisions, especially coverage of an estimated 47 million uninsured US citizens, are likely to mirror steps already taken here.
Cost is a proven issue. Nationwide, hospitals have committed themselves to forgoing $155 billion in government reimbursements over 10 years, but even that may not be enough. James J. Mongan, chief executive of Partners HealthCare, which operates Brigham and Women’s and Massachusetts General hospitals, said providers must find ways to deliver top care for less money.
“The hospitals understand they’re going to have to give up something, but believe there’s room for more efficiency over the coming decade,’’ said Mongan. He said Partners hospitals are working to cut costs, through methods such as improved disease management and electronic medical records.
Hospital executives said those steps may eventually pare expenses, as will preventive care if more people sign up with primary care doctors. But a wave of newly insured patients will almost certainly drive up short-term costs for insurers and employers, executives said.
That has happened in Massachusetts. The stress of paying for universal coverage is showing, too; last month, the Connector Authority, which oversees the state’s healthcare program, cut $155 million, or about 12 percent, from Commonwealth Care, which subsidizes insurance for low-income residents.
With the federal government proposing to decrease reimbursement payments to hospitals at the same time they are forced to take on more patients, “what you could get is a gradual degradation in the ability of hospitals to deliver services,’’ said Paul Levy, president of Beth Israel Deaconess Medical Center in Boston.
Ralph de la Torre, chief executive of Caritas Christi Health Care, a six-hospital chain, said hospitals will have to make smarter choices about care. “It needs to be more based on quality and less based on the number of procedures,’’ said de la Torre, who suggested doctors can be too quick to order tests.
For insurers, the biggest stumbling block is a government insurance plan, proposed by President Obama as an alternative to private insurers.
“Proponents say it will add a level of competition,’’ said Cleve L. Killingsworth, chairman of Blue Cross and Blue Shield of Massachusetts, based in Boston. “But when you’re introducing a plan that doesn’t have to make a [profit] and can go to the Treasury to get bailed out, you’re creating an unlevel playing field.’’
James Roosevelt Jr., president of Tufts Health Plan in Watertown, said the national overhaul effort is taking aim at some problems - such as the exclusion of patients with pre-existing conditions - that are more prevalent nationally than in Massachusetts. The government could set lower prices, forcing insurers to follow suit, Roosevelt said, possibly limiting care for many people. “Providers would get less money and fewer conditions would be covered,’’ he said.
Massachusetts life sciences companies worry about unintended consequences. Trimming budgets at teaching hospitals could crimp their ability to collaborate with researchers on medical devices and biotech drugs, executives said. For medical-device makers, there is the added concern that expanded healthcare could be financed partly by taxing their products.
“We have to make sure that, in making changes, we don’t damage patient outcomes or innovation,’’ said Ray Elliott, who took over this month as president of Boston Scientific Corp., a Natick maker of stents, defibrillators, and other medical equipment.
US drug companies have pledged $80 billion in cost savings to help build a new healthcare system. But deliberations on Capitol Hill have left industry leaders wary about price controls on drugs. Companies say they depend on high profits to cover research and development. That’s especially true of biologic drugs - costly treatments made from living cells that have allowed Massachusetts’ biotech sector to grow. “If they do this in a way that interrupts the innovation cycle, that would be a very high cost,’’ said Henri A. Termeer, chief executive of the Cambridge-based biotech Genzyme Corp.
-
Robert Weisman can be reached at weisman@globe.com.
-
------------
www.ama-assn.org/amednews/2009/08/03/gvl10803.htm
------------
-

-
"Health fund for jobless runs low: Surging enrollment empties state coffers Businesses chafe at talk of tax hike"
By Kay Lazar, Boston Globe Staff, August 5, 2009
A unique state program that helps pay most health insurance costs for 27,000 unemployed Massachusetts residents is on the cusp of going broke, setting off a debate between healthcare advocates and business leaders who say funding it is a burden on companies fighting for their survival.
The state’s Medical Security Program, financed solely by a tax on employers, will run out of money in January because of the surge in unemployment over the past year, state officials said yesterday. The most logical way to maintain it, officials said, is to increase the per-employee tax, which hasn’t been raised since 1990.
“In order to save the program, something has got to be done to get more revenue,’’ said Robb Smith, director of policy and planning at the Massachusetts office of Labor and Workforce Development, which oversees the program.
But business leaders say that keeping the program afloat by hiking the tax on employers - $16.80 per employee, per year - would hit hard on many companies already battered by higher costs across the board.
“At some point we have to take a good look at the economy and employers’ ability to keep the doors open and decide whether we are maybe being too generous,’’ said Jon Hurst, president of the Retailers Association of Massachusetts.
The program’s rate of growth this year has been defying monthly calculations. Enrollment is up 186 percent since last summer, reaching more than 27,000 as of June. Not all of the state’s roughly 250,000 unemployment recipients qualify. The program is geared toward middle-income people who made too much money to qualify for Medicaid and other state-subsidized healthcare programs designed for the poor.
A three-member board meets annually in November to monitor the program’s finances and will probably vote then to make changes, Smith said. No legislative approval is needed to raise or lower the employer tax. While the program had $49.2 million in reserves in June, it spent over $28 million in the most recent quarter. The monthly expenditures surged 70 percent alone from April to June.
“We think we’ll be OK until November, but it’s next year we are really concerned about,’’ Smith said. “With the trends we have now, we will probably run out of money [in January] unless something dramatically changes . . . or unless we see a really quick recovery, which I am not counting on.’’
Traditionally the state program has paid 80 percent of a qualified laid-off worker’s monthly health insurance premium for as long as the worker is collecting unemployment benefits. Because the federal government designated stimulus money earlier this year toward health insurance for the unemployed, most recipients are paying about 9 percent of their monthly premium. For those who can’t afford to keep their previous insurance, even with the subsidies, the state program provides basic health coverage and charges recipients modest copayments of about $15 for a doctor’s visit.
For Weymouth resident John Phelan, who lost his retail job in January, the prospect of the Medical Security Program going broke is unsettling. It has helped him afford to keep the insurance he had while working, so he pays just under $200 a month.
“It’s such a relief, so I don’t have to look for affordable health insurance while I am looking for a job,’’ he said. “Just knowing it’s there, should I get sick, is a huge load off my mind.’’
Launched 19 years ago under the administration of governor Michael S. Dukakis, the Medical Security Program is unique to Massachusetts. Governor Deval Patrick transferred $15 million out of the fund last fall - before unemployment spiked - to help pay for other insurance subsidy programs. The tax on businesses to fund the program has not been raised since it was created.
But business leaders said it’s time to abolish this program, given the state’s 2006 overhaul of the health insurance system. That revamp included the creation of another insurance program to help lower-income residents afford coverage. It is run by a different state agency than the Medical Security Program, has different eligibility requirements, different rules, and a different target: the chronically poor.
“It doesn’t make sense to be running two separate programs with two administrative departments,’’ said Rick Lord, president of Associated Industries of Massachusetts, the state’s largest business trade group.
Lord said officials should merge the two programs, instead of hiking the tax on employers, and subsidize both programs from the state’s general fund. The Medical Security Program is the only state insurance program funded by a tax on employers.
Smith, the state director, said officials are considering some form of merger, but are unlikely to get rid of the tax on employers.
“We will be unveiling reforms in the fall to help make the system more integrated,’’ he said, while declining to provide details.
Other business leaders said officials should consider lowering benefits in the Medical Security Program, as it has done during other recessions.
“There’s probably not a worse tax the state could do now on businesses,’’ said Bill Vernon, state director the National Federation of Independent Business, which primarily represents smaller companies.
Smith said lowering benefits is not a legal option without renegotiating agreements with the federal government.
Unlike other state-run health insurance that is geared to lower-income residents, the Medical Security Program is open to people who have been making substantially higher salaries. Eligibility is calculated by adding a family’s income for the six months prior to an applicant’s unemployment to projected income for the next six months. The total annual income can not exceed 400 percent of the federal poverty level, which translates to as much as $88,200 for a family of four.
As business and state leaders debate the future of the unusual program, Health Care for All, a large consumer group, says the lifeline needs to be resuscitated and asking businesses to pay more is reasonable.
“The tax on employers hasn’t gone up since 1990,’’ said Brian Rosman, the group’s research director. “We would certainly support examining the employer tax, to bring it in line with increased costs since then.’’
-
Kay Lazar can be reached at klazar@globe.com
-
------------
"Health care agency’s payroll bloated: Staff, salary has ballooned since inception"
By Hillary Chabot and Joe Dwinell, Thursday, August 6, 2009, www.bostonherald.com - Local Politics
The payroll at the agency steering the state’s controversial universal health care effort has swollen to more than four times its original size in just 18 months - with a top-heavy bureaucracy led by dozens of high-paid managers, newly released records show.
The Commonwealth Health Insurance Connector’s staff and salary explosion - including 17 managers now paid more than $100,000 a year and numerous contracted employees - has continued despite protest from Beacon Hill lawmakers.
“At a minimum, all of the salaries need to be frozen and reviewed with an eye towards cutting them, and there should be a hiring freeze,” said Sen. Mark Montigny (D-New Bedford), vice chairman of the Legislature’s public health committee. “We’re in a crisis. That’s what happens when we’re in a crisis.”
The Massachusetts universal health coverage mandate - the creation of former Gov. Mitt Romney - is being ripped by critics of President Obama’s health care plan as a glaring example of out-of-control costs, jacked-up insurance rates and failed goals.
In a recent letter to the Minnesota congressional delegation, Gov. Tim Pawlenty compared Obama’s plan to the Bay State’s, noting: “That state’s experience should caution Congress against this approach” because “costs have been significantly higher than expected.”
Despite the national spotlight on its first-in-the-nation work, the Connector agency has in just a year and a half larded its bureaucracy with a dozen directors and assistant directors, and 14 bosses with the word “manager” in their titles. It also doled out 3 percent raises this year. The agency has 89 staffers on its payroll and is headed by Executive Director Jon M. Kingsdale, who makes $238,703.
Richard Powers, spokesman for the Connector, defended the salaries, saying they are in line with the employees’ “experience, knowledge and responsibilities.”
“There are people who came here from the private sector who took a cut in pay just to be involved in something that’s cutting edge,” Powers said.
Saying the agency was in “ramp-up mode” when there were only 22 employees in 2007, Powers said they had always projected a roughly 50-member staff.
The Connector has signed up 439,000 newly insured Bay State residents since it was created by the Legislature in 2006. Customers pay between 3.5 to 4.5 percent from their insurance costs for the agency’s salaries, Powers said.
The state, which has struggled with subsidizing the new law, spent $800 million to insure low-income residents last year.
In some cases, the Connector’s titles appear redundant. There is, for example, a chief communication officer, chief information officer, director of public affairs and chief marketing officer - all at six-figure salaries.
“The agency has exceeded my worst expectations. It’s clearly bloated and top-heavy with a number of positions that seem to be expendable,” said David Tuerck of the Beacon Hill Institute, a conservative think tank.
Rick Lord, head of Associated Industries of Massachusetts, who sits on the unpaid board that oversees the Connector, said he would be open to re-examining the higher payroll now that the state has insured all but 2.6 percent of the population. “It’s always good to revisit these issues on some kind of regular basis,” Lord said.
The Connector is just one of 52 quasi-state agencies under review by Gov. Deval Patrick, who announced the study after his disastrous push to install Sen. Marian Walsh as the $175,000 assistant director of the Health and Education Facilities Authority.
“The very life of these quasis should be in jeopardy,” said Montigny. “Their only purpose is to provide inflated salaries and bury patronage hires, and they’re generally less accountable and less effective.”
------------
"Too many Chiefs?"
By Herald staff, Thursday, August 6, 2009, www.bostonherald.com - Local Politics
The quasi-state agency Commonwealth Health INS Connector has 16 employees making over $100,000 per year.
Jon M. Kingsdale Executive Director $238,703
Rosemarie W. Day Deputy Director & Chief Operating Officer $186,188
Patrick M. Holland Chief Financial Officer $185,658 Joan E. Fallon Chief Communications Officer $184,306
Kevin J. Counihan Chief Marketing Officer $181,602
Jamie W. Katz General Counsel $173,774
Robert E. Nevins Chief Information Officer $161,136
Melissa A. Boudreault Director of Commonwealth Care $148,526
Patricia Andriolo-bull Director of Commonwealth Choice $147,445
Dominic M. Divito Director of Accounting $121,115
Michael A. Norton Manager Of Mmco Contracts $120,227
Christine Ballas Manager of Commonwealth Care Operations $110,583
Paul D. Wingle Director of Outreach-Commonwealth Choice $109,772
Steven P. Mcstay Senior Project Manager $110,000
Richard R. Powers Director of Public Affairs $103,211
Nicoletta Conte Director of Outreach-Commonwealth Care $100,052
------------
"Massachusetts health insurers post losses: Increased use of benefits is among contributing factors"
By Robert Weisman, Boston Globe Staff, August 15, 2009
The state’s four health insurers posted net losses for the second quarter, citing continuing pressure from the economic downturn.
Among the factors contributing to the nonprofits’ performance were increasing medical expenses, higher claim costs associated with newly insured members, employers shifting to less profitable products, and people using more health services because they fear losing their jobs and company-paid insurance coverage.
Last year, all four insurers showed gains during the second quarter.
Because the state is a highly competitive insurance market, health plans typically operate on thin margins. But the recession has eroded their profitability, at least temporarily, according to financial reports filed with the state Department of Insurance.
“We’ve been seeing some signs of increased utilization of health care services that appears to be fueled by people anticipating losing their jobs or by people who have already been terminated but haven’t yet lost their health benefits,’’ said Jim DuCharme, chief financial officer at Harvard Pilgrim Health Care in Wellesley, the state’s second-largest health insurer.
DuCharme said it is too soon to say whether the trend will accelerate enough to throw off insurers’ budget projections for the rest of 2009.
Health plans say they expect their financial conditions to improve in the second half of the year when higher premiums - paid by employers to insurers - typically go into effect.
Boston-based Blue Cross and Blue Shield of Massachusetts, the state’s largest health plan, reported the biggest net loss: $33.6 million for the three months ending June 30. That included a $23.1 million loss for its health maintenance organization subsidiary. The insurer posted combined income of $30.8 million in last year’s second quarter.
Fallon Community Health Plan, based in Worcester, reported a net loss of $3.9 million for the April-to-June period, compared with net income of $1.2 million for the same quarter in 2008.
Harvard Pilgrim Health Care posted a loss of $2.3 million for the most recent quarter. It had net income of $600,000 last year.
Tufts Health Plan in Watertown had the narrowest deficit of the four insurers, reporting a second-quarter net loss of $204,000. A year ago, it posted quarterly income of $24.9 million.
-
Robert Weisman can be reached at weisman@globe.com.
-
------------
TELL ME WHERE IT HURTS
"Mass. numbers crunched"
The Boston Globe, Letters, August 16, 2009
THE AUG. 5 editorial “Mass. bashers take note: Health reform is working’’ states that “the cost to the state taxpayer’’ of the Massachusetts health reforms is “about $88 million a year.’’ In fact, the cost to state taxpayers is 19 times that amount, while the total cost is 24 times that amount.
The Massachusetts Taxpayers Foundation explains that the $88 million figure represents not the total cost to the state government, but the average annual increase in the state government’s costs.
Worse, the editorial ignores new spending by the federal government and the private sector, which account for 80 percent of the law’s cost.
According to Massachusetts Taxpayers Foundation estimates, health reform will cost at least $2.1 billion in 2009. The total cost to state taxpayers is at least $1.7 billion and growing. (The fact that other states’ taxpayers bear the balance should not be a source of pride.)
One wonders how such a distortion comes to appear on a leading editorial page.
Michael F. Cannon
Director of health policy studies
Cato Institute
Washington
------------
-

-
"Bay State health insurance premiums highest in country: Rein in health costs, Massachusetts urged"
By Kay Lazar, Boston Globe Staff, August 22, 2009
Massachusetts has the most expensive family health insurance premiums in the country, according to a new analysis that highlights the state’s challenge in trying to rein in medical costs after passage of a landmark 2006 law that mandated coverage for nearly everyone.
The report by the Commonwealth Fund, a nonprofit health care foundation, showed that the average family premium for plans offered by employers in Massachusetts was $13,788 in 2008, 40 percent higher than in 2003. Over the same period, premiums nationwide rose an average of 33 percent.
The report did not break out how much premiums have increased in Massachusetts since the 2006 changes went into effect, so it does not show whether the law affected the rate of price increases. Still, with the state’s law often cited as a model for a national health care overhaul, advocates on various sides of the issue said the report underscores the urgency of including cost controls in any large-scale federal or state overhaul.
“While expanding coverage was the logical first step in Massachusetts, cost control is equally as important,’’ said Andrew Dreyfus, an executive vice president at Blue Cross Blue Shield of Massachusetts, the state’s largest private insurer with 3 million members. “And if you don’t face the cost issue directly, then you can jeopardize the progress you’ve made in expanding coverage.’’
President Obama has championed a national health care overhaul that includes cost controls, as well as coverage expansion to nearly every American. But critics have questioned some of his administration’s projected savings, and his proposal for a public insurance plan to compete with private insurers is faltering in Congress.
In Massachusetts, brokering the 2006 overhaul was such a delicate and years-long undertaking that the disparate interest groups - insurers, businesses, consumers, hospital and doctors organizations - all agreed to first tackle health coverage expansion and leave the cost question for a later date.
Now, the Commonwealth Fund report projects that without significant cost reforms, an annual family premium in Massachusetts will soar to $26,730 by 2020.
While Massachusetts residents face the highest premiums in the country, the costs do not eat as big a hole in the typical family budget as in most other states, the report said. That’s because household income in Massachusetts is much higher than the national average. For middle class families that make too much to qualify for state insurance subsidies, however, the premiums can be a significant burden.
One of the first steps to control costs was taken last year, when the Legislature passed a sweeping bill sponsored by Senate President Therese Murray, Democrat of Plymouth. Among other provisions, it restricted some payments and gifts to doctors from pharmaceutical and medical device companies and created a commission to recommend changes in how providers are paid.
Last month, the commission suggested that private and public insurers scrap their method of paying doctors and hospitals negotiated fees for individual visits or procedures, and instead put providers on a “global budget,’’ paying a set amount intended to cover a patient’s medical care for an entire year.
The idea is so controversial and the suggested fix so time-consuming to achieve that the commission recommended phasing it in over five years.
But other efforts to control health spending are already moving ahead.
Blue Cross, for instance, is already signing up providers to participate in an insurance plan similar to the commission’s recommended “global budget,’’ and it now covers nearly 20 percent of its patients in health maintenance organizations.
Health Care for All, a Boston-based consumer group, is pushing interim steps that include reducing payments to hospitals for patients who have to be readmitted because of preventable complications.
“This report heightens the urgency of doing these short-term steps now,’’ said Health Care for All’s research director, Brian Rosman.
Another panel, created by the 2006 law, is poised to release a report in September that will probably detail specific interim measures that can be taken to rein in costs.
Anya Rader Wallack, a council member, said one of the big cost drivers in the state’s health insurance system is that Massachusetts residents like their big, brand-name hospitals, perhaps too much.
“We tend to use more academic medical centers, which are expensive and are, in general, more expensive than community hospitals or nonhospital settings,’’ Wallack said.
In many other states, she said, patients tend to have more medical tests and procedures done in nonhospital settings. She would not disclose the remedies being considered by her group, but the panel has posted price-comparison data for Massachusetts hospitals on its website.
Bottom line, said Dr. Marylou Buyse, president of the insurers’ trade group, the Massachusetts Association of Health Plans, is that the high cost of health insurance is not necessarily the insurer’s fault.
“The increase [in Massachusetts premiums] is attributed to an increase in charges by physicians and hospitals,’’ Buyse said, referring to a 2008 state report that tracked the trend from 2002 to 2006.
The Commonwealth Fund report concluded that a number of changes, including limits on insurance companies’ administrative costs and profits, as well as changes in the way doctors and hospitals are paid, could bring better-quality patient care and could reduce national costs by an average of 1 to 1.5 percentage points per year over the next decade. That translates to a savings of $2 trillion to $3 trillion nationally, the report said.
-
Kay Lazar can be reached at klazar@globe.com.
-
------------
"Will safety net hospitals survive health reform?"
By Carla K. Johnson, AP Medical Writer, September 7, 2009
CHICAGO --Janie Johnson has no health insurance, so when she cut her toe while giving herself a pedicure, she limped to the emergency room at one of Chicago's safety net hospitals and waited her turn.
"I'm 44, but I probably look about 55 right now," Johnson joked in Stroger Hospital's emergency department where more than 100 patients sat waiting. Urgent cases, from chest pains to gunshot wounds, are rushed to doctors first. Johnson was glad to have somewhere to go for health care.
"I don't know what I would do" without the hospital, she said. "My health would probably get worse."
To all the knotty issues involved in health care overhaul, add one more: The proposals in Congress may threaten the funding and future of the nation's already-struggling safety net hospitals.
It's an irony hospital leaders are expressing quietly as Congress reconvenes this week to take up health care again. Hospital leaders support expanding insurance coverage to more Americans, but they worry financing the expansion will cause some teetering urban hospitals to deteriorate and close.
They point to Massachusetts, the laboratory for health care overhaul, where one safety net hospital, Boston Medical Center, is suing the state claiming it's covering too much of the cost for expanding coverage. Another safety net standby, Cambridge Health Alliance, has closed health centers and cut services; its Somerville Hospital no longer keeps patients overnight.
"It looks like a national plan will be modeled on Massachusetts and it's a disaster for poor people," said Dr. Steffie Woolhandler, Harvard Medical School professor and a doctor at Cambridge Hospital.
"The insurance offered doesn't cover everyone," she said. "It's filled with gaps like copayments and deductibles. Patients can't afford it, so they turn to the public sector and the public sector isn't there anymore."
What worries Woolhandler and others are proposals to finance national reform that would reduce payments gradually to hospitals handling more than their share of uninsured patients. One proposal would reduce these funds -- called DSH payments for "disproportionate share hospital" -- by $20 billion, in three large annual chunks starting in 2017.
About 2,700 U.S. hospitals receive DSH payments. That's about half the nation's hospitals, according to the American Hospital Association.
A small segment of those hospitals provides most of the nation's charity care to the poor. These institutions, largely supported by reimbursements from Medicaid and other government insurance programs, receive 12 percent of their revenues from DSH payments.
Lawmakers reason that when more Americans have insurance, there will be less need for the payments. Instead, hospitals would get paid by their newly covered patients' insurance plans. A trigger in the House health care legislation would start the cuts only after the nation achieved a significant increase in insurance coverage.
But critics say illegal immigrants, the mentally ill and drug addicts will keep arriving at safety net hospitals without insurance. Illegal immigrants will be ineligible for the expanded coverage proposed by Congress. The mentally ill and addicted will be unlikely to sign up.
"If they start cutting, I'm scared," said Dr. Simon Piller, who cares for patients at a county clinic that's part of the same health system as Stroger Hospital. He describes patients who've lost jobs, are living with friends and ran out of medications for chronic conditions months, or years, ago.
Safety net hospitals will continue to have unusual expenses, such as translation services and security, to deal with. And some newly insured patients won't be able to afford the out-of-pocket copays and deductibles.
"Copays for us are no-pays," said Dr. Steven Safyer, president and CEO of Montefiore Medical Center in New York City. "Health care reform to me is an issue of humanity. How you can have 47 million uninsured in this country is shocking. But you can't throw the baby out with the bathwater."
DSH cuts are part of a deal the White House reached with the American Hospital Association and two other hospital groups. When the hospitals agreed to cuts totaling $155 billion over 10 years, a group of public hospitals wasn't at the table.
"We were never part of the negotiations and did not sign onto the agreement," said Larry Gage, president of the National Association of Public Hospitals and Health Systems. The group contends DSH payments also help maintain trauma centers, burn units and other community assets that could be threatened.
Nancy-Ann DeParle, who directs the White House health reform office, said there's adequate protection for safety net hospitals in the House bill. The payments would be reduced -- gradually and starting only after the rate of uninsured Americans declines -- in a way that differs greatly from what happened in Massachusetts, DeParle said.
President Barack Obama supports phasing in DSH reductions over 10 years.
"As people get insurance, there will be less of a need for hospitals to get additional funds," DeParle said. She acknowledged it may be "scary" for hospital administrators to shift from getting these additional payments to a reality where more of their patients have insurance cards.
But hospitals can and must adapt, DeParle said. "We will always need safety net hospitals."
It's unclear how much would be cut. The House legislation calls for cuts of $20 billion, representing 8 percent of what the Congressional Budget Office projects in federal outlays to DSH over 10 years. The White House supports larger cuts.
Many urban hospitals already operate on small margins or at a loss. Chicago's Mount Sinai Hospital had only 1.42 days of cash on hand in August. Its bad debt, the bills left unpaid by patients, was $62.3 million last year. It received $10 million in DSH money last year.
Stroger is a public hospital, subject to cuts from Cook County government. The county's health system is considering laying off nearly 500 workers. Chicago's Stroger Hospital received $42 million last year in DSH.
"This is definitely going to be a change. It's not health care as usual," said Stephen Zuckerman, a health economist in the Urban Institute's Health Policy Center in Washington.
Safety net hospitals may need help raising money to spruce up and modernize to become more competitive with private hospitals, Zuckerman said. But they won't disappear.
"The capacity they provide to the system is going to be needed," Zuckerman said. "I don't think the rest of the system is ready to absorb the patient population the public hospitals now serve."
Lawmakers have wanted to cut DSH payments for years, said Wendy Parmet, health law professor at Boston's Northeastern University School of Law. With rising Medicare and Medicaid costs driving up national debt, the payments will continue to be a juicy target, she said.
"Hospitals are going to cry that it hurts," Parmet said. "But it's going to happen, whether or not there's health insurance reform."
-
On the Net:
National Association of Public Hospitals and Health Systems: www.naph.org
American Hospital Association: www.aha.org
-
------------
"Questions, answers on requiring health insurance"
By Steve Leblanc, Associated Press Writer, September 9, 2009
BOSTON --Should the federal government require virtually all Americans to be insured or face thousands of dollars in fines? Proponents say this requirement is crucial to extending coverage and reining in costs as Massachusetts has done. Critics say it would impose an unfair burden on individuals and families already struggling in harsh economic times.
A look at the issue in question-and-answer form:
------
Q: What's being proposed?
A: Democratic Sen. Max Baucus of Montana, chairman of the Senate Finance Committee, is proposing that, as part of any overhaul, insurance be mandatory for all Americans, much the way car owners are required to have auto coverage. People making up to three times the federal poverty level -- about $66,000 for a family of four and $32,000 for an individual -- would be eligible for tax credits to help cover the cost of premiums. Those who fail to get insurance would face stiff fines, from $750 a year for an individual to $1,500 for families. The maximum penalty on individuals would be $950, while families could face maximum fines of $3,800.
------
Q: What is the proposal based on?
A: The plan is based in part on an element of Massachusetts' sweeping health care law, known as an "individual mandate." When Massachusetts passed the 2006 law, it became the first state to require that virtually all residents have health insurance or face a series of steadily increasing fines. To help soften the penalty, Massachusetts first created state subsidized insurance plans for those earning up three times the federal poverty level, with the poorest residents getting essentially free care and those earning more paying increasingly higher premiums and copays. The state also created a Health Care Connector -- similar to the "health care exchange" being proposed on a federal level -- to help those ineligible for subsidized care connect with lower-cost private health plans. Finally, Massachusetts decided to exempt from fines for anyone who doesn't qualify for the subsidized plans but still can't find any affordable private plan based upon state affordability standards.
------
Q: Who has been fined in Massachusetts?
A: Massachusetts decided to phase in its fines. During 2007, the first full year of the health care law, those who refused to get insurance lost the personal exemption on their state tax returns -- equivalent to a $219 fine. In subsequent years, the fines were scheduled to increase dramatically. In 2008, a fine for an individual who could afford insurance but refused was $76 for each uninsured month or $912 for the entire year. For couples, the maximum fine for the entire year would be $1,824. In 2009, the fines increased again, to $89 a month or $1,068 for an entire year for an individual. For couples, the maximum fine was $2,136.
------
Q: So how many people have actually been fined in Massachusetts?
A: The state has so far only released numbers for the first year. In 2007, nearly 3 percent of state's taxpayers -- about 97,000 filers -- were uninsured even though they could have afforded health care and were stripped of the $219 exemption. An additional 2 percent -- or about 62,000 filers -- were found not to earn enough for health care and weren't fined. The state allows taxpayers to appeal the fines. Numbers for 2008 are expected later this year.
------
Q: Why have fines at all?
A: There are a few basic arguments for requiring health care for as many people as possible. One argument is that it spreads risk among as wide a group as possible, which helps lower overall costs. Another argument is that insuring the largest number of Americans will take some of the pressure off premiums for those who are already insured. President Barack Obama has said insured Americans pay what amounts to a hidden fee to help pay hospitals for the cost of covering the uninsured. Without fines, advocates say, there would be no way of enforcing the mandate.
------
Q: What has Obama said about an individual mandate?
A: During the presidential campaign, Obama criticized the idea of fining individuals for not having health insurance. During a Democratic debate in February 2008, Obama warned that fines could lead to a situation like that in Massachusetts, where, he said, some residents were choosing to accept a fine because it was less expensive than health care premiums. "We don't want to put adults in a situation in which, on the front end, we are mandating them, we are forcing them to purchase insurance, and if the subsidies are inadequate, the burden is on them, and they will be penalized," he said.
------------
"Feds: Massachusetts health plan has problems"
By Jennifer Heldt Powell / Small Business Matters, Sunday, September 20, 2009, www.bostonherald.com - Business & Markets
The Bay State hasn’t gone bankrupt or fallen off into the ocean despite dire predictions when sweeping health-care reform requiring everyone to get insurance was passed three years ago.
In fact, there are many wonderful stories about people who have been able to get excellent care because they were able to find affordable insurance. Overall, the changes have been so successful, they have served as a model for federal reforms now being debated in Washington.
That gives chills to some small business owners.
“It’s a horror show,” said Bill Fields of Health Plan Solutions, which advises small business owners on benefits. His job has morphed largely into helping companies stay compliant with the law and figuring out what to do when they haven’t. Some face thousands of dollars in fines even though they offered health insurance.
He’s become a vocal advocate for reforms to the reforms, spending a great deal of time on Beacon Hill fighting for fixes to make things easier for small business owners.
The problem, he says, is in how the law is being administered and confusion over what it says. Small businesses are required to offer health insurance if they have more than 11 employees. But that’s measured by something called “full-time equivalents,” which means it’s about the number of hours employees put in rather than the number of workers.
A small restaurant, for instance, might have five full-time workers and then hire part-time workers for the summer. If those workers put in enough hours, the restaurant falls under the insurance requirement.
Another problem is that in order for a company to comply with the law, at least 25 percent of employees must participate in the company-sponsored plan. That can be difficult for a business with high turnover rates where employees don’t stay long enough to sign up. It’s also a challenge for companies that attract workers who get insurance through their spouse or another job.
Even if a company is compliant and doing everything correctly, the owner still has the burden of proving it.
“There’s a fair amount of paperwork and the state hasn’t been particularly clear about things,” said Tom Erb, president of Electric Time, a Medfield clock manufacturer. “You have to make sure it’s all done right or there are severe fines.”
Small business owners probably wouldn’t mind the paperwork so much if the reforms had curbed costs. But instead, they’re still watching their bills climb in the double digits.
“We must tackle costs if we want to increase coverage on the federal level, as we’re seeing from what’s happening in Massachusetts,” said Amanda Austin, director of federal public policy for the National Federation of Independent Businesses.
The rates for Electric Time were set to jump nearly 30 percent this year. Erb was able to bring the increase down to around 17 percent only by increasing the plan members’ deductible. Seeing what’s happened here, he’s concerned about what’s ahead.
“I’m worried because I don’t see the federal government doing anything efficiently,” he said.
------------
"Many Massachusetts companies fall short on health care"
Associated Press, Thursday, October 1, 2009
BOSTON (AP) -- A state audit has found that a significant number of Massachusetts businesses may not be by complying with the state's landmark 2006 insurance law.
Auditors targeted employers that provided incomplete or inconsistent information to the state in earlier reports. Of the 426 companies audited so far, 172, had violated the law's requirement that most employers contribute a portion of their workers' insurance premiums or pay a penalty.
State officials say those companies combined owed $5 million.
Regulators say 97 percent of Massachusetts businesses are meeting the law's requirements.
Bill Fields, a consultant who has advised dozens of companies about the law, tells The Boston Globe most of the companies falling short are just making honest mistakes.
-
www.topix.net/forum/source/berkshire-eagle/TCTE30MLFOC302R2E
-
www.boston.com/news/health/articles/2009/10/01/compliance_uneven_on_health_care_law/
-
------------
"Massachusetts health care authority closes loopholes"
Associated Press, Friday, October 9, 2009
BOSTON (AP) -- The board that oversees Massachusetts' landmark health care law is moving to close loopholes that allow insurers to cap prescription drug benefits or deny maternity coverage for customers' dependents.
The Boston Globe reports that the new regulations, given initial approval Thursday by the Connector Authority, will be the subject of a public hearing in November before a final vote scheduled for December.
The state's 2006 health care law requires most residents to have insurance that meets minimum standards, but regulators have discovered loopholes that have allowed employers' plans to restrict coverage in ways regulators said they never intended.
The Authority deferred action on a proposal to limit how much consumers pay each year for medications.
-
www.topix.net/forum/source/berkshire-eagle/TTVLFV6HK9F0M3KH7
-
------------
"Doctors prepare for fee change: Efforts to cut costs would overhaul payment system"
By Robert Weisman, Boston Globe Staff, November 21, 2009
Health care providers in Massachusetts are preparing for a dramatic change in how they get paid. But whether the state’s proposed payment system overhaul can succeed in reining in costs and boosting the quality of care will depend on how it’s structured and put into practice.
That was the consensus of speakers on a health care panel yesterday during a summit on business leadership and public policy at the John F. Kennedy Library in Dorchester. The event was sponsored by the Progressive Business Leadership Network, a group that promotes socially and environmentally responsible economic growth.
“We’ve been reinvesting in the infrastructure of our organization to be ready for the moment that’s about to arrive,’’ said Gene Lindsey, chief executive of Atrius Health, a Newton-based alliance of community physicians groups that includes Harvard Vanguard Medical Associates. “We’re ready and excited. We believe that everything we’re doing now is like building Noah’s Ark, and the flood is coming.’’
Lindsey was referring to the recommendation of a special commission created by the state Legislature to stem the annual escalation of health care costs, which, according to Secretary of Health and Human Services JudyAnn Bigby, averages $3,000 more per person in Massachusetts than other states. If left unchecked, Bigby said, state health costs are on track to double between now and 2020.
The commission recommended that Massachusetts insurers and public payers scrap their current method of paying doctors and hospitals negotiated fees for individual visits or procedures. Instead, it wants to put pro viders on a budget, paying a set amount intended to cover the cost of a patient’s medical care for a year.
That proposal, which would have to be approved by lawmakers, is being called a “global payment’’ system.
“The fee-for-services system was viewed uniformly as being broken,’’ Bigby told the panel, citing increases in the volume of tests, procedures, and other services. “The feeling was there’s just too much incentive to do more volume as a way to generate revenue.’’
Yet she acknowledged that “we could reform the payment system and still not get the results we’d like to see.’’ Bigby said the danger is if the state’s biggest hospitals and doctors groups, which would team up as “accountable care organizations,’’ used their clout to command higher reimbursements.
Paul F. Levy, chief executive of Beth Israel Deaconess Medical Center in Boston, said rates paid to insurers already are based on market power, rather than clinical outcomes, under today’s system. He said Partners HealthCare System, the state’s largest hospital group that includes Boston’s Massachusetts General Hospital and Brigham and Women’s Hospital, gets the highest rates, followed by Beth Israel Deaconess.
“Everyone else gets less,’’ Levy said.
To avoid locking that system into place in the new global payments era, Levy said, state government would have to set the rates or require public disclosure of health providers’ insurance rates statewide. That would pressure payers and providers to set rates more fairly, he said.
Another potential problem with a “per body, per year’’ approach is that it could shift the risk of calculating health costs to providers from insurers, which keep larger cash reserves on hand than hospitals, Levy said.
The new system could also make it more difficult for employers to be smart buyers of medical coverage - by designing their insurance plans to give employees incentives to be healthier and find more efficient care, said Philip J. Edmundson, chief executive of William Gallagher Associations, an insurance brokerage company based in Boston.
“One concern of businesses [that] are paying for most of the insurance is that the ability to control costs, manage costs, and get information about costs will no longer be available,’’ Edmundson warned.
Richard Pops, chief executive of Cambridge biotechnology company Alkermes Inc., which makes drugs to treat alcoholism, depression, and other diseases, said a new payment system should be flexible enough to allow insurance coverage of new treatments that drive down medical costs in the long run.
Potential pitfalls notwithstanding, health care companies are preparing themselves for payment changes. That was one goal of an expanded alliance struck last week between Beth Israel Deaconess and Atrius Health that is aimed at controlling costs while maintaining quality.
Lindsey called payment overhaul a first step toward revamping the health care system. “We can be trapped into trying to fix it all at once or just getting started,’’ he said. “I vote for just getting started.’’
-
Robert Weisman can be reached at weisman@globe.com.
-
------------
"Health care subsidy set to expire"
By JIM KINNEY, Business writer, The (Springfield) Republican, November 27, 2009
SPRINGFIELD - A nine-month program put in place by Congress to help subsidize the cost of COBRA health insurance for the unemployed will expire on Tuesday, but a state program will soften the blow for the unemployed in Massachusetts, according to a state official.
"We don't expect that we will have a large number of people in Massachusetts dropping off their medical coverage because they can't afford it," said Gerald A. McDonough, general counsel for the Executive Office of Labor and Workforce Development.
The federally subsidized program covers up to 65 percent of the cost of COBRA. With a state program, called the Massachusetts Medical Security Program picking up 80 percent of the remaining out-of-pocket cost.
The result can be a monthly insurance premium of $9.52 instead of $136.
The state this week released figures showing that 289,700 Massachusetts residents are unemployed. Of those, 31,000 people in Greater Springfield are unemployed, 1,044 in the Amherst area and 1,812 in Greenfield and surrounding towns.
Barbara C. Raines, director of administration and finance at CareerPoint , a one-stop job center in Holyoke, said many long-term unemployed who come to the center will be affected, including at least one person CareerPoint itself laid off due to budget cuts.
COBRA (Consolidated Omnibus Budget Reconciliation Act) programs usually allow people to continue on their previous employer's health-care plan by paying all of the cost of that coverage, including the percentage normally paid by the employer, generally about $380 a month for a single person or $1,250 for a family, Raines said.
The $787 billion federal stimulus package passed in February provided for the COBRA subsidy. Under that plan, the laid-off worker pays 35 percent of the cost and the employer pays 65 percent. Then the employer claims that expense as a deduction on its payroll taxes.
"That way the employer is reimbursed," Raines said.
McDonough said unemployed people in Massachusetts can also apply for the state's Medical Security Program. That program reimburses people for 80 percent of the individual's COBRA costs. Coupled with the federal program, the Medical Security Program can bring an unemployed person's COBRA payments down to about 7 percent of the total cost.
Without the federal subsidy, the state program will still reimburse 80 percent, McDonough said. But it will be 80 percent of a higher cost.
"We like the federal program because it lessens the cost of our Medical Security Program," he said.
The Medical Security Program telephone number is 1-800-908-8801, according to the state.
According to state figures, the Medical Security Program cost $47 million in 2008, $118.8 million in 2009 and is expected to cost $123.7 million in 2010.
Staff members for both U.S. Rep. Richard E. Neal, D-Springfield and John W. Olver, D-Amherst, said the congressmen support extending the federal program. R. Hunter Ridgway, Olver's chief of staff, said the matter might come up when lawmakers return to Washington in December.
-
Jim Kinney can be reached at jkinney@repub.com
-
------------
"Mass. lawmakers may make colleges insure students"
Boston.com - November 29, 2009
BOSTON (AP) -- Lawmakers are weighing a bill to require every full and part-time college student in Massachusetts to have at least the basic level of health insurance required under the state's landmark 2006 health care law.
Under the proposal, any public or private institution of higher learning that fails to insure its students would face fines of $1 per student for every day the student remains uninsured.
All fines would be deposited in the state's Health Safety Net Trust Fund, which helps cover the health costs of the uninsured.
The bill is sponsored by Sen. Richard Moore, an Uxbridge Democrat and Senate chair of the Health Care Financing Committee. The bill is scheduled for a public hearing Thursday at the Statehouse before Moore's committee.
------------
"Berkshire Medical Center, 5 others will file lawsuit: The hospitals allege the state Executive Office of Health and Human Services violated Medicaid paybacks."
Berkshire Eagle Staff, December 1, 2009
PITTSFIELD -- Berkshire Medical Center will join five other Massachusetts hospitals in filing a lawsuit in Boston today that alleges the state Executive Office of Health and Human Services (EOHHS) has violated state statutes regarding Medicaid reimbursements, BMC spokesman Michael Leary said.
The five other hospitals are Holyoke Medical Center, Quincy Medical Center, Merrimack Valley Hospital, Cape Cod Hospital, and Signature Healthcare Brockton Hospital. The suit will be filed in Suffolk Superior Court, Leary said.
BMC's parent company, Berkshire Health Systems, is Berkshire County's largest employer with some 3,000 employees.
All six hospitals are known as "disproportionate share hospitals" because at least 63 percent of their patients are covered by public health insurance. The figure at BMC is 72.5 percent, Leary said.
"By state law, the state is required to reimburse hospitals equal to the cost of Medicaid appointments, and they are not doing that," Leary said.
State law requires that for disproportionate-share hospitals, the state must establish rates that equal a DSH's financial requirements.
According to the complaint, the state has based reimbursement primarily on a statewide average cost of care for all hospitals, even though the dominance of Medicaid as a payer, and the resource intensiveness of the patient population served, varies greatly among hospitals across Massachusetts.
Medicaid's reimbursement rate is between 40 and 86 percent of each hospital's costs over the past six years, according to the complaint.
EOHHS spokeswoman Jennifer Kritz said in a statement that the agency "is confident that the state's actions comply with all applicable laws and will be upheld."
BMC is participating in the lawsuit because it wants to receive additional reimbursement funding on the state level if it becomes available, Leary said.
The amount of damages sought by the six hospitals could not be obtained Monday. But Leary said state cuts to Medicaid and the decision to cap hospital costs in lieu of state budget cuts last December have resulted in a three-year shortfall of more than $70 million at all six hospitals.
BMC's share of the funding shortfall is $4.8 million. Berkshire Health Systems has shed the equivalent of 130 full-time positions this year in two workforce reductions -- one in July and one in September. Leary said the funding shortfall was partly responsible for the job cuts.
Dramatic shortfalls in state revenue in 2008-2009 required Gov. Deval L. Patrick to make emergency cuts in state payments for health care services, which included the elimination of $3 million in payments to BMC.
BMC receives about 256,000 patient visits a year, a total that includes 48,237 emergency room visits, according to the hospital.
"The hospitals are unable to recoup these staggering losses from the small percentage of privately insured patients that they serve," according to the complaint.
Kritz said the EOHHS recognizes the important role that the six hospitals play in the health care system and that it will continue to work with them.
On Nov. 1, EOHSS increased state payments to disproportionate share hospitals by 10 percent to $18 million.
-
To reach Tony Dobrowolski: TDobrowolski@berkshireeagle.com (413) 496-6224.
-
www.topix.net/forum/source/berkshire-eagle/T52LN70FU78I7MFQ9
-
------------
"Spending on the insured rises: Outpatient care at expensive Massachusetts hospitals fuels hike"
By Liz Kowalczyk, Boston Globe Staff, February 13, 2010
In just three years, medical spending on privately insured Massachusetts residents grew more than 15 percent, fueled in large part by outpatient care in expensive hospitals, according to three reports released yesterday examining the state’s climbing health care costs.
The findings by Massachusetts regulators bolster Governor Deval Patrick’s proposal this week to give the state the power to cap health care price increases. The reports also provide a preview of state hearings scheduled to begin March 16, investigating why medical costs here are so high compared with the United States as a whole - and to propose solutions.
The data suggest that care is being provided in increasingly expensive places. Outpatient care in Massachusetts - which includes day surgery, imaging tests, and procedures like colonoscopies - is almost entirely provided at hospitals, and most of the rise in outpatient hospital spending was for care provided in teaching hospitals in the Boston area, one of the reports concludes.
Outpatient spending at hospitals grew 26 percent from 2006 to 2008, from $2.4 billion to $3.1 billion, regulators found. This increase was driven by hospitals both charging higher prices and doing more procedures.
In addition, hospital admissions are shifting toward higher-cost providers, with the teaching hospitals’ portion of total overnight admissions of privately insured patients increasing by 5 percentage points over the three years.
Dr. JudyAnn Bigby, Patrick’s secretary of health and human services, said that while state officials knew Massachusetts spending on health care is 15 percent higher than the national average, she was surprised that “we see a lot of increased consumption of medical care in outpatient hospital departments. That is different from what I’d been hearing from hospitals, saying that these services have been leaving them and going to freestanding outpatient facilities competing with them.’’
Spending on outpatient care in nonhospital facilities, such as surgery clinics and rehabilitation centers, dropped 14 percent from 2006 to 2008.
State regulators also examined insurance premiums and the impact of growing medical costs on businesses, concluding that average monthly premiums grew 12.2 percent from 2006 to 2008.
Premiums paid by small businesses, however, grew fastest, when adjusted for differences in benefits, demographics, and location. From 2007 to 2008, adjusted small group premiums grew 5.8 percent, while midsize groups’ rates grew 4.8 percent, and large groups’ grew 5.4 percent.
Patrick’s legislation filed on Wednesday - which would give the insurance commissioner sweeping authority to review and reject rates charged by hospitals, physician groups, medical imaging centers, and insurers - was particularly intended to help small businesses.
The Massachusetts Hospital Association said in a statement that the reports fail to address the role inadequate government payments for Medicaid and Medicare patients play in pushing up health care costs.
Hospitals are forced to make up for these poor payments by charging private insurers more, the group has said.
“It is important to remember that just as there is no single ‘silver bullet’ to conquer costs, neither is there one member of the healthcare community that is single-handedly responsible for causing costs to increase,’’ the association said.
Health insurers applauded the reports’ conclusions. “This is what we’ve been saying all along, that the prices providers charge, [hospital] market power, the expansion of academic medical centers into the suburbs, these are driving the cost increases in Massachusetts,’’ said Lora Pellegrini, acting president of the Massachusetts Association of Health Plans. “These reports focus squarely on the issues policy makers need to be dealing with.’’
-
Liz Kowalczyk can be reached at kowalczyk@globe.com.
-
------------
"Cost of health care, not a lack of competition, driving up costs of coverage, Massachusetts insurers maintain"
By Jim Kinney, The Republican, March 08, 2010
SPRINGFIELD – Local health insurers said the cost of care, not a lack of competition among insurers or a thirst for profits, is driving up the cost of health care coverage.
“It’s higher than last year because medical costs have gone up since last year,” said Peter F. Straley, president and CEO of Springfield-based Health New England.
Straley said Health New England, which insures 114,000 people at 5,000 employers in the four counties of Western Massachusetts, raised its rates about 15 percent compared with last year. he said that will be about the average rate increase for any plan in Massachusetts
He said it’s not just that doctor visits, medicines, procedures and tests cost more, it is that there are more of them going on.
“We as individuals are using more, we getting more prescriptions filled, we’re getting more lab tests, more MRIs,” Straley said.
On Monday, President Barack H. Obama pushed for his health care reforms at an event near Philadelphia by drawing attention to analysis from the Goldman Sachs investment bank that health insurance companies face little price pressure and too little competition.
U.S. Secretary of Health and Human Services Kathleen Sebelius said the insurers knew that raising rates would cost them customers, but were content to make more money from fewer customers being charged a higher rate.
“In the meantime, the insurance numbers just don’t match up with medical trend,” Sebelius said in a conference call with reporters from around the country after appearing with the president. Sebelius called for health-care plans to post financial information including profit margin and executive salaries on their Web sites.
Straley said the Goldman Sachs analyst couldn’t have been speaking of the insurance market in Massachusetts.
He said most of Health New England’s business is with employers of fewer than 50 employees which have been hit hardest by rate increases over the years. Under state law, all the health plans have to submit bids when a group of 50 or fewer employees is looking for insurance.
“That’s really the key thing here because everyone is focus on small business,” Straley said.
Health New England is the smallest health insurer in the state. The largest plan, Blue Cross Blue Shield of Massachusetts, referred calls on the subject to Eric Linzer, senior vice president of the Massachusetts Association of Health Plans.
“We’ve got close to a dozen different health insurers operating in the state,” Linzer said. “We have plenty of competition in Massachusetts.”
But a recent report from the Massachusetts attorney general’s office said there is too little competition among health care providers and physicians groups, especially in eastern Massachusetts, Linzer said.
Linzer said the health insurance market in Massachusetts is dominated by not-for-profit organizations, like Blue Cross Blue Shield of Massachusetts.
Straley said Health New England is a for-profit company owned by a not-for-profit, Baystate Health. It has a profit margin of 0.9 percent, he said.
------------
Massachusetts Health Reform
"Owners hit with millions in fines: Penalties are levied against businesses for failing to provide employees with insurance."
Associated Press via The Berkshire Eagle (online), March 20, 2010
BOSTON -- Massachusetts has fined more than a thousand companies over $18 million for failing to offer medical insurance to their workers -- a precursor of what some business owners fear could happen on a national scale if President Obama signs a sweeping health care overhaul.
The fines are for violating a provision in Massachusetts' landmark 2006 health care law that requires larger companies to offer insurance or pay an annual fine of $295 per full-time employee.
In 2008, 807 of 23,128 eligible Massachusetts firms were found liable for the fine, known under the law as the "fare share contribution." They were on the hook for a total of $8.6 million, or an average of $10,663 per employer. In 2007, 1,045 firms were found liable for $10.5 million, or an average of $10,047 each. Statistics for 2009 were not yet available.
The Massachusetts law has been used as a blueprint for a national health care bill heading to a critical vote in the U.S. House on Sunday, and it could foreshadow how national health care reform plays out across the country.
Like the Massachusetts law, the federal legislation includes penalties for businesses that don't comply. While the federal bill would not require coverage as Massachusetts does, it hits employers with a $2,000-per-employee fee if the government subsidizes their workers' coverage.
The House bill would exempt companies with fewer than 50 employees, compared to the tighter threshold of companies with 11 or fewer workers under the Massachusetts law. The bill would also offer tax credits to help small employers provide coverage.
In Massachusetts, the law saw an uptick in the number of employers offering insurance, from 70 percent in 2005, the year before the law was passed, to 76 percent in 2009, according to the state's Division of Health Care Finance and Policy.
Overall, the state has added more than 400,000 people to the ranks of the insured since the law took effect, bringing the total number of insured residents to more than 97 percent.
That increase bucked a national trend.
In 2001, 69 percent of Massachusetts companies offered coverage, compared to 68 percent of companies nationally. By 2007, the percentage of companies offering insurance nationally had slipped to 60, compared to Massachusetts' 72 percent.
Massachusetts business groups have been split on the merits of the state's health care law.
Rick Lord, president of the Associated Industries of Massachusetts, said that since 2006, more than 100,000 workers have signed up for insurance through their employers to comply with law's "individual mandate" requiring nearly everyone have insurance or face tax penalties.
"I haven't been hearing complaints (from companies), just an acknowledgment that the percentage of their workers taking insurance is increasing," said Lord, who also sits on the Commonwealth Health Insurance connector Authority Board, which oversees the health care law.
Other business leaders in Massachusetts are chafing under the added state regulations of the 2006 law.
Bill Vernon, state director for the National Federation of Independent Business, said the pressure to offer insurance is a "job inhibitor" at a time when the state has seen its unemployment numbers climb.
"It makes it very difficult to create a job in this state. It makes it very difficult to retain the employees you have now given the cost of insurance," he said.
-
www.topix.net/forum/source/berkshire-eagle/TGS5E69Q3OMSHAK0V
-
------------
Massachusetts
"State's health law may need tweaking"
Associated Press, March 23, 2010
BOSTON -- Massachusetts is facing a host of perplexing questions as it looks to mesh its landmark 2006 health care law with the sweeping health overhaul approved by the U.S. House.
One of the thorniest questions focuses on the so-called "individual mandate" -- the tax penalties levied on those who refuse to obtain health insurance.
Massachusetts is the only state with an individual mandate. In 2009, those who failed to get insurance even though the state deemed they could afford coverage faced an annual penalty of nearly $1,100.
Under the federal bill, which President Barack Obama plans to sign on Tuesday, those who don't get insurance will begin facing federal tax penalties in 2014, with individuals having to pay fines reaching $750 by 2017.
What's unclear is whether Massachusetts residents without insurance would face both a federal and state penalty.
State officials said Massachusetts could either ask for an exemption from the federal mandate or adjust its own fines so uninsured residents wouldn't be hit twice.
"There is a provision that would allow states to apply for waivers," said Massachusetts Health and Human Services Secretary Dr. JudyAnn Bigby. "We have a very strong case for making a point that we have some of these policies in place related to the individual responsibility (mandate)."
Bigby also said that the bill gives the federal secretary of health and human services leeway in drafting regulations to match the intent of the legislation -- leeway that could take into account Massachusetts' early role in establishing an individual mandate.
The individual mandate isn't the only element of the federal legislation that clashes with state law.
Under the Massachusetts law, businesses with 11 or more workers who fail to offer insurance to their workers face an annual fine of $295 per full-time employee.
Although the federal legislation doesn't require businesses to offer coverage, it hits employers with a $2,000-per-employee fee if the government subsidizes their workers' coverage. Companies with fewer than 50 full time employees would be exempt under the federal bill.
Another area of potential conflict between the state law and federal bill is on the creation of state-based "exchanges" beginning in 2014 that would allow individuals to pool their resources to gain the same kind of health care purchasing power of big companies.
Under the 2006 law, Massachusetts created its own health care exchange -- known as the Health Care Connector -- that oversees the law, setting regulations and helping connect individuals with lower cost private health plans.
Jon Kingsdale, executive director of the Commonwealth Health Insurance Connector Authority, said the federal bill also allows for regional exchanges, meaning that smaller states like Rhode Island have the option of creating their own exchange or joining with Massachusetts.
Many of the conflicts between the state law and the federal bill were inevitable given that the Massachusetts law provided the blueprint for the legislation, leading to many overlapping policies, according to Kingsdale.
"There's a bunch of decisions to be made," he said. "The devil is in the details and a lot of those details aren't clear."
But Kingsdale also said there is plenty of time for any wrinkles to be ironed out, particularly given that many of the elements of the federal legislation don't kick in for a few years.
There are other parts of the federal bill that will be a clear boon to Massachusetts.
Under the bill, the state is scheduled to receive an additional $2 billion in Medicaid assistance between 2014 to 2020 to expand coverage for lower income residents.
The federal legislation also expands the pool of people eligible for subsidized care.
Under the state law, individuals making up to three times the federal poverty level, or about $32,500 a year, are eligible for subsidized care. The federal bill expands that to 400 percent, or $43,320 for an individual.
The federal law also includes coverage for legal immigrants. Massachusetts lawmakers last year voted to deny coverage to legal immigrants in an effort to save $130 million as the state struggled to close a budget gap.
Bigby said she's confident that after all the kinks are worked out, Massachusetts will end up being rewarded rather than punished for being at the vanguard of overhauling health care.
"There is recognition that some states are already doing some of these things and they should be allowed to build on pieces of the federal reform that already exist in their state," she said.
-
www.topix.net/forum/source/berkshire-eagle/TNJ0DGOHFED52O245
-
------------
"Mitt Romney gets it right"
By Joan Vennochi, Boston Globe Columnist, April 1, 2010
MITT ROMNEY’S latest position on the Massachusetts health care reform law is, finally, an honest one. “Overall, ours is a model that works,’’ the former Bay State governor and would-be presidential candidate said in Iowa.
But, as Romney also notes, it’s a work in progress and needs fiscal fine-tuning.
That’s different from demonizing it.
Tim Cahill, the Massachusetts state treasurer who is running for governor as an independent, made national headlines by proclaiming that health reform is bankrupting the state. This mantra was happily picked up by opponents of the recently enacted federal health care reform law, which used Massachusetts as a template.
Asked to respond to Cahill’s dire conclusion, Romney, via spokesman Eric Fehrnstrom, replied, “It is irresponsible to say it is bankrupting the state, as Tim Cahill claims.’’
Romney, who has been for health care reform and against it, now appears to be for it, at least in its Massachusetts incarnation. There’s still a lot of contorting going on, as he embraces states’ rights and tries to finesse the controversial issue with his Republican base.
But at least he is also celebrating the core goal of universal health care — getting insurance coverage to virtually all Massachusetts citizens — which he helped the Bay State achieve. As he does, he points out a legitimate challenge: how to make sure it remains economically viable.
“I don’t pretend for a minute that our system is perfect,’’ he said recently. “I think it’s better than what we had, and I think people can learn from what we have done and I think there are changes I would make to it.’’
Cahill, meanwhile, is doing his best to reduce the complicated subject of soaring health care costs to to a simple soundbite — universal health care costs too much.
“He’s got a political shorthand which says health care reform is causing the state to go bankrupt. It isn’t,’’ counters Tim Murphy, who was secretary of health and human services for Massachusetts during the Romney administration. But it could deplete resources.
A year ago, the Massachusetts Taxpayers Foundation produced a report that is considered the bible on Massachusetts health care costs. In the first four years since the law was enacted, the report concluded that state budget spending on health reform grew from a base of $1.041 billion in fiscal 2006 to a projected $1.748 billion in fiscal 2010. “That is an increase of $707 million, half of which is supported by federal reimbursements. The $353 million state share translates into an average yearly increase of only $88 million,’’ the report stated.
It doesn’t take a math whiz to wonder what happens if federal reimbursements disappear and conclude that Massachusetts shouldn’t ignore the upward trend of longterm health costs.
Everyone — liberals, conservatives, politicians, health insurers, and providers — agree to that in principle. The problem is how to get there in practice. Asked how he would do it, Cahill said he wasn’t sure.
In a recent article for Politico.com, Murphy, who is now president and CEO of Beacon Health Strategies, laid out several areas that he said need to be addressed. Translated from wonk-speak into English, they encompass tough political decisions.
The first involves reversing what Murphy calls the “Kumbaya’’ approach of the Connector Authority, which links the uninsured with private health plans. Coverage, he wrote, should be pared down from “a series of expensive, government-decided, pre-paid benefits’’ to a basic plan that provides protection from “financial calamity during a serious health crisis.’’ Massachusetts, he wrote, also needs to reduce “the number of coverage requirements, for everything from in-vitro fertilization to chiropractic care.’’
He also argues that the state must stop paying hospitals for so-called “free care’’ and direct more limited funding “to only financially distressed and essential providers.’’ That could save as much as $400 million annually.
Massachusetts got to universal health care because Romney worked with the Democrats who control the Legislature. Those Democrats ultimately stripped out Romney’s cost containment propositions. If they don’t have the political will to do what it takes to bring down costs, Romney will be proven right. And, someday, so will Cahill.
-
Joan Vennochi can be reached at vennochi@globe.com.
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2010/04/01/fine_tuning_health_care_costs/?comments=all#readerComm
-
------------
"Health insurers stop writing policies for some"
By Robert Weisman, Boston Globe Staff, April 6, 2010
Most Massachusetts health insurers have temporarily halted writing new policies for individuals and small businesses through a state-sponsored broker, according to a notice posted today on the website of the Massachusetts Health Connector.
The agency, which was set up after the state passed its universal health care law in 2006, acts as a marketing channel to connect formerly uninsured residents with plans offered by nonprofit carriers that sell insurance through a program called Commonwealth Choice. The plans are part of the so-called small group market, and pool individual and small business policies.
Citing last week's decision by the state Division of Insurance to reject most new health premium increases proposed by the insurance companies for April 1 in the small group market, the Connector site today said "insurers must pull their Commonwealth Choice plans until they reset the rates. We expect new rates soon."
Insurers and state officials didn't immediately return phone calls seeking comment this afternoon.
As of now, rates set in 2009 remain in effect for existing policies under last week's decision by the insurance division.
Six insurers yesterday filed suit in state Superior Court asking a judge to invalidate the state's rejection of rates and allow them go forward with premium increases averaging 8 to 32 percent. A judge on Thursday is expected to hear their request for a preliminary injunction.
This afternoon, the only insurance plan being quoted on the Health Connector site was offered by CeltiCare Health Plan, a Boston-based managed care organization.
------------
"Head of Massachusetts Health Connector Resigns"
By SACHA PFEIFFER, wbur.org - April 15, 2010
BOSTON — Jon Kingsdale, head of the Commonwealth Health Insurance Connector Authority, is stepping down. He has led the agency since it was created by the state’s 2006 landmark health care reform law to help uninsured residents sign up for coverage.
In Kingsdale’s four years on the job, the state has gotten more than 97 percent of its residents insured. His next task would have been to integrate Massachusetts health reform with the new national health care reform law.
Kingsdale said he concluded that a new executive director would have the fresh eyes — and could make the years-long commitment — needed to do that.
“I decided this was the right time to kind of step off the cliff and see where I landed, see if I can’t combine my two passions — to build something from scratch and to implement national reform,” he said.
Kingsdale said he doesn’t have a new job lined up yet. But he said he wouldn’t rule out working on health reform for the Obama administration if the opportunity comes up.
“I can’t tell you it’s an impossibility,” he added, referring to the likelihood that he might work on reform at the national level, “but there’s absolutely nothing in the works.”
Kingsdale’s last day on the job will be June 4.
Gov. Deval Patrick immediately announced Kingsdale’s successor: Glen Shor, assistant secretary for health care policy at the state’s Executive Office for Administration and Finance. In that role, he has been a key point person for Patrick in implementing state health reform.
In a letter to the Connector board Wednesday, Kingsdale wrote that he will leave the agency “with a mixture of pride in our achievements and sorrow at saying goodbye to a truly exceptional team…They are my good friends now as well, and I will truly miss working with them.”
In February, the Connector’s chief financial officer, Patrick Holland, also announced his departure.
------------
-

-
(George Rizer/Globe Staff)
-
A BOSTON GLOBE EDITORIAL
"Kingsdale: Health reform in action"
April 19, 2010
Once Congress passed a national health reform law that followed the Massachusetts plan, the state was almost sure to lose Jon Kingsdale’s services. The former insurance executive is the first head of the agency overseeing reform here, and he makes no bones about his interest in bringing what he has learned to the national stage, whether for government, the private sector, or a non-profit.
During his four years as head of the Connector Authority, the state agency managed to balance the interests of employers, insurers, medical providers, and the public, while reducing the number of uninsured to fewer than 3 percent. Its website exchange of insurers’ offerings will be a model for many other states. The Connector helped persuade most of the state’s young invincibles to buy insurance, in part by enlisting a valuable ally — the Boston Red Sox. Not everything that works in Massachusetts is transferable to the national level, of course, but the task of putting a complex law into action takes expertise that few other than Kingsdale possess.
The health care problem that Massachusetts has come nowhere near to solving is cost. Kingsdale offers no panacea, but has enough experience to know what doesn’t work — and what just might.
-
www.boston.com/bostonglobe/editorial_opinion/editorials/articles/2010/04/19/kingsdale_health_reform_in_action/?comments=all#readerComm
-
------------
JON KINGSDALE
"Lessons from the health care rollout"
By Jon Kingsdale, Boston Globe, Op-Ed, May 3, 2010
IMPLEMENTING NATIONAL health care reform could pose the greatest domestic policy challenge since executing the Civil Rights Acts of the 1960s.
National health insurance has been a long time coming — nearly a century. This past year of highly partisan health care debates has exhausted Congress and the nation.
Now what?
A whole lot of work, of course — hundreds of new, complex federal regulations to be drafted, lobbied, and revised; nearly 50 state exchanges to be set up; and explaining the many complexities of new insurance options and requirements to millions of employers and hundreds of millions of citizens anxious to know how they are affected.
All this in the face of heated resistance from many angry Americans and nearly the entire Republican Party. Efforts to outlaw the “individual mandate’’ are now proceeding in dozens of states, cast in the emotional rhetoric of personal freedom and states’ rights.
Most Americans are still confused about this reform. As with last summer’s debate about “death panels,’’ fears are easily stirred. Like politics, all medicine is local and personal. Implementing reform across this diverse country will require sensitivity to local realities. It also depends on the cooperation and varied capabilities of 50 state governments. The law will take nearly four years to put into effect and years more to assess, adjust, and evaluate.
All the while, public support must be built and sustained. While not freighted with the emotions of civil rights, the arcane technicalities of health financing are far more impenetrable than the moral imperatives of racial equality. And the level of trust in government has never been lower.
Even liberal Massachusetts saw its first effort at universal coverage, enacted in 1987, stymied and then repealed. Massachusetts implemented a very different approach in 2006. Proponents and opponents of national reform have assessed our model, ad nauseam, as a proxy in the national debate.
Four years after enactment, Massachusetts has learned about the challenges of implementing near-universal coverage. Here are a few lessons:
1. It’s a campaign: In any successful campaign, continuous progress must be demonstrated and broadly communicated. In Massachusetts, we built partnerships with private and public groups, so that people heard and read about the law everywhere — at Fenway Park, in church, while shopping, or riding the subway. We launched this effort with the Red Sox, and held more than 300 educational forums across the state, the equivalent on a national scale of 15,000 outreach meetings. As a result, voter support for reform has remained high, ranging from 59 percent to 75 percent.
2. Adequate resources: The Massachusetts Legislature appropriately funded implementation with $35 million in the first year; the equivalent on a national scale would be $1.65 billion. Never were shortages of time, expertise, or resources allowed to stand in the way of meeting legislated deadlines.
3. Coordination: Somebody has to be on point to drive implementation across federal agencies and the other organizations needed to execute this undertaking. The Health Connector used multiple consultants and outsourcing strategies, while staffing up, to meet deadlines. With 50 states and far broader legislation, the federal effort will require a Herculean coordination effort.
4. Experiment and evaluate: This effort is new and not everything will go as planned. For example, running an exchange means offering customers what they want to buy, but that’s neither obvious nor unchanging. Massachusetts’ exchange is a learning organization. Key initiatives were launched as pilots, and we have not been afraid to revise them and try again.
5. Transparency: The biggest challenge Washington faces in “helping’’ Americans gain access to care is their distrust of government. Transparency is the antidote: making tough decisions in public; meeting endlessly with employers, unions, insurers, clinicians, and citizens; and both talking and listening out there, in at least 15,000 communities. These are essential to building trust.
6. Harness the market: State exchanges are essentially stores that sell insurance, combining government’s responsibility to protect consumers with a retailer’s need to serve customers. Brow-beating various industries may be good partisan politics, but the Health Connector has worked diligently at creating solid, long-term working relationships.
The Red Sox lent our campaign a reservoir of nonpartisan good will. The campaign worked: more than 97 percent of Massachusetts residents are insured, the individual mandate has been accepted, and bipartisan support remains strong.
Congress and the president have labored mightily to bring forth national reform, modeled after Massachusetts. Now the executive branch has 3 1/2 years to work with 50 very different states in bolstering popular support and executing effectively. That will require massive amounts of technical expertise and project management, combined with public outreach and creative communications.
The real campaign has just begun.
-
Jon Kingsdale is executive director of the Massachusetts Health Connector.
-
www.boston.com/bostonglobe/editorial_opinion/oped/articles/2010/05/03/lessons_from_the_health_care_rollout/?comments=all#readerComm
-
------------
"In the State"
The Berkshire Eagle, December 31, 2010
"Health care mandate penalties to increase"
Massachusetts residents who can afford health insurance but fail to buy it face steeper penalties in 2011.
A key element of the state's landmark 2006 health care law requires virtually all residents to have insurance. Those who remain uninsured face tax penalties if they are deemed able to afford coverage.
Starting in January anyone aged 27 and older who makes more than three times the federal poverty level -- about $32,500 annually -- faces penalties of $101 a month or $1,212 for the entire year. That's up from $93 a month or $1,116 annually in 2010.
Those aged 18-26 who also earn more than $35,000 annually face penalties of $72 per month or $864 annually, up from $66 a month or $792 annually in 2010.
There are no changes for those making less than three times the poverty level.
------------
"Medicaid cost crisis looms for Bay State: Budget is pushed to brink as more enroll in program"
By Michael Levenson, Boston Globe Staff, January 3, 2011
The money, it seems, is never enough.
Governor Deval Patrick approved a record $9.6 billion last July for the state’s health insurance program for the poor — sufficient, he assumed, to last a year. But the program’s costs quickly outpaced expectations, forcing the governor to approve an additional $329 million in October and then seek $258 million more, which lawmakers approved last week.
And even that may not last, with six months remaining in the budget year.
The ballooning cost of Medicaid is one of the biggest challenges facing Massachusetts and other states, which have seen demand for the program jump during the recession as increasing numbers of unemployed residents enroll in the subsidized insurance plan.
With Massachusetts confronting an estimated $1.5 billion shortfall in the coming budget year, Patrick has said he is committed to financing the program, known as MassHealth. But he has acknowledged that it cannot continue to grow at this rate.
“Containing growth in our health care costs, particularly MassHealth, is something we absolutely need to do, because it is unsustainable at the rate that it’s been growing,’’ said Jay Gonzalez, Patrick’s budget chief.
The choices confronting the governor, however, are hard.
Massachusetts last summer slashed dental benefits for MassHealth recipients, forcing hundreds of thousands of poor, elderly, and disabled residents to visit community health centers, instead of their regular dentists, for fillings, root canals, dentures, and other routine procedures. Bigger cuts or restrictions loom.
Arizona recently made national headlines when it stopped financing certain organ transplant operations under its Medicaid program. Wisconsin stopped paying for caesarean sections unless they were deemed medically necessary. In Texas, Governor Rick Perry has entertained the idea of abolishing the state’s Medicaid program entirely.
Patrick, who is set to unveil his latest budget plan later this month, has not said what steps he will take to control Medicaid costs, but further cuts are all but certain.
“We need to do some things differently,’’ Gonzalez said, declining to elaborate. “There are going to be some hard decisions.’’
MassHealth is open to a range of people who meet certain criteria, including some individuals 65 and over, disabled residents, and those with low or moderate income — generally defined as earnings below 133 percent of the federal poverty level, or less than about $29,327 a year for a family of four.
Qualifying for Medicaid is easier in Massachusetts than it is in two-thirds of other states, said Brian Rosman, research director of Health Care For All, an advocacy organization.
Massachusetts, even though it has approved an additional $587 million in Medicaid spending this budget year, will be on the hook for only $223 million, because the federal government pays for part of the program.
Even so, Medicaid is putting unprecedented pressure on state finances.
Health care spending, most of which is for Medicaid, now accounts for 37 percent of the state budget, up from 21 percent in 2000, according to the Massachusetts Taxpayers Foundation. In the last three years, as the state cut services and weathered a historic economic downturn, Medicaid costs grew by $2 billion, according to the foundation, a business-backed budget watchdog group.
One reason is clear: As the slow economy was sapping the state of revenue, layoffs and wage cuts were forcing more people onto Medicaid. As of September, about 1.3 million residents were enrolled in MassHealth, an increase of 24 percent since 2006, according to state officials. The figure includes 107,000 residents identified as “long-term unemployed,’’ a number that has nearly doubled since 2006.
“Medicaid has been a so-called budget-buster for 25 years,’’ said Michael J. Widmer, president of the taxpayers foundation. “There’s no easy fix for Massachusetts or any other state. But its relentless growth is forcing cuts in other state programs. So it’s a longtime problem, but it’s reached the breaking point.’’
During his reelection campaign, Patrick said controlling health care costs would be his top priority in his second term. House Speaker Robert A. DeLeo and Senate President Therese Murray have also embraced the goal. But such talk is common on Beacon Hill.
“It’s been talked about for several years now and kicked around . . . but we’re getting to the point where the rubber meets the road,’’ said Charles A. Murphy, chairman of the House Ways and Means Committee. “If we continue on the same track, it’s a recipe for disaster.’’
The state is also being pushed by Washington, which is cutting back its support. The federal government, which had been paying 62 percent of the state’s Medicaid costs as part of the stimulus program, will pay only 50 percent when the program ends this July.
Richard T. Moore, Senate chairman of the Legislature’s Committee on Health Care Financing, said the state may have to respond by tightening eligibility requirements for Medicaid, or further slashing benefits.
“We really have to be looking at what we can do to rein in costs, and it may mean some curtailment of health care services that may not be critically needed,’’ said Moore, an Uxbridge Democrat.
“It’s not just the cost of the program’’ that is to blame, he said. “It’s the cost of health care’’ overall.
Harriett L. Stanley, House chairwoman of the committee, said if the state is serious about controlling Medicaid costs, it will require standing up to advocates for the poor, elderly, and disabled, who have long opposed attempts to cut benefits or move recipients into managed care.
“We now have to begin messing with Medicaid,’’ said Stanley, a West Newbury Democrat. “Everybody says it, but no one is willing to be the bad guy and do something about it.’’
-
Michael Levenson can be reached at mlevenson@globe.com.
-
------------
"Patrick should approve waiver"
The North Adams Transcript, Letters, February 22, 2011
To the Editor:
We are gratified by the Patrick administration and the Massachusetts congressional delegation’s recent success in obtaining significant financial relief for Massachusetts hospitals as part of the recently approved Medicaid waiver.
We are dismayed, however, to learn of the administration’s recent determination to use the funding for only six hospitals in the state, to the exclusion of others, including North Adams Regional Hospital, which rely on this support to cover services for low-income patients. The impact of this funding to NARH is $262,000.
The Center for Medicare and Medicaid Services approved payments to Massachusetts hospitals up to $270 million -- $230 million was appropriately prioritized for the six hospitals with the highest Medicaid volume; however, the waiver proposal specified that $40 million was to be dedicated to all other private acute-care hospitals, including NARH. This does not require use of additional state general funds, but is already included in the approved waiver financing.
NARH, like all hospitals providing care to MassHealth patients, has experienced significant reductions in Medicaid reimbursement. This federal waiver offers some badly needed relief.
We urge the Patrick administration to allocate the full amount approved in the Medicaid waiver to enable NARH to continue to serve the low-income members of our community.
Richard T. Palmisano
North Adams, Massachusetts
February 21, 2011
The writer is president and CEO of Northern Berkshire Healthcare, parent company of North Adams Regional Hospital.
------------
"Mass. Medicaid waiver approved through June 2014"
By Chelsea Conaboy, Boston Globe Staff, 12/20/2011
The federal government today approved a plan that extends Medicaid funding for the state’s innovative health insurance law through mid-2014 and shifts the way hospitals that treat a large portion of poor patients are paid for their care.
The Centers for Medicare & Medicaid Services sent a letter to Dr. JudyAnn Bigby , the state Health and Human Services secretary, saying it would extend the state’s so-called Medicaid waiver through June 2014.
The waiver is key to funding the 2006 health care law that provides subsidized insurance plans for low-income people and requires most state residents to have health insurance. It expired in June and federal officials have been issuing incremental extensions as they negotiated with the state.
The $26.75-billion deal, the result of a year and a half of negotiations, includes $120 million in new federal funding to change the way safety-net hospitals are paid, moving them toward a system in which they are given a set budget to treat Medicaid patients. Hospitals eligible for the program are Boston Medical Center, Cambridge Health Alliance, Brockton Hospital, Lawrence General Hospital, Holyoke Medical Center, and Mercy Medical Center in Springfield.
The hospitals were receptive to the idea, Bigby said. “We worked with them to develop the strategy, to get them to agree to the transformation that they have to make,” she said.
Last year, Boston Medical Center received about $90 million as a supplemental payment for treating a large portion of the state’s Medicaid patients. In the coming year, under the waiver, the hospital will be eligible to receive up to $103 million and must meet quality and cost benchmarks to get all of that money, said chief executive Kate Walsh.
The new system will help to stabilize the hospital’s finances and improve patient care, she said. “It provides support and financial resources to begin the transformation so that we’re ready for whatever health care reform brings,” she said.
Hospitals such as BMC that care for many poor patients say they have suffered under the 2006 law because state aid they received for treating the uninsured was diverted to pay for insurance subsidies. And they say the number of newly insured patients they now see has not made up for the lost revenue.
News of the waiver approval came a day after federal officials announced that five Massachusetts systems, including Partners HealthCare and Steward Health Care System, have agreed to be paid on a budget system for the management of elderly and disabled patients on Medicare, starting Jan. 1.
Governor Deval Patrick has proposed legislation that would move more hospitals and doctors to such a system, known generally as global payments. Currently, most are paid a separate fee for each treatment, test, and visit -- a system that has been blamed for driving up costs because it creates incentives for unnecessary care.
Brian Rosman, research director for the consumer group Health Care for All, said the waiver “reflects the shared principles of both the Obama administration and the Patrick Administration to use Medicaid to remake our (health care) delivery system.”
More than 1.3 million people in Massachusetts have some form of Medicaid coverage. Rosman said the waiver “will be good for both the Medicaid recipients and for the state.”
Bigby said the initiative to restructure payment systems was one reason that negotiations dragged on. The other was a new plan to cover early intervention services for some children with autism.
The state also will launch a pilot program to give providers a “bundled” payment for the work they do with low-income children with high-risk asthma, which would provide money for health workers to visit the children’s homes.
“By allowing providers some flexibility about the type of care they’re providing to the kids, we can do a better job of controlling their asthma and they will stay out of the hospital,” Bigby said.
The new agreement also streamlines enrollment for children. It allows the state to use income information in the state food stamp program to calculate eligibility for Medicaid coverage rather than requiring annual re-enrollment. That change is meant to improve continuity for families and reduce administrative costs for the state, Bigby said.
The waiver represents “a strong step forward” for the state’s health system, Cindy Mann, deputy administrator of the Centers for Medicare & Medicaid Services, said in an e-mail.
“The demonstration will support the Commonwealth’s delivery and payment reforms while also helping it to move forward on several innovative new programs,” she said.
Chelsea Conaboy can be reached at cconaboy@boston.com. Follow her on Twitter @cconaboy.
------------
"Massachusetts Takes On Health Costs"
The New York Times, Editorial, August 4, 2012
Give Massachusetts credit for setting audacious health care goals. It took the lead in guaranteeing near-universal health insurance coverage for its residents, providing a template for the federal reforms to follow.
Now a bill passed last week by the Legislature — and enthusiastically endorsed by Gov. Deval Patrick — aims to tackle the much harder problem of controlling health care costs. Massachusetts will be the first state to try to cap overall health care spending, both private and public, so that it will grow no faster than the state economy.
The state was able to reach near-universal coverage because the vast majority of its population was already covered by some form of insurance. It also could subsidize coverage for the uninsured using a big pool of money that had been used for charity care.
But when it comes to controlling health care costs, Massachusetts has no advantage, and in fact is starting behind most other states. Its costs are among the highest in the nation, and they have been growing in recent years at 6 percent to 7 percent while the economy has been growing at less than 4 percent. That bleak picture may be changing. The growth rate of health costs has slowed significantly over the past year or two, but nobody knows if this is a temporary or lasting change.
The new legislation sets a very ambitious target: to hold the annual increase in total health care spending to the rate of growth of the state’s gross domestic product for the first five years, through 2017, and then even lower for the next five years, to half a percentage point below the economy’s growth rate. The savings are projected to be as high as $200 billion over a 15-year period.
Setting goals is a necessary step, but there is skepticism among health care analysts that these targets could be met in such a short time given the lack of a strong enforcement mechanism in the legislation.
That does not mean the bill is completely toothless. It will establish a commission to monitor the growth in spending and require that health care providers or insurers explain themselves if their costs rise above the target growth rate. If there is no valid reason, the commission can demand that an organization submit a plan to bring its spending back in line. As a last resort, the commission can impose a $500,000 fine if it finds that the organization failed to make a good-faith effort. Many analysts expect the state will have to become increasingly aggressive in demanding cost cutting by providers and insurers if savings do not materialize.
The bill also contains other policy changes. It encourages more hospitals and doctors to set up “accountable care organizations” that would move away from traditional fee-for-service billing, which encourages needless tests and procedures. How successful those organizations will be at cutting costs is uncertain.
The law requires the state’s Medicaid program, state employee health care program and all other state-financed health care programs to adopt alternatives to fee-for-service payments, like paying a flat fee for all the care a patient will need over a year or bundling payments for doctors and hospitals to coordinate a patient’s care.
Other useful provisions include a requirement that health care providers report regularly on cost trends and quality measures, which should help patients shop comparatively; a new $60 million fund to invest in programs to reduce obesity, diabetes, asthma and other chronic diseases; $30 million to accelerate conversion to electronic health records; and malpractice reforms that could reduce litigation without imposing caps on damage awards.
Some critics worry that the state will not have the personnel and resources to do an effective job of enforcing these provisions. Others warn that the bill could impose burdensome regulations on health care providers and damage a cornerstone of the state’s economy.
Still, hospital and doctors’ groups have been supportive, and the bill was approved unanimously in the Senate and overwhelmingly in the Assembly. That may be a sign, some say, that the bill lacks the teeth needed to control the way providers set prices.
But don’t count Massachusetts out. It led the way in expanding coverage. What happens there on cost control will offer valuable lessons for the rest of the country.
------------
"State health care industry spent $19M lobbying lawmakers"
By Steve LeBlanc, Associated Press, May 23, 2015
BOSTON (AP) — Hospitals, insurers, doctors, unions and pharmaceutical companies spent a record $19 million trying to sway Beacon Hill lawmakers last year, a reflection of the industry's political and economic muscle and a rapidly changing health care landscape.
In less than a decade, lobbying by the industry has nearly doubled from the $10.8 million spent in 2007, according to an Associated Press review of lobbying reports filed with the state secretary's office.
During those years the industry has had to adapt to the state's landmark 2006 health care law and the rollout of the federal law it inspired, signed by President Barack Obama in 2010.
The group that spent the most on health care lobbying last year was the Massachusetts Association of Health Plans, which represents 17 insurers providing coverage to more than 2.6 million Massachusetts residents. It reported spending more than $1 million.
MAHP President Lora Pellegrini said the industry has faced a number of challenges, from grappling with last year's failed launch of the new Health Connector website to the implementation of a 2012 law designed to overhaul the state's health care payment system.
"Our activities reflect the seriousness and volume of issues our industry tackled in 2014," Pellegrini said.
Tim Gens, executive vice president of the Massachusetts Hospital Association, echoed that frustration. He said nearly one in five of the 6,000 or so bills filed at the Statehouse touch on health care.
"The health care sector is the largest sector in the state," he said. "We are going through a dynamic period in which virtually every aspect of the delivery and payment systems is subject to change."
The group reported spending $882,470 on lobbying last year, the second most of any group.
An emerging trend in health care lobbying in Massachusetts is among companies hoping to grow and sell marijuana for medicinal use under a 2012 ballot question approved by voters.
No dispensaries have opened, but at least nine companies filed lobbying reports for last year, although less than half reported spending any money, a total of $143,000. That could expand in coming years as more dispensaries win licenses and begin opening their doors.
Lobbying reports typically detail a range of expenses, from the salaries of paid lobbyists to office costs like photocopying, rent, public relations, telephone bills and computer equipment.
Of the more than $1 million spent by the Massachusetts Association of Health Plans, for example, $701,000 went to salaries, $245,000 went to operating expenses and $110,000 went to meals, entertainment and transportation costs.
Companies are barred from making direct contributions to lawmakers, but the lobbyists they hire can donate up to $200 a year to lawmakers and candidates.
Government watchdog groups have warned that the millions of dollars spent by health care groups could crowd out the voices of citizens and patients who don't have the deep pockets of hospitals and insurers.
But the health care groups argue that the lobbying they are engaged in will also help patients by improving the overall delivery of care.
Rich Copp, a spokesman for Partners HealthCare, Massachusetts' largest hospital and physicians' network, said their top concerns include access to substance abuse treatment and mental health services and making sure the state offers adequate reimbursement for the care doctors and nurses provide to MassHealth, the state's Medicaid program.
"We have an obligation to ensure that our patients and employers have a voice in the ongoing health care conversation," Copp said.
Copp said a decision by Partners to abandon plans to merge with South Shore Hospital after a court rejected the agreement and Attorney General Maura Healey said she would try to block any future merger wasn't much of a factor in the $645,000 the company spent on lobbying last year.
One of the state's largest unions, the Massachusetts Nurses Association, was also among the top five in the industry measured by lobbying dollars. The group reported spending $576,000 last year.
David Schildmeier, a spokesman for the union, said the group was focused on a handful of initiatives last year, including one that sets strict limits on the number of patients that registered nurses who work in intensive care units can be assigned at a given time.
The law, approved by the Legislature last June, took effect in October.
"Our main concern has been to ensure safer care for patients," Schildmeier said.
------------






































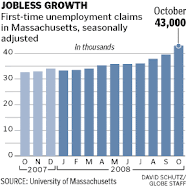







































































































.png)












































































































































































































































































1 comment:
Thiis is a great post thanks
Post a Comment